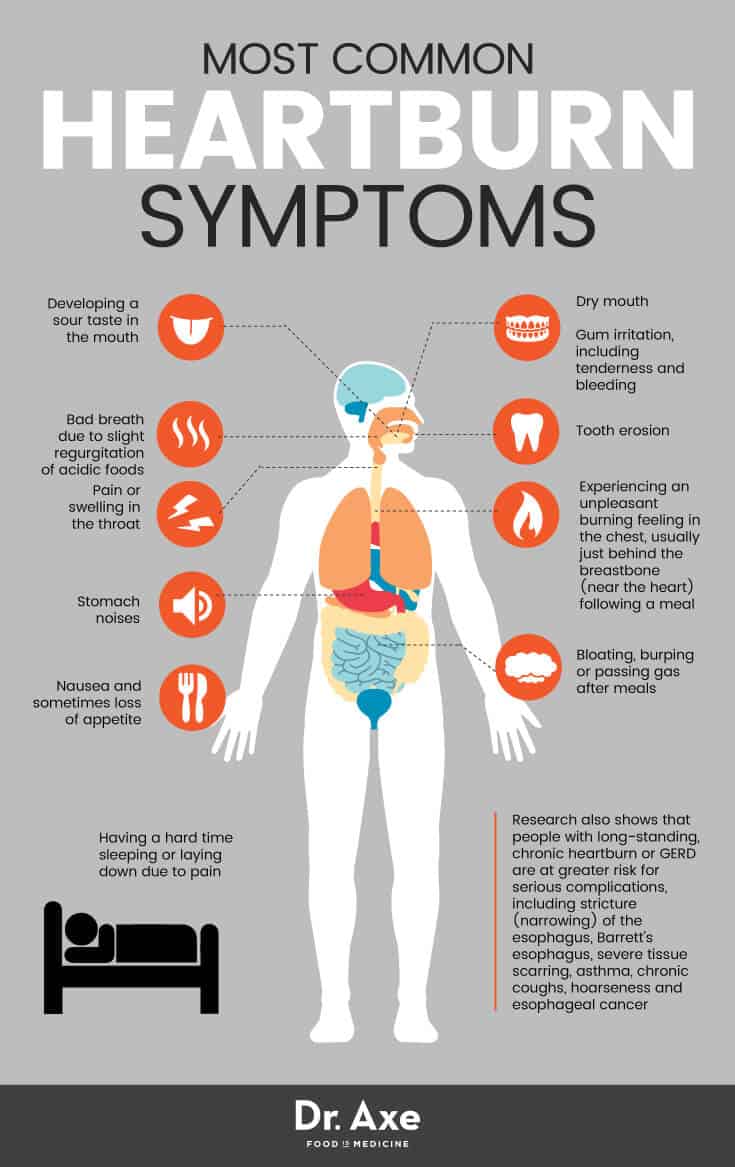
Got a burning sensation in your chest out of nowhere? In most cases it's just an acid reflux flare-up, but a few red-flag signs can mean something more serious.
Read on to discover the common triggers, how to tell if it might be a heart attack, and the safest steps you can take tonight.
Why It Happens
The anatomy of a burn esophagus vs. heart
Think of your esophagus as a stretchy tube with a tight door at the bottom called the lower esophageal sphincter (LES). When the LES relaxes at the wrong time, stomach acid sneaks back up, creating that familiar heartburn feeling. The heart, on the other hand, sits just behind the breastbone and doesn't involve acid at all.
