Ever woken up and found that your voice sounded like a whisper, even though theres no sore throat or cold? That sudden, baffling loss of voice can be psychogenic dysphonia, a condition where stress, anxiety, or trauma shut down the vocal cords without any physical damage. The good news? Its treatable, and with the right blend of voice work and emotional support, most people get their voice back.
What Is Psychogenic Dysphonia
Think of your voice as a radio station that needs a clear signal to broadcast. In psychogenic dysphonia, the signal is interrupted by the brains emotional wiring rather than a broken speaker. The vocal folds themselves are perfectly healthy; its the nervous systems control that gets tangled up, often because of intense stress, unresolved trauma, or chronic anxiety.
Medical professionals sometimes label it functional or conversion dysphonia, which simply means the problem is functional (no structural damage) and may arise from a conversion of emotional distress into physical symptoms.
How It Happens
The larynx (voice box) is regulated by a complex network of nerves. When youre under severe emotional strain, that network can go into a protective mode, effectively turning off the voice to avoid further stress. Its similar to how you might freeze in a scary situationyour body adopts a defense strategy that isnt meant to last.
Whos Affected
- Women are diagnosed more often than men, especially between ages 2050.
- People with a history of anxiety, depression, or past trauma are at higher risk.
- Highpressure professions (teachers, singers, callcenter agents) sometimes experience it after prolonged vocal stress.
Key Symptoms to Spot
If youve noticed any of these signs persisting for more than two weeks, its time to investigate further:
- Sudden hoarseness or complete loss of voice.
- A breathy, weak, or strained sound when you try to speak.
- No pain, cough, or throat irritation accompanying the voice change.
- Symptoms that worsen during stressful moments and improve when youre relaxed.
Red Flags That Suggest Something Else
Not every hoarse voice is psychogenic. If you also experience pain, frequent throat clearing, a sensation of a lump in the throat, or neurological signs (like facial weakness), you might be dealing with or . Those conditions involve actual physical changes to the vocal folds or surrounding muscles.
Quick Comparison
| Feature | Psychogenic Dysphonia | Spasmodic Dysphonia | MuscleTension Dysphonia |
|---|---|---|---|
| Onset | Sudden, stressrelated | Gradual, involuntary spasms | Chronic, posturerelated |
| Voice Quality | Breathy, weak, strained | Harsh, strained, tight | Variable, often tight |
| Neurologic Signs | None | Possible | None |
| Typical ICD10CM | F45.9 or R49.0 | G51.1 | J38.5 |
Differences From Other Disorders
Understanding where psychogenic dysphonia fits among voice disorders helps you (and your clinician) choose the right treatment path.
Conversion Dysphonia vs. Psychogenic Dysphonia
Both terms describe voice loss without organic cause, but conversion often emphasizes a psychological conversion of emotional distress into a physical symptom. Psychogenic dysphonia is the broader, more contemporary label used by speechlanguage pathologists.
Functional Dysphonia vs. Psychogenic Dysphonia
Functional dysphonia covers any voice problem without structural damage, including psychogenic dysphonia. Think of functional dysphonia as the umbrella; psychogenic dysphonia is one specific reason under that umbrella.
Spasmodic & MuscleTension Dysphonia
These involve real muscular or neurological disturbances of the vocal cords. Unlike psychogenic dysphonia, they often require medication, botox injections, or specific surgical interventions.
Diagnosis & ICD10 Code
Getting an accurate diagnosis is a collaborative effort between an ENT specialist, a speechlanguage pathologist (SLP), and often a mentalhealth professional.
Clinical Workup Steps
- ENT Exam & Laryngoscopy: A doctor looks at your vocal folds with a tiny camera to rule out nodules, polyps, or tumors.
- Voice Assessment: An SLP records your voice, measures acoustic parameters, and rates quality on standardized scales.
- Psychological Screening: Tools like the PHQ9 (depression) and GAD7 (anxiety) help identify underlying emotional factors.
ICD10CM Coding
The most common code used is F45.9 Somatoform disorder, unspecified, which captures the psychogenic nature of the condition. If the voice change is documented without a confirmed psychological cause, clinicians may use R49.0 Dysphonia, unspecified. Either code ensures proper insurance billing while reflecting the conditions nature.
Quick Coding CheatSheet
- F45.9: Primary psychogenic dysphonia.
- R49.0: When cause is uncertain or secondary.
Treatment Options Overview
Think of treatment as a twotrack train: one track focuses on restoring the voices mechanics, the other on untangling the emotional triggers.
Voice Therapy The Core
Speechlanguage pathologists use evidencebased techniques to retrain the vocal folds:
- Resonant Voice Therapy: Teaches you to produce sound with minimal vocal fold impact.
- LSVTLO (Lee Silverman Voice Treatment LO): Intense, higheffort exercises that boost vocal intensity and coordination.
- Breathing & Posture Drills: Aligning your diaphragm and shoulders reduces tension that can choke the voice.
Typical programs run 612 weeks, with one or two sessions per week, plus daily home practice.
