Thinking about uvula removal? In a nutshell, its a short officebased procedure that trims or removes the little dangly tissue at the back of your throat to help with snoring, sleep apnea, or chronic throat irritation. Most folks bounce back in about a week, but like any medical decision there are pros, cons, costs, and a few quirks to know before you say yes.
Below well walk through why people consider it, what actually happens during the surgery, the short and longterm side effects, recovery tips, costs, alternatives, and realworld stories from people whove been there. Grab a coffee, and lets dive in together.
Why Consider Removal?
What problems can a uvulectomy help solve?
The uvula isnt just decorativeit can become a real nuisance. An enlarged or inflamed uvula can cause:
- Persistent snoring or mildtomoderate obstructive sleep apnea
- Chronic throat irritation, especially after infections
- Recurrent uvulitis or tonsillitis
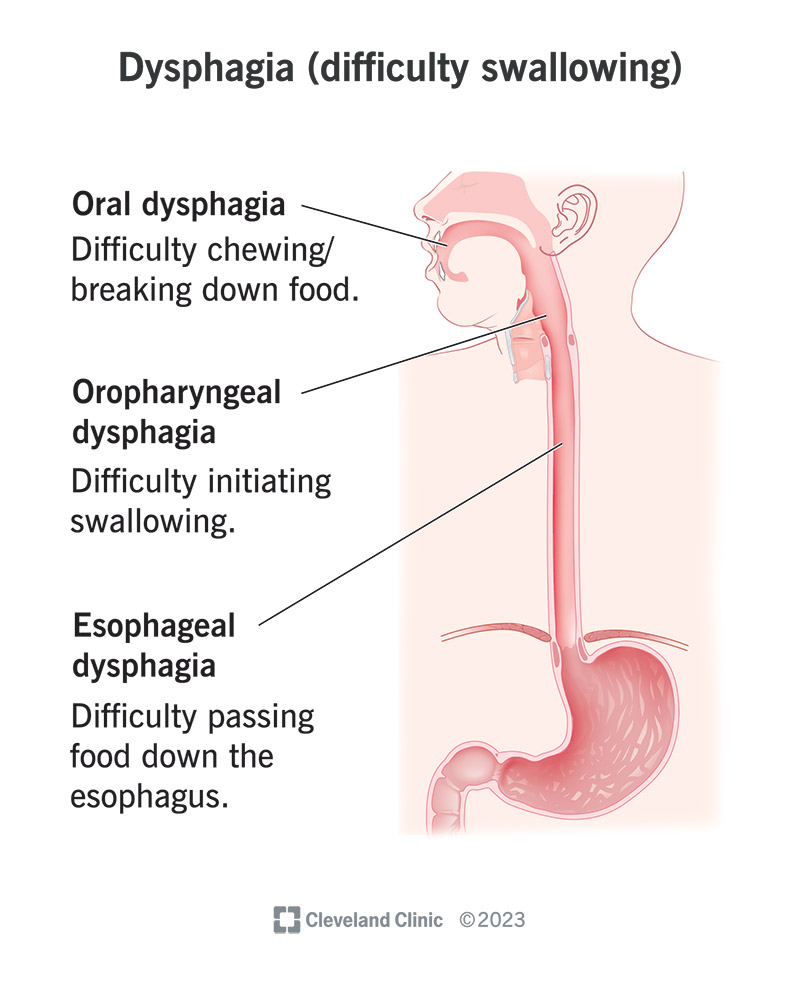
- Difficulty swallowing certain foods
When conservative treatments (like CPAP or lifestyle tweaks) fail, many ENT specialists suggest a uvulectomy as a focused way to open the airway. According to , a partial uvulectomy can reduce snoring intensity by up to 60% in some patients.
