Youre looking for a clear, stepbystep guide on what to do first when caring for a patient with cystic fibrosis. Below youll find the most critical nursing actions, why they matter, and practical tips you can start using today. Lets dive in no fluff, just the essentials you need to keep your patients breathing easier, staying nourished, and feeling supported.
Airway Management
What is the top airwayrelated intervention?
Clearing the airway is the numberone priority for anyone with cystic fibrosis. Thick, sticky mucus can block the bronchi in minutes, leading to reduced oxygenation and a higher risk of infection. The best first move? A systematic chest physiotherapy (CPT) session combined with the right inhaled medications.
How do I perform chest physiotherapy safely for kids and teens?
Kids love a good story, so turn the session into a game. For infants, use gentle percussion on the back while the baby lies prone. Adolescents respond well to active cycle of breathing techniques (ACBT) think of it as a choreography of breathing, huffing, and coughing.
Chest Physiotherapy Checklist
| Step | Action | Tips |
|---|---|---|
| 1. Position | Sidelying or seated upright | Align spine, keep shoulders relaxed |
| 2. Percussion | 30second rhythmic claps over each lobe | Use cupped hands, avoid bones |
| 3. Vibration | Gentle shaking for 1015 seconds | Focus on areas with crackles |
| 4. Postural Drainage | Hold each position 510 minutes | Gravity helps mucus flow |
| 5. Breathing Exercise | Inhale deeply, hold 23 sec, exhale with huff | Repeat 35 cycles |
When should bronchodilators and hypertonic saline be used together?
If the patient shows wheezing or has a recent decline in spirometry, give a shortacting bronchodilator (e.g., albuterol)510minutes before nebulized hypertonic saline (37%). The bronchodilator opens the airways, allowing the saline to draw out the mucus more effectively.
RedFlag Signs for Worsening Obstruction
- Increased work of breathing (retractions, nasal flaring)
- SpO dropping below 92% despite supplemental O
- New or worsening cough thats not productive
Infection Control
Which nursing actions most reduce respiratory infections?
Hand hygiene is the backbone, but with CF patients we add a few layers: mask use during aerosolgenerating procedures, thorough equipment disinfection, and strict isolation when a new pathogen is identified.
How can I teach families about handhygiene and aerosol precautions?
Start with a quick demo: soap and water for 20 seconds, or an alcoholbased sanitizer if hands are dry. Then roleplay a clinic visit where the family practices putting on a surgical mask correctly and handling nebulizer tubing without crosscontamination.
What role do prophylactic antibiotics play in daily care?
Many CF centers prescribe oral azithromycin three times a week to curb Pseudomonas colonisation. The nurses job is to ensure the dose is taken consistently, check for GI upset, and document any sideeffects.
InfectionControl Protocol (CDC guidance)
- Handwash before and after patient contact
- Wear a surgical mask when performing nebulizer treatments
- Disinfect nebulizer mouthpieces with 70% alcohol after each use
- Use contact precautions if for multidrugresistant organisms
Case Vignette: HospitalAcquired Pseudomonas
Eightyearold Maya was admitted for a flare. After a week, her sputum culture grew a new strain of Pseudomonas. The bedside nurse initiated droplet precautions, educated the family on strict hand hygiene, and coordinated with the respiratory therapist to adjust her inhaled antibiotics. Within three days, Mayas fever subsided and her lung sounds cleared. This story highlights how rapid infection control can turn the tide.
Oral vs. Inhaled Antibiotics (Comparison)
| Route | Typical Drug | Benefits | Common Sideeffects |
|---|---|---|---|
| Oral | Azithromycin | Systemic coverage, easy adherence | GI upset, QT prolongation |
| Inhaled | Tobramycin | High concentration at infection site | Cough, ototoxicity |
Nutritional Support
What are the priority nutritionrelated nursing interventions?
Because CF patients burn calories faster, the nurse must ensure they receive 110150% of their recommended daily allowance. That means highprotein, highcalorie meals, plus pancreatic enzyme replacement with every feed.
How do I assess and document caloric intake accurately?
Use a simple foodfrequency chart. Record everything the patient eatssnacks count! Compare the total to the prescribed caloric goal and flag any gaps.
When should pancreatic enzyme replacement be reinforced?
Anytime the patient eats a meal containing fat, protein, or carbohydrates. The typical dosage is 5002500IU lipase per gram of fat, adjusted for age and weight. The nurse should watch for steatorrhea (fatty stools) as a sign the dose is too low.
