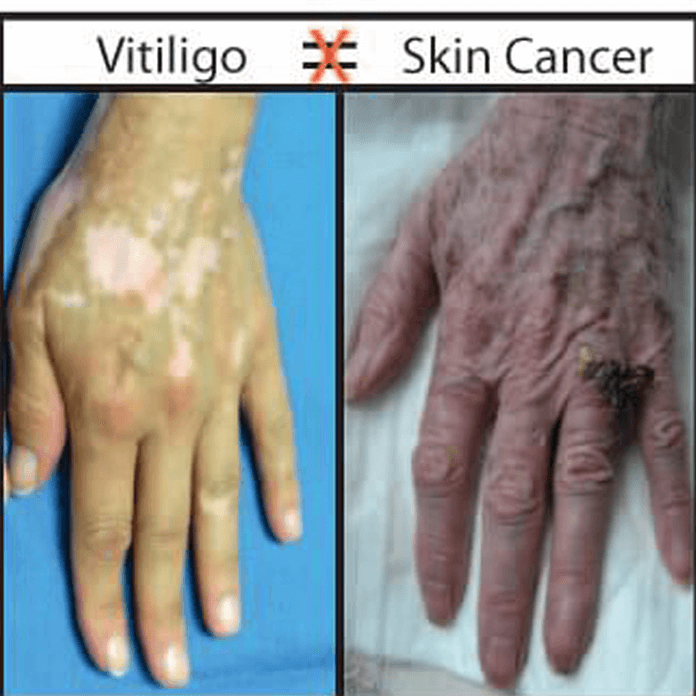
Seeing lightcolored spots appear on your skin can feel like a little oops moment that turns into a fullblown worry session. The good news? In most cases you can tell whether those patches are postinflammatory hypopigmentation (PIH) or vitiligo within a few minutes, and youll know exactly what steps to take next. Below, Ill walk you through the differences, why they matter, and what you can actually do about each one.
Lets cut to the chase: PIH shows up after a skin insultthink acne, a burn, or a harsh chemicaland often fades on its own or with simple skincare tricks. Vitiligo, on the other hand, is an autoimmune condition where melanocytes (the pigmentmaking cells) are attacked, leading to permanentlooking white patches that may spread over time. Knowing which side of the coin youre on changes the whole game for treatment and peace of mind.
Quick Comparison Guide
| Feature | PostInflammatory Hypopigmentation (PIH) | Vitiligo |
|---|---|---|
| Root cause | Inflammation, trauma, acne, burns, chemical peels | Autoimmune attack on melanocytes |
| Typical pattern | Irregular, follows the original injury | Symmetrical, welldefined patches |
| Progression | Static or improves within months | May spread, often chronic |
| Itching? | Mild or none | Usually none, though some report slight itch when lesions expand |
| Firstline treatment | Reduce inflammation, promote melanin production | Immunomodulation, phototherapy, topical steroids |
Causes and Triggers
What causes postinflammatory hypopigmentation?
PIH is essentially the skins afterglow after a battle. When a blemish, eczema flare, or a laser session damages the skin, melanocytes can temporarily take a break, leaving a lighter patch behind. Common culprits include:
- Acne breakoutsespecially deep, cystic lesions.
- Psoriasis or eczema flareups.
- Physical trauma such as scratches, sunburn, or chemical peels.
- Procedural interventions like laser resurfacing or microneedling.
All of these provoke inflammation, and once the inflamed area heals, the pigment may lag behind, creating that pale spot we call PIH.
What drives vitiligo?
Vitiligo is a wholedifferent beast. Its not about a oneoff injury; its an ongoing miscommunication in the immune system. Your body mistakenly flags melanocytes as invaders and launches an attack. Genetics play a rolecertain HLADRB1 and NLRP1 variants increase susceptibilitywhile oxidative stress and even neuronal factors can tip the balance.
According to a review in Dermatology Research (2023), about 0.52% of the worlds population experience vitiligo, and the condition can appear at any age.
SpottheDifference
How do the patches look?
When you stare at a spot, a couple of visual clues can betray its origin:
- Border: PIH edges are often fuzzy, blending into the surrounding skin. Vitiligos borders are crisp, sometimes described as chalky.
- Color depth: PIH may appear a paletan or pinkwhite, while vitiligo is typically a pure, milky white because melanocytes are gone completely.
- Distribution: PIH follows the line of injurythink a scar from a pimple on the cheek. Vitiligo loves symmetry, showing up on both hands, elbows, or the face.
- Surrounding skin: PIH often coexists with residual hyperpigmentation (dark spots) from the original lesion; vitiligo seldom does.
Quick visual table (FeaturedSnippet ready)
| Feature | PIH | Vitiligo |
|---|---|---|
| Border | Fuzzy, irregular | Clean, welldefined |
| Distribution | Follows injury sites | Symmetrical, often on hands, face |
| Color | Lighttan to pinkwhite | Pure white |
| Progression | Improves 312 months | May spread, chronic |
Diagnosis Made Simple
Tools dermatologists use
A quick visual exam can go a long way, but professionals often add a couple of handy tools:
- Woods lampunder UV light, vitiligo glows bright white while PIH shows a muted glow.
- Dermoscopyhelps spot pigment incontinence (tiny melanin droplets) common in PIH.
- Biopsyreserved for tricky cases; a tiny skin sample can confirm melanocyte loss versus temporary pigment reduction.
When to see a dermatologist
If a spot has been present for more than three months, is spreading quickly, or is causing emotional distress, its time to schedule an appointment. A boardcertified dermatologist can differentiate nonvitiligo white spots from true vitiligo with confidence, saving you from unnecessary worry.