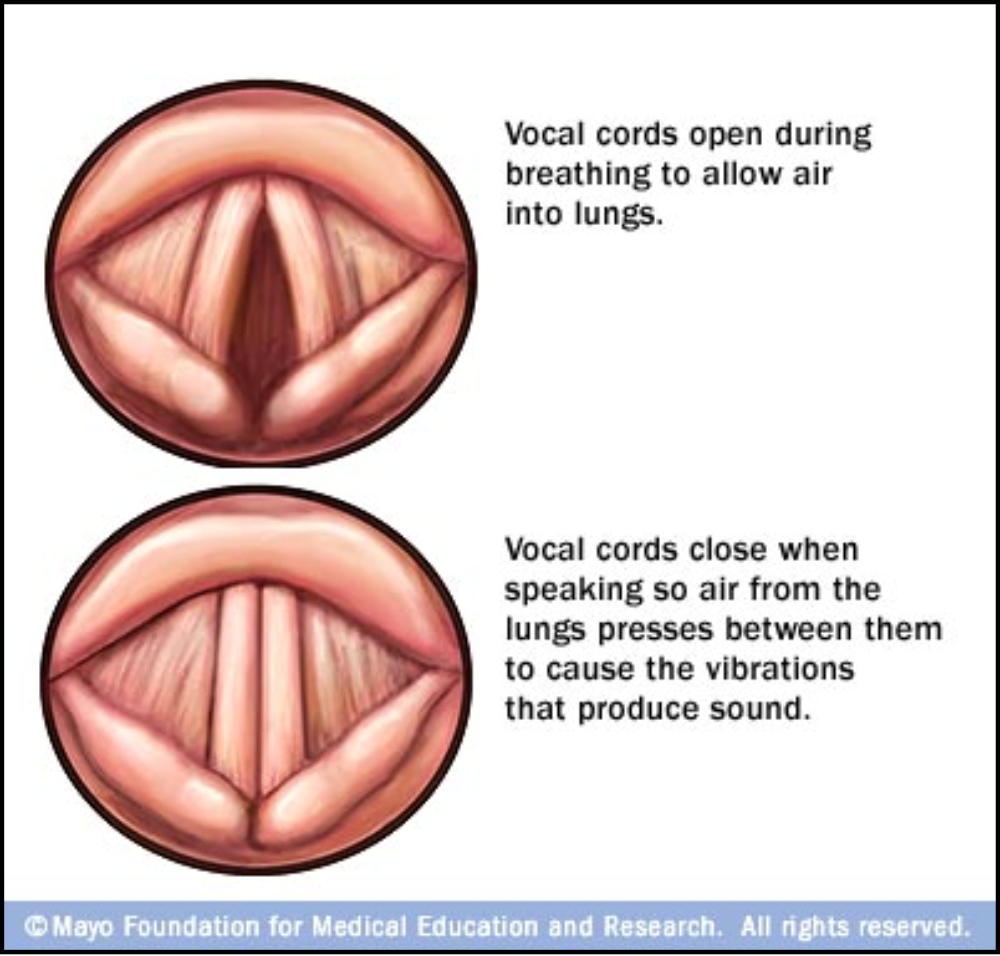
How does a shorter uvula improve breathing?
Picture your airway as a hallway. The uvula hangs like a lowhanging curtain; trim it, and the hallway widens. With more space, air flows more freely during sleep, lowering the chances of vibrations (snoring) and brief pauses (apneas). A simple diagram from the illustrates this nicely.
Partial vs. Total Uvulectomy Quick Comparison
| Aspect | Partial | Total |
|---|---|---|
| Amount removed | Middle third or less | Entire uvula |
| Typical recovery | 47 days | 710 days |
| Voice impact | Minimal | Possible deeper tone |
| Regrowth risk | Low | Very low |
Procedure Overview Steps
How is the surgery performed?
Most surgeons use one of three techniques:
- Laser precise, minimal bleeding.
- Electrocautery uses heat to seal vessels.
- Radiofrequency a newer, tissuesparing method.
All three are typically done in an ENT office with local anesthesia (a spray or injection) and take about 515 minutes. The surgeon lifts the uvula, applies the chosen tool, and trims the targeted portion.
Local or general anesthesia?
