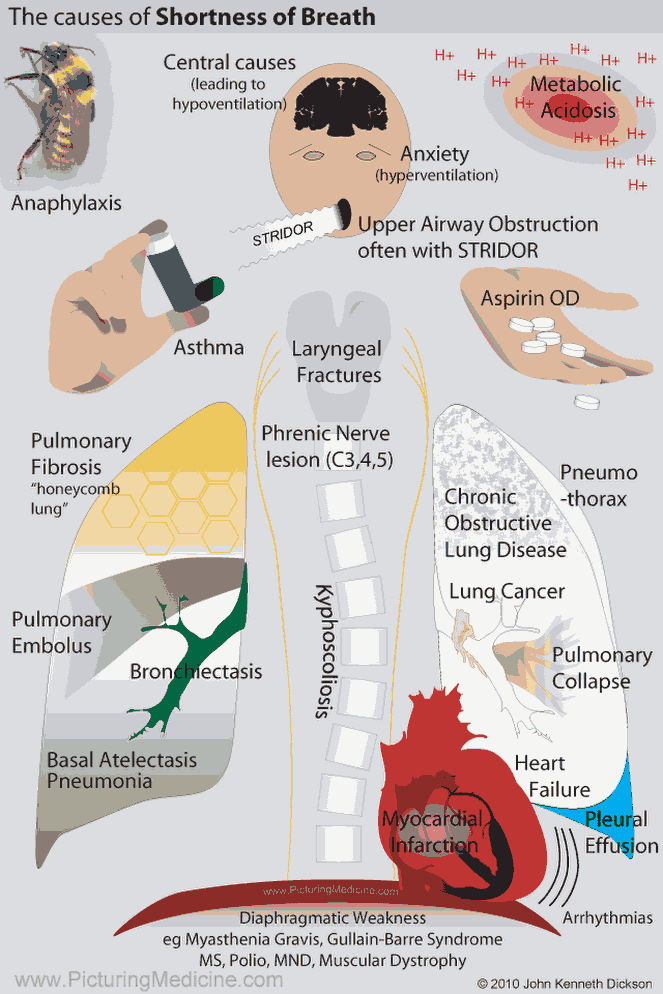
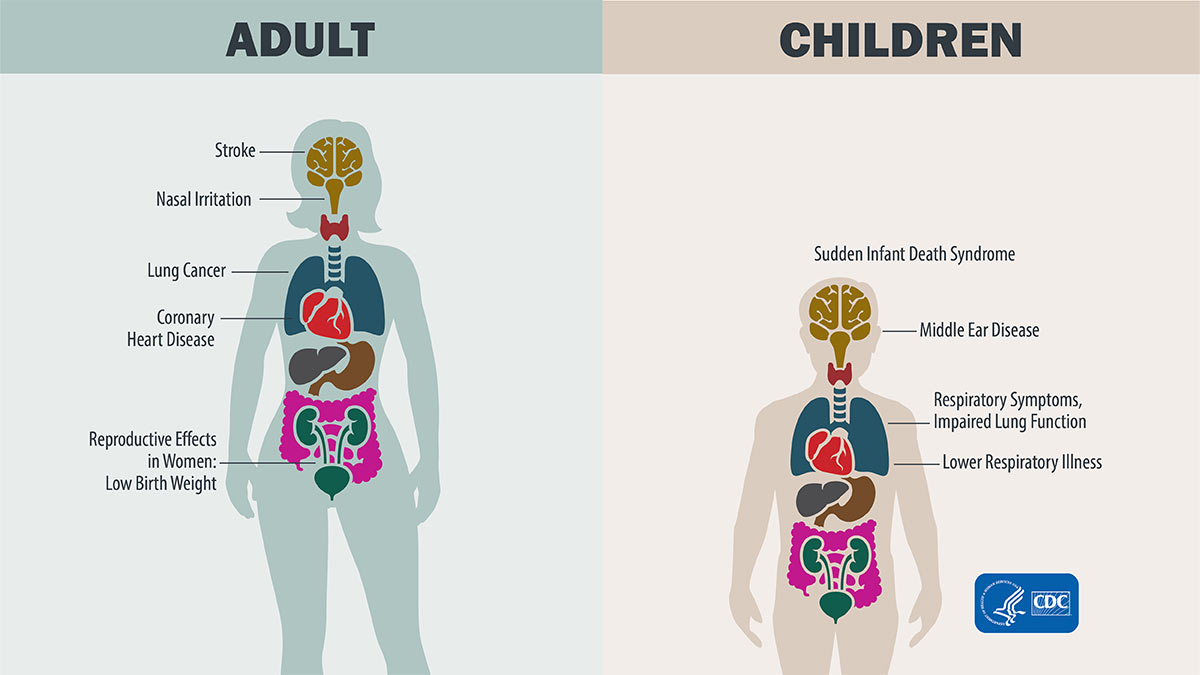
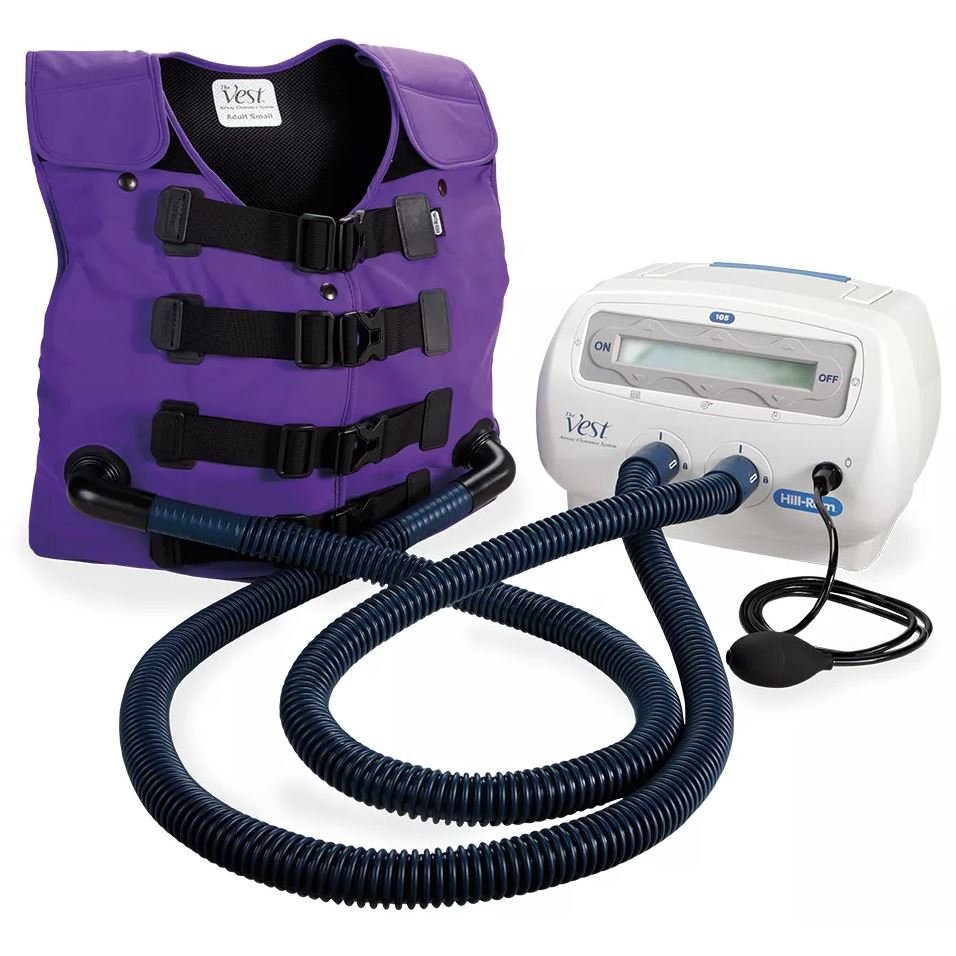
Ever felt like you cant catch a breath even though your lungs are perfectly healthy? That sudden, unsettling shortness of breath is what clinicians call psychogenic dyspnea a real, minddriven breathing disturbance that can be puzzling, frightening, and, fortunately, treatable.
What Is Psychogenic Dyspnea
In plain language, psychogenic dyspnea is a functional breathing problem. Your lungs and airways are fine; the issue lives in the brainbody connection, often sparked by anxiety, stress, or other emotional triggers. Think of it as a hissing kettle that whistles even when theres no water boiling the signal is there, but the source is different.
Medical textbooks separate it from organic dyspnea (the shortness of breath caused by heart or lung disease) by noting normal imaging, normal spirometry, and normal oxygen levels. Instead, the pattern aligns with heightened nervoussystem activity.