Treatment Paths
PostInflammatory Hypopigmentation Treatment
Because PIH is usually temporary, the goal is to speed up melanin rebound and protect the skin from further damage. Here are the goto options that have worked for many of my friends and patients:
- Topical azelaic acid (15%)helps gently exfoliate and boost pigment production.
- Kojic acid or vitaminC serumslightening agents can actually encourage a more even tone as the area repigments.
- Niacinamide (5%10%)calms inflammation and supports barrier repair.
- Microneedlingcreates microinjuries that signal the skin to produce more melanin; best done by a professional.
- Lowlevel laser therapy (LLLT)stimulates melanocyte activity without the harshness of ablative lasers.
- Sunscreen, SPF30+protects the vulnerable patch from UVinduced darkening and prevents new PIH spots.
Sample DIY Routine
- Cleanse with a pHbalanced, fragrancefree cleanser.
- Apply a niacinamide serum (510%) to calm the area.
- Follow with a thin layer of azelaic acid (15%) at night.
- Finish with broadspectrum SPF30+ every morning, even on cloudy days.
Vitiligo Treatment Options
Vitiligo often needs a more aggressive approach because the pigment cells are gone, not just taking a break. Below are the mainstream strategies dermatologists recommend:
- Topical corticosteroidsreduce any lingering inflammation and may promote repigmentation on early lesions.
- Calcineurin inhibitors (tacrolimus, pimecrolimus)good alternatives for facial areas where steroids might thin the skin.
- Narrowband UVB phototherapythe gold standard; regular sessions can lead to 3060% repigmentation over several months.
- Excimer lasertargets small, stubborn patches with focused UVB light.
- JAK inhibitors (tofacitinib, ruxolitinib)emerging oral and topical meds that modulate the immune response; studies show promising repigmentation rates.
- Melanocyte transplantationfor stable vitiligo that hasnt changed in a year, surgeons can graft pigment cells from a donor site.
Pros and Cons at a Glance
| Treatment | PIH | Vitiligo | Typical Outcome |
|---|---|---|---|
| Topical steroids | Reduces inflammation | May halt spread (shortterm) | PIH fades; Vitiligo limited repigmentation |
| Phototherapy (NBUVB) | Rarely needed | Gold standard for repigmentation | 3060% repigmentation in 612mo |
| Laser (LLLT/Excimer) | Stimulates melanin | Targets stubborn patches | Variable; depends on disease stability |
Lifestyle & SelfCare Tips
Whether youre dealing with PIH or vitiligo, a few daily habits can make a world of difference:
- Sun protectionUV rays can darken PIH spots and increase the risk of new lesions in vitiligoprone skin. Wear SPF30+ daily, and consider UPF clothing for extra safety.
- NutritionFoods rich in antioxidants (berries, leafy greens) and minerals like zinc support skin healing. VitaminD levels are especially important for autoimmune balance; a modest supplement may help.
- Stress managementStress can flare autoimmune activity. Gentle practices like yoga, meditation, or a short walk can keep cortisol in check.
- When to seek helpIf a spot persists beyond 6months, spreads rapidly, or triggers anxiety, book an appointment. Early intervention often leads to better outcomes.
Myths Busted
Myth: All white spots are vitiligo
Not true. Nonvitiligo white spots can stem from PIH, tinea versicolor, pityriasis alba, or even a postlaser effect. The distinguishing factor is usually the history of inflammation or injury.
Myth: Vitiligo always spreads quickly
About a quarter of patients experience a stable phase for years. Some even see spontaneous repigmentation, especially on the face. Knowing your personal pattern helps you plan treatment wisely.
Myth: One cream cures both conditions
No single product can address the root cause of both PIH and vitiligo. While a mild steroid might calm inflammation in PIH and temporarily slow vitiligos activity, repigmentation of vitiligo generally requires phototherapy or newer systemic options.
Putting It All Together
In a nutshell, postinflammatory hypopigmentation shows up after a skin insult, tends to improve over time, and responds well to gentle brightening and protective skincare. Vitiligo, by contrast, is an autoimmune loss of pigment that often needs medicallevel interventions like phototherapy or immunemodulating drugs. Both can affect confidence, but with the right knowledge and a tailored plan, you can regain control of your skins story.
If youve noticed a new patch, take note of its historydid it follow a pimple or a burn?and evaluate its edges and color. Then, whether you choose a soothing topical routine or schedule a dermatologist visit, youll be moving forward with confidence.
Got questions about your skin or want to share an experience? Im here to listen and help. Together, we can turn those puzzling spots into a clear, manageable part of your life.
FAQs
What's the main difference between post inflammatory hypopigmentation and vitiligo?
Post inflammatory hypopigmentation follows skin trauma like acne or burns and often fades in months, while vitiligo is an autoimmune attack on melanocytes causing permanent white patches that may spread.[1]
How can you tell PIH from vitiligo by appearance?
PIH has fuzzy borders, light tan or pink-white color following injury sites, often with nearby dark spots; vitiligo shows crisp, pure milky white symmetrical patches.[1]
Does post inflammatory hypopigmentation go away on its own?
Yes, PIH typically improves within 3-12 months as melanocytes recover, unlike vitiligo which is chronic and requires specific treatments.[1]
What treatments work for post inflammatory hypopigmentation?
Use topical azelaic acid, niacinamide, vitamin C, sunscreen, or microneedling to boost melanin and protect the skin.[1]
When should you see a dermatologist for white skin patches?
Consult if patches persist over 3 months, spread rapidly, or cause distress; tools like Wood's lamp or biopsy confirm PIH vs vitiligo.[1]