Lets cut to the chase: dysautonomia happens when the autonomic nervous systemyour bodys autopilot for heart rate, blood pressure, digestion, temperature, and morefails to keep everything running smoothly. The reasons range from genetic quirks and past injuries to hidden infections and everyday habits. Knowing whats behind the chaos can turn a confusing, exhausting journey into a roadmap for better control.
Why does this matter to you? Because once you spot the root cause, you and your doctor can target treatment, dodge flareups, and improve daytoday life. Ready to dig in? Grab a cup of tea (or coffee, no judgment) and lets explore together.
Understanding Dysautonomia Basics
What is the autonomic nervous system (ANS)?
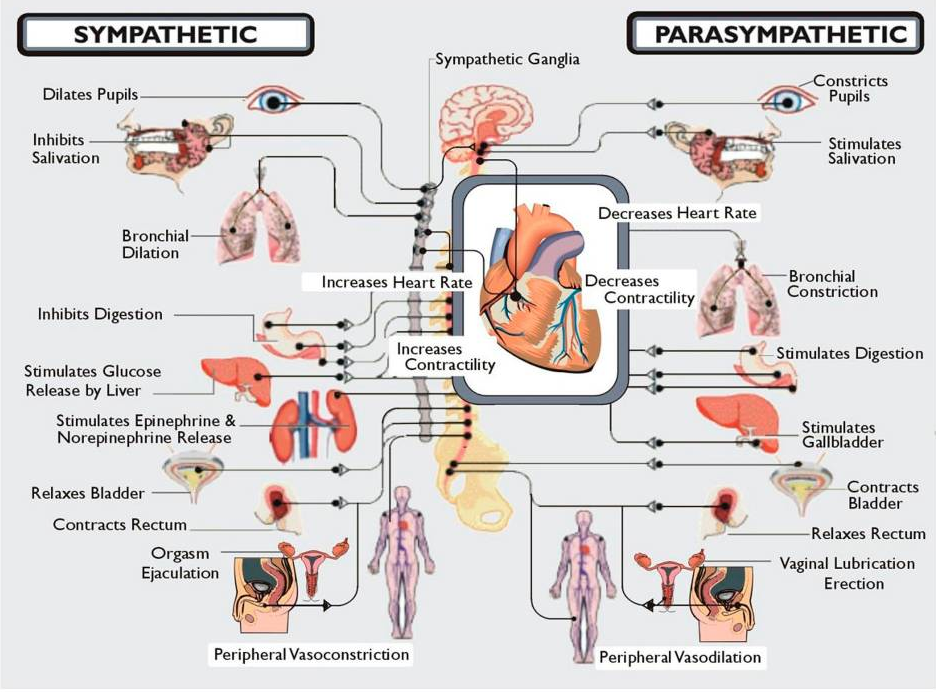
The ANS is the part of your nervous system that works behind the scenes, like a backstage crew that makes sure the lights, sound, and curtains move at the right time. It controls heart rhythm, blood vessel tone, sweat glands, digestion, and even how you react to stress. When it misfires, you feel symptoms like dizziness, rapid heartbeat, or digestive troubles.
Quick visual: Think of the ANS as a thermostat that also runs the kitchen, the security system, and the engine all at once.
How does ANS dysfunction become dysautonomia?
