Hey there! If youve ever wondered why you sometimes hear doctors talk about OHS and OSA as if theyre twins, youre not alone. In a nutshell, obesity hypoventilation syndrome (OHS) is a chronic condition that keeps your blood gas levels off even when youre awake, while obstructive sleep apnea (OSA) mainly hijacks your breathing at night. Both love to show up together, especially when excess weight is in the picture, but they each demand its own playbook. Lets break it all down in plain language, so you can figure out whats really going on with your body.
Quick Answer Snapshot
Whats the quick take? OHS is a daytime breathing disorder that causes high carbondioxide (CO) and low oxygen (O) levels, whereas OSA is a nighttime airwaycollapse problem that leads to snoring, pauses, and daytime sleepiness. If you have OHS, youll likely need more than the standard CPAP machine that usually fixes OSA.
What Is OHS?
Definition & Pickwickian Name
Obesity hypoventilation syndrome (sometimes called Pickwickian syndrome) is defined by three core features: a bodymassindex (BMI) of30kg/m or higher, daytime hypercapnia (PaCO>45mmHg), and the exclusion of other causes of hypoventilation. The Pickwickian triad obesity, hypoventilation, and sleepdisordered breathing is where the old nickname comes from.
Obesity Hypoventilation Syndrome Criteria
To diagnose OHS you need to check off these boxes:
- BMI30kg/m (often >35kg/m in severe cases)
- Daytime arterial CO >45mmHg on at least two separate measurements
- Absence of alternative explanations like COPD, neuromuscular disease, or chest wall deformities
Typical Symptoms
People with OHS often report a mix of day and nighttime complaints. During the day you might feel:
- Persistent fatigue, even after a full nights sleep
- Morning headaches that fade as the day goes on
- Shortness of breath after climbing a flight of stairs
- A vague air hunger sensation
At night the picture looks a lot like OSA: loud snoring, witnessed pauses, and restless sleep that leaves you exhausted in the morning.
RealWorld Example
Take John, a 52yearold accountant with a BMI of38. He thought his snoring was just a typical OSA problem, but when his doctor ordered an arterial blood gas test, the results showed a PaCO of52mmHg. That single number shifted his treatment plan from a simple CPAP to a BiPAP machine and a structured weightloss program. Stories like Johns illustrate why recognizing OHS matters.
What Is OSA?
Definition & Prevalence
Obstructive sleep apnea (OSA) occurs when the upper airway collapses repeatedly during sleep, causing 5 or more apneahypopnea events per hour. Its surprisingly commonabout 1 in 5 adults in the U.S. have moderatetosevere OSA, and the numbers climb steeply when obesity enters the mix.
Core Symptoms
- Loud, chronic snoring
- Witnessed breathing pauses or choking sensations
- Excessive daytime sleepiness (often measured by the Epworth Sleepiness Scale)
- Morning dry mouth or sore throat
Standard Diagnostic Workup
Polysomnography (overnight sleep study) remains the gold standard. In many cases a home sleeptesting device can also capture the apneahypopnea index (AHI) needed for diagnosis. The test tells you how many breathing interruptions happen per hour, which guides treatment intensity.
Quick Fact Box
- Prevalence rises to90% in people with OHS
- Risk factors: high BMI, male sex, age>40, neck circumference>17cm
- Firstline therapy: continuous positive airway pressure (CPAP)
Direct Comparison Table
| Feature | Obesity Hypoventilation Syndrome (OHS) | Obstructive Sleep Apnea (OSA) |
|---|---|---|
| Primary Problem | Chronic daytime hypoventilation hypercapnia & hypoxemia | Intermittent upperairway collapse nighttime events |
| Daytime BloodGas Abnormality | Yes (PaCO, PaO) | Usually normal |
| Typical BMI | >30kg/m (often >35) | Elevated but can be lower |
| Key Diagnostic Test | Arterial blood gas + sleep study | Sleep study alone |
| Firstline Treatment | BiPAP/ASV, weightloss, oxygen if needed | CPAP |
| Mortality Risk (Untreated) | Higher risk of pulmonary hypertension, heart failure | Elevated but lower than OHS |
Overlap vs Distinct Entities
While OHS can exist without OSA, the two love to cooccur. Studies show up to 88% of OHS patients also meet OSA criteria. Think of OSA as a nighttime sidekick that often aggravates OHS, but its not the whole story.
