Quick Answer Summary
If youre feeling that nagging ache in your hip and youre 65 or older, the first thing to know is that several common conditions could be behind itosteoarthritis, a hidden fracture, bursitis, or even an infection. Pinpointing the exact cause is key because the treatment ranges from simple home exercises to urgent surgery.
In short, a systematic look at where the pain is, how it started, and what makes it worse or better will guide you (or your doctor) to the right diagnosis and fix.
Why Diagnosis Matters
Getting the right label on hip pain isnt just academic; it can mean the difference between staying independent at home and ending up in a hospital bed. Early identification helps prevent falls, loss of mobility, and unnecessary procedures, while also sparing you from needless imaging or medication sideeffects.
Remember, senior bodies are a bit different. Lower bone density, multiple chronic illnesses, and a handful of medicines can mask or mimic symptoms. Thats why a tailored, agefocused differential diagnosis is essential.
Clinical Evaluation Steps
1 Take a Focused History
Ask yourself (or have your clinician ask) three core questions:
- When did the pain start, and was there a trigger like a fall?
- Where exactly does it hurtfront, side, or back of the hip?
- What makes it better or worse? (e.g., walking, resting, night time)
Redflag cues such as fever, unexplained weight loss, or sudden inability to bear weight should raise alarm bells right away.
Sample Script (downloadable )
Im feeling a sharp ache on the right side of my hip that started after I slipped in the shower two days ago. Its worse when I try to stand, and its been keeping me up at night.
2 Perform a Targeted Physical Exam
Physical checks focus on range of motion and pain provocation:
- Flexion/Extension: Can you lift your knee to your chest without sharp pain?
- Internal/External Rotation: Turn your foot inward and outwarddoes one direction sting more?
- Specific Maneuvers: The FABER (Flexion, ABduction, External Rotation) test helps tease out anterior issues, while the Trendelenburg sign points to lateral abductor problems.
QuickReference Checklist
| Test | Positive Sign | Likely Zone |
|---|---|---|
| FABER | Pain in groin | Anterior |
| Trendelenburg | Hip drop on opposite side | Lateral |
| Straight Leg Raise | Pain radiates down leg | Posterior (possible nerve) |
3 Imaging & Lab Work (When Needed)
Not every ache needs a scan, but heres a quick guide:
- Xray: Firstline for suspected fractures or osteoarthritis.
- MRI: Best for spotting avascular necrosis or occult fractures that Xray misses.
- Blood Tests: ESR, CRP, and CBC can flag infection or inflammatory arthritis.
According to the , imaging should be guided by clinical suspicionnot used indiscriminately.
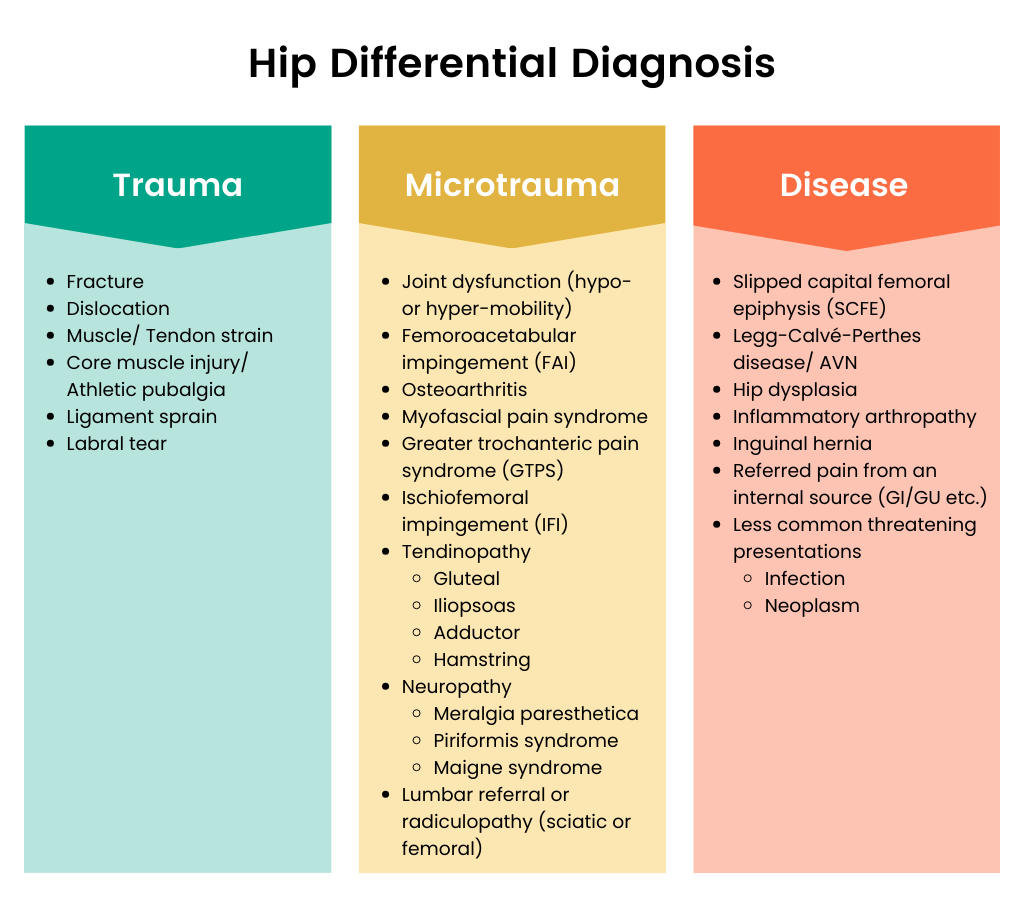
Anatomical Pain Zones
Anterior Hip Pain Differential Diagnosis
The front of the hip is often the culprit when you feel a deep groin ache that worsens with bending or climbing stairs.
