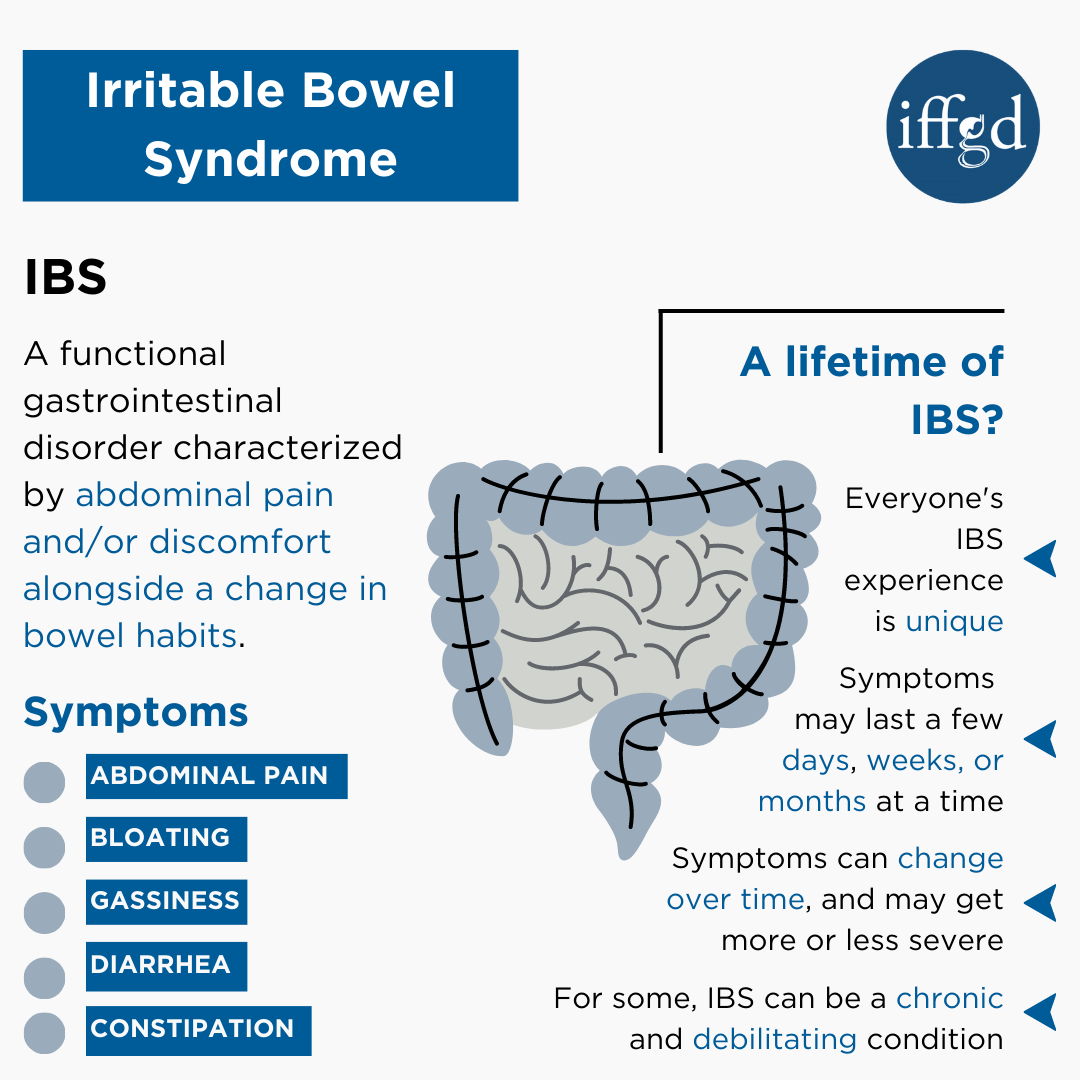
Short answer: IBS isnt caused by a single thing. It usually springs from a mix of gutbrain miscommunication, certain foods, stress, past infections, genetics, and an outofbalance microbiome. Knowing which pieces are playing a role in your own story can be the first step toward feeling better.
In the next few minutes Ill walk you through the most common triggers, how they show up in everyday life, and what evidencebased steps you can take to calm the chaos in your gut. Think of it as a chat over coffee with a friend who just happens to have a lot of research and a few personal anecdotes to share.
Why It Matters
What does cause really mean for IBS?
When doctors talk about causes, theyre really talking about factors that tip the delicate balance between your brain, nerves, and intestines. If any one of those parts gets out of sync, you can end up with cramping, bloating, and the dreaded bathroom dash.
How does knowing the cause improve treatment?
Imagine trying to fix a leaky faucet without knowing whether the leak is in the pipe, the faucet handle, or the water pressure. Same idea with IBS pinpointing the main culprit lets you target therapy, whether thats a diet tweak, a stressreduction practice, or a specific medication. For example, some people benefit from targeted ulcerative colitis supplements when inflammatory patterns are suspected, while others need a strict dietary reset or stress-focused therapy.