When a patient reports breathlessness but every test comes back clear, we start looking at the psychological landscape, explains Dr. Maya Patel, boardcertified pulmonologist at the Center for Functional Respiratory Disorders.
Recognizing the Symptoms
Spotting psychogenic dyspnea early can save you countless ER trips. Here are the most common clues:
- Panictype breathlessness: Sudden onset, often during a stressful event, with a feeling of air hunger.
- Psychogenic hyperventilation: Fast, shallow breaths that can cause tingling in the fingers and lightheadedness.
- Sighing dyspnea: Repetitive, deep sighs that dont improve oxygenation.
- Normal test results: Chest Xray, CT, ECG, and spirometry all read no abnormalities.
- Associated sensations: Mild chest tightness, throat clearing, or a feeling that the throat is closing (sometimes linked to psychogenic dysphonia or dysphagia).
| Feature | Psychogenic Dyspnea | Cardiac Dyspnea | Pulmonary Dyspnea |
|---|---|---|---|
| Onset | Triggered by stress or anxiety | Exercise, exertion | Gradual, worsens with activity |
| Chest Xray | Normal | Possible enlargement, fluid | Emphysema, infiltrates |
| O Saturation | Normal | May drop | May drop |
| Typical accompanying symptoms | Tingling, sighing, chest tightness | Pain, swelling | Cough, wheeze |
These patterns show why a thorough history is more telling than any scan.
How Doctors Diagnose
Diagnosing psychogenic dyspnea is a methodical byexclusion process. Think of it as peeling an onionlayer by layer, you remove organic causes until what remains is clearly functional.
Step 1: Detailed History & MentalHealth Screening
Clinicians ask about recent stressors, panic attacks, and use questionnaires like GAD7 (for anxiety) and PHQ9 (for depression). Your answers help map the emotional terrain that could be fueling breathlessness.
Step 2: Physical Exam & Baseline Tests
Even if you feel fine, doctors will order:
- Spirometry to assess airflow
- Chest Xray or CT to rule out structural disease
- Electrocardiogram (ECG) for heart rhythm
- Pulse oximetry to confirm normal oxygen levels
Step 3: Specialized Evaluations (When Needed)
If basic tests are inconclusive, the next tier might include capnography (measures CO) or laryngoscopy to check for vocalcord dysfunctionoften linked to .
Diagnostic Flowchart (Quick Visual)
In the final article, well provide a clean flowchart that starts with Shortness of Breath? and ends with Functional Breathing Disorder?. For now, remember: normal tests + anxiety triggers = psychogenic dyspnea.
Effective Treatment Options
Good news: there are evidencebased pathways to calm the breath and the brain. Treatment is usually a blend of psychology, gentle medication, and practical breathing tools.
Psychological Therapies
CognitiveBehavioral Therapy (CBT) is the gold standard. It helps you identify catastrophic thoughts (Im going to suffocate) and replace them with realistic ones. A 2022 randomized trial showed that 68% of participants reported a 50% reduction in breathlessness after eight CBT sessions to a study in JAMA.
ExposureBased Breathing Retraining gradually confronts feared situations (like crowded spaces) while practicing paced breathing, building confidence that the breath will stay steady.
Pharmacologic Support
- SSRIs or SNRIs (e.g., sertraline, venlafaxine) for underlying anxiety/depressionespecially when CBT alone isnt enough.
- Shortacting anxiolytics (like lorazepam) for acute panic spikes, but only under careful supervision to avoid dependence.
Adjunctive & SelfManagement Tools
These are the DIY parts you can start today:
- Diaphragmatic breathing: Slow, bellyfocused breaths (424 count) restore CO balance.
- Biofeedback apps: Visualize your breathing pattern and learn to smooth it out.
- Relaxation training: Progressive muscle relaxation or guided imagery before stressful events.
- Physiotherapy breathingreeducation programs: Often run in multidisciplinary clinics.
PseudoDyspnea Treatment Checklist
| Action | When to Use |
|---|---|
| CBT session | Persistent anxietyrelated breathlessness |
| SSRIs/SNRIs | Coexisting depression or chronic anxiety |
| Diaphragmatic breathing | Any time you feel a tight chest |
| Biofeedback app | During panic spikes or before public speaking |
| Physiotherapy program | When you want structured, supervised training |
Living With Psychogenic Dyspnea
Learning to live with this condition isnt about curing a disease; its about reclaiming control over your breath.