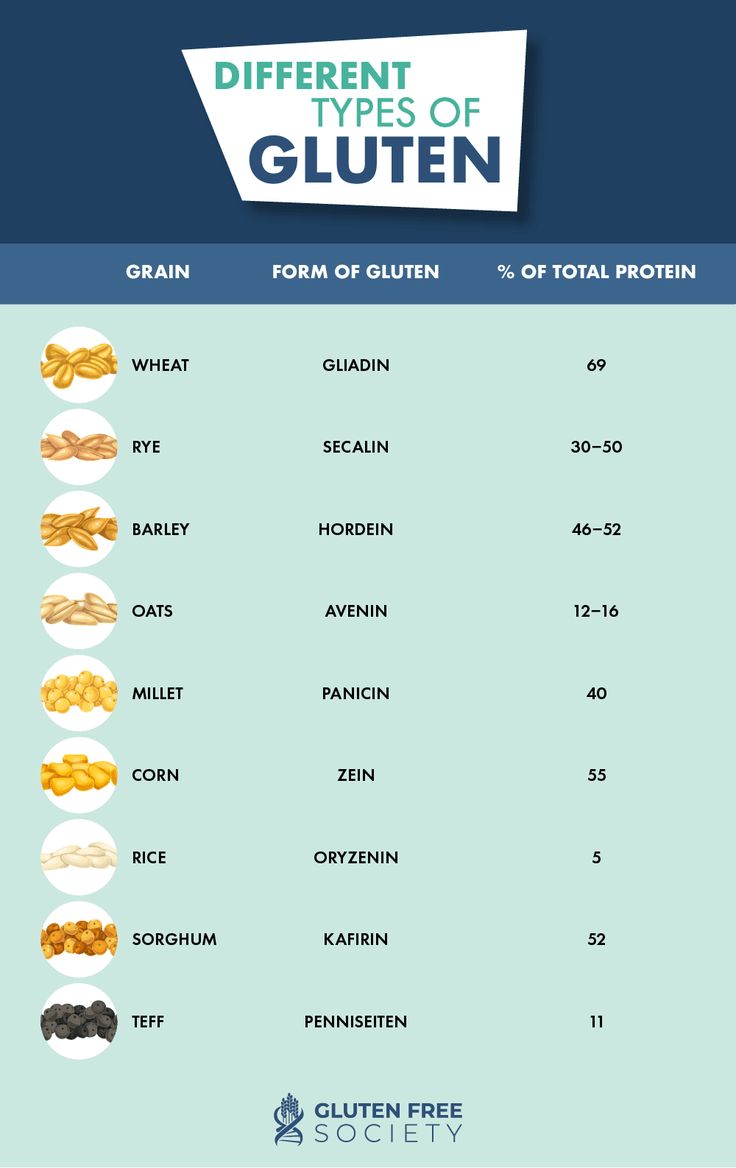
For a clear visual, the LES should stay closed after you swallow; if it's weak or relaxes too often, you get that sudden sting. GI infections or ulcers can also play a role in making your esophagus more sensitive to acid; those interested in specific digestive sensitivities and approaches may find our article on gluten detox helpful in understanding certain trigger management.
Top 7 nonfood triggers (especially for women)
While a greasy burger can certainly spark reflux, many nonfood culprits catch us off guardespecially women.
| Trigger | Why It Matters |
|---|---|
| Stress & anxiety | Hormonal stress hormones relax the LES, letting acid flow back. |
| Hormonal shifts | Pregnancy, menstrual cycles, and menopause change stomach pressure. |
| Medications | NSAIDs, certain antibiotics, and some blood pressure pills irritate the lining. |
| Smoking & alcohol | Both reduce LES tone and increase acid production. |
| Hiatal hernia | The stomach pushes up through the diaphragm, making reflux easier. |
| Nighttime reflux | Lying flat lets gravity stop helping you; sudden heartburn female at night is surprisingly common. |
| GI infections or ulcers | Inflammation can sensitize the esophagus to any acid that returns. If you're concerned about more persistent digestive issues, you may want to learn about ulcerative colitis supplements which might support gut balance during flare-ups. |
When lifestyle isn't the culprit underlying health issues
If you've tried everythingfrom ditching chocolate to sleeping with pillows under your headand the burn keeps coming, it may be time to look deeper.
- GERD (gastroesophageal reflux disease): A chronic version of the same problem, often needing prescription medication.
- Peptic ulcer disease: Ulcers can create a pressure cooker effect, pushing acid upward.
