Hey there If you're stuck in the endless cycle of sneezing, watery eyes, and that stubborn stuffy nose every spring, you've probably wondered whether there's a more permanent fix than popping antihistamines forever. Short answer: seasonal allergies surgery can be a game-changer for many, but it's not a magic cure-all. Let's walk through what the surgery really does, how much it might cost, which meds you can (or can't) take before going under, and how to prepare so you feel confident and comfortable.
Can Surgery Help?
Will surgery actually ease my allergy symptoms?
Think of surgery as a structural makeover for the inside of your nose and sinuses. It won't stop your immune system from reacting to pollen, but it can clear the blockages that make those reactions feel downright miserable. By opening up the airways and removing inflamed tissue, most patients notice a dramatic drop in congestion, fewer sinus infections, and a big improvement in sleep quality.
What do specialists say?
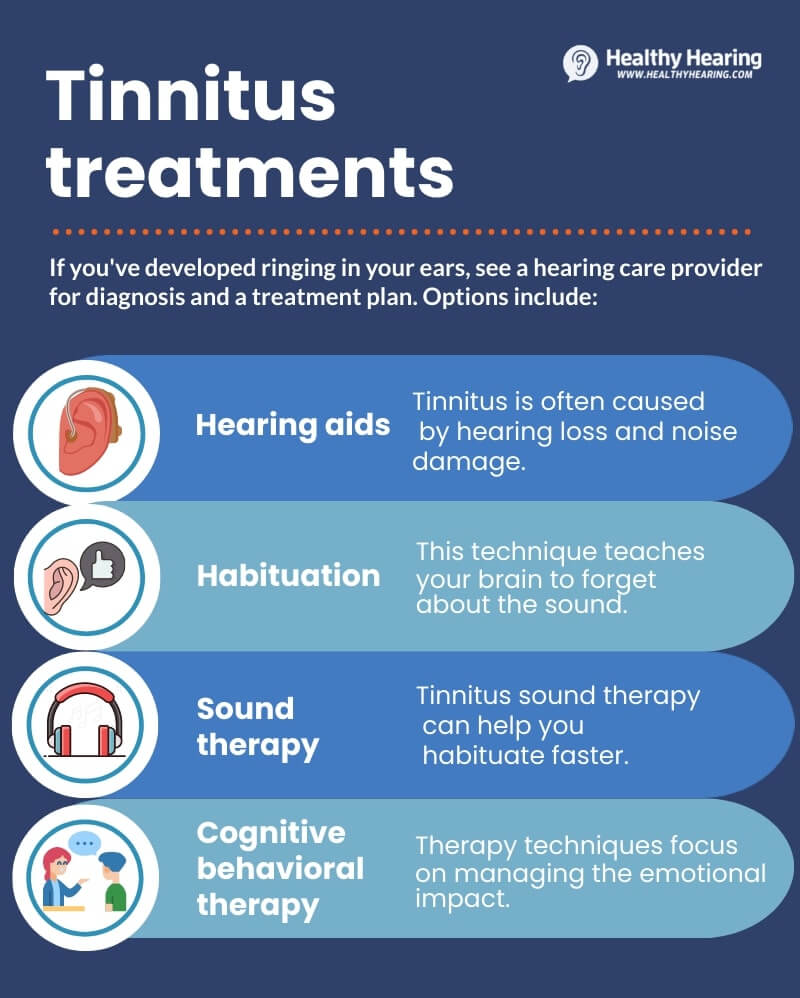
According to a systematic review of dozens of studies, more than 70% of people report significant relief from nasal obstruction after undergoing procedures like inferior turbinate reduction. That's a solid endorsement from the medical communityespecially when you consider the alternative of living with chronic, medication-dependent symptoms. For those who are interested in exploring non-surgical remedies for other conditions, such as tinnitus, there are various approaches available. For instance, some people find relief through natural tinnitus remedies or practices like tinnitus meditation.
Surgery Types Explained
Which procedures are on the table?