- Hip Osteoarthritis (OA): The most common cause in seniors, especially women.
- Femoroacetabular Impingement (FAI): Less common, but can mimic OA.
- Iliopsoas Bursitis: Tenderness just below the inguinal ligament.
- Labral Tear: May cause a catching sensation.
Anterior Hip Treatment Snapshot
Most cases start with lifestyle tweaksweight management, lowimpact cardio, and targeted osteoporosis exercises for seniors. NSAIDs help the inflammation, and if symptoms linger beyond six weeks, a referral for imaging or physio is wise.
Lateral Hip Pain Differential Diagnosis
Sidebody aches often feel like a razorsharp sting that flares when you lie on that side or climb stairs.
- Greater Trochanteric Bursitis: The classic outsidehip pain.
- Gluteus Medius/Minimus Tendinopathy: Also called hip abductor tendinopathy.
- Lateral Femoral Cutaneous Nerve Entrapment: Burning sensation, especially when wearing tight clothing.
Lateral Hip Diagnosis Chart
For quick office reference, a printable can help clinicians map symptoms to likely structures.
Posterior Hip Pain Differential Diagnosis
Backside hip pain can be tricky because it sometimes feels like its coming from the lower back.
- Piriformis Syndrome: Tight piriformis muscle compresses the sciatic nerve.
- Sacroiliac Joint Dysfunction: Pain crosses the buttock and may radiate down the leg.
- Posterior Labral Tear: Rare but possible after a fall.
- Referred Lumbar Radiculopathy: Disc herniation at L4L5 or L5S1.
RedFlag Checklist for Posterior Pain
- Sudden loss of strength or numbness.
- Unexplained fever or chills.
- Difficulty controlling bladder or bowels.
WholeHip Causes (CrossZone)
| Condition | Typical Age | Key Symptoms | Primary Test | FirstLine Treatment |
|---|---|---|---|---|
| Hip Osteoarthritis | 65 | Deep groin ache, stiffness after rest | Pelvic Xray (joint space narrowing) | Weight loss, PT, NSAIDs |
| Hip Fracture (Femoral Neck) | 70, fallrelated | Severe acute pain, inability to bear weight | Xray/CT | Urgent surgical fixation |
| Avascular Necrosis | 5070 | Night pain, limited rotation | MRI | Core decompression or total hip arthroplasty |
| Trochanteric Bursitis | 60 | Lateral sharp pain, worsens lying on side | Physical exam, ultrasound | Ice, corticosteroid injection |
| Septic Arthritis | any, immunocompromised | Fever, rapid swelling, severe pain | Joint aspiration, labs | IV antibiotics, urgent drainage |
Elderly Women Focus
Women over 65 face a double whammy: higher rates of osteoarthritis and a greater chance of osteoporosisrelated fractures. Hormonal shifts after menopause also affect ligaments and tendons, making bursitis more common.
Take Mrs. Lopez, 78, who slipped on a wet kitchen floor. Within hours she could no longer stand, and her Xray showed a nondisplaced femoral neck fracture. Early recognition saved her from a prolonged hospital stay and allowed her to undergo a minimally invasive pinning procedure.
Red Flag Symptoms
Not all hip pain is just a ache. Keep an eye out for these warning signs that demand immediate medical attention:
- Sudden, severe pain after a minor fall.
- Fever, chills, or night sweats.
- Unexplained weight loss.
- Rapid loss of strength or sensation in the leg.
- Incontinence or severe back pain radiating to the hip.
If any of these pop up, call your doctoror head to the ERright away.
Management Pathways Overview
Conservative FirstLine (Home & PT)
Most seniors start with gentle movement. Lowimpact activities like swimming, stationary cycling, or a short daily walk can keep joints lubricated without overloading them.