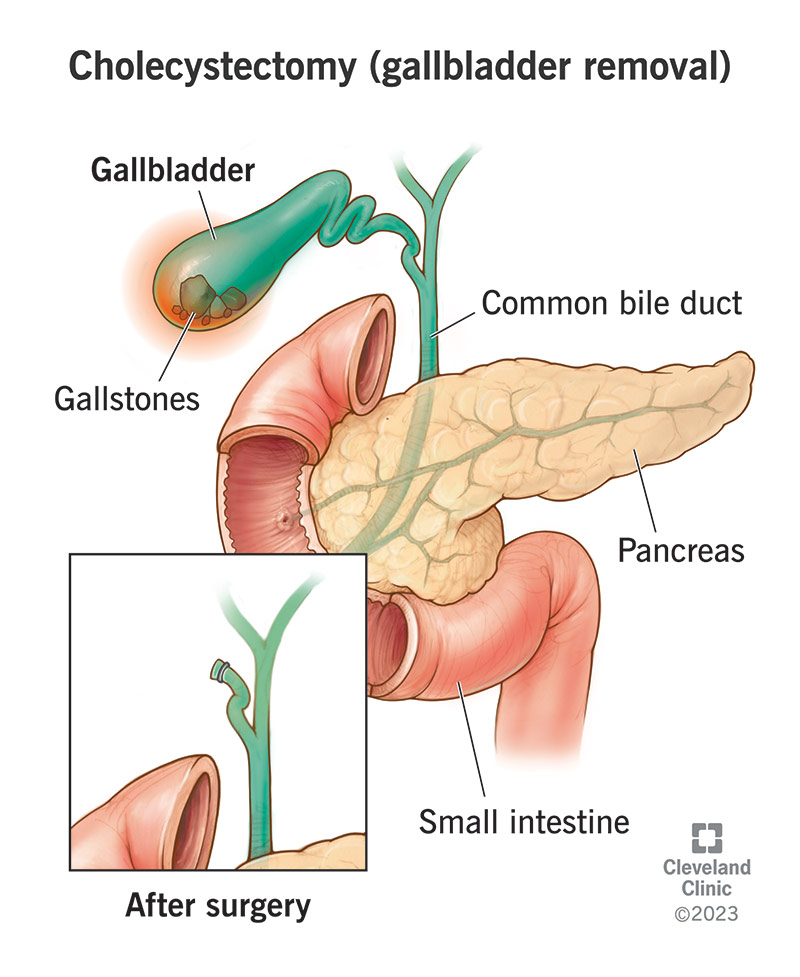
- Gallbladder problems: Bile reflux can mimic heartburn.
- Rare but serious: Conditions like esophageal cancer or Zollinger-Ellison syndrome produce relentless acid.
When in doubt, a quick chat with a gastroenterologist can pinpoint the cause. Proper testinglike an upper endoscopyhelps separate the everyday flare from something that needs stronger intervention. Chronic constipation and stool issues can also sometimes intersect with upper GI symptoms; if you notice ongoing changes in bowel habits, investigate topics like big stool constipation for more personalized advice.
Heart Attack vs. Heartburn
Key symptom differences (perfect for a quick snippet)
Both can feel like pressure, but there are telltale signs that separate them:
- Location: Heartburn burns behind the breastbone and often rises toward the throat. A heart attack pressure sits in the center of the chest and can radiate to the left arm, jaw, or back.
- Triggers: Heartburn usually appears after a big or spicy meal, when you lie down, or after bending over. A heart attack often strikes during exertion or even at rest, accompanied by a cold sweat.
- Duration: Heartburn fades after 530 minutes, especially with antacids. A heart attack pain lasts longer, typically more than 15 minutes, and doesn't ease with over-the-counter meds.
- Associated symptoms: Nausea, shortness of breath, or a feeling of impending doom points toward cardiac trouble.
Red-flag signs that require emergency care
If any of the following show up, treat the situation as urgentdon't wait for the burning to subside.
- Pain that persists >15 minutes and doesn't improve after an antacid.
- Shortness of breath, lightheadedness, or profuse sweating.
- Sudden onset while at rest, especially in women sudden heartburn female heart attack is a phrase you'll see in medical literature highlighting how women sometimes mistake cardiac pain for reflux.