5Step GroundYourBreath Exercise
- Sit comfortably, shoulders relaxed.
- Place one hand on your belly, the other on your chest.
- Inhale slowly through the nose for a count of4, feeling the belly rise.
- Hold for a count of2.
- Exhale gently through pursed lips for a count of6, feeling the belly fall.
Repeat this cycle five times whenever you sense the urge to hyperventilate. Youll notice the air hunger fading as CO normalizes.
Lifestyle Tweaks
- Sleep hygiene: Aim for 79hours; poor sleep amplifies anxiety.
- Caffeine moderation: Too much coffee can trigger jittery breathing.
- Regular movement: Yoga or tai chi blends gentle stretch with breath focus.
Breathing Toolkit
Keep a small notebook or phone note titled My Breath Log. Jot down:
- Date, time, and setting (e.g., Meeting, 2pm).
- Symptoms felt (e.g., Chest tightness, sighing).
- What you did (CBT technique, breathing exercise).
- Outcome (symptom reduction, still present).
Over weeks, patterns emergemaybe you notice that traffic jams are the biggest trigger. Knowing this, you can proactively use a coping strategy. If you or a partner has a chronic respiratory condition such as cystic fibrosis, consider tailored advice on relationships and safety while managing breathlessness resources on cystic fibrosis relationships can help couples balance emotional support with practical care.
RealWorld Story
Sarah, a 28yearold graphic designer, visited the ER three times in six months with asthmalike attacks. All tests were clean. After a referral to a functional breathing clinic, she started CBT and practiced diaphragmatic breathing daily. Within three months, her episodes dropped from weekly to once a quarter, and she finally felt confident taking a flight overseassomething shed avoided for years.
Stories like Sarahs illustrate that, with the right mix of professional help and selfcare, psychogenic dyspnea can become a manageable part of life rather than a mysterious enemy.
When to Seek Professional Help
While psychogenic dyspnea itself isnt lifethreatening, it can coexist with real cardiac or pulmonary conditions. Keep an eye out for red flags that demand immediate attention:
- Sudden, severe chest pain
- Fainting or loss of consciousness
- Persistent fever, cough, or sputum production
- Rapid heart rate (>120bpm) at rest
If any of these appear, call emergency services or head straight to the nearest ER.
For nonemergent concerns, start with a primarycare physician. They can order baseline tests and, if needed, refer you to a pulmonologist, psychologist, or an interdisciplinary breathing clinic. Bring your Breathing Log and any notes about recent stressorsthese help the team see the whole picture.
Conclusion
Psychogenic dyspnea is a genuine functional breathing disorder where the mind sends false alarms to the lungs. By recognizing the hallmark symptoms, undergoing a careful byexclusion diagnosis, and embracing a blend of CBT, targeted breathing exercises, and, when appropriate, medication, most people regain a steady, confident breath.
Remember, youre not alone, and help is within reach. Track your symptoms, talk openly with your healthcare team, and give yourself credit for every small victoryeach calm breath is a step toward freedom.
Whats your experience with breathlessness? Share your story in the comments or ask any questions belowwere all in this together.
FAQs
What exactly is psychogenic dyspnea?
Psychogenic dyspnea is a functional breathing disorder where a person feels short‑of‑breath despite having normal lung and heart tests. The sensation is driven by anxiety, stress, or other emotional factors rather than structural disease.
How is psychogenic dyspnea diagnosed?
Diagnosis is made by exclusion: doctors first rule out cardiac, pulmonary, and metabolic causes with spirometry, imaging, ECG, and oxygen saturation. A detailed history, anxiety/depression questionnaires, and sometimes capnography or laryngoscopy complete the work‑up.
Can medication help with psychogenic dyspnea?
Yes. Selective serotonin reuptake inhibitors (SSRIs) or serotonin‑norepinephrine reuptake inhibitors (SNRIs) are often prescribed for underlying anxiety or depression. Short‑acting anxiolytics may be used for acute panic spikes under close supervision.
What breathing techniques are most effective?
Diaphragmatic (belly) breathing, paced 4‑2‑6 counts, and biofeedback‑guided breathing exercises help normalize CO₂ levels and reduce the sensation of “air hunger.” Regular practice combined with CBT yields the best results.
When should I seek urgent medical care?
If breathlessness is accompanied by severe chest pain, fainting, rapid heart rate over 120 bpm at rest, fever, or productive cough, treat it as an emergency and call 911 or go to the nearest ER.