When the signals that travel between your brain, spinal cord, and the rest of your body get scrambled, the autopilot cant adjust to changeslike standing Lets cut to the chase: dysautonomia happens when the autonomic nervous systemyour bodys autopilot for heart rate, blood pressure, digestion, temperature, and morefails to keep everything running smoothly. The reasons range from genetic quirks and past injuries to hidden infections and everyday habits. Knowing whats behind the chaos can turn a confusing, exhausting journey into a roadmap for better control. Why does this matter to you? Because once you spot the root cause, you and your doctor can target treatment, dodge flareups, and improve daytoday life. Ready to dig in? Grab a cup of tea (or coffee, no judgment) and lets explore together. The ANS is the part of your nervous system that works behind the scenes, like a backstage crew that makes sure the lights, sound, and curtains move at the right time. It controls heart rhythm, blood vessel tone, sweat glands, digestion, and even how you react to stress. When it misfires, you feel symptoms like dizziness, rapid heartbeat, or digestive troubles. When the signals that travel between your brain, spinal cord, and the rest of your body get scrambled, the autopilot cant adjust to changeslike standing up fast or warming up after a workout. This mismatch produces the classic dysautonomia symptoms. While anyone can develop dysautonomia, its more common in: Some forms of dysautonomia are baked into our DNA. Rare mutationslike PHOX2B for congenital central hypoventilation syndromecan directly disrupt autonomic control. Even more common genetic predispositions can make you more vulnerable when a trigger (like illness or stress) shows up. Head injuries, spinal cord damage, or even major surgeries can sever or irritate the nerve pathways that the ANS relies on. The damage doesnt always show up on standard scans, but the symptomslike abnormal heart rate or blood pressure spikescan be a clear sign. Viruses love to hijack nerve cells. Lyme disease, EpsteinBarr virus, and the lingering effects of COVID19 (often called long COVID) are notorious for triggering dysautonomia. The immune response can inflame autonomic pathways, leaving them permanently altered. Diseases that already mess with nerves, blood vessels, or hormones can later evolve into dysautonomia. Diabetes (through peripheral neuropathy), Parkinsons disease (affecting heart rate regulation), and autoimmune disorders are major culprits. Some drugsespecially certain antidepressants, betablockers, and chemotherapy agentscan inadvertently suppress autonomic function. Heavy metal poisoning (lead, mercury) or chronic alcohol use also mess with the ANS. Even everyday choices can nudge the autonomic system toward trouble. Dehydration, excessive caffeine or alcohol, tight clothing, and exposure to extreme heat or cold are frequent flareup catalysts. Stress spikes adrenaline, which can overwhelm an already fragile autonomic system. Likewise, lack of sleep impairs the brains ability to regulate heart rate and blood pressure. Women often notice worsening symptoms during their menstrual cycle or menopause. Hormones like estrogen influence blood vessel tone, making the ANS more susceptible to swings. Hot, humid days can cause vasodilation and a sudden drop in blood pressure, while high altitude reduces oxygen availability, both challenging the ANS. Heres a Trigger vs. Quick Fix cheat sheet: First, your doctor will ask about every odd sensation youve hadpalpitations, dizziness, digestive upsets, even temperature swings. A thorough dysautonomia symptom checklist can help you remember the details. Tests like the tilttable study, QSART (Quantitative Sudomotor Axon Reflex Test), and heartrate variability analysis objectively measure autonomic function. These procedures are usually done at referral centers or university hospitals. There are reputable online quizzes that give a preliminary indicationthink of them as a quick screen. However, theyre not diagnostic tools. If your quiz results suggest dysautonomia, schedule a professional evaluation. Blood panels can reveal underlying conditions: blood glucose for diabetes, thyroid hormones for thyroid disease, antibodies for autoimmune disorders, and viral serologies for infections. If dysautonomia stems from diabetes, tighter glucose control can halt