Daily Nutrition Assessment Tool
| Parameter | Target | Notes |
|---|---|---|
| Weight | Maintain or gain 0.51kg/mo | Track weekly |
| Calories | 110150% RDA | Log each meal |
| FatSoluble Vitamins | A, D, E, K within normal range | Lab check q36mo |
Nutrition Education Handout for Schools
When a child with CF returns to class, the nurse can give teachers a onepage sheet covering: 1) snack timing (every 34hours), 2) allowance for extra calories during PE, and 3) emergency plan if the child vomits after a dose of enzymes. This aligns with the cystic fibrosis care plan for school many families request.
Evidence Snapshot
A 2022 study in the Journal of Cystic Fibrosis showed that patients who met 120% of their caloric goal grew 0.8cm taller per year and had a 15% lower rate of pulmonary exacerbations ().
Psychosocial Education
What teaching points should a nurse cover in the first 24hours?
Start with the basics: how to use the inhaler, why enzymes matter, and the importance of hand hygiene. Then move to what to expect normal sideeffects, when to call the doctor, and how to keep a symptom diary.
How do I tailor education for adolescents vs. younger children?
Teens appreciate autonomy. Give them a checklist they can tick off on their phone. Younger kids respond better to visual aidsthink colorful stickers on a MucusMonster chart that tracks daily airway clearance.
When should I refer to a multidisciplinary CF team?
Any sign of psychosocial distressdeclining school attendance, chronic anxiety about treatments, or family conflictwarrants a referral to the social worker or psychologist on the CF team.
TeachBack Script for Medication Adherence
Nurse: Can you walk me through how youll take your inhaled antibiotics tonight?
Patient: repeats steps.
Nurse: Great, thats exactly right. If anything feels off, give me a call.
Community Resources
- Cystic Fibrosis Foundation (online support groups)
- Local CF camp programs
- Nutrition counseling at your nearest university clinic
RealWorld Example
When I cared for 12yearold Luis, his mother was overwhelmed by the medication schedule. We spent a halfhour building a colorful wallcalendar together, assigning each medication a color. Within a week, Luis was proudly checking off each dose himself, and his adherence jumped from 60% to 95%.
Monitoring & Documentation
Which vital signs and labs need daily review?
SpO, respiratory rate, temperature, and body weight are musthaves. Lab work should include CBC, sputum culture, and serum levels of fatsoluble vitamins.
How do I document the effectiveness of each intervention?
Use the SOAP format: Subjective (patient reports feeling less short of breath), Objective (SpO improved from 89% to 94% after CPT), Assessment (airway clearance effective), Plan (continue twicedaily CPT).
When is escalation to the physician indicated?
If any of the following occur: SpO<88% despite O, temperature>38.5C for >24hrs, or a new sputum organism. Prompt notification can prevent a fullblown exacerbation.
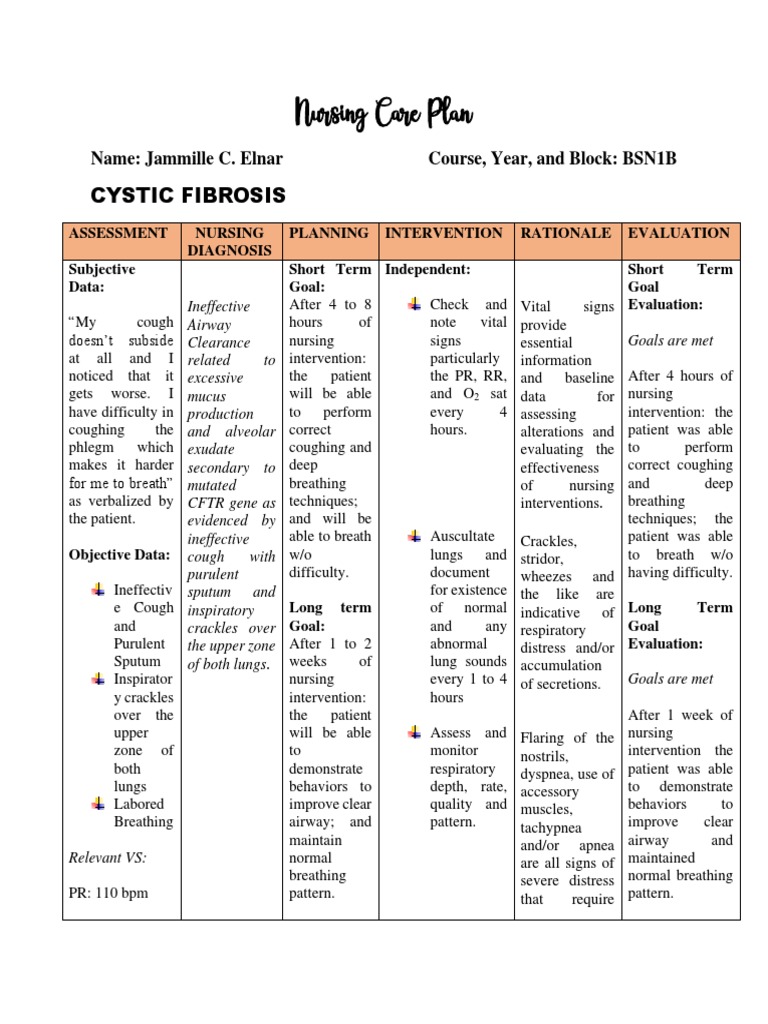
NANDA Nursing Diagnosis List for CF
- Impaired Gas Exchange
- Risk for Infection
- Imbalanced Nutrition: More Than Body Requirements
- Anxiety
- Deficient Knowledge
Nursing FlowChart Example
| Diagnosis | Intervention | Expected Outcome | Evaluation |
|---|---|---|---|
| Impaired Gas Exchange | Chest physiotherapy + bronchodilator | SpO94% within 30min | Documented SpO rise |
| Risk for Infection | Hand hygiene + mask | No new fever for 48hrs | Temperature chart |
| Imbalanced Nutrition | Highcalorie diet + enzymes | Weight gain0.5kg/mo | Weekly weight log |
Medication Overview
What are the cornerstone medications for CF?
