You're probably scrolling through a sea of medical jargon, wondering which prostate operation actually gives you relief without turning your life upsidedown. Lets cut to the chase: there are several solid options, each with its own pros, cons, and recovery story. In the next few minutes, I'll walk you through every major type, explain how long the procedures usually take, and share what the data say about life after surgery. Think of this as a friendly coffeechat where I've done the homework so you don't have to.
Why Surgery?
When is surgery really needed?
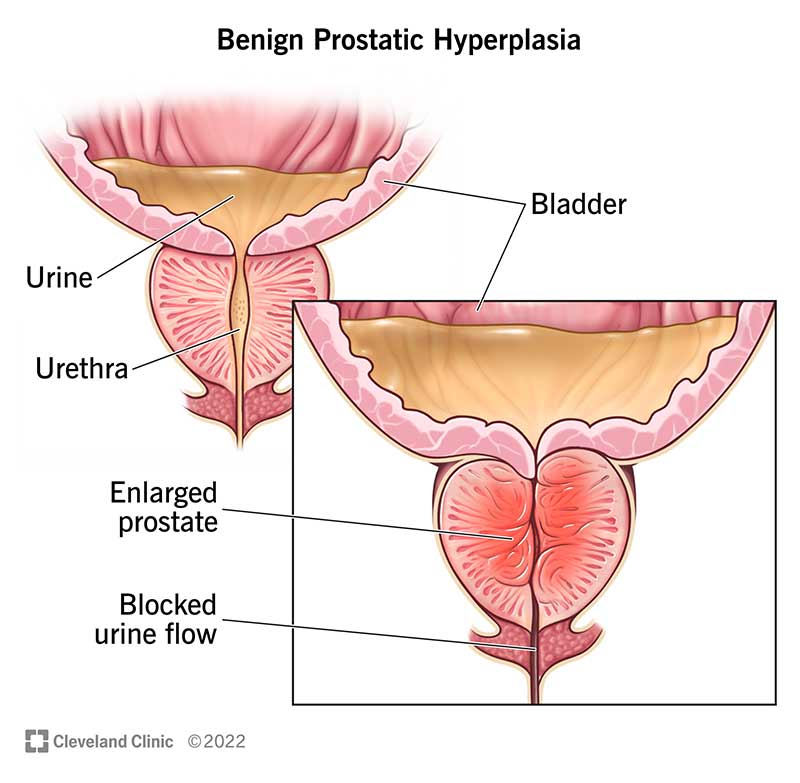
Most men consider surgery because medication isn't enough to tame a stubbornly enlarged prostate (BPH) or to remove a localized prostate cancer. Typical red flags include:
- Persistent urinary retention that forces you to catheterize.
- Frequent urinary tract infections that keep you in the doctor's office.
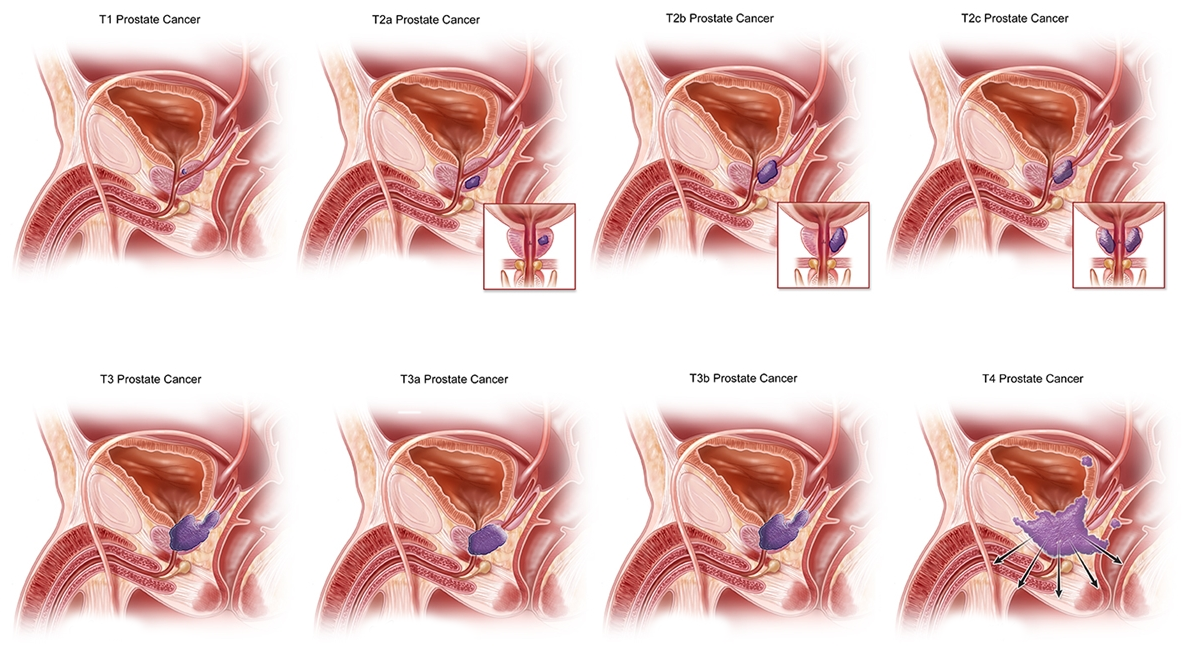
- A Gleason score of 7 or higher on a biopsy, indicating cancer that's likely to grow.
