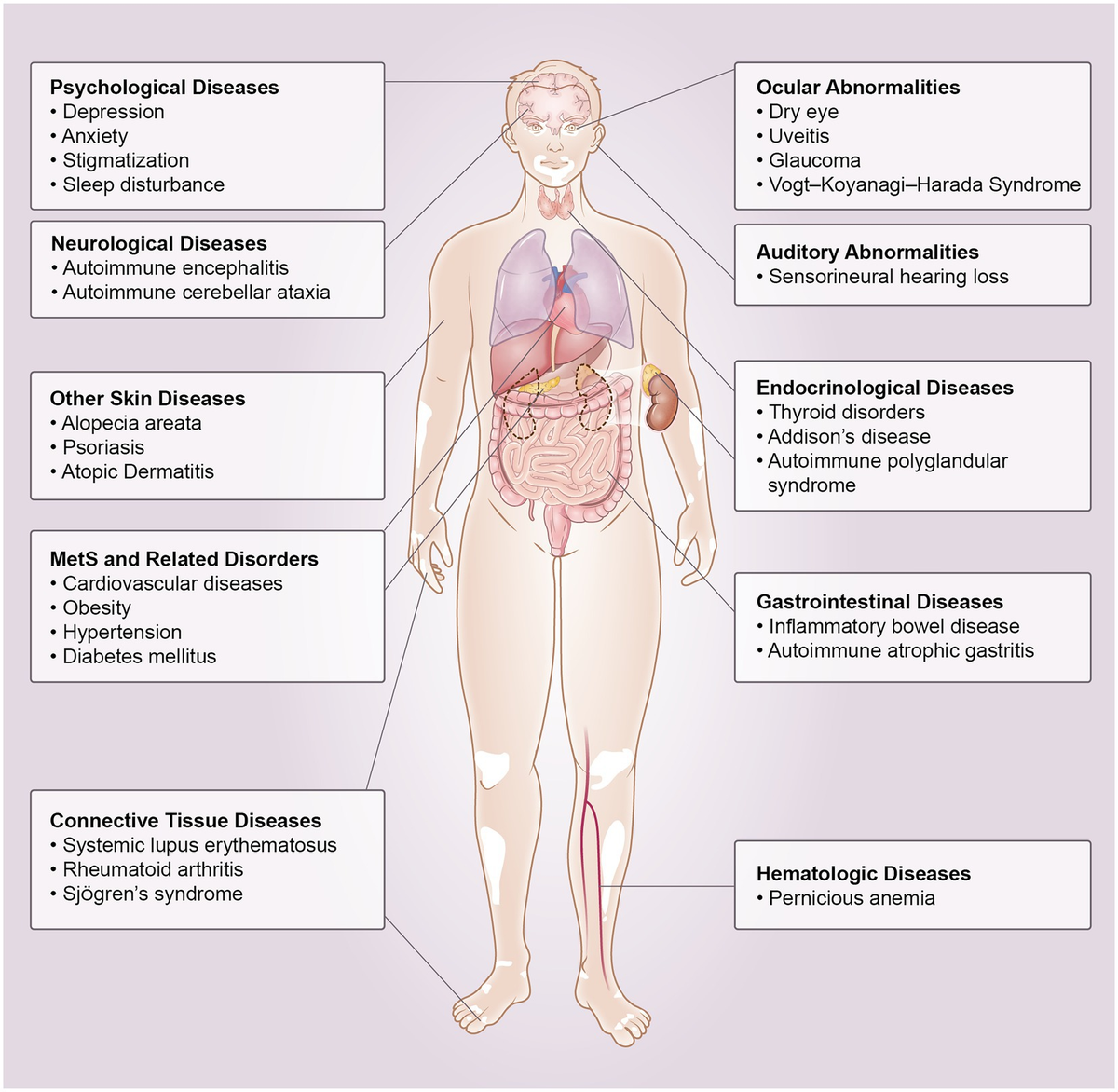
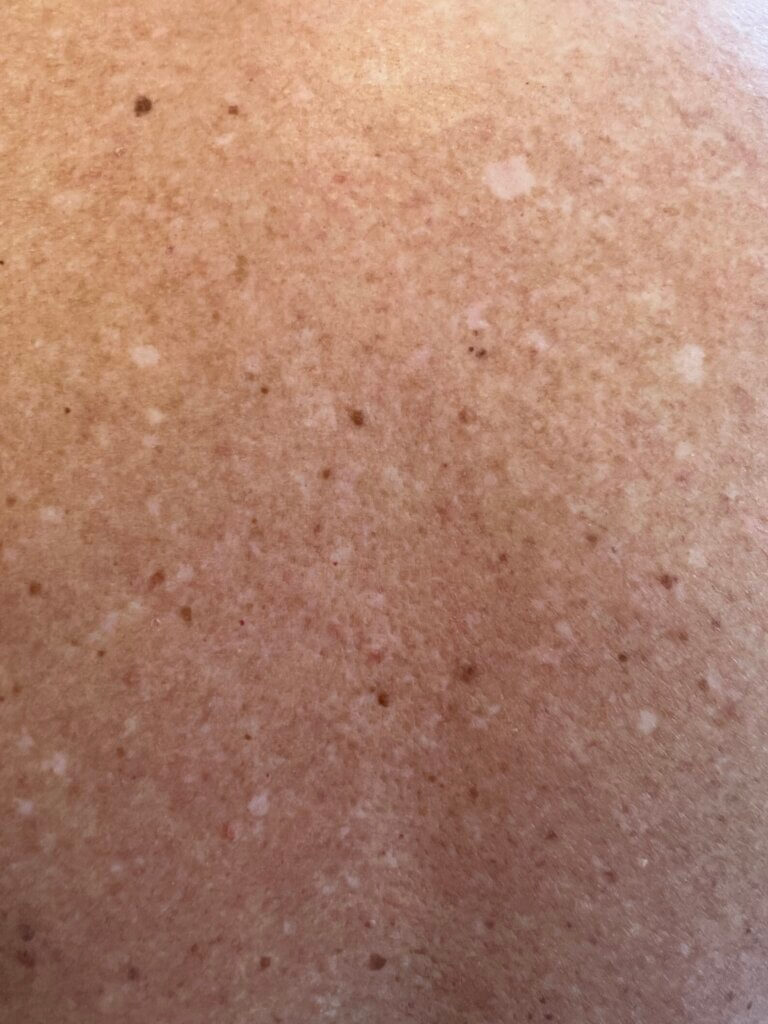
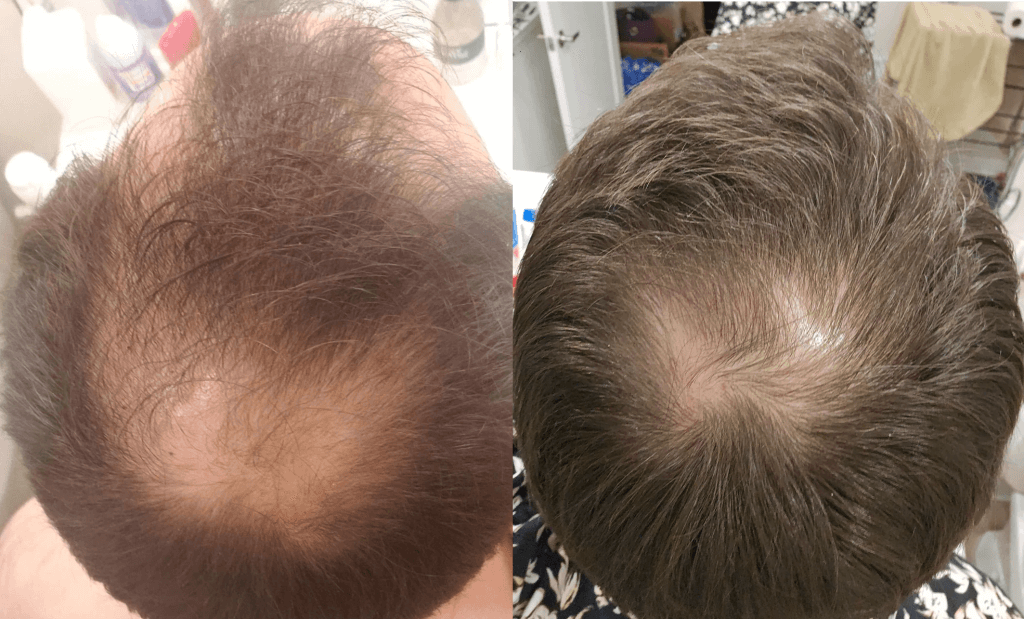
If youve noticed those sudden white patches on your skin, you might wonder if its just a cosmetic quirk or something deeper. The reality is a bit messier, and often the skin changes are just the tip of an immune-system iceberg. In the next few minutes well dive straight into the link between vitiligo and other autoimmune diseases, explore why it sometimes runs in families, and give you practical steps to keep both your skin and overall health in balance.
Quick Summary
Most specialists consider vitiligo an autoimmune conditionyour bodys defenders mistakenly attack the cells that give skin its color. Around 1525% of people with vitiligo develop a second autoimmune disorder, most commonly thyroid disease, type1 diabetes, or rheumatoid arthritis. Knowing this connection can turn a vague worry into a solid plan for early detection and treatment.
Common Companions
Autoimmune Thyroid Disease
