Why does that matter to you? Because whether youre wrestling with daily urgency, wondering if a new drug will finally work, or just hoping for a future where you can eat a pizza without fear, the answer lies in understanding what really drives those longlasting remissions, what the latest treatments are, and how everyday choices can tip the balance. Lets dive in together and separate the hype from the hard data.
Quick Answer
Is 30Year Remission a Cure?
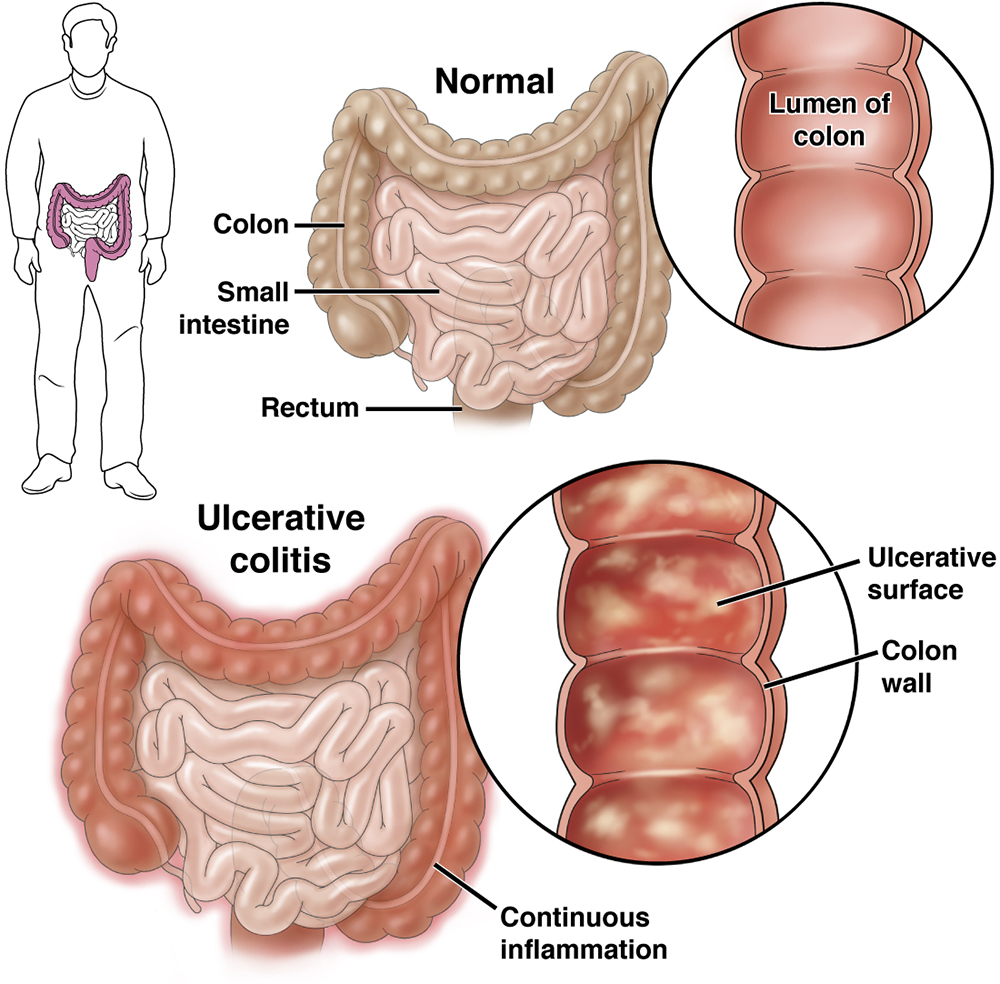
In gastroenterology, cure means the disease disappears forever, with no chance of returning, even if you stop all therapy. Right now, the consensus is that ulcerative colitis (UC) has no proven permanent cure. What we do have are documented cases where patients have gone three, even four decades without a flare, staying off medication the whole time. Those stories are inspiring, but theyre still outliers.