Minicase study: Janes threeyear IBS journey
Jane spent years blaming just stress for her flareups. After keeping a simple food and symptom diary, she discovered that a daily latte and a nightshift schedule were the real triggers. Cutting back on caffeine and adding a short mindfulness routine shrank her episodes by half.
Quickreference table: Cause Typical symptom pattern
| Trigger | How it Shows Up |
|---|---|
| Stress | Intermittent cramping, altered bowel habit |
| Postinfectious | Sudden onset of diarrhea after gastroenteritis |
| HighFODMAP foods | Gas, bloating, pain after meals |
| Hormonal shifts | Worsening around menstrual cycle |
Common Triggers
Stress, anxiety & the braingut connection
The gut and brain talk through the vagus nerve, hormones, and even immune signals. When youre stressed, that conversation can turn into a shouting match. The result? Muscles in the colon contract too hard or not enough, leading to the classic IBS rollercoaster.
Postinfectious IBS
Ever had a stomach bug that seemed to clear up, only to be followed by weeks of belly trouble? Thats postinfectious IBS. An infection can inflame the lining of the intestine, and for some people the inflammation sticks around, messing with motility and sensation.
Foodrelated triggers
Some foods are notorious for fermenting in the gut and producing excess gas. The lowFODMAP dietnamed after fermentable oligo, di, monosaccharides and polyolshas become the goldstandard approach for many.
Top10 IBStrigger foods
- Beans and lentils
- Onions and garlic
- Wheat (especially in bread)
- Rye and barley
- Apples, pears, stone fruits
- Cauliflower and broccoli
- Carbonated drinks
- Artificial sweeteners (e.g., sorbitol)
- Caffeine
- Alcohol
Hormonal influences especially for women
Research from the shows that estrogen and progesterone can affect gut motility. Many women notice that symptoms flare up just before or during their perioda phenomenon called menstrualrelated IBS.
Lifestyle Factors
Daily routine changes
Travel, shift work, or even a new exercise schedule can scramble your internal clock. When your circadian rhythm is off, the guts own timingwhen it contracts and relaxescan get out of sync, leading to occasional IBS bursts.
Toilet habits
Delaying the urge to go, or constantly checking for a bathroom, can train the colon to hold stool longer than it should. Over time, this can increase sensitivity and pain.
Psychological distress
Depression, PTSD, or chronic anxiety dont just live in the mindthey can amplify gut pain. A study in highlights this braingut loop.
Reallife anecdote: Marks nightshift cramps
Mark switched to a rotating night shift at his warehouse. Within a month, he was waking up with sharp lowerabdominal cramps. By moving his biggest meals to earlier in the day and adding a short evening meditation, his symptoms faded dramatically.
Food & Diet
The lowFODMAP diet explained
LowFODMAP works by temporarily removing the biggest fermentable carbs, then systematically reintroducing them to see which ones truly cause you trouble. Its not a foreverforever restrictionjust a detectives toolkit.
IBS foods to avoid (quick list)
Onion, garlic, beans, wheat, rye, apples, honey, dairy (if lactose intolerant), and sugarfree gum (sorbitol) tend to be the biggest culprits.
Can diet cure IBS permanently?
While a welldesigned diet can put many people into remission, theres no universal cure. The gut is a living ecosystem; changes in stress, hormones, or a new infection can bring symptoms back. Think of the diet as a sturdy foundation you can build on, not a onetime fix.
Balancing nutrients while cutting triggers
Dont fear losing fiber or vitamins. Replace highFODMAP fruits with berries, use glutenfree whole grains like quinoa or rice, and swap dairy with lactosefree or fortified plant milks. If gluten or gluten reactions are a concern, consider reading more about mindful approaches to a gluten detox as part of a structured plan rather than an indefinite restriction.
Sample grocery list & swap ideas
- Swap wheat bread for sourdough (lowFODMAP portion)
- Replace cabbage slaw with carrotginger salad
- Use lactosefree yogurt for probiotic boost
- Choose almond milk instead of cows milk
Medical & Biological Factors
Genetics does family history matter?
If a parent or sibling has IBS, your odds are higher, suggesting a hereditary component to gutbrain signaling and microbiome composition.
Gut microbiome imbalance & SIBO
Smallintestinal bacterial overgrowth (SIBO) can mimic or worsen IBS. A breath test can identify excess hydrogen or methane, guiding targeted antibiotic or probiotic therapy.
Neurological signaling the braingut axis
The brain communicates with the gut via nerves and hormones. When that line gets static, the gut may overreact to normal stimuli, making you feel pain after a tiny bite of food.
Other conditions that mimic IBS
Inflammatory bowel disease (IBD), celiac disease, and thyroid disorders can produce similar symptoms. Proper testing helps rule these out, ensuring you get the right treatment.
