Feeling constantly tired, shivering in a warm room, or wondering why your skin feels like sandpaper? Those are classic clues that somethings off with your thyroid. But when the thyroids trouble stems from the pituitary gland instead of the gland itself, the pattern of secondary hypothyroidism symptoms can feel especially confusing. Below, Ill walk you through the signs, the lab numbers, what usually causes this condition, and how doctors set the diagnosis and treatment in motion all in a friendly, stepbystep chat.
Core Symptoms Overview
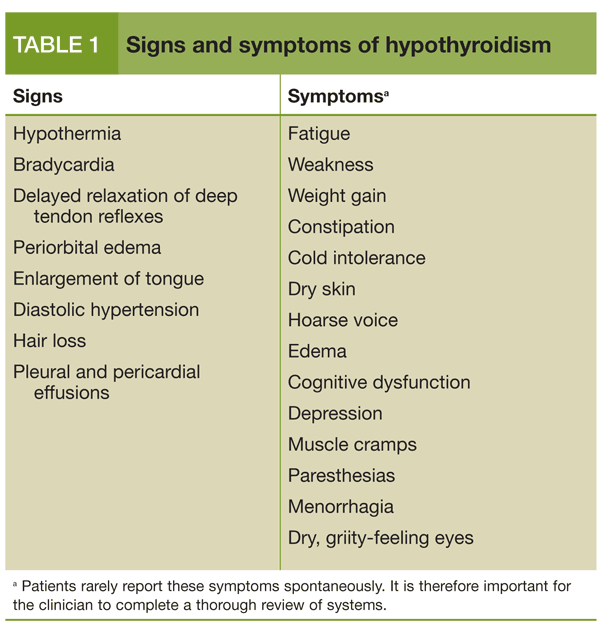
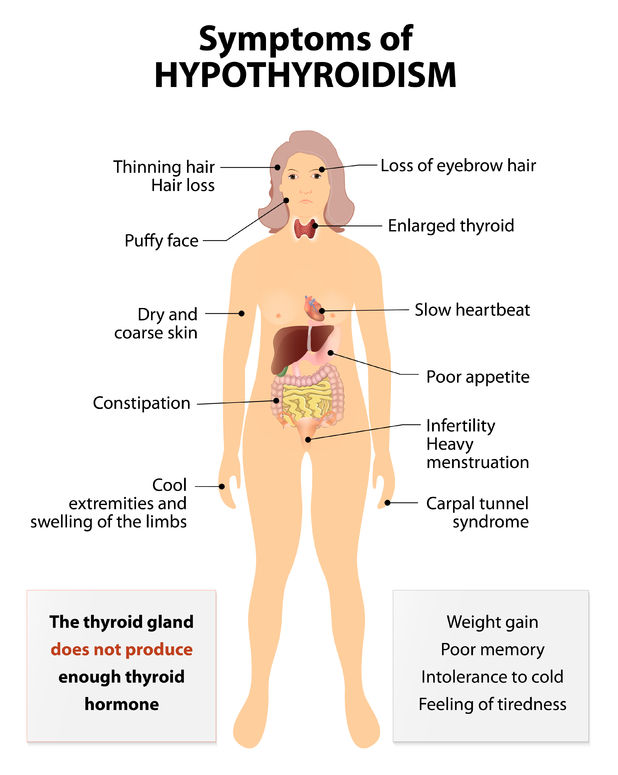
Lets start with the basics. Most of the symptoms you hear about for regular hypothyroidism show up here too. The pituitary simply isnt sending the right turn on the thyroid signal, so the thyroid stays quiet.
What overlaps with primary hypothyroidism?
- Persistent fatigue that no amount of coffee can fix
- Intolerance to cold you might feel chilly even in summer
- Dry, flaky skin and brittle nails
- Weight gain despite unchanged eating habits
- Constipation and sluggish digestion
- Depression or a general sense of brain fog
- Slowed speech and a hoarse voice
Whats unique to pituitaryorigin (secondary) hypothyroidism?