For most adults, a topical anesthetic spray plus a shortacting sedative is enough. Children or anxious patients may receive deeper sedation or even general anesthesia, though thats less common.
Whats the duration?
The actual cutting takes under a minute, but you should plan for 3045 minutes total to include prep, the brief procedure, and postop observations.
Preop Checklist
- Confirm youve stopped blood thinners (aspirin, ibuprofen) 4872 hrs prior.
- Fast for at least 6 hours if using any sedation.
- Arrange a ride homedont drive yourself.
- Bring a list of current medications for the surgeon.
Postop Immediate Care
After the uvula is trimmed, youll likely feel a sore throat, a bit of swelling, and maybe a few drops of blood. Thats normal. Most clinicians prescribe a mild pain reliever and recommend cool liquids for the first 24hours.
Immediate Side Effects
What should you expect in the first couple of days?
Typical shortterm side effects include:
- Sore throat like youve just gargled a lemon.
- Mild bleeding a few spots of blood on your spit.
- Swollen uvula area it may look puffier before it calms down.
- Increased gag reflex the throat can be extra sensitive for a few days.
When is it time to call a doctor?
If you notice any of these red flags, reach out ASAP:
- Heavy bleeding that wont stop after applying gentle pressure.
- Fever over 101F (38.3C).
- Severe pain thats not relieved by OTC meds.
- Difficulty breathing or swallowing large amounts of liquid.
Quick FAQ for Featured Snippet
What are the shortterm side effects of uvula removal? Expect a sore throat, mild swelling, occasional light bleeding, and a temporary increase in gag reflex. Most symptoms ease within a week.
Realworld anecdote
John, a 42yearold teacher, told me his throat felt like a sandpaper brush for three days after his procedure. I could barely swallow water without a wince, he said, but by day four I was back to grading papers and drinking coffee. Stories like his remind us that discomfort is real but shortlived.
LongTerm Side Effects
Can the uvula grow back?
Partial regrowth is possibletiny tissue fragments may stitch themselves back together over months, but a fullsize uvula returning is extremely rare. Studies in show less than 2% of patients notice any regrowth that causes symptoms.
Will my voice change?
Some people report a subtle shiftoften a slightly deeper tone or a tiny nasal quality. This is usually due to the altered shape of the soft palate. Professional singers sometimes notice the change more acutely, so a preop voice evaluation can help set expectations.
How does it affect the gag reflex?
Right after surgery, the gag reflex can feel hypersensitive because the throats protective mechanisms are on alert. Most folks report it normalizes within two weeks as the tissue heals.
Rare complications
While uncommon, a few longterm risks exist:
- Persistent pain or ulceration.
- Infection requiring antibiotics.
- Scarring that slightly narrows the airway (rare).
- Unintended voice alterations that dont improve with therapy.
Frequency of LongTerm Effects
| Effect | Incidence |
|---|---|
| Regrowth | 12% |
| Voice change | 510% |
| Prolonged gag reflex | 3% |
| Infection | 1% |
Recovery & Lifestyle
Typical recovery timeline
Days 13: Sore throat, softfood diet, plenty of fluids.
Week 1: Swelling subsides, you can introduce gentle solids.
Weeks 24: Full voice and swallowing function return; most people are back to normal activities.
Diet and hydration tips
- Start with cool broths, yogurt, applesauce, and smoothies.
- Avoid spicy, acidic, or crunchy foods for the first week.
- Stay hydratedwarm teas with honey can soothe.
Pain and swelling management
Overthecounter pain relievers like ibuprofen (if not contraindicated) work well. Some clinicians prescribe a short course of steroids to reduce swellingask your surgeon if thats appropriate for you.
When can you resume normal activities?
Most patients can return to desk work after 23 days and light exercise after a week. If youre a singer, public speaker, or athlete, give yourself at least two weeks before heavy vocal or cardio stresses.
