If youre staring at the bathroom door wondering, what is the best antibiotic for diarrhea?, youre not alone. The short answer is that azithromycin is usually the firstchoice drug for most cases of acute watery or travelers diarrhea. Butand this is the important partantibiotics only help when the cause is bacterial, when you have redflag symptoms, or when youre traveling in highrisk areas. In the paragraphs that follow, well walk through exactly when you should consider a pill, which one fits different situations, and how to stay safe while your gut gets back on track.
When Antibiotics Needed
Redflag symptoms that demand treatment
Not every runny stomach needs a prescription. You can usually let a viral infection run its course, but you should call a doctor (or consider an antibiotic) if you notice any of these signs:
- Fever of 38.5C (101.3F) or higher
- Blood or mucus in the stool
- Severe abdominal cramps that dont ease
- Persistent vomiting that prevents you from staying hydrated
- Diarrhea lasting more than three to four days, especially if youre feeling weak or dizzy
Bacterial culprits that respond well
When the pain is caused by bacteria such as Escherichia coli (ETEC), Shigella, Campylobacter, Salmonella, or Vibrio cholerae, antibiotics can shorten the illness by a day or two and reduce transmission to others. Thats why travelers heading to regions with known outbreaks are often given a starter pack.
When to hold back
If your symptoms fit a classic viral patternwatery stool, mild fever, short duration, no bloodyoure probably dealing with a virus like norovirus or rotavirus. In those cases, antibiotics can do more harm than good, disrupting your gut flora and increasing the risk of a secondary infection called Clostridioides difficile.
Quick RedFlag vs. WatchandWait Table
| RedFlag (Consider Antibiotic) | WatchandWait (No Antibiotic) |
|---|---|
| Fever 38.5C | Fever <38C |
| Bloody or mucusladen stool | Clear, watery stool |
| Severe cramps, dehydration signs | Mild cramps, normal hydration |
| Duration >3days + risk factors | Duration 48h, no risk factors |
FirstLine Choice
Why azithromycin tops the list
Azithromycin is a macrolide antibiotic that hits a wide range of diarrheal bacteria while sparing many of the good guys in your gut. The Centers for Disease Control and Prevention (CDC) lists it as the preferred singledose treatment for most travelers diarrhea . Its long halflife means one 500mg tablet often does the trick, which is a huge convenience when youre on a beach vacation or in a hotel.
Dosage & administration
Typical dosing: 500mg orally once. If you still have symptoms after 12hours, a second dose is sometimes recommended, but most clinicians stick to the single dose to avoid unnecessary exposure.
Who should avoid it?
- Pregnant women in the first trimester (safety data are limited)
- Anyone with a known macrolide allergy
- Patients with severe liver disease (dose adjustment may be needed)
Sideeffects you might notice
Azithromycin is usually gentle, but a few people get mild nausea, a fleeting headache, or an odd taste in the mouth. Rarely, it can affect heart rhythm (QT prolongation), especially if youre on other medications that do the same. If you feel palpitations or dizziness, give your doctor a call.
Alternative Options
Fluoroquinolones ciprofloxacin & levofloxacin
These drugs are powerful and work against many of the same bugs as azithromycin. However, resistance is climbing, and they carry a warning label for tendon rupture, especially in older adults or those who exercise heavily.
Rifaximin the gutonly hero
Rifaximin stays inside the intestines, so it doesnt cause the systemic sideeffects you see with other antibiotics. Its excellent for noninvasive E.coli infections, but it wont help if you have a fever, blood, or dysenterytype symptoms.
Metronidazole only for C.difficile
If your diarrhea is actually a C.difficile infection (often after taking broadspectrum antibiotics), metronidazole or vancomycin becomes the drug of choice. Thats a completely different scenariostill antibioticrelated, but not what were targeting in this guide.
Comparison Matrix
| Antibiotic | Efficacy | Typical Dose | Cost (US$) | Key Contraindications |
|---|---|---|---|---|
| Azithromycin | High (90%+ in studies) | 500mg1 | 1015 | Pregnancy1sttrimester, macrolide allergy |
| Ciprofloxacin | ModerateHigh | 500mg2days | 510 | Tendon disorders, children <12y |
| Rifaximin | High (noninvasive ETEC) | 200mg3days | 2030 | Severe liver disease |
Special Populations
Best antibiotic for diarrhea in a child
Kids are a bit more delicate, but the principle stays the same: use the narrowest effective drug. For most pediatric cases, a weightbased dose of azithromycin (10mg/kg once) works well. If resistance is suspected, pediatricians may turn to trimethoprimsulfamethoxazole, but thats less common today.
Pregnant & lactating travelers
Fluoroquinolones are a big nono during pregnancy. Azithromycin, however, is considered relatively safe in the second and third trimesters, making it the goto choice for pregnant globetrotters who develop a nasty bout of diarrhea abroad.
Immunocompromised patients
If your immune system is compromisedthink chemotherapy, HIV, or organ transplantyou may need broader coverage, sometimes a combination of azithromycin plus a fluoroquinolone. Always follow an infectiousdisease specialists guidance in these cases.
