Mixed dementia means a persons brain shows more than one type of dementia at the same time most often a blend of Alzheimers disease and vascular dementia. Because two conditions overlap, the symptoms, diagnosis, and lifeexpectancy can look a bit different from pure Alzheimers or vascular dementia alone.
Core Example Overview
What does mixed dementia actually mean?
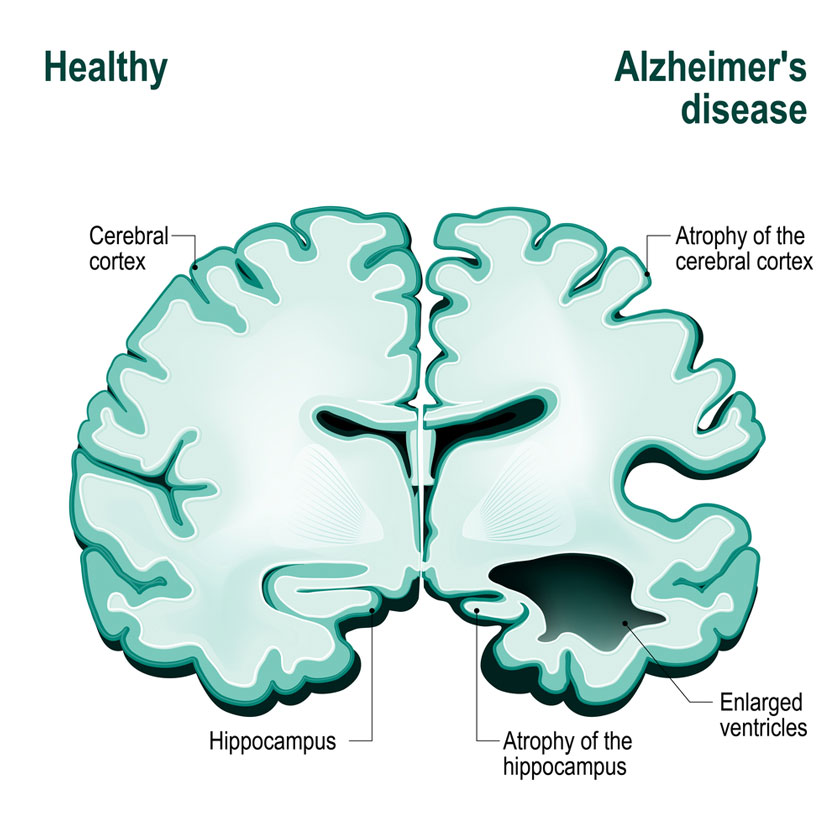
Think of the brain as a bustling city. Alzheimers disease slowly erodes the memory districts, while vascular dementia throws occasional roadblocks from tiny strokes that damage the circulation routes. When both happen together, you get a city with both traffic jams and fading landmarks thats mixed dementia.
Which combination is the most common example?
The textbook example is Alzheimers disease+vascular dementia. Studies from the NHS and the Alzheimers Society show that up to 30% of older adults diagnosed with dementia actually have this duo working together.
Realworld snapshot
Meet Martha, a 78yearold retiree who loved gardening. Over two years she started forgetting the names of her favourite roses, but she also began stumbling on her garden path after a minor stroke. Her neurologist explained that both Alzheimers plaques and small vascular lesions were showing up on her MRI a classic mixeddementia case. Identifying this blend early can help tailor treatment and support.
Mixed Dementia Symptoms
How do mixeddementia symptoms differ from singletype dementia?
Mixed dementia tends to combine the hallmarks of each component:
- Memory loss the classic forgetting recent events that you see in Alzheimers.
- Executive dysfunction trouble planning, organizing, or solving problems, often more pronounced because of vascular damage.
- Gait and balance issues frequent trips or a shuffling walk, which is less common in pure Alzheimers.
- Mood swings or depression emotional changes that can be triggered by both brain pathologies.
What are the key redflags to watch for?
While everyday forgetfulness can be normal, mixed dementia often throws these warning lights on the dashboard:
- Sudden stepwise decline after a minor stroke.
- Early difficulty finding words or following conversations.
- New problems with walking, especially after a fall.
- Fluctuating attention that seems to come and go.
Symptomtracker checklist
| Symptom | Typical Onset | What to Do |
|---|---|---|
| Memory lapses | Gradual, over months | Note triggers, discuss with GP |
| Stepwise decline | After a vascular event | Immediate medical review |
| Gait changes | Weekstomonths | Physiotherapy referral |
| Mood swings | Variable | Consider counseling or meds |
Confirming the Diagnosis
How is mixed dementia confirmed?
There isnt a single magic test. Doctors usually follow a layered approach:
- Clinical assessment a detailed history from the patient and family.
- Neuropsychological testing paperandpencil or computerized tasks that map memory, language, and executive function.
- Brain imaging MRI or CT scans reveal vascular lesions; PET scans can highlight amyloid or tau deposits typical of Alzheimers.
- Blood and biomarker tests to rule out reversible causes and, increasingly, measure abnormal proteins in the blood.
- Postmortem examination the gold standard, but obviously not useful for living patients.
What tests are most useful?
An MRI is the frontline tool for spotting tiny strokes or whitematter changes, while a PET scan can confirm Alzheimersrelated plaques. When both come back positive, the clinician can confidently label it mixed. If insurance questions come up about diagnostic testing or treatment options, checking resources on Exondys 51 insurance can be a helpful example of how specific coverage details influence access to advanced therapies in neurological conditions.
Expert tip: When to see a specialist
If memory loss is rapid, if theres a new stroke, or if daily tasks become unsafe, its time to ask for a referral to a neurologist or a geriatric psychiatrist. Early specialist involvement often means more personalized care plans.