7Day PostOp Checklist
| Day | What to Do |
|---|---|
| 1 | Stick to liquids, use pain reliever, monitor bleeding. |
| 23 | Introduce soft foods, continue hydration, avoid shouting. |
| 45 | Gradually add easychew items, gentle vocal warmups. |
| 67 | Check in with surgeon if any concerns, resume light activity. |
Uvula Removal Cost
Typical price range in the United States
The outofpocket cost can vary widely depending on geography, facility, and whether you have insurance. Roughly:
- Officebased laser uvulectomy: $600$1,200
- Hospitalbased procedure (often with general anesthesia): $1,500$2,500
These figures come from pricing info posted by the and reflect typical charges in 20232024.
Whats included in the price?
Usually the fee covers:
- Surgeons professional fee
- Facility or office use
- Local anesthesia or sedation
- Postop medication prescriptions
Some clinics may charge extra for lab work, preop imaging, or followup visits.
Insurance and billing tips
Most insurers classify uvulectomy under CPT codes 42130 (partial) or 42140 (total). Before scheduling, call your insurer and ask:
- Is the procedure covered for sleepapnea or chronic throat issues?
- What is the patient responsibility after copay?
- Do you need a prior authorization?
CostComparison Chart
| Setting | Typical Cost | Insurance Coverage | Recovery Time |
|---|---|---|---|
| Office (laser) | $600$1,200 | Often covered with diagnosis code | 47 days |
| Hospital (general) | $1,500$2,500 | May need preauthorization | 710 days |
Alternative Treatment Options
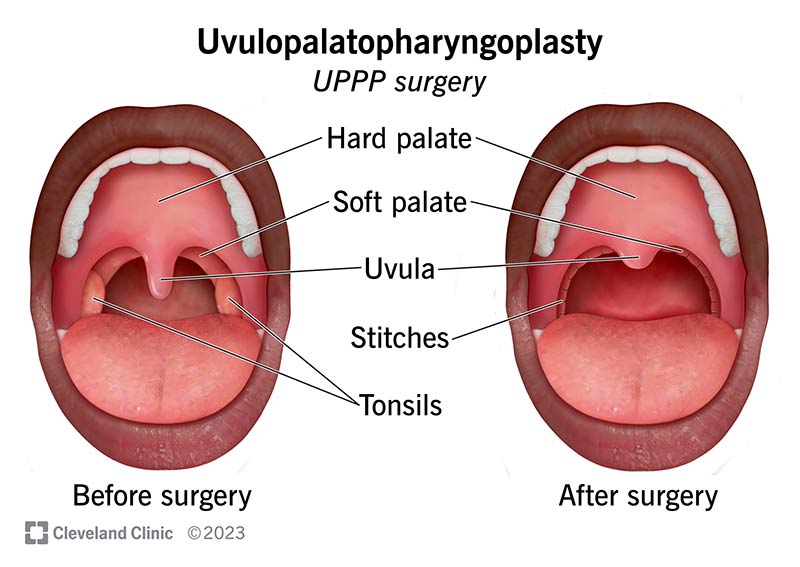
Uvulopalatopharyngoplasty (UPPP)
UPPP is a more extensive surgery that trims excess tissue from the soft palate, tonsils, and uvula. Its usually reserved for severe sleep apnea when a simple uvulectomy isnt enough. According to the , UPPP can reduce apneahypopnea index by up to 85% but carries higher risk of pain and longer recovery.
Nonsurgical alternatives
- Continuous Positive Airway Pressure (CPAP) the gold standard for moderatetosevere sleep apnea.
- Oral appliance therapy custommade mouthguards that advance the lower jaw.
- Weight management and positional therapy losing excess weight and sleeping on the side can lessen snoring.
Many patients also explore adjunctive wellness approaches to reduce overall sleep disturbance. For people who experience ringing or head noise alongside sleep issues, techniques like tinnitus meditation can sometimes help reduce stress and improve sleep quality when used with medical treatments.
When to combine with tonsillectomy?
If you have enlarged tonsils in addition to an oversized uvula, many surgeons recommend a combined tonsillectomy and uvulectomy. This doublehit approach often yields the biggest reduction in airway obstruction.