Can I avoid the knife?
Sure. For many, alpha-blockers, 5-alpha-reductase inhibitors, or simply watchful waiting can keep symptoms at bay. The key is a candid talk with a board-certified urologist who can weigh your PSA trends, prostate volume, and overall health.
Four Prostatectomy Types
When surgery is the clear path, urologists generally talk about four core prostatectomy techniques. Below is a quick-glance table that answers what are the three types of prostate surgery? and even the longer version, how long does prostate surgery take?
| Procedure | Typical Indication | Invasiveness | Estimated OR Time | Key Risks |
|---|---|---|---|---|
| Open Radical Prostatectomy | Localized cancer | Full abdominal incision | 24 hrs | Blood loss, incontinence, erectile dysfunction |
| Laparoscopic Radical Prostatectomy | Cancer, prefers smaller scars | Multiple small ports | 23 hrs | Similar to open, but less bleeding |
| Robot-Assisted Laparoscopic (RALP) | Most common for cancer today | Robotic arms through ports | 23 hrs | Learning-curve dependent complications |
| Simple (Subtotal) Prostatectomy | Severe BPH with obstruction | Open or laparoscopic | 12 hrs | Bleeding, irritative urinary symptoms |
Open Radical Prostatectomy the classic
This is the old-school approach where the surgeon makes a sizeable incision to directly visualize the prostate and surrounding tissue. It's rarely the first choice unless the cancer is very large or the hospital lacks robotic tech. According to long-term series, cancer control rates are excellent, but the tradeoff can be a longer hospital stay.
Laparoscopic & Robot-Assisted the high-tech twins
Both use tiny incisions, but the robot adds a 3D view and wristed instruments that can mimic a surgeon's hand movements with millimetre precision. Patients love the smaller scars and often go home within 24 hours. A study showed that RALP patients reported less postoperative pain than those who had open surgery.
Simple Prostatectomy for an enlarged gland
If the primary problem is BPH rather than cancer, a simple prostatectomy removes only the obstructive tissue, leaving the capsule intact. Recovery is usually a bit quicker than radical cancer surgery, but you'll still have a Foley catheter for about a week.
Minimally Invasive Options
Transurethral Resection of the Prostate (TURP)
TURP remains the gold standard for moderate-to-severe BPH. The surgeon slides a resectoscope through your urethra and chips away excess tissue. The whole procedure takes about 4590 minutes, answering the how long does prostate surgery take? query for many. You'll likely leave the OR with a catheter for 12 days and notice a dramatic drop in nighttime trips.
Transurethral Incision of the Prostate (TUIP)
When the prostate isn't huge (usually under 30 cm), a few strategic cuts can relieve pressure without removing much tissue. The operation is swiftoften under an hourand the recovery is gently smooth.
HoLEP Holmium Laser Enucleation
HoLEP is the laser-powered cousin of TURP. A high-energy holmium laser precisely separates the enlarged lobe from the prostate capsule, allowing the surgeon to pull it out in one piece. It works for prostates of any size, which is why many ask, what are the three types of prostate surgery? and add HoLEP to the list.
GreenLight Laser Photovaporization
Think of it as a laser that vaporizes excess tissue without cutting. It's an outpatient procedure for many, meaning you might go home the same day with just a short-term catheter.
Decision Tree pick your path
Here's a quick mental flowchart:
If your prostate is under 40 g consider TUIP or GreenLight.
If it's 4080 g TURP or HoLEP are strong contenders.
If it's over 80 g HoLEP or open/simple prostatectomy often work best.
Choosing the Best Option
What matters most to you?