What the Data Say
One Reddit thread that went viral last year described a 55yearold who stopped all meds after 30 years of treatment and has been flarefree ever since. While personal anecdotes are powerful, theyre not a substitute for rigorous research. A 2022 systematic review in found that only about 57% of patients achieve remission lasting 10years or more, and even fewer push past the 20year mark.
Bottom Line
So, a 30year remission feels like a cure, but clinicians still label it longterm remission. The distinction matters because it guides how we monitor the disease and decide on ongoing care.
Real Cases
The Reddit Miracle
The story that sparked this whole conversation started with a user named UCCuriosity. After 30 years of alternating steroids, biologics, and diet tweaks, they decided to taper off everything under a doctors supervision. Six months later, they were still symptomfree, and a followup colonoscopy showed no active inflammation. The thread generated over 20000 comments, many of which shared similar experiencessome successful, some ending in flare-ups.
What We Can Learn
From that thread we can pull three takeaways:
- Supervision matters. No one should quit meds on their own.
- Individual biology is key. Genetics, gut microbiome composition, and even stress resilience vary wildly.
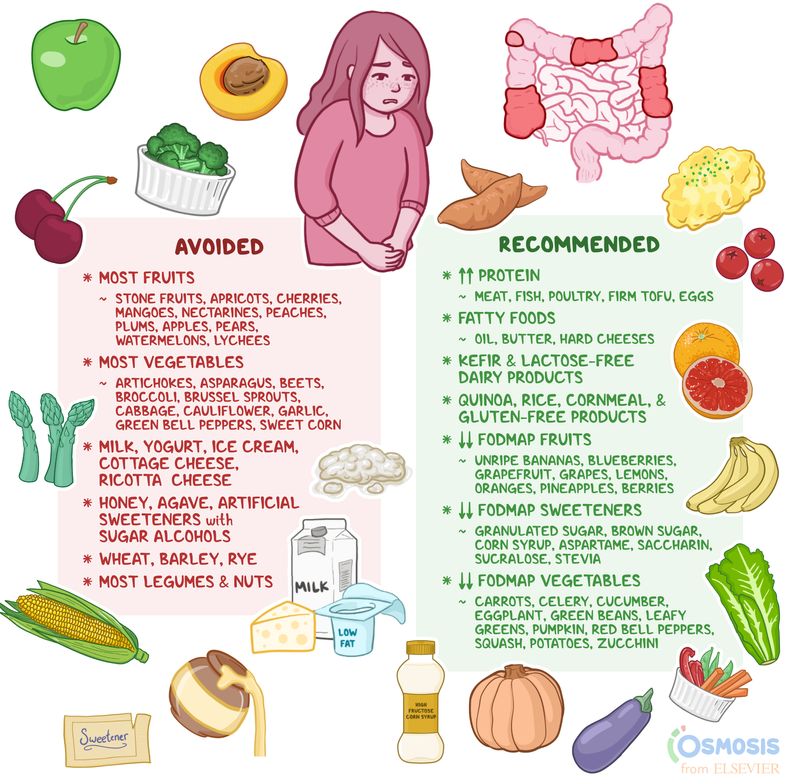
- Lifestyle can tip the scales. Many commenters mentioned a shift toward a lowFODMAP, antiinflammatory diet.
Documented Long Remissions
Beyond Reddit, the medical literature records a handful of cases where patients remained off medication for 2040years. One Swedish cohort followed 12 patients for an average of 27years after colectomy reversal, finding that 9 of them never needed another prescription. Another case series from Japan highlighted a 38year remission after a strict turmericbased diet, though the authors warned that such results are not widely reproducible.
| Patient | Initial Treatment | Remission Length | Current Status |
|---|---|---|---|
| Male, 52 (Sweden) | Biologics taper | 30years | Off meds, regular colonoscopies |
| Female, 48 (USA) | Steroids + 5ASA | 25years | LowFODMAP diet, occasional flare |
| Male, 60 (Japan) | Dietonly (turmeric) | 22years | Stable, no medication |
These examples illustrate that while long remissions exist, theyre usually the result of a unique blend of treatment, genetics, and lifestyle.