There isn't a one-size-fits-all operation, but here are the most common sinus surgery options that ENT doctors talk about when you bring up seasonal allergies:
| Procedure | Ideal Candidate | Recovery Time | Typical Cost (US) | Success Rate |
|---|---|---|---|---|
| Functional Endoscopic Sinus Surgery (FESS) | Chronic sinusitis, polyps, structural blockage | 12 weeks for basic recovery; 46 weeks for full healing | $8,000$15,000 | 8090% |
| Balloon Sinuplasty | Mild-to-moderate sinus blockage, want minimally invasive option | 35 days off work | $4,000$9,000 | 7080% |
| Inferior Turbinate Reduction | Persistent nasal congestion from allergic rhinitis | 57 days | $3,000$7,000 | 7585% |
| Septoplasty + Turbinate Surgery | Deviated septum + allergy-related congestion | 12 weeks | $6,000$12,000 | 80% |
What's the vibe of each?
FESS is the heavyweight championgreat for deep, stubborn disease but comes with a longer recovery. Balloon sinuplasty feels like inflating a tiny balloon inside your sinus passages; many love its quick turnaround. Turbinates are the nose-airflow boosters that shave down swollen tissue, which can be a lifesaver when antihistamines only mask the problem.
Safety & Allergies
Is it safe to go under the knife when I'm allergic?
Absolutelyprovided you give your surgeon and anesthesiologist a thorough allergy history. Uncontrolled allergies can raise the risk of airway irritation or bronchospasm during anesthesia, but with a proper pre-op plan those risks shrink to a tiny fraction.
Why no antihistamine before surgery?
Most non-sedating antihistamines (like Claritin or Allegra) are perfectly fine, but you'll want to avoid sedating antihistamines like Benadryl. They can linger in your system, make you drowsy, and interfere with the anesthetic's effects. That's why the rule "no Benadryl 24 hours before surgery" is so common.
Medication QuickGuide
| Medication | Safe? | When to Stop |
|---|---|---|
| Claritin (loratadine) | Yes | None can continue up to day of surgery |
| Allegra (fexofenadine) | Yes | None |
| Loratatine (generic) | Yes | None |
| Benadryl (diphenhydramine) | No | At least 24hrs before |
| Flonase (nasal spray) | Yes | Morning of surgery is fine |
| Montelukast (Singulair) | Yes | Unless your doctor says otherwise |
What else should I tell my team?
Bring a list of every allergy you've ever hadeven the ones that seem unrelated, like latex or certain foods. Mention any past reactions to anesthesia, and be honest about the severity of your seasonal symptoms. The more details you share, the better they can tailor the anesthesia plan.
Cost of Surgery
How much will it set me back?
Money talks, and it's a major factor when you're weighing options. Here's a quick snapshot of average prices in 2025 (based on data from leading healthcare cost calculators):
- FESS: $8,000$15,000
- Balloon sinuplasty: $4,000$9,000
- Turbinates reduction: $3,000$7,000
- Septoplasty + turbinates: $6,000$12,000
Will my insurance cover it?
Most major insurers will foot the bill if they deem the procedure medically necessary. That usually means you have chronic sinusitis, repeated infections, or obstructive sleep apnea that can't be managed with medication alone. Knowing the CPT codes (e.g., 31254 for FESS) can help you talk to your provider's billing department and avoid surprise out-of-pocket costs.
Tips to keep the price down
1. Schedule your surgery during the offseason (late fall or early winter) when clinics are less busy.
2. Ask for an in-network ENT surgeon.
3. Explore financing plans or healthcare credit cards if you need to spread out payments.
4. Double-check whether your pre-op labs and imaging are truly needed; sometimes a simple CT scan can be avoided.
Benefits vs Risks
The bright side
When the surgery goes well, you often enjoy:
- Clearer breathing no more feeling like you're trying to inhale through a straw.
- Fewer sinus infections those nasty pressure-pop headaches become rare.
- Reduced reliance on daily antihistamines less risk of side-effects like dry mouth.
- Improved sleep quality because you're no longer fighting a constant blocked nose battle at night.
The flip side
Every medical intervention carries a risk. Here are the most common downsides people talk about:
- Bleeding or infection the usual post-op worries, but they're manageable with proper care.
- Temporary dryness or crusting inside the nose a few weeks of saline rinses usually sort it out.
- Rare anesthesia reactions, especially if allergies aren't fully disclosed.