Typical regimens include: CFTR modulators (e.g., ivacaftor), inhaled antibiotics (tobramycin), bronchodilators (albuterol), hypertonic saline, and pancreatic enzymes. Each serves a distinct purposesome open the airway, others fight infection, and a few help the pancreas digest food.
Key nursing considerations for nebulized antibiotics vs. oral therapies?
For nebulized drugs, watch for bronchospasm during the first five minutes and be ready with a rescue inhaler. Oral meds require checking liver function tests regularly and ensuring the patient takes them with food to improve absorption.
How to monitor for adverse effects?
Common red flags: ringing in ears (ototoxicity) with tobramycin, persistent cough with hypertonic saline, and skin rash with CFTR modulators. Document any new symptom and notify the prescriber promptly.
Medication Matrix
| Drug | Route | Typical Dose | Monitoring | Patient Teaching |
|---|---|---|---|---|
| Ivacaftor | Oral | 150mg PO BID | Liver enzymes q3mo | Take with fatty meal |
| Tobramycin | Inhaled | 300mg nebulized BID | Audiogram quarterly | Rinse mouth after use |
| Albuterol | Inhaler | 2 puffs q46hr PRN | Pulse, tremor | Use spacer, hold breath 10sec |
| Pancreatic Enzymes | Oral | 5002500IU lipase per gram fat | Stool consistency | Take with every meal/snack |
Conclusion
In the world of cystic fibrosis care, the nurses checklist is lifechanging. By focusing on airway clearance, rigorous infection control, tailored nutrition, compassionate education, and vigilant monitoring, you set the stage for better lung function, steady growth, and a brighter outlook for your patients. Remember, every small actionwhether its a gentle chest percussion or a friendly reminder about enzymesadds up to a healthier, happier life for the person youre caring for.
For practical guidance on preparing patients for common procedures and optimizing recovery after interventions, nurses may also find resources on post op recovery helpful for example, a concise post op recovery checklist can guide discharge teaching and shortterm monitoring post op recovery.
Keep this guide handy, share it with your team, and lets keep those lungs clear together.
FAQs
What are the most critical airway nursing interventions for cystic fibrosis?
The top priority is airway clearance using chest physiotherapy (CPT), including percussion, vibration, postural drainage, and breathing exercises—all aimed at mobilizing and removing thick mucus from the lungs[1][2][3].
How can nurses help prevent infections in cystic fibrosis patients?
Nurses should enforce strict hand hygiene, mask use during aerosol-generating procedures, and proper disinfection of equipment. They also administer prophylactic antibiotics as prescribed and monitor for early signs of infection[1][3].
What nutritional support is essential for cystic fibrosis patients?
Patients need high-calorie, high-protein meals, pancreatic enzyme replacement with every meal or snack, and regular monitoring of weight and fat-soluble vitamin levels to support growth and prevent malnutrition[1][5].
Which medications are most important in cystic fibrosis management?
Key medications include CFTR modulators, inhaled antibiotics, bronchodilators, hypertonic saline, and pancreatic enzymes. Each addresses different aspects of the disease, from mucus clearance to infection control and nutrient absorption[3][5].
How should nurses support the psychosocial needs of cystic fibrosis patients?
Nurses should provide age-appropriate education, emotional support, and involve the patient and family in care decisions. Referrals to social work or mental health services are important if distress or adherence issues arise[1].