progression. For postviral cases, antiviral or antiinflammatory therapies may alleviate the autonomic strain. Simple habits can make a world of difference. Regular, moderate exercise (like recumbent cycling), a balanced salty diet, and consistent sleep hygiene are cornerstone strategies. Scientists are exploring autonomic neurostimulation, geneediting for rare hereditary forms, and novel immunomodulators for autoimmunedriven dysautonomia. While still experimental, these avenues offer hope for future breakthroughs. For most people, life expectancy remains normal if the condition is managed well and serious complications (like severe heart rhythm problems) are avoided. The key is early diagnosis and targeted treatment. Heres a quick rundown of the most commonly recognized forms. Knowing the label can guide you to the right specialists and support groups. So, whats the big picture? Dysautonomia isnt a single monster; its a collection of possible bugs in the bodys automatic pilot, each with its own backstory. Whether its a genetic script, a head injury, a lingering virus, or the simple fact that youre not drinking enough water, each cause shapes how you feel daytoday. Understanding the cause empowers you to: Remember, youre not alone. Communities, specialist clinics, and research groups are continuously learning and sharing. If youve spotted a pattern in your own symptoms, jot it down, bring it to your clinician, and start the conversation. Feeling a little overwhelmed? Thats totally okay. Start small: track your water intake for a week, note any moments when you feel lightheaded, and see if theres a connection to meals, stress, or temperature. Then, schedule a visit with a neurologist or cardiologist who knows autonomic disorders. Bring this guide (or a printed copy) alongyoull look prepared and proactive. Have you discovered a hidden trigger that helped you feel better? Or perhaps youre just beginning to piece together the puzzle. Share your story in the comments below, or reach out if you have questions. Were all learning together, and your experience could be the missing clue someone else needs. If you need help with insurance or financial support for complex treatments related to autonomic disorders, resources on Exondys 51 insurance provide useful examples of navigating coverage and assistance programs.Understanding Dysautonomia Basics
What is the autonomic nervous system (ANS)?
Quick visual: Think of the ANS as a thermostat that also runs the kitchen, the security system, and the engine all at once.
How does ANS dysfunction become dysautonomia?
For a deeper dive into the physiology, see .
Who is most at risk?
Primary Causes Overview
Genetic & Inherited Factors
Storytime: Ella, a 28yearold teacher, discovered that her familys history of fainting episodes traced back to a genetic mutation. After genetic testing, she finally understood why her random collapses werent random at all.
Trauma and Physical Injury
According to , up to 30% of patients report a traumatic event preceding symptom onset.
Infections & PostViral Syndromes
Quick stat: A 2023 study found that 12% of longCOVID patients develop newonset dysautonomia symptoms.
Chronic Medical Conditions
Table: Prevalence of Dysautonomia Across Select Conditions
Condition Approx. % with Dysautonomia Diabetes 1520% Parkinsons disease 3040% EhlersDanlos syndrome 7080% Autoimmune thyroiditis 1012% Medications & Toxic Exposures
Tip: If you suspect a medication is a trigger, never stop it coldturkey. Talk to your provider about alternatives.
Lifestyle & Environmental Triggers
Checklist for a quick selfaudit (great for a dysautonomia symptom checklist):
Common FlareUp Triggers
Daily stress and poor sleep
Quick fix: Aim for 79 hours of quality sleep and practice a 5minute breathing exercise before bed.
Hormonal changes
Consider keeping a hormonesymptom diary to spot patterns.
Weather & altitude
Practical tip: On heatwaves, stay indoors with a fan and hydrate aggressively; at altitude, ascend gradually and monitor your pulse.
Managing triggers
Trigger Quick Fix Dehydration Drink 2L water + 1g salt Excess caffeine Swap one cup for herbal tea Standing too fast Rise slowly, do calf pumps Heat exposure Cool shower, loose clothing How Diagnosis Works
Medical history and symptom checklist
Pro tip: Bring a written list to appointments. It shows youre proactive and helps the clinician spot patterns.