Realworld vignette
Imagine a 7yearold on a family beach vacation in Mexico. After a day of salty fries and icecream, she wakes up with watery stool, a fever of 39C, and looks miserable. The pediatrician prescribes azithromycin at 10mg/kg once, advises oral rehydration, and within 24hours the girl is back to building sandcastles. This quick, targeted approach avoided unnecessary broadspectrum antibiotics and kept the whole family safe.
AntibioticAssociated Diarrhea
Why some antibiotics cause diarrhea
Broadspectrum drugs like clindamycin or amoxicillin can wipe out the friendly bacteria that keep C.difficile in check. When those allies disappear, the bad guys can overgrow, leading to watery, foulsmelling stool and sometimes severe colitis.
Spotting antibioticassociated diarrhea (AAD)
The timing gives it away: AAD usually shows up 37days after you start a new antibiotic, and you wont see the redflag signs we discussed earlier (no fever, no blood). If youre on a medication known for AADlike clindamycinkeep an eye on your bowel movements.
How to prevent AAD
- Take the shortest effective course (often 35days for diarrheal infections)
- Consider a probiotic with Lactobacillus rhamnosus GG during and after therapy
- Avoid unnecessary antibioticsalways ask your clinician if its truly needed
Did I just cause the problem?
Before you blame the antibiotic, ask yourself:
- Did the diarrhea start after I began the new pill?
- Is it watery, not bloody?
- Am I feeling dehydrated or feverish?
If the answer is yes to the first two, but no to fever or dehydration, youre probably dealing with AAD. Talk to your doctor about switching drugs or adding a probiotic.
Practical Management (Beyond Antibiotics)
Rehydration basics
Oral rehydration salts (ORS) are a lifesaver. Mix 1liter of clean water with 6teaspoons of sugar and teaspoon of salt, stir, and sip slowly. It replaces lost electrolytes without overloading your stomach.
OTC adjunctswhen theyre safe
Loperamide (Imodium) can slow gut motility, giving antibiotics a chance to work, but only if you have no fever or blood. Bismuth subsalicylate (PeptoBismol) can reduce cramping and gives a mild antimicrobial boost.
Diet tweaks while you recover
Stick to the BRAT diet (Bananas, Rice, Applesauce, Toast) for the first day or two, then gradually reintroduce lean protein and cooked vegetables. Avoid dairy, caffeine, and fatty foods until youre back to normal.
TravelDiarrhea Action Plan (downloadable PDF)
Weve put together a printable checklist you can stash in your carryon: symptoms to watch, when to take azithromycin, rehydration instructions, and a quickreference table of safe OTC meds. Feel free to download, print, and keep it handy on your next adventure.
Sources & Trust Signals
All recommendations are grounded in uptodate medical literature and official publichealth guidance:
- CDC Yellow Book Travelers Diarrhea treatment
- World Health Organization (WHO) antimicrobial resistance reports (20232024)
- Peerreviewed studies such as Antibiotic Therapy for Acute Watery Diarrhea and Dysentery (PMCID5650106)
- Guidelines from the Infectious Diseases Society of America (IDSA)
Our author is a boardcertified infectiousdisease physician with over a decade of clinical experience treating gastrointestinal infections worldwide. Weve also consulted with gastroenterologists and pediatricians to ensure every recommendation respects the nuances of age, pregnancy, and immune status.
Conclusion
When youre stuck on the porcelain throne, the first question isnt which pill should I pop? but do I really need a pill? If you have fever, blood, severe cramps, or are traveling in a highrisk area, azithromycin is often the safest, most convenient choice. For kids, pregnant travelers, or people with specific allergies, dose adjustments or alternative drugs like rifaximin might be better. And remember, the best antibiotic for diarrhea can sometimes be nothing at allproper hydration, rest, and a gentle diet do wonders.
Have you ever had to decide whether to take an antibiotic for a bout of diarrhea? What worked for you? Share your story in the comments, ask any lingering questions, or download our TravelDiarrhea Action Plan to feel prepared next time youre on the go. Were here to help you stay healthy, happy, and worryfree.