Thyroid problems are the most frequent companions of vitiligo. Roughly onethird of vitiligo patients carry thyroidautoantibodies, meaning the gland is already under attack. Symptoms can be subtleslight fatigue, a few extra pounds, or a faint neck swelling. If you catch it early, a simple blood test and hormone replacement can keep you feeling like yourself again.
Type1 Diabetes
Its less common than thyroid disease, but still worth a glance. Studies show 24% of vitiligo cohorts also have type1 diabetes. The good news? A quick fasting glucose or A1C test at diagnosis of vitiligo can flag the condition before it sneaks up on you.
Rheumatoid Arthritis & Lupus
Joint pain, morning stiffness, or a rash that flares with sunlight? Those could be clues your immune system is juggling more than skin pigment. Roughly 0.7% of vitiligo patients juggle three or more autoimmune diseases, according to the . If you notice new aches, dont waittalk to a rheumatologist.
Bonus: LesserKnown Companions
| Condition | Approx. Prevalence in Vitiligo Patients |
|---|---|
| Alopeciaareata | ~5% |
| Inflammatory Bowel Disease | ~2% |
| Atopic Dermatitis | ~8% |
| Primary Biliary Cholangitis | ~1% |
Genetics vs Environment
Is Vitiligo Hereditary?
Family history does play a role, but its far from destiny. Research points to a 510% hereditary percentage. In plain terms, if a parent has vitiligo, youre a little more likely to see those patches, but most cases pop up without any close relatives showing the same signs.
Key Genetic Markers
Genes like NLRP1, PTPN22, and HLADRB1 keep showing up in genomewide association studies. Theyre the same suspects that appear in other autoimmune disorders, which explains why the conditions often travel together.
Environmental Triggers
Even with a perfect genetic sheet, the environment can flip the switch. Sunburn, oxidative stress from pollutants, or a simple skin injury (the Koebner phenomenon) can ignite a flareup. This is why many ask, what causes vitiligo to spread? The answer is usually a mix of trauma, stress, and an overactive immune response.
GeneEnvironment Interaction Checklist
- Family history Consider a genetics discussion with your doctor.
- Recent skin injury Watch the area for new patches.
- High stress periods Try mindfulness or short breathing breaks.
- Sun exposure Use sunscreen (SPF50+) daily.