DecisionMaking Flowchart (text version)
1. Do you have confirmed sleep apnea or chronic snoring?
2. Have you tried CPAP or oral devices?
3. Is the uvula visibly enlarged or inflamed?
4. Consult a boardcertified ENT; discuss uvulectomy vs. UPPP vs. nonsurgical options.
5. Choose the path that balances effectiveness, cost, and recovery time for your lifestyle.
Patient Case Studies
Case #1 SleepApnea Relief
Sarah, a 35yearold graphic designer, suffered from moderate obstructive sleep apnea despite a diligent CPAP routine. After a thorough assessment, her ENT performed a partial laser uvulectomy. Six weeks later, her apneahypopnea index dropped from 18 to 6, and she reported feeling refreshed for the first time in years. Sarahs voice stayed the same, and she resumed yoga without the nightly CPAP mask.
Case #2 Unexpected Voice Change
Mike, a 28yearold karaoke enthusiast, chose a total uvulectomy to eliminate chronic throat irritation. Postop, his voice deepened by about two semitonesa change he liked for rock songs but found unsettling for spoken presentations. A speechlanguage pathologist helped him adjust his technique, and within two months his voice settled into a comfortable middle ground.
Expert commentary
Both Dr. Laura Mendes (ENT, Jefferson Health) and Dr. Alan Rogers (voice specialist) stress that individual anatomy dictates outcomes. A tiny shift in softpalate tension can translate to a noticeable voice change, says Dr. Mendes, so we always counsel patients to expect mild variations.
Living Without a Uvula
Most people adapt quickly. The uvulas primary roleshelping with speech articulation, gag reflex, and producing certain guttural soundscan be compensated by the surrounding throat muscles. Over time, youll likely forget that a piece of tissue is missing. Staying hydrated, practicing gentle vocal exercises, and keeping followup appointments ensures a smooth transition.
If youve been scared by the idea of living without a uvula, remember that thousands undergo the procedure each year with minimal longterm issues. The key is informed decisionmaking, open communication with your surgeon, and realistic expectations.
Conclusion
Uvula removal can be a gamechanger for snorers, sleepapnea patients, and those plagued by chronic throat irritation. The procedure is quick, recovery is usually swift, and most side effects fade within weeks. Yet, like any surgery, there are tradeoffspossible voice changes, a brief gagreflex spike, and a cost that varies by setting.
Take the time to weigh the benefits against the risks, check your insurance coverage, and consider alternatives such as CPAP or UPPP. Talking to a boardcertified ENT, reading real patient stories, and asking the right questions will empower you to make the best choice for your health and peace of mind.
Whats your experience with uvula removal, or are you still on the fence? Share your thoughts below, or reach out if you have more questions. Your voice mattersboth literally and figuratively!
FAQs
What is uvula removal and why is it performed?
Uvula removal (uvulectomy) is a short office‑based surgery that trims or eliminates the uvula to reduce snoring, mild‑to‑moderate obstructive sleep apnea, chronic throat irritation, or recurrent infections when other treatments fail.
How long does recovery take after a uvula removal?
Most people experience sore throat and mild swelling for the first 3‑5 days. Soft foods are recommended for the first week, and normal activities are usually resumed within 7‑10 days. Full healing of the tissue may take up to 2‑4 weeks.
What are the common risks or complications?
Short‑term risks include light bleeding, sore throat, and a temporarily heightened gag reflex. Long‑term complications are rare but can involve voice changes, infection, scar tissue, or minimal regrowth of the uvula (≈1‑2% of cases).
Will my voice change after the surgery?
Some patients notice a subtle deepening or slight nasal quality to their voice due to altered soft‑palate dynamics. The change is usually mild (5‑10% of patients) and often resolves with voice therapy if bothersome.
How much does uvula removal typically cost and is it covered by insurance?
Office‑based laser uvulectomy ranges from $600‑$1,200, while hospital‑based procedures can cost $1,500‑$2,500. Most insurers cover the surgery when it’s medically indicated (CPT 42130/42140), but prior authorization and a diagnosis code are usually required.