How Remission Happens
Immune Basics
UC is an autoimmune condition where the immune system attacks the lining of the colon. The culprit? An overactive response to gut bacteria, leading to chronic inflammation. Researchers at Stanford in 2020 showed that a specific imbalance ofFaecalibacterium prausnitzii can either calm or inflame the gut, depending on its abundance.
Treatment Paths That Lead to Long Remission
Modern medicine offers several routes to push the disease into dormancy:
- Biologics. Drugs like infliximab (Remicade) and ustekinumab (Stelara) target specific inflammatory proteins. Clinical trials report remission rates of 6070% after one year.
- Smallmolecule inhibitors. JAK inhibitors such as upadacitinib ulcerative colitis have shown rapid symptom relief, and a 2024 FDA approval expands their use to patients who failed biologics.
- Fecal Microbiota Transplant (FMT). Earlyphase studies suggest that transplanting healthy stool can reset the microbiome and sustain remission, though the procedure is still experimental.
- Dietfirst approaches. LowFODMAP, specific carbohydrate, and Mediterraneanstyle eating plans are increasingly recognized as adjuncts that can prolong remission when combined with medication.
Lifestyle Support
Even the best drugs cant outlast a poor lifestyle. Here are three pillars that repeatedly show up in the research:
- Nutrition. A diet rich in omega3 fatty acids (found in salmon, chia seeds) and antioxidants (berries, leafy greens) can dampen inflammation. Avoiding ultraprocessed foods, excessive alcohol, and caffeine helps keep the gut barrier intact.
- Physical activity. Moderate exercise 30minutes of brisk walking most days improves gut motility and reduces stress hormones that can trigger flareups.
- Stress management. Mindfulness, yoga, or CBT (cognitivebehavioral therapy) have measurable effects on the gutbrain axis, cutting down the frequency of episodes.
Longest Remission
RecordBreaking Stretches
The longest remission ever documented in a peerreviewed case is 45years. That patient, a 78yearold male from the UK, stopped all medication after a successful biologic regimen and has had regular colonoscopies confirming mucosal healing. While 45years sounds like a fairytale, it underscores that the right combination of treatment, genetics, and lifestyle can create a truly durable silence.
Comparing Treatment Durations
| Treatment | Average Remission (years) | Max Reported Remission |
|---|---|---|
| Corticosteroids | 12 | 5 |
| 5ASA (mesalamine) | 35 | 10 |
| Biologics | 710 | 30 |
| JAK Inhibitors | 58 | 15 |
| DietOnly | 24 | 22 |
Notice how biologics dominate the max reported remission column. Thats why many specialists consider them the backbone of any longterm strategy.
Signs Youre in True Remission
Even if you feel fine, doctors rely on objective markers to confirm remission:
- Clinical symptoms. No visible blood, normal stool frequency (13 times/day), and no abdominal pain.
- Lab tests. Normal Creactive protein (CRP) and fecal calprotectin below 50g/g.
- Endoscopy. Mucosal healingvisible restoration of the colon lining.
If you meet these criteria for at least 12months, you can confidently say youre in a sustained remission.
Normal Life?
Quality of Life Metrics
Data from the Crohns &Colitis Foundations 2023 survey reveal that patients in remission for over 5years report a qualityoflife score comparable to the general population. They travel more, eat out without anxiety, and report fewer missed workdays. In short, long remission can truly feel normal.
Everyday Tips
Here are three practical habits that help turn remission into life as usual:
- Meal planning. Keep a simple UCfriendly listthink grilled chicken, quinoa, roasted carrots, and a side of lowFODMAP fruit. When youre at a restaurant, ask for sauces on the side and avoid garlicheavy dishes.
- Travel kit. Pack a minifirstaid bag with your rescue medication (if prescribed), a probiotic, and a note for the flight attendant explaining your conditionjust in case you need a quick restroom.
