But theres more to it than just a onesizefitsall plan. Sun protection, the right diet, and honest conversations with a skin specialist all play a role. Lets walk through everything you need to know, step by step, so you can feel confident making the best decision for your skin and your peace of mind.
Understanding Vitiligo
What causes vitiligo?
In simple terms, vitiligo happens when your immune system mistakenly attacks the cells that give skin its colourmelanocytes. Genetics, oxidative stress, and certain triggers (like severe sunburn or exposure to harsh chemicals) can tip the balance. The explains that its not a contagion, and it isnt caused by poor hygiene. Its a deeply personal, often emotional journey.
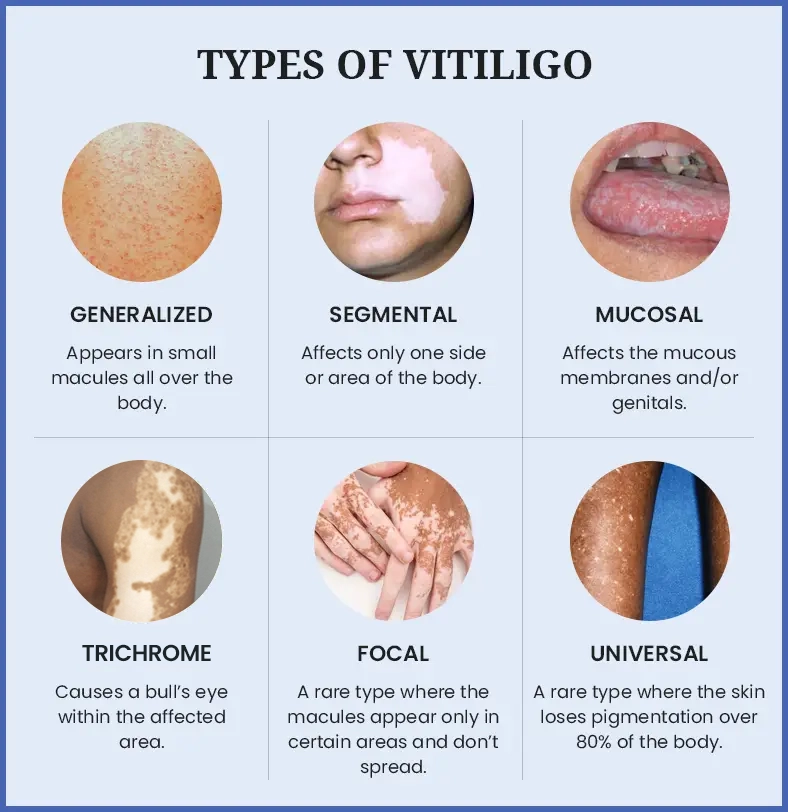
How does vitiligo progress?
There are two main patterns: nonsegmental (the most common, spreading symmetrically) and segmental (confined to one area). Some people notice rapid spreading, while others experience stability after a few months. Knowing your type helps your dermatologist tailor a plan that matches the pace of your skins changes.
When should you seek treatment?
Anytime the patches bother youwhether its the way sunlight makes them look brighter, the emotional toll, or a sudden flareupyou deserve professional help. Early intervention usually leads to better repigmentation rates, so dont wait for the patches to settle down.
Treatment Overview
What categories of vitiligo treatment exist?
Think of treatment options as a toolbox:
- Topical therapies prescription creams like corticosteroids, calcineurin inhibitors, and the newer ruxolitinib cream (OPZELURA).
- Light/phototherapy narrowband UVB (NBUVB), excimer laser, and PUVA.
- Systemic medications oral JAK inhibitors or shortterm steroids for extensive disease.
- Surgical options minipunch grafting, blister grafting, or melanocyte transplantation for stable, smallarea vitiligo.
- Cosmetic/camouflage makeup, selftanning products, and OTC vitiligo treatment creams that are purely cosmetic.
How effective are these options?
Research from the American Academy of Dermatology (AAD) shows that NBUVB combined with a topical steroid can achieve 3050% repigmentation after 1224 weeks. Ruxolitinib cream, the only FDAapproved vitiligo treatment cream, delivered notable colour return in roughly one-third of patients in a phase III trial.
What are the risks?
Every treatment carries a tradeoff. Topicals may thin the skin; phototherapy can cause temporary redness or, over many years, a slight increase in skincancer risk; systemic drugs bring infection concerns and require lab monitoring. Balancing benefits against sideeffects is key to a trustworthy plan.
Topical Creams
Which cream is the best vitiligo treatment cream?