Because the problem starts upstream, a few extra clues can pop up:
- Low libido or reduced sexual desire
- In women, lighter or irregular periods and, for nursing mothers, a sudden drop in milk production
- Occasional lowgrade fever that just wont quit
- Subtle changes in growth patterns for children (slow height gain)
Do symptoms look different by age?
| Age Group | Typical Signs |
|---|---|
| Newborns | Jaundice, poor feeding, prolonged sleep |
| Children | Slow growth, delayed puberty, constipation |
| Adults | Fatigue, cold intolerance, menstrual changes |
| Seniors | Weight gain, depression, slowed speech |
Seeing these patterns in yourself or someone you love? Its worth a chat with a healthcare professional especially if the symptoms have been creeping in for months.
Lab Results Explained
The lab work is the GPS that tells doctors whether the thyroid itself is at fault or if the pituitary is sending the wrong directions.
What TSH & T4 numbers raise red flags?
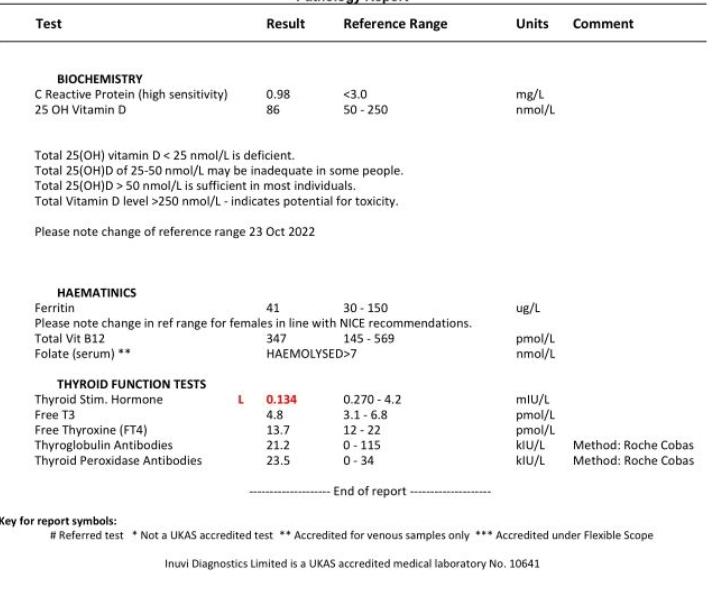
In primary hypothyroidism, the pituitary tries to compensate by pumping up TSH (thyroidstimulating hormone). In secondary hypothyroidism the opposite happens: TSH is lownormal or frankly low, while free T4 is also low. That combination is the hallmark.
Other hormone panels to consider
- ACTH and cortisol to check adrenal function
- Prolactin high levels can hint at a pituitary adenoma
- LH/FSH helpful if reproductive symptoms are present
When is imaging needed?
If labs point toward a pituitary issue, doctors often order an MRI of the brainspecifically the sellar regionbecause it gives a clear picture of any tumor, cyst, or scar tissue that might be interfering with hormone production.
Quick Reference CheatSheet
| Lab Result | Typical Secondary Pattern |
|---|---|
| TSH | Lownormal or low (<0.5IU/mL) |
| Free T4 | Low (<0.8ng/dL) |
| Prolactin | May be elevated if adenoma present |
| ACTH | Variable check cortisol if low |
According to , these lab patterns are the golden fingerprint for secondary hypothyroidism. Keep this table handy when you discuss test results with your doctor.
Main Causes Explained
Knowing why the pituitary isnt sending the right signal helps you understand the bigger picture and plan the right treatment.
Pituitary tumors (nonfunctioning adenomas)
These are the most common culprits. Even a tiny lesion can press on normal pituitary cells, reducing TSH output. Surgery or radiation often becomes part of the solution.
Surgery or radiation damage
If youve had brain surgery, especially near the sella turcica, or received radiation for a head/neck cancer, the pituitary may have been inadvertently affected.