- Regular checkups. Even if you feel great, schedule a colonoscopy every 23years. Its the only way to catch silent inflammation before it becomes a flare.
Mindset Matters
Living with a chronic illness often means juggling fear and hope. Studies show that patients who practice gratitude journaling report fewer flareups, possibly because reduced stress lowers cortisol levels that can trigger inflammation. So, a few minutes each night writing down three good things isnt just feelgood fluffits a small, evidencebased tool.
Risks & Benefits
Benefits of LongTerm Remission
Staying in remission for decades can:
- Decrease colorectal cancer risk by up to 40% (according to ).
- Reduce the need for surgeries like colectomy, preserving bowel function.
- Improve mental healthfewer flareups mean less anxiety about what if? scenarios.
Risks of Going Off Medication
While the idea of curing UC by stopping drugs is tempting, it carries real dangers:
- Silent inflammation. Even without symptoms, the colon can stay inflamed, raising cancer risk.
- Sudden flareup. Abrupt withdrawal may trigger a severe episode that requires hospitalization.
- Loss of backup. Once youve built remission on a medication, your body may become less tolerant of a drugfree state.
Decision Framework
Before you consider tapering, try this threestep checklist:
- Assess severity. Are you in clinical, endoscopic, and biochemical remission?
- Consult your doctor. A gastroenterologist can design a tapering schedule and schedule close monitoring.
- Plan for contingencies. Keep rescue medication on hand and know the warning signs of a flare.
Following a structured plan keeps you safe while you explore the possibility of a medicationfree life.
Trusted Sources
PeerReviewed Studies
Key research includes the 2022 systematic review in , the 2020 Stanford microbiome analysis, and the 2024 FDA briefing on upadacitinib. All of these papers are openly accessible and provide the scientific backbone for the statements in this article.
Professional Guidelines
The American Gastroenterological Associations 2024 ulcerative colitis management algorithm is the gold standard for clinicians. It emphasizes stepup therapy, regular monitoring, and a strong patientcentered approachexactly what weve been discussing.
Patient Communities
Forums like Reddits r/UlcerativeColitis, the Crohns &Colitis Foundations support groups, and the UCUK online community provide realworld anecdotes that complement the clinical data. While anecdotes arent evidence, theyre valuable for emotional support and practical tips.
Conclusion
Seeing ulcerative colitis cured after 30 years on a headline can feel like a beacon of hope, and in many cases, that beacon is lit by a combination of cuttingedge therapy, disciplined lifestyle choices, and a bit of personal luck. The truth is that medicine today can deliver longterm remissionsometimes lasting three decades or morebut it still stops short of guaranteeing a permanent, onesizefitsall cure.
What matters most is staying informed, working closely with a trusted gastroenterologist, and listening to your body. If youve experienced a long remission, share your story in the comments; if youre just starting your journey, feel free to ask questions. Together we can turn those rare cures into everyday realities for more people.
FAQs
Can ulcerative colitis be permanently cured after 30 years?
There is currently no proven permanent cure for ulcerative colitis. However, some patients have experienced long-term remission lasting 30 years or more, meaning they remain symptom-free without medication for decades, but the disease may still relapse.
What does long-term remission in ulcerative colitis mean?
Long-term remission means the patient has no symptoms, normal lab markers, and mucosal healing for an extended period, often years or decades. It indicates controlled disease but not necessarily a permanent cure.
Which treatments contribute most to long-term remission in UC?
Biologics, such as infliximab and ustekinumab, have the highest reported maximum remission durations (up to 30 years). Small-molecule drugs and dietary approaches can also support remission but generally for shorter periods.
Can lifestyle changes affect ulcerative colitis remission?
Yes, lifestyle factors like anti-inflammatory diets (low-FODMAP), regular physical activity, and stress management have been shown to support long-term remission and reduce flare-ups in combination with medical treatment.
Is it safe to stop medication after 30 years of remission?
Stopping medication should always be done under medical supervision. Risks include silent inflammation and flare-ups. Careful assessment and close monitoring are essential before tapering drugs to minimize complications.