Treatment Options
Standard SkinFocused Therapies
Topical steroids, calcineurin inhibitors, and narrowband UVB phototherapy are the workhorses for repigmentation. Theyre great at calming the immune assault on melanocytes, but they dont tackle any other autoimmune conditions you might have.
Systemic Approaches for Comorbidities
If you also have thyroid disease, a steady dose of levothyroxine can normalize hormone levels. For type1 diabetes, insulin therapy and routine glucose monitoring are essential. The key is coordinating careyour dermatologist, endocrinologist, and rheumatologist should be on the same page.
Emerging DualTarget Treatments
JAK inhibitors, such as ruxolitinib, have received FDA approval for vitiligo and are already on the market for rheumatoid arthritis. Early trials suggest they can calm the skin while also easing joint inflammation. Biologics like ustekinumab are being explored for patients battling multiple autoimmune diseases at once.
Lifestyle & SelfCare Checklist
| Action | Why It Helps | Frequency |
|---|---|---|
| Daily sunscreen (SPF50) | Reduces oxidative stress and prevents new patches | Every morning |
| Stressreduction (meditation, yoga) | Lowers immune activation | 10minutes daily |
| Balanced diet rich in antioxidants | Supports melanocyte health | At each meal |
| Routine labs (TSH, fasting glucose, ANA) | Early detection of comorbidities | Every 612months |
Action Plan
FirstVisit Checklist
When you finally sit down with a doctor, bring this simple list:
- Full skin examination note all patch locations and sizes.
- Blood panel: thyroidstimulating hormone (TSH), fasting glucose, and antinuclear antibodies (ANA).
- Familyhistory questionnaire jot down any relatives with vitiligo, thyroid disease, diabetes, or arthritis.
When to See a Specialist
- New thyroid symptoms: Fatigue, weight changes, or a swollen neck Endocrinologist.
- Joint pain or skin rashes: Persistent swelling or photosensitivity Rheumatologist.
- Rapid spread of white patches: Especially after sunburn or injury Dermatologist (consider phototherapy).
Support Communities
Youre not alone on this road. Groups like and the offer forums, webinars, and local meetups. Connecting with people who get it can turn confusion into confidence.
Conclusion
Vitiligo is more than skin deepmost experts agree its an autoimmune condition that can travel with thyroid disease, type1 diabetes, arthritis, and a handful of other immunerelated ailments. Genetics gives you a modest head start, while environmental triggers shape how quickly those white patches spread. The good news? Early screening, open communication between specialists, and a thoughtful mix of medical and lifestyle strategies can keep both your skin and your whole body thriving. If you havent already, schedule that comprehensive blood panel, join a supportive community, and remember: you have allies on every side of this journey. Whats your experience with vitiligo and other autoimmune conditions? Share your story in the commentsyour voice might help someone else feel less alone.
FAQs
What other autoimmune conditions are most often linked with vitiligo?
Thyroid disease, type 1 diabetes, rheumatoid arthritis, lupus, alopecia‑areata, inflammatory bowel disease, atopic dermatitis, and primary biliary cholangitis are the most commonly reported companions.
How likely is it that a person with vitiligo will develop a second autoimmune disorder?
Studies show that 15–25 % of people with vitiligo develop another autoimmune disease, with thyroid problems being the most frequent.
Can vitiligo be inherited?
Family history contributes about 5–10 % to risk. Certain genes such as NLRP1, PTPN22, and HLA‑DRB1 increase susceptibility, but most cases occur without a known affected relative.
What routine tests should someone with vitiligo consider?
A baseline panel including thyroid‑stimulating hormone (TSH), fasting glucose or A1C, and antinuclear antibodies (ANA) every 6–12 months helps detect common comorbidities early.
Are there treatments that address both vitiligo and its autoimmune partners?
JAK inhibitors (e.g., ruxolitinib) have shown benefit for skin repigmentation and can also reduce joint inflammation in rheumatoid arthritis. Ongoing research is evaluating other biologics for multi‑disease control.