Psychotherapy & Stress Management
Because stress is the chief culprit, addressing it directly yields the best outcomes. Common approaches include:
- CognitiveBehavioral Therapy (CBT): Helps reframe anxious thoughts that trigger voice shutdown.
- Eye Movement Desensitization & Reprocessing (EMDR): Often used when past trauma fuels the voice loss.
- Mindfulness & Biofeedback: Teaches you to notice tension early and release it before it silences you.
A showed that combining CBT with voice therapy improved voice quality in 78% of participants within three months.
Medication When It Helps
Medication isnt a firstline treatment, but it can support therapy when anxiety or depression is severe:
- SSRIs (e.g., sertraline): Reduce underlying anxiety, making voice exercises easier.
- ShortTerm Anxiolytics: May be prescribed during a crisis, but only under close medical supervision.
Always discuss medication with both your ENT and mentalhealth provider to ensure a coordinated approach.
Integrated Care Pathway
Heres a simple flow you might follow:
- Visit an ENT to rule out structural issues.
- Get a referral to an SLP for voice therapy.
- Simultaneously, see a psychologist or psychiatrist for CBT/EMDR.
- Reevaluate after 8 weeks adjust therapy intensity or add medication if needed.
RealWorld Experience Stories
Sarahs Story: From Whisper to Song
Sarah, a 34yearold elementary teacher, woke up after a stressful parentteacher conference with a voice that sounded like shed been shouting into a pillow. After two weeks of hoarseness, she saw an ENT who found no physical abnormality. An SLP started resonant voice exercises, while a therapist introduced CBT to manage her perfectionism. Six weeks later, Sarah could lead her classroom again, and her voice felt richer than ever.
Dr. Martinezs Clinical Insight
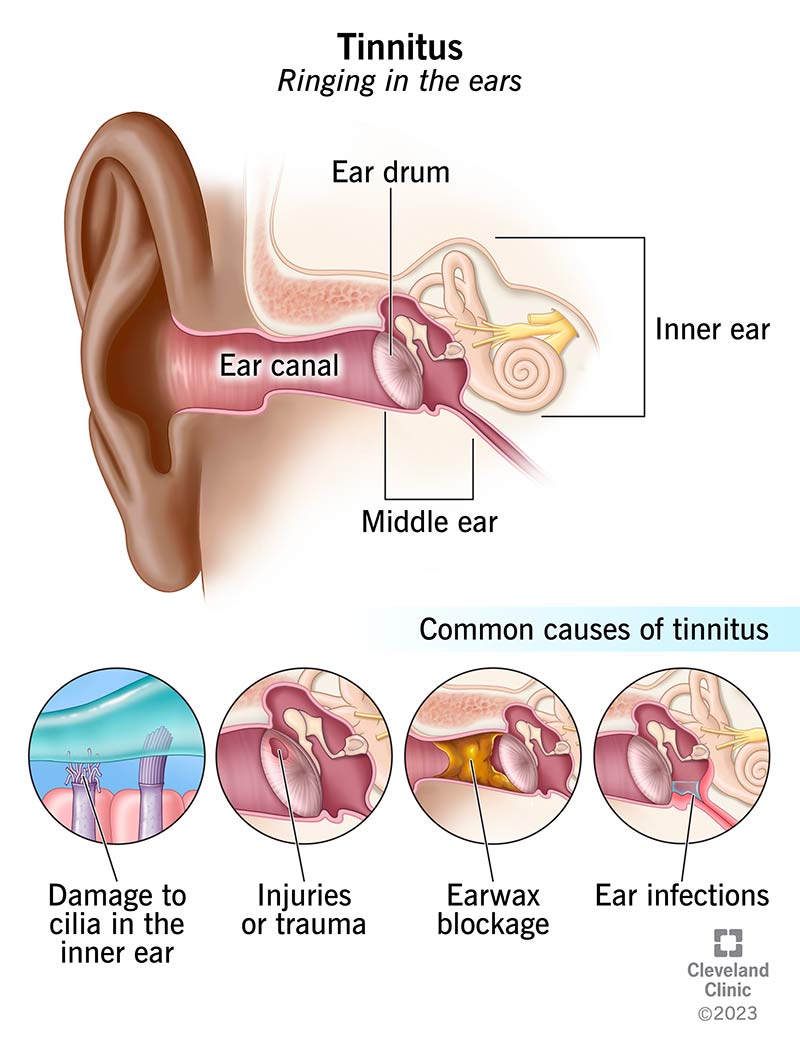
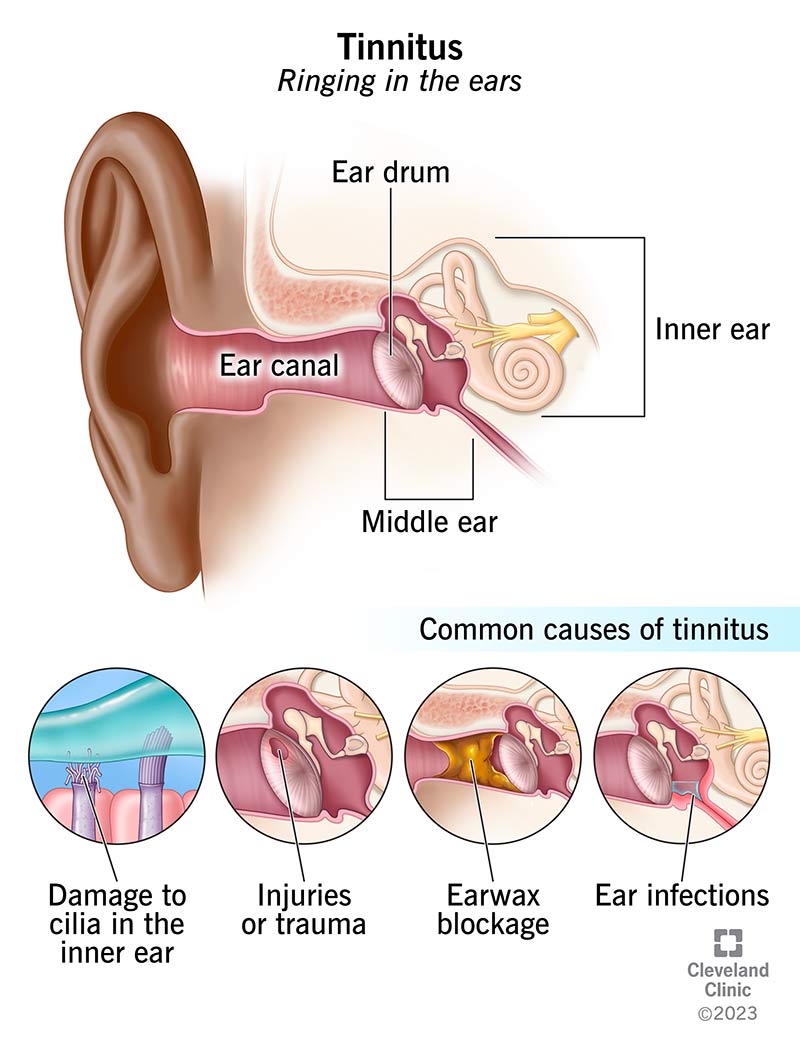
Dr. Martinez, an otolaryngologist whos published on voice disorders, notes that most patients who think they have a throat infection actually have a psychogenic component when the onset coincides with a highstress event. He emphasizes early referral to both an SLP and mentalhealth professional to prevent chronic voice loss. For patients also experiencing anxiety-related symptoms like ringing in the ears, techniques such as tinnitus meditation can be a helpful adjunct to reduce hyperarousal and improve overall treatment response.
When to Seek Help
Dont wait for the hoarseness to become a permanent part of your life. Consider reaching out if:
- Your voice has been altered for more than two weeks.
- The change interferes with work, school, or social activities.
- You experience anxiety, panic attacks, or overwhelming stress alongside the voice issue.