Flowchart: When to test for SIBO
| Symptom Pattern | Next Step |
|---|---|
| Frequent bloating, gas, alternating constipation/diarrhea | Breath test for hydrogen/methane |
| Sudden onset after antibiotics | Consider SIBO workup |
| Persistent symptoms despite diet | Consult gastroenterologist |
Diagnosing the Underlying Cause
Clinical interview symptom checklist
A good doctor will ask about timing (e.g., Does it get worse before your period?), diet, stress levels, and any recent infections. This conversation is often the most revealing part of the diagnosis.
Laboratory tests
Stool analysis can detect inflammation or infection. Blood work may rule out anemia, thyroid issues, or celiac disease. Breath tests check for SIBO or lactose intolerance.
Imaging & endoscopy
Usually reserved for redflag signs: weight loss, blood in stool, or severe pain. Colonoscopy or CT scans can rule out IBD or tumors.
Sample questionnaire: Spotting patterns
- Do you notice symptoms after stressful meetings?
- Do certain foods consistently trigger bloating?
- Do symptoms change with your menstrual cycle?
- Have you had a recent stomach infection?
Managing & Treating IBS Based on Identified Causes
Targeted dietary therapy
If highFODMAP foods are the main culprit, a structured lowFODMAP plan can bring relief. If stress is dominant, diet alone may not clear the sky.
Stressreduction techniques
Mindfulness meditation, yoga, and cognitivebehavioral therapy (CBT) have strong evidence for reducing IBS severity. Even a fiveminute breathing exercise before meals can calm the gut.
5minute breathing script
Sit upright, inhale slowly for 4 seconds, hold for 2, exhale gently for 6. Repeat five times while visualizing your stomach relaxing.
Probiotics & microbiome modulation
Not all probiotics are equal. Strains like Bifidobacterium infantis and Lactobacillus plantarum have shown benefit in randomized trials. Choose a product with at least 10billion CFU and a clear strain list.
Pros & cons table of popular probiotic products
| Product | Pros | Cons |
|---|---|---|
| Brand A (B. infantis) | Clinically studied for IBS | Higher price |
| Brand B (L. plantarum) | Broad spectrum | Mixed research outcomes |
| Generic multistrain | Affordable | Less specific evidence |
Medications
When diet and stress tools arent enough, doctors may prescribe antispasmodics for cramping, loperamide for diarrhea, or a lowdose tricyclic antidepressant to calm visceral pain. Always discuss benefits and sideeffects with your provider.
When surgery or advanced therapies are considered
Rarely, severe, refractory cases may need procedures like nerve block injections or, in extreme cases, bowel resection. These are lastresort options after exhausting conservative measures.
Putting It All Together
IBS is a puzzle with many moving pieces. By listening to your body, tracking food and stress, and partnering with a knowledgeable clinician, you can often identify the key triggers that keep you stuck in a loop of discomfort.
Take a moment now to jot down any patterns youve noticed over the past weekmaybe its that latenight coffee, a stressful Zoom call, or even the time of month. That simple act of awareness can be the first brick in building a life with fewer flareups.
Remember, youre not alone in this. Millions share the same confusing symptoms, and the good news is that science, combined with personal trialanderror, offers a roadmap to relief.
Conclusion
What causes irritable bowel syndrome? A blend of gutbrain signaling glitches, dietary triggers, stress, past infections, genetics, and microbiome shifts. By pinpointing which of these play a role in your own experience, you can tailor a plan that feels both realistic and effectivewhether thats a lowFODMAP reset, a daily mindfulness habit, or a targeted medication. Stay curious, keep tracking, and dont hesitate to reach out to a healthcare professional who can help you translate these insights into a personalized care plan that truly works for you.
FAQs
What is the main cause of irritable bowel syndrome (IBS)?
IBS is caused by a combination of factors including gut-brain miscommunication, certain foods, stress, prior infections, genetics, and an imbalance in gut microbiome. No single cause is responsible; rather, it's the interaction of these elements that triggers symptoms.
How do stress and anxiety contribute to IBS?
Stress and anxiety disrupt the communication between the brain and gut, causing irregular muscle contractions in the colon. This can lead to cramps, bloating, and changes in bowel habits commonly seen in IBS.
Can infections cause IBS?
Yes, postinfectious IBS can develop after a gastrointestinal infection such as gastroenteritis, where inflammation persists and affects intestinal function, leading to ongoing symptoms.
Which foods are commonly known to trigger IBS symptoms?
Foods high in fermentable carbohydrates like beans, onions, garlic, wheat, certain fruits (apples, pears), cruciferous vegetables, caffeine, alcohol, and artificial sweeteners often trigger IBS symptoms by producing excess gas and discomfort.
Is there a genetic component to IBS?
Family history does increase the likelihood of developing IBS, which suggests genetics may influence gut-brain signaling or microbiome composition contributing to IBS symptoms.