Quick self-check: Do and don't list
Do try an over-the-counter antacid or a calcium carbonate tablet. If relief comes within 10 minutes, the odds are you're dealing with reflux.
Don't ignore crushing chest pressure, especially if it spreads to the arm or jaw. Call 911 or head to the nearest emergency department right away.
Instant Relief Tips
Home remedies that work tonight (even if you've had heartburn for 3 days in a row)
When the burn hits hard, reach for these simple fixes that most people have in their kitchen.
- Baking soda water: Dissolve teaspoon of baking soda in an 8oz glass of water. The alkaline solution neutralizes stomach acid quicklyjust don't make this a daily habit.
- Alkaline water: A glass of slightly alkaline water (pH 8) can calm the esophagus without the sodium load.
- Elevate your head: Prop up the head of your bed 68 inches with sturdy blocks or use a wedge pillow. Gravity becomes your ally.
- Loose clothing: Tight belts or waistbands increase abdominal pressure, pushing acid upward.
- Chew gum: Chewing stimulates saliva, which naturally buffers acid.
Dietary tweaks for the next 48 hours
If you're wondering what causes heartburn everyday, the answer often lies in small, repeatable habits.
- Avoid citrus, tomato-based sauces, chocolate, spicy foods, and fried snacks.
- Eat smaller, more frequent mealsthink 56 mini-meals rather than three huge plates.
- Stay upright for at least 23 hours after eating. A short walk or gentle stretching does wonders.
- Limit caffeine and carbonated drinks; the bubbles expand your stomach, increasing pressure on the LES.
When to see a professional (if heartburn shows up every day)
Persistent symptoms longer than two weeks deserve a professional's eye. A gastroenterologist may suggest:
- Prescription-strength H2 blockers or proton pump inhibitors (PPIs).
- Diagnostic testingpH monitoring, an upper endoscopy, or a Helicobacter pylori breath test.
- Lifestyle counseling tailored to your specific triggers.
Long-Term Strategies
Habit changes that lower risk (answering heartburn everyday all of a sudden)
Making a few steady adjustments can keep the occasional flare from becoming a chronic nuisance.
- Maintain a healthy weight: Extra belly fat pushes on the stomach, forcing acid upward.
- Exercise regularly: Moderate activities like walking or swimming help digestion, but avoid vigorous workouts right after meals.
- Quit smoking: Smoking weakens the LES and increases acid production.
- Limit alcohol: One drink a day for women, two for men, is generally safe. Anything more spikes reflux risk.
Medical treatments & when they're needed
Not everyone needs prescription meds, but for stubborn cases they can be lifesavers.
- OTC options: Antacids (Tums, Rolaids) give quick relief. H2 blockers (famotidine) work within an hour and last up to 12 hours.
- Prescription PPIs: Drugs like omeprazole or esomeprazole reduce acid production dramatically. Doctors usually recommend a short course (48 weeks) to avoid long-term side effects.
- When meds aren't enough: Surgery (fundoplication) or newer endoscopic procedures become options for severe, medication-resistant GERD.
Monitoring for complications is heartburn dangerous?
Occasional heartburn is usually harmless, but repeated exposure can lead to:
- Esophagitis: Inflammation that may cause bleeding or difficulty swallowing.
- Barrett's esophagus: A precancerous change of the lining that requires regular endoscopic surveillance.
- Strictures: Narrowing of the esophagus that can cause food to get stuck.
If you notice trouble swallowing, persistent vomiting, or a sudden weight loss, schedule a doctor's visit promptly. Early detection of complications dramatically improves outcomes.
Conclusion
Sudden heartburn is often just a fleeting acid spill, but knowing the difference between a harmless burn and a possible heart attack can save lives. By spotting red-flag signs, using quick-fix home remedies, making smart lifestyle tweaks, and seeking professional help when needed, you can keep the fire at bay and enjoy meals without fear. Have you tried any of these tips? Share your experiences in the comments, and if you'd like a printable Heartburn-Free Night checklist, click the link below. Let's beat the burn together!