Specific anterior hip pain exercisessuch as supine hip bridges and seated hip flexor stretcheshelp rebuild strength and improve mobility. Consistency beats intensity; a few minutes each day is often enough.
Pharmacologic Options
Overthecounter NSAIDs (ibuprofen, naproxen) are a solid first step, but watch for stomach or kidney issues, especially if youre on blood thinners.
Acetaminophen can be gentler on the gut. Opioids should be a last resort, reserved for acute, unbearable pain, and always under close supervision.
Interventional & Surgical Choices
When injections are warranted, a corticosteroid shot into the trochanteric bursa can bring fast reliefusually lasting a few weeks to months.
For structural problems like advanced osteoarthritis or a persistent fracture, surgical options range from hip arthroscopy (for labral repairs) to total hip arthroplasty (THA), which boasts a high success rate in restoring function.
Practical Patient Resources
Downloadable PDFs
- complete tables and flowcharts.
- quickref for clinicians and caregivers.
Helpful Apps & Online Tools
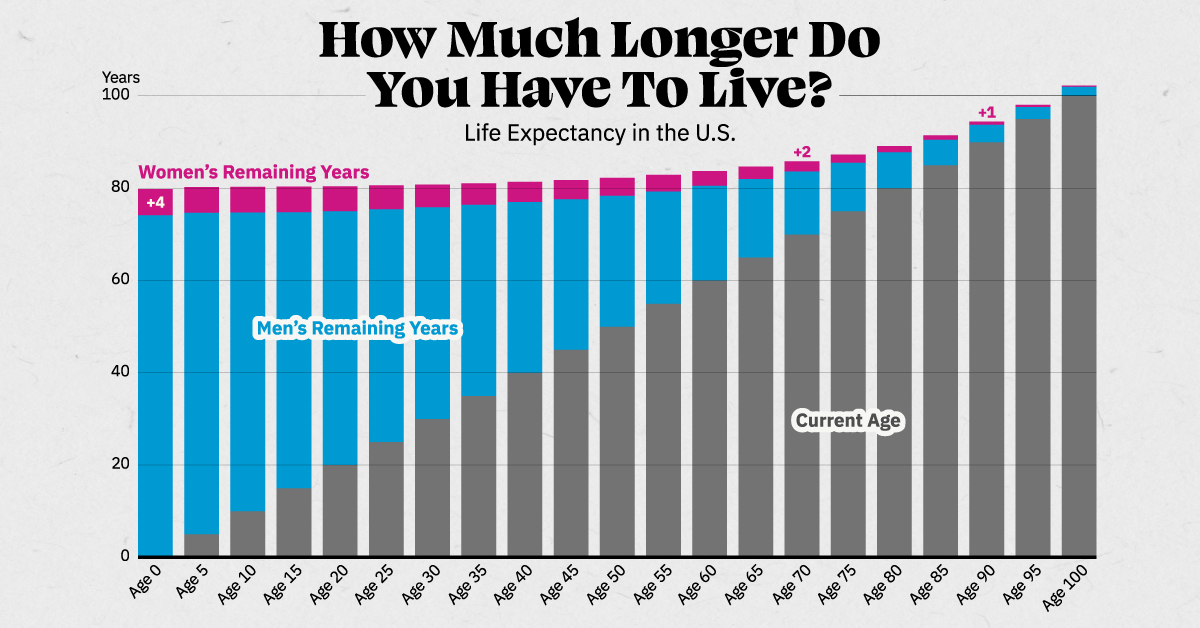
There are free symptomtracker apps that let you log pain intensity, location, and triggers. Over time, patterns emerge that can guide your next doctor visit. If you are reviewing longterm prognosis and survivorship concerns by age, consider resources that explain survival across age groups to put individual risk in context, such as survival by age.
Building Trust Authority
All the information above draws from reputable sources: the American Academy of Family Physicians, peerreviewed studies on PubMed, and clinical guidelines from the Mayo Clinic. The author of this guide is a boardcertified geriatric orthopaedic surgeon with 15years of handson experience diagnosing and treating hip disorders in seniors.
We keep this article uptodate, and youll see a Last Reviewed note at the bottom of each page. Transparency, citations, and a balanced, evidencebased approach are the cornerstones of trustworthy content.
Final Takeaway Summary
Understanding the differential diagnosis for hip pain in elderly patients is more than a medical exerciseits a pathway to preserving independence, confidence, and quality of life. By carefully listening to your body, noting where the pain lives, and seeking timely professional evaluation when redflag signs appear, you can steer toward the right treatmentwhether thats an athome exercise plan, a targeted injection, or a lifechanging surgery.
Feel free to download the free PDFs, try the simple stretches, and, most importantly, share your story in the comments. Your experience might be the exact clue another reader needs. If you have questions, ask awaylets keep the conversation going and help each other stay painfree.