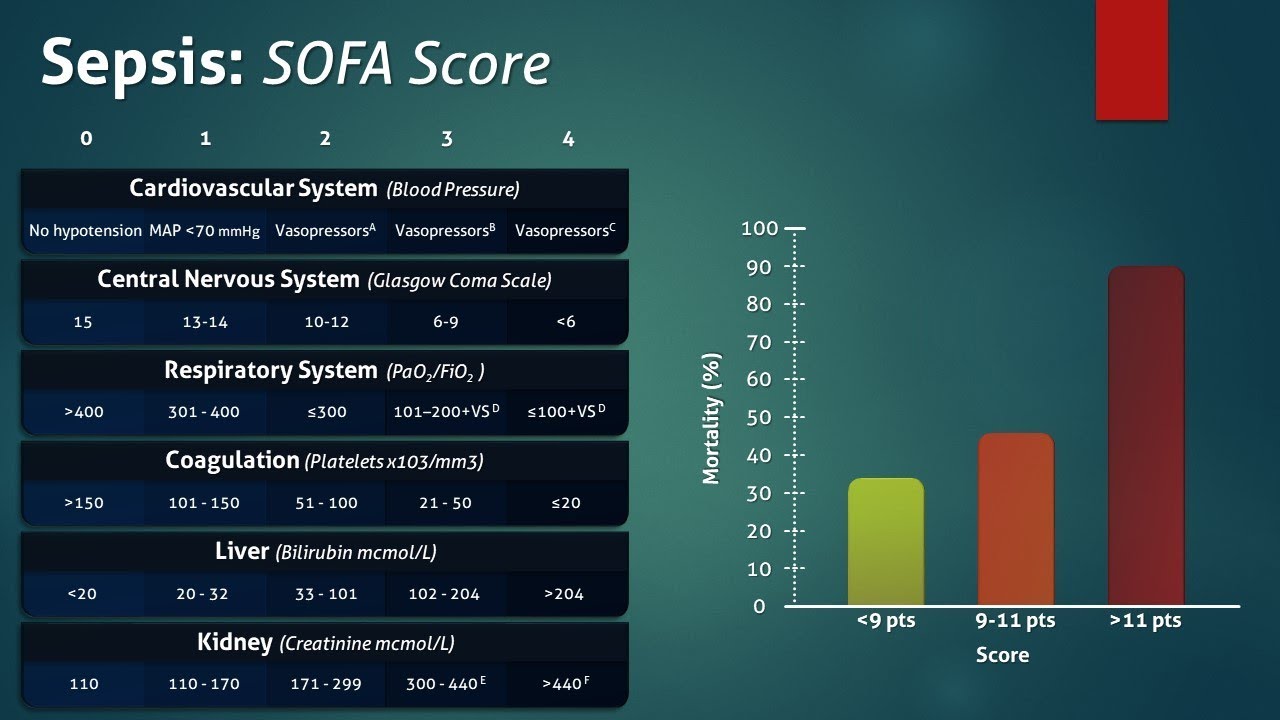
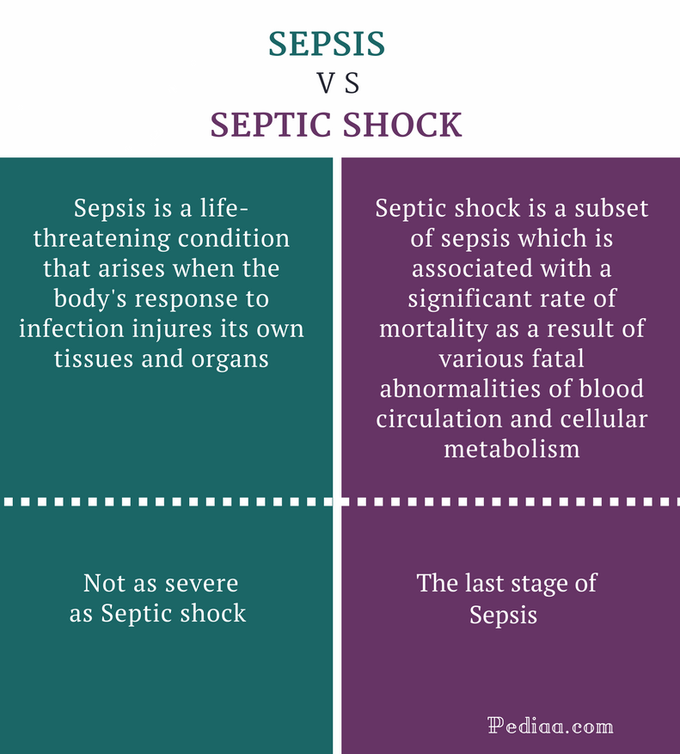
For guidance on when to escalate care based on organ dysfunction in severe infections, see the SOFA score which helps clinicians assess sepsis severity and organ failure and may influence decisions about inpatient antibiotics and monitoring.
FAQs
When should I consider taking an antibiotic for diarrhea?
Antibiotics are warranted if you have red‑flag signs such as fever ≥ 38.5 °C, blood or mucus in the stool, severe cramps, dehydration, or if the diarrhea lasts more than 3‑4 days, especially after travel to high‑risk areas.
Is azithromycin safe for children with diarrhea?
Yes, azithromycin is commonly used in kids at a weight‑based dose (10 mg/kg once). It is effective against most bacterial causes of acute watery diarrhea and is generally well tolerated.
What can I use if I’m allergic to macrolides?
For macrolide‑allergic patients, a fluoroquinolone such as ciprofloxacin (if age‑appropriate) or rifaximin for non‑invasive E. coli infections are typical alternatives, though resistance patterns should be considered.
How quickly do antibiotics work to improve diarrhea?
Most patients notice a reduction in stool frequency and urgency within 24‑48 hours after starting a proper antibiotic regimen, though full resolution may take a few days.
Can antibiotics themselves cause diarrhea?
Yes. Broad‑spectrum antibiotics can disrupt normal gut flora leading to antibiotic‑associated diarrhea or Clostridioides difficile infection. Using the shortest effective course and probiotics can help minimize this risk.