The gold standard right now is OPZELURA (ruxolitinib). Its a JAKinhibitor that targets the inflammatory pathway behind melanocyte loss. Approved for patients 12years and older, its shown a 3040% improvement in repigmentation after 24weeks.
How do corticosteroid and calcineurin creams work?
Corticosteroids calm the immune attack, giving melanocytes a chance to bounce back. Calcineurin inhibitors (like tacrolimus) work similarly but tend to cause less skin thinning, making them a good option for delicate areas such as the face.
Can overthecounter creams help?
Most OTC vitiligo treatment creams are simply camouflage or moisturisers they wont repigment skin. Theyre handy for daytoday confidence, but dont expect a medical effect.
Application tips for maximum benefit
- Clean the area with gentle soap.
- Apply a thin layerno need to slather it on.
- Avoid covering the cream with airtight bandages unless your dermatologist advises.
- Combine with NBUVB sessions for a synergistic boost.
| Product | Type | Age Limit | Typical Cost (US$) | Success Rate |
|---|---|---|---|---|
| OPZELURA (ruxolitinib) | JAKinhibitor cream | 12+ | $250$300/month | 3040% repigmentation |
| Clobetasol propionate | Highpotency steroid | Any | $15$30 tube | 2030% (when combined) |
| Tacrolimus 0.1% | Calcineurin inhibitor | 2+ | $30$45 tube | 1525% (face & neck) |
Light Therapy
What is narrowband UVB phototherapy?
NBUVB emits light at 311313nm, a sweet spot that stimulates melanocyte migration without the severe sideeffects of older PUVA treatment. Sessions usually last 25 minutes, two to three times a week, and are considered the backbone of modern vitiligo care.
How does NBUVB compare to PUVA and excimer laser?
| Method | Pros | Cons | Typical Cost (US$) |
|---|---|---|---|
| NBUVB | Effective for many body sites, lower cancer risk | Requires multiple clinic visits | $100$150 for a course |
| PUVA | Good for thicker skin | Higher nausea, more UVA exposure | $150$200 |
| Excimer laser | Targets small areas, fast results | Expensive, limited to focal patches | $250$350 per session |
Can I use a home phototherapy unit?
Yesthere are FDAcleared home NBUVB devices. Theyre convenient but demand strict adherence to safety guidelines: proper distance, eye protection, and a physician's supervision to avoid overexposure.
Typical treatment protocol
Most dermatologists start with 23 sessions per week, gradually increasing exposure time based on skin response. A full course can range from 1224 weeks. Combining with a topical like ruxolitinib often accelerates colour return.
Longterm risks?
While NBUVB is relatively safe, prolonged use can cause premature ageing and a slight uptick in skincancer riskespecially for those with a history of intense sunburn. Regular skin checks keep things in check.
Systemic Options
When are oral medicines considered?
If vitiligo spreads quickly across large body areas, or if topical and light treatments arent moving the needle, doctors may turn to systemic drugs for a short, controlled rescue phase.
What oral options are out there?
- JAK inhibitors (tofacitinib, ruxolitinib tablets) offlabel use shows promise, especially paired with NBUVB.
- Oral corticosteroids usually a brief highdose burst to calm aggressive disease.
Success stories & limitations
Small studies published in JAMA Dermatology reported up to 60% repigmentation with tofacitinib plus NBUVB after six months. However, these drugs arent FDAapproved for vitiligo, and they require careful monitoring for infections and blood work abnormalities.
Safety monitoring
Anyone on systemic JAK inhibitors should have baseline labs (CBC, liver enzymes) and periodic checks every 23 months. Discuss any signs of infection with your doctor promptly.
Surgical Procedures
What surgical techniques are available?
When the disease has been stable for at least a year, surgery becomes an option. Common methods include:
- Minipunch grafting tiny skin plugs from pigmented donor sites.
- Blister grafting uses a suction blister to transfer epidermis.
- Melanocytekeratinocyte transplantation labgrown pigment cells placed onto depigmented skin.
Who is a good candidate?
If you have less than 20% of your body surface affected, the patches are stable (no new lesions for 12months), and youre comfortable with minor scarring, surgery could give you a lasting colour boost.
Success rates & recovery
Academic centers like UCDavis report 7080% colour match in carefully selected patients. Healing takes 12 weeks, with a followup period of several months to gauge durability.
Risks & costs
Potential complications include infection, graft failure, or mismatched colour. Costs vary widelyoften $3,000$8,000 per sessionso insurance coverage should be verified early.
Home Care Tips
Can vitiligo be treated at home?