- You notice the problem worsening during stressful moments.
Finding the right professionals is key. Look for a boardcertified SLP who specializes in voice disorders and a psychologist experienced in CBT or traumafocused therapy. When you call, mention psychogenic dysphonia and the ICD10CM code F45.9 to ensure proper billing.
Resources & Further Reading
For those who love to dig deeper, the following sources are reliable and easy to understand:
- The American SpeechLanguageHearing Associations portal.
- PubMed article Psychogenic voice disorders and traumatic stress experience (PMID 14513954) a foundational read on the link between trauma and voice loss.
- Recent review in the International Journal of Depression & Anxiety (2024) discussing treatment outcomes.
- Support groups such as the Voice Foundations patient community and the National Alliance on Mental Illness (NAMI) forums.
Conclusion
Psychogenic dysphonia may feel like an invisible wall between you and the world, but its a wall you can climb over with the right mix of voice training, emotional care, and professional guidance. Early recognition, a thorough medical checkup, and an integrated treatment plan give you the best chance of reclaiming your voiceand the confidence that comes with it. If youve experienced sudden hoarseness, dont waitreach out to a qualified voice clinic today. And hey, if youve walked this path before, share your story in the comments; your experience could be the encouragement someone else needs.
FAQs
What is psychogenic dysphonia?
Psychogenic dysphonia is a voice disorder where emotional stress or psychological factors disrupt normal vocal function, causing voice loss without any physical damage to the vocal cords.
What are common symptoms of psychogenic dysphonia?
Symptoms include sudden hoarseness or loss of voice, breathy or strained voice quality, absence of throat pain or irritation, and voice worsening during stress but improving during relaxation.
How is psychogenic dysphonia diagnosed?
Diagnosis involves ruling out physical causes with an ENT exam and laryngoscopy, assessing voice quality with a speech-language pathologist, and psychological screening for stress or anxiety.
What treatments are effective for psychogenic dysphonia?
Treatment combines voice therapy to retrain vocal function with psychotherapy techniques like cognitive-behavioral therapy to address emotional triggers and stress management.
When should someone seek help for voice loss?
If voice changes persist longer than two weeks, interfere with daily activity, or worsen with stress, consulting professionals experienced in voice and mental health disorders is advised.