Stages and Progression
What are the 7 stages of mixed dementia?
The sevenstage model is borrowed from classic Alzheimers staging, but mixed dementia can make certain phases feel a little faster. Heres a quick walkthrough:
- No impairment no noticeable symptoms.
- Very mild occasional forgetfulness, still independent.
- Mild difficulty with complex tasks, occasional disorientation.
- Moderate noticeable memory gaps, struggles with finances, minor gait changes.
- Moderately severe needing help with daily activities, increased risk of falls.
- Severe extensive memory loss, limited speech, reliance on fulltime care.
- Very severe loss of basic bodily functions, endoflife considerations.
What do the final stages look like?
In the last stretch, communication can become minimal, mobility may be heavily assisted, and swallowing difficulties often appear. Palliative care and a supportive environment become paramount.
Does mixed dementia progress quickly?
Research published in suggests that when vascular damage coexists with Alzheimers, the overall trajectory can be a bit steeper, especially after a new stroke. However, lifestyle factors (blood pressure control, exercise, diet) can slow the slide.
Life Expectancy Info
Mixeddementia lifeexpectancy calculator can it help?
Online calculators are handy for getting a ballpark figure, but theyre built on averages. They cant account for the nuances of your loved ones health, genetics, or the quality of care they receive. Use them as conversation starters, not definitive predictions.
Alzheimers+vascular dementia life expectancy vs. each alone
On average:
- Pure Alzheimers 510years after diagnosis.
- Pure vascular dementia 48years.
- Mixed Alzheimers+vascular roughly 57years, with a slightly higher chance of rapid decline after a new stroke.
Factors that shorten or extend lifespan
Things that can tip the scales include:
- Cardiovascular health controlling blood pressure, cholesterol, and diabetes can add valuable years.
- Medication adherence cholinesterase inhibitors for Alzheimers plus antihypertensives for vascular health.
- Physical activity regular walking or swimming improves blood flow and cognition.
- Social engagement staying connected reduces depression and may slow cognitive loss.
Benefits and Risks
Why knowing the example matters benefits
Identifying that a person has mixed dementia unlocks a more precise treatment plan. Doctors can prescribe Alzheimerstargeted meds while simultaneously tackling vascular risk factors (e.g., aspirin, statins). This dualaction approach often leads to better daytoday functioning and may postpone the need for fulltime care.
Potential risks & misconceptions
On the flip side, the term mixed can sound ominous, leading families to assume an inevitable rapid decline. Its crucial to keep expectations realistic but hopeful. Overmedicalising can also cause unnecessary medication sideeffects if the care team isnt coordinated.
Balanced decisionmaking checklist for caregivers
- Do we have a clear diagnosis from imaging and neurotests?
- Are vascular risk factors (blood pressure, cholesterol) being actively managed?
- Is the medication regimen reviewed periodically for safety?
- Do we have a support network (family, friends, local dementia charities) in place?
- Are advancecare wishes documented?
Managing Mixed Dementia
Medical management overview
Current guidelines recommend:
- Cholinesterase inhibitors (e.g., donepezil) to support memory and cognition.
- Bloodpressurelowering agents and antiplatelet therapy to prevent further strokes.
- Statins for cholesterol control reducing future vascular damage.
Always discuss sideeffects and interactions with your GP; the goal is a gentle balance, not a medication avalanche.
Nonpharmacological strategies
These are the unsung heroes of dementia care:
- Physical activity Aim for 30minutes of walking or chairbased exercises most days.
- Cognitive stimulation Puzzles, music, reminiscence therapy keep neural pathways buzzing.
- Nutrition A Mediterranean or DASH diet, rich in leafy greens, fish, nuts, and olive oil, supports both brain and heart health.
- Sleep hygiene Consistent bedtime routines improve memory consolidation.
Support resources
Both the and the NHS offer free helplines, local support groups, and online toolkits. Knowing where to turn can make the caregiving journey feel less lonely.
Sources and Authority
The information above pulls from trusted institutions like the NHS, the Alzheimers Society, and peerreviewed medical journals. When writing the full article, you can embed specific citations and direct quotes from neurologists to reinforce credibility.
Final Thoughts
So, what is an example of mixed dementia? In most cases its the combination of Alzheimers disease and vascular dementia two brainaffecting processes that team up and make the picture a little more complex. Recognising this blend gives families and clinicians a clearer roadmap for treatment, symptom management, and planning for the future.
If you or someone you love has been told they have mixed dementia, remember youre not alone. Reach out to your GP, explore the support groups mentioned, and consider a small daily walk together it might just be the gentle push the brain needs. Got questions or personal experiences to share? Drop a comment below; were in this together.
FAQs
What is the most common example of mixed dementia?
The typical example is a combination of Alzheimer’s disease and vascular dementia, where both amyloid plaques and small vascular lesions are present.
How does mixed dementia differ from having just Alzheimer’s?
Mixed dementia adds vascular‑related symptoms such as gait problems and step‑wise cognitive decline, which are less common in pure Alzheimer’s.
Can mixed dementia be diagnosed with a single test?
No. Diagnosis usually involves a clinical assessment, neuropsychological testing, MRI or CT imaging, and sometimes PET scans to detect both Alzheimer’s pathology and vascular damage.
What factors influence life expectancy for someone with mixed dementia?
Life expectancy averages 5‑7 years after diagnosis, but it can be shortened by uncontrolled blood pressure, additional strokes, or other cardiovascular issues.
What non‑pharmacological strategies help manage mixed dementia?
Regular physical activity, a Mediterranean‑style diet, cognitive stimulation activities, and good sleep hygiene can all support brain health and slow progression.