While homecare cant replace medical therapy, it can enhance results and protect your skin:
- Sunscreen SPF30+ daily, reapply every two hours outdoors.
- Moisturizers keep skin barrier healthy.
- Camouflage makeup products like Dermablend blend patches for confidence.
- Balanced diet antioxidants (vitaminC, E) and adequate vitaminD may support melanocyte health.
What about DIY cures?
Theres a flood of how I cured my vitiligo stories online. Most involve unproven herbal mixes or extreme diets. While personal anecdotes are inspiring, they rarely stand up to scientific scrutiny. Treat them as motivational, not medical, content.
When to seek professional help?
If you notice rapid spreading, new lesions, or emotional distress, its time to book a dermatologist. Early, evidencebased treatment wins the day.
Choosing Your Plan
How to build a treatment plan with your dermatologist?
Bring photos of your patches (both closeup and fullbody), a list of any previous therapies, and a clear set of goalswhether you aim for full colour, partial improvement, or simply slowing progression. Open, honest dialogue helps your doctor tailor a plan that fits your lifestyle and budget.
Factors to consider
- Skin type and location of patches.
- Extent of depigmentation (percentage of body surface).
- Availability of phototherapy centres.
- Financial comfortsome treatments are pricey.
- Tolerance for sideeffects.
Decisionmaking checklist
- Is my vitiligo stable?
- Do I have access to NBUVB or a home unit?
- Am I comfortable using prescription creams daily?
- Whats my budget for ongoing care?
Costcomparison table
| Option | Typical OutofPocket Cost (US$) | Frequency | Notes |
|---|---|---|---|
| NBUVB (clinic) | 100150 per 12week course | 23/week | Most effective firstline |
| OPZELURA cream | 250300 per month | Twice daily | Only FDAapproved cream |
| Oral JAK inhibitor (offlabel) | 8001,200 per month | Daily | Requires lab monitoring |
| Surgical grafting | 3,0008,000 per session | Onetime | Best for stable, small areas |
| Camouflage makeup | 3080 onetime | As needed | Boosts confidence, no medical effect |
Future Research & Hope
What new drugs are on the horizon?
Phase II trials are testing more selective JAK1 inhibitors that may offer stronger pigment return with fewer systemic risks. Early data look promising, but well need larger studies before they become standard care.
Are geneediting or stemcell therapies real?
Researchers at Yale are exploring melanocyte stemcell transplants that could one day rebuild pigment from the ground up. Its still earlystage, but the science is moving faster than ever.
Will a permanent cure appear soon?
Experts, including Dr.King from the University of Pennsylvania, caution that vitiligo is a chronic autoimmune conditionmeaning permanent cure remains unlikely in the near term. However, many patients achieve longterm remission with consistent therapy, which is as close as we get right now.
Conclusion
At the end of the day, effective vitiligo treatment isnt a magic bullet; its a thoughtful blend of proven medical therapies, diligent home care, and emotional support. By partnering with a boardcertified dermatologist, using evidencebased options like NBUVB and the best vitiligo treatment cream (OPZELURA), and staying mindful of lifestyle factors, you give yourself the best shot at lasting colour and confidence.
If youre ready to take the next step, download our free treatmentplan worksheet below and schedule that dermatologist appointment. Your skin journey is personal, but you dont have to walk it aloneshare your thoughts, ask questions, or tell us how youve navigated treatment in the comments. Were all in this together.
For more on how autoimmune processes contribute to vitiligo, see the vitiligo autoimmune link discussion that explores the immune mechanisms and common triggers further.
FAQs
What is the most effective first‑line vitiligo treatment?
The combination of narrow‑band UVB phototherapy and the FDA‑approved ruxolitinib cream (OPZELURA®) is currently considered the most reliable first‑line option for achieving lasting repigmentation.
Can I use over‑the‑counter creams to restore colour?
Most OTC “vitiligo treatment creams” are purely cosmetic and do not stimulate repigmentation. They can help with camouflage, but for medical improvement prescription‑grade products are needed.
How often should I attend NB‑UVB sessions?
Typical protocols involve 2‑3 sessions per week, each lasting 2‑5 minutes, for a period of 12‑24 weeks. Your dermatologist will adjust the exposure based on your skin response.
Are oral JAK inhibitors safe for vitiligo?
Oral JAK inhibitors (e.g., tofacitinib) are used off‑label and can be effective, especially with phototherapy. They require baseline labs and regular monitoring for infections and blood abnormalities.
When is surgical grafting an appropriate option?
Surgery is considered when vitiligo has been stable for at least 12 months, affects less than 20 % of body surface, and other therapies have not provided satisfactory results.