Ultimately, the best surgery for enlarged prostate is the one that aligns with your life goals. Ask yourself:
- Do I want the fastest return to work?
- How important is preserving sexual function?
- Am I comfortable with a longer hospital stay for potentially better cancer control?
Questions to fire at your surgeon
Show up armed with these:
- What's my chance of keeping potency after this procedure?
- Will I need a catheter, and for how long?
- How many of these surgeries have you performed in the past year? (Surgeon volume matters.)
Quick-look pros & cons grid
| Option | Pros | Cons |
|---|---|---|
| Open Radical | Highest cancer control for large tumors | Longer recovery, more blood loss |
| Robot-Assisted | Smaller incisions, less pain | Depends on surgeon's experience |
| TURP | Proven, fast, affordable | Risk of retrograde ejaculation |
| HoLEP | Works for any prostate size | Longer learning curve for surgeon |
Life Expectancy Outlook
Surviving cancer after removal
When the prostate is removed for localized cancer, the five-year survival rate tops 95% in most large registries. In real-world terms, most men live a full, active life after surgery, provided the cancer hasn't spread beyond the gland.
Quality of life after surgery
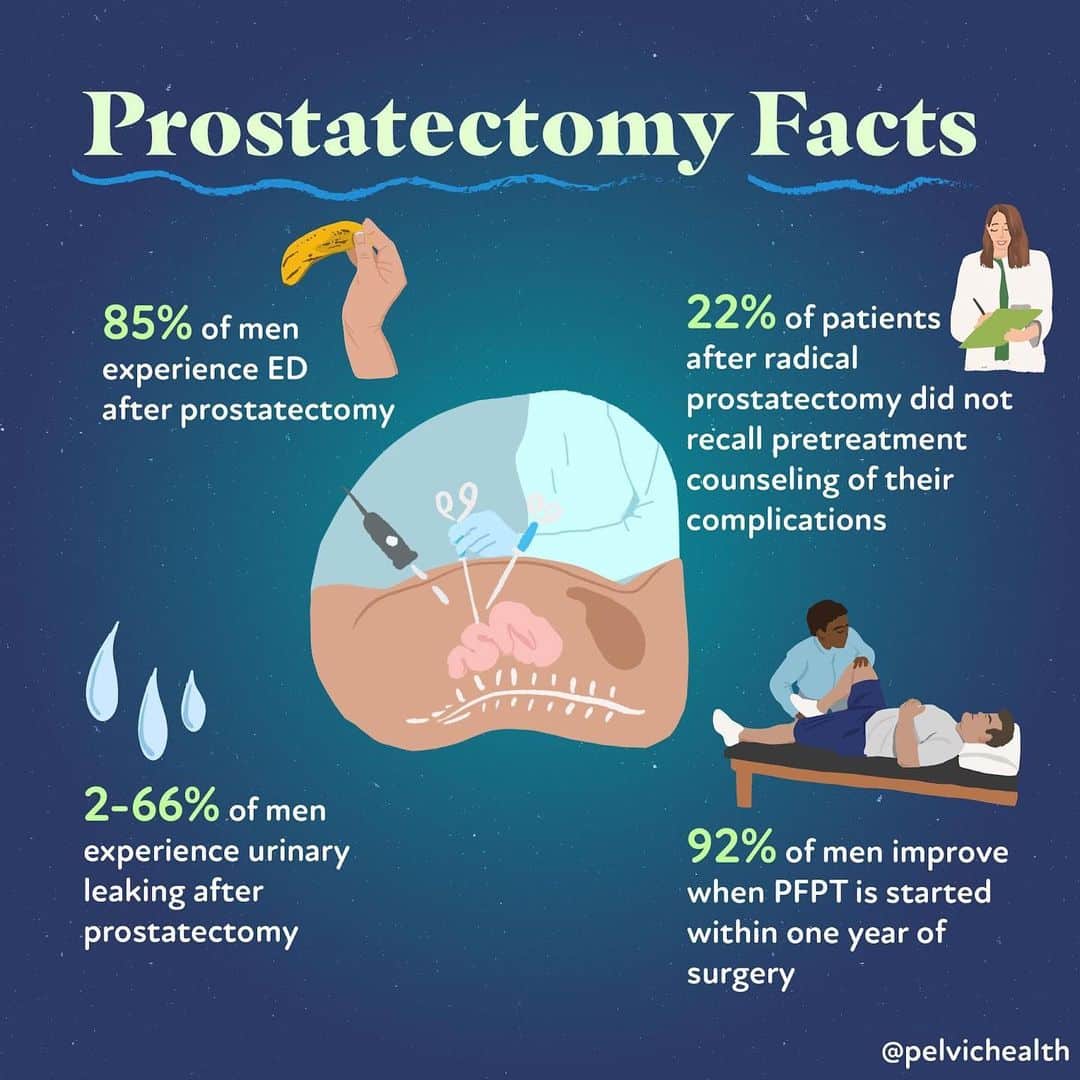
Studies indicate that about 20% of men experience temporary urinary incontinence, but most regain control within six months. Erectile function can be trickier; nerve-sparing techniques improve odds, yet 3040% may need medication or devices afterward.