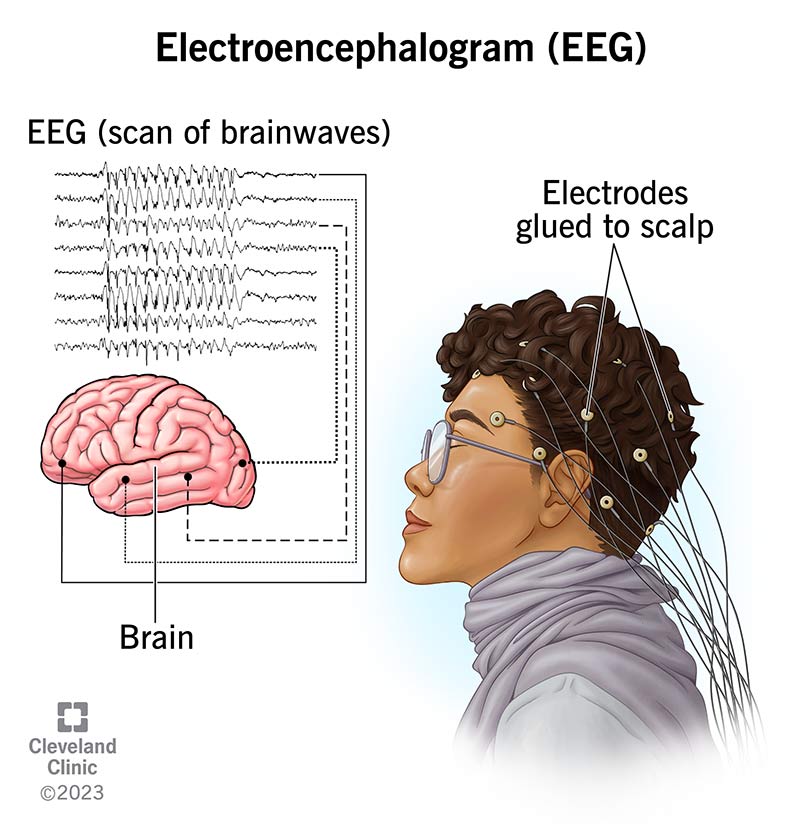
Specialized autonomic testing
According to a recent review, a tilttable test correctly identifies orthostatic intolerance in over 85% of suspected cases.
Do I have dysautonomia quiz?
Remember: A quiz is a conversation starter, not a final verdict.
Laboratory workup
Sample lab panel: CBC, CMP, HbA1c, TSH, antinuclear antibodies (ANA), Lyme PCR.
Tailored Treatment Options
Addressing the underlying cause
Case vignette: Marks blood pressure spikes vanished after his endocrinologist adjusted his insulin regimen and added a lowdose fludrocortisone.
Symptomfocused therapies
Lifestyle modifications
New research from the 2024 Autonomic Society suggests that a combined approachmedication plus structured exercisereduces symptom severity by up to 45%.
Emerging therapies & research
What about dysautonomia life expectancy?
Types of Dysautonomia
What are the 15 types?
Type Key Symptoms Typical Triggers Primary Causes Postural Orthostatic Tachycardia Syndrome (POTS) Rapid heart rate on standing, fatigue Heat, dehydration Autoimmune, hypermobile joints Neurocardiogenic Syncope (NCS) Fainting, lightheadedness Stress, prolonged standing Vagal overactivity Pure Autonomic Failure (PAF) Low blood pressure, anhidrosis Cold exposure Degenerative nerve loss Multiple System Atrophy (MSA) Parkinsonlike symptoms, bladder issues Progressive Alphasynuclein accumulation Familial Dysautonomia (FD) Impaired pain perception, blood pressure swings Genetic PHOX2B mutation Baroreflex Failure Severe blood pressure spikes Neck surgery, radiation Baroreceptor damage Vasovagal Syncope Fainting triggered by emotion Stress, pain Vagal reflex Orthostatic Hypotension (OH) Dizziness on standing Medications, dehydration Peripheral neuropathy ColdInduced Autonomic Dysfunction Extreme cold intolerance Cold exposure Unknown/idiopathic Autoimmune Autonomic Ganglionopathy Broad autonomic failure Autoimmune activity Antibodymediated Diabetic Autonomic Neuropathy GI motility issues, urinary problems Longstanding diabetes Chronic hyperglycemia Hyperadrenergic POTS High norepinephrine, anxietylike Stress, caffeine Excess sympathetic tone Postviral Dysautonomia Fatigue, tachycardia Recent infection Immunemediated nerve injury Chronotropic Incompetence Inadequate heart rate response Exercise limitation Sinus node dysfunction Putting It All Together
Next Steps & Gentle Call to Action