Traumatic brain injury or infiltrative diseases
Severe head trauma, sarcoidosis, or hemochromatosis can infiltrate the gland, dampening its hormonemaking ability.
Medicationinduced suppression
Highdose glucocorticoids, dopamine agonists (like bromocriptine), and some antipsychotics can blunt TSH production. If youre on any of these, a medication review with your endocrinologist is essential.
A recent study in Endocrine Reviews highlighted that up to 15% of secondary hypothyroidism cases are medicationrelated, underscoring the need for a thorough medication history.
Diagnosis StepbyStep
Getting a solid diagnosis isnt just about ordering a blood test; its a systematic journey.
1. Clinical evaluation symptom checklist
Your doctor will start with a conversation, ticking off the symptoms we listed earlier. This helps prioritize lab work.
2. Laboratory workflow
- First: TSH & free T4
- If low TSH + low T4 move to pituitary panel (ACTH, prolactin, LH/FSH)
- Optional: Thyroid antibodies to rule out autoimmune primary disease
3. Imaging algorithm
If labs hint at secondary disease, an MRI with contrast is the next step. A CT scan is only used when MRI isnt possible.
4. Differential diagnosis
Doctors must rule out primary hypothyroidism, euthyroid sick syndrome, and even rare central nervous system disorders that can mimic the lab pattern.
Treatment & Management
Once the diagnosis is clear, treatment splits into two tracks: fixing the hormone deficit and addressing the underlying pituitary problem.
Levothyroxine the mainstay
Most patients start on a low dose of synthetic T4 (levothyroxine) and titrate upward every 46 weeks. The goal is to normalize free T4 while keeping TSH in the lownormal range.
Combination therapy (T4+T3)
Only a minority need added T3 (liothyronine) typically those who still feel sluggish despite normal T4 levels. This decision is best made with an endocrinologist.
Addressing the underlying cause
- Microadenoma surgery (transsphenoidal approach) if a tumor is present
- Radiation therapy for inoperable lesions
- Medication adjustments if a drug is suppressing TSH
According to , careful monitoring is key overtreatment can push you into hyperthyroidism, causing heart palpitations and bone loss.
Lifestyle tweaks that help
- Stay warm layer up, use heating pads, and keep your living space comfortably heated.
- Balanced diet rich in iodine, selenium, and zinc (but avoid excessive supplements).
- Gentle exercise (walking, yoga) to boost energy without overtaxing the heart.
- Stressreduction techniques mindfulness or light breathing exercises can improve overall wellbeing.
RedFlag Situations
Even with treatment, some warning signs demand immediate medical attention.
- Rapid, unexplained weight gain paired with swelling around the face and neck (possible myxedema).
- Sudden drop in heart rate below 50bpm or body temperature under 95F.
- Severe depression, confusion, or memory loss that worsens quickly.
- Pregnant women experiencing worsening hypothyroid symptoms untreated hypothyroidism can affect fetal development.
If any of these pop up, call your doctor right away or head to the emergency department. Early intervention can prevent serious complications.
Bottom Line Summary
Secondary hypothyroidism can feel like a mystery because its symptoms mirror those of the more common primary form, yet the root cause lies in the pituitary. Recognizing the classic signs persistent fatigue, cold intolerance, dry skin, and the extra clues like low libido or menstrual changes is the first step. Lab work showing low TSH and low free T4 points the finger at the pituitary, and imaging often confirms the picture.
The good news? Most cases respond well to levothyroxine, and when a tumor or medication is the trigger, targeted treatment can restore normal hormone balance. The key is to stay vigilant, ask questions, and partner with a knowledgeable endocrinologist who can tailor therapy to your unique situation.
If youve noticed any of these symptoms, dont wait. Schedule a checkup, bring this guide along, and let your doctor run the appropriate labs. Knowledge is power, and the sooner you act, the faster youll get back to feeling like yourself again.
For readers comparing treatment options for thyroid hormone replacement, some patients research Armour vs levothyroxine to understand differences between desiccated thyroid products and synthetic T4 therapy.