When surgery feels like a nightmare
There are stories of prostate surgery ruined my life, and they're real. Those cases often involve complications, poor postop rehab, or a mismatch between patient expectations and surgical reality. That's why a balanced, transparent discussion up front can keep the drama out of your recovery.
Balancing Benefits & Risks
The upside
- Immediate relief from urinary obstruction.
- Potential cure for organ-confined prostate cancer.
- Improved sleep and daytime energy once nocturia drops.
The downsides
- Risk of urinary incontinence (roughly 1020%).
- Erectile dysfunction (up to 40% without nerve-sparing).
- Infection, blood clots, or anesthesia reactionsalways a small statistical chance.
When to walk away
If you have low-grade cancer on active surveillance, severe heart disease, or a life expectancy under 57 years, the risks of surgery may outweigh the benefits. In those cases, watchful waiting or medication can be a sensible route.
Preparing & Recovering
Preop checklist
- Complete blood work and PSA test.
- Stop blood thinners as directed.
- Talk to anesthesia about any allergies.
- Arrange help at home for the first 48 hours.
Day-of-surgery snapshot
Most minimally invasive procedures let you walk into the OR in the morning and head home by late afternoon. You'll have a small catheter attached, a brief monitoring period, and a nurse who will explain how to manage the catheter at home.
Recovery timeline
| Time Frame | Typical Milestones |
|---|---|
| Day 02 | Catheter care, light walking, pain meds. |
| Week 12 | Catheter removal (if applicable), start gentle pelvic floor exercises. |
| Month 13 | Gradual return to work, monitor urinary patterns. |
| Month 36 | Many men see continuing improvement in continence and sexual function. |
Tips to speed healing
- Stay hydrated (but avoid caffeine if it irritates the bladder).
- Do Kegel exercises twice dailystrengthening the pelvic floor can cut incontinence risk.
- Follow a high-protein diet to support tissue repair.
- Keep follow-up appointments; early detection of any complication makes all the difference.
Conclusion
There's no one-size-fits-all answer when it comes to the types of prostate surgery. Whether you lean toward an open radical prostatectomy, a robot-assisted lap, or a laser-driven HoLEP, the decision should balance the expected benefit with the realistic risk profilealways in partnership with an experienced urologist. Armed with the information above, you're better prepared to ask the right questions, set clear expectations, and move forward with confidence. If you've been through any of these procedures, or if you're just starting to explore your options, share your story in the commentsyour experience could be the lighthouse for someone else navigating the same waters.
FAQs
What are the main types of prostate surgery?
The primary options include open radical prostatectomy, laparoscopic radical prostatectomy, robot‑assisted laparoscopic prostatectomy, simple (subtotal) prostatectomy for BPH, TURP, TUIP, HoLEP, and GreenLight laser photovaporization.
How long does each prostate surgery typically take?
Open radical prostatectomy: 2–4 hours; laparoscopic and robot‑assisted: 2–3 hours; simple prostatectomy: 1–2 hours; TURP: 45–90 minutes; TUIP and most laser procedures are usually under an hour.
What are the recovery times and expectations after prostate surgery?
Hospital stay ranges from same‑day discharge (laser/TURP) to 2–4 days (open surgery). Catheter removal occurs 1–2 weeks post‑op. Most men return to light activities within 2–4 weeks and full work duties by 6–8 weeks, depending on the procedure.
What are the risks of urinary incontinence and erectile dysfunction after prostate surgery?
Incontinence affects about 10‑20 % of men, often improving within six months. Erectile dysfunction can occur in up to 40 % without nerve‑sparing techniques; nerve‑sparing approaches reduce this risk but do not eliminate it.
How should I choose between robotic, laparoscopic, and laser prostate procedures?
Consider tumor size, prostate volume, surgeon experience, desired recovery speed, and personal priorities such as preserving sexual function. Discuss these factors with a board‑certified urologist to match the technique to your health goals.