- Symptom recurrence if you keep exposing yourself to high pollen counts without allergy shots or immunotherapy, the benefits can fade over time.
Real-World Snapshot
Take Maya, a 34-year-old graphic designer from Seattle. She tried every over-the-counter antihistamine, still waking up with a congested head each night. After a thorough evaluation, she opted for a turbinate reduction combined with a minor FESS. Six months later, Maya reports breathing feels like she's "finally taken off a heavy backpack." She still takes a low-dose nasal steroid during peak pollen season, but she's no longer dependent on multiple pills throughout the day.
Preparing for Surgery
Pre-op checklist for you
Getting ready can feel overwhelming, so here's a handy list to tick off:
- Complete an allergy questionnaire (bring a printed copy to the office).
- List every medication you're onprescription, OTC, supplements.
- Stop sedating antihistamines (Benadryl) at least 24 hours before.
- Schedule the operation during a low-pollen month if possible.
- Arrange transportation and a post-op caregiver for the first 24-48 hours.
- Stock up on saline rinse kits and a gentle nasal moisturizer.
Day-of-surgery expectations
You'll check in, meet the anesthesiologist, and receive a short briefing about what to expect. The actual sinus surgery part usually lasts 45-90 minutes, depending on the procedures. You'll wake up in a recovery room feeling a bit groggy but generally alert. Most people are discharged the same day, though some clinics keep you overnight for observation if the surgery was extensive.
Recovery roadmap
First week: Light activity, nasal saline rinses 2-3 times a day, avoid heavy lifting.
Weeks 2-4: Gradual return to normal exercise; you may notice some crustingjust keep the rinses going.
Month 2 onward: Follow-up with your ENT, discuss long-term allergy management (like immunotherapy), and enjoy the newfound airflow.
Bottom Line Decision
Choosing seasonal allergies surgery isn't about jumping on a quick fix; it's about weighing a real, lasting improvement in quality of life against the natural risks of any operation. If you're fed up with endless antihistamine cycles, frequent sinus infections, and sleepless nights, a thoughtful conversation with a board-certified ENT could open the door to clearer breathingand a happier you.
Ready to explore your options? Book a consultation with a trusted ENT specialist, bring your medication list, and let's get you on the path to breathing easy again. Have you or someone you know gone through sinus surgery? Share your story in the commentsyour experience could be the encouragement a friend needs!
Conclusion
Seasonal allergies can feel like an unwelcome guest that never leaves, but surgery offers a solid strategy to change the game. By understanding the different procedures, getting a clear picture of costs, and knowing exactly which meds are safe before the operation, you empower yourself to make a confident choice. Remember, the goal isn't to erase allergies completelyit's to give your nose the room it needs to function without constant blockage. If you think surgery might be right for you, reach out to a qualified ENT, ask all the questions you have, and take the first step toward clearer, calmer days ahead.
FAQs
What types of surgery are available for seasonal allergies?
Common procedures include Functional Endoscopic Sinus Surgery (FESS), Balloon Sinuplasty, Inferior Turbinate Reduction, and Septoplasty combined with turbinate surgery. The choice depends on the severity of blockage and underlying anatomy.
How long is the recovery period after sinus surgery?
Recovery varies by procedure: basic turbinate reduction may take 5‑7 days, Balloon Sinuplasty 3‑5 days off work, and FESS 1‑2 weeks for basic healing, with full recovery in 4‑6 weeks.
Which medications must I stop before undergoing seasonal allergies surgery?
Avoid sedating antihistamines such as Benadryl (diphenhydramine) at least 24 hours before surgery. Non‑sedating antihistamines (Claritin, Allegra), nasal steroids, and montelukast are usually safe to continue.
Will my insurance cover the cost of allergy‑related sinus surgery?
Most insurers cover the procedure when it’s deemed medically necessary—typically for chronic sinusitis, repeated infections, or significant obstruction. Providing CPT codes (e.g., 31254 for FESS) helps ensure coverage.
Can seasonal allergies surgery permanently cure my allergy symptoms?
Surgery does not eliminate the allergic response, but it removes structural blockages, greatly reducing congestion, infections, and medication dependence. Ongoing allergy management (e.g., immunotherapy) may be needed to maintain results.