WhatIf Scenarios
- Can CPAP alone treat OHS? In many cases, CPAP helps but often falls short because it doesnt adequately offload CO. BiPAP or adaptive servoventilation (ASV) is usually recommended.
- Is bariatric surgery curative? Weightloss surgery can dramatically improve both conditions, especially when BMI>40. It isnt a guaranteed cure, but many patients see a reduction in AHI and a normalization of daytime PaCO.
Treatment Options Overview
FirstLine PAP Therapy
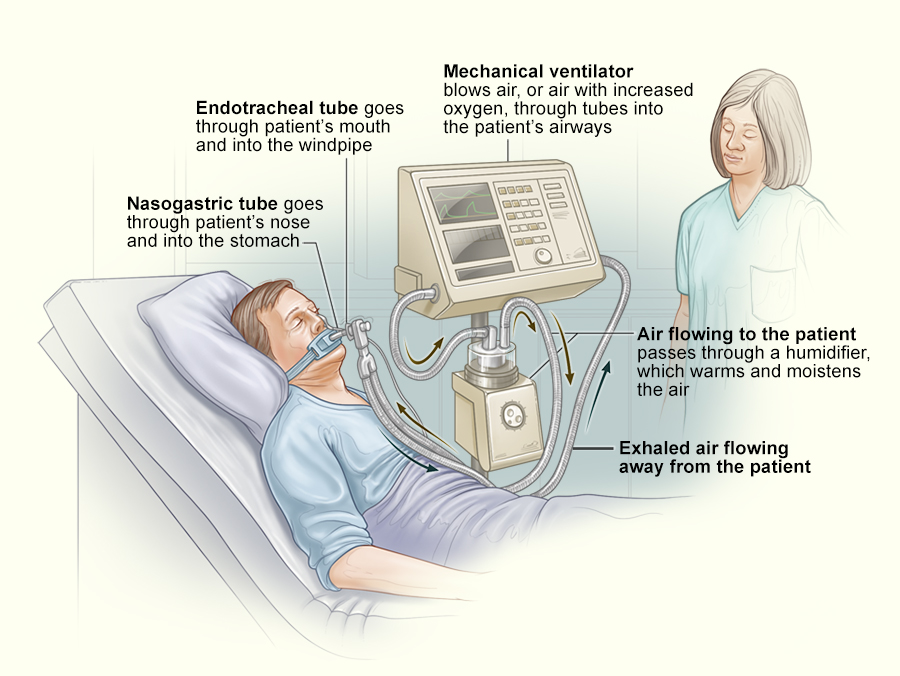
For pure OSA, a CPAP (continuous positive airway pressure) machine keeps the airway open. When OHS is in the mix, clinicians typically step up to BiPAP (bilevel) or ASV, which provides higher pressure support during inhalation and can better wash out excess CO.
Lifestyle & WeightManagement
Weight loss is the cornerstone of both disorders. A structured lowcalorie diet, regular aerobic exercise, andwhen appropriatebariatric surgery can lower AHI scores and improve daytime gas exchange. The gives a handy visual guide on combining diet, activity, and behavioral coaching.
Pharmacologic & Adjunct Therapies
- Supplemental nocturnal oxygen for severe hypoxemia (but only after PAP is optimized).
- Diuretics if pulmonary hypertension develops.
- Rarely, respiratory stimulants like acetazolamide, under specialist supervision.
StepbyStep Guide
- Confirm diagnosis with ABG and sleep study.
- Start appropriate PAPCPAP for OSA, BiPAP/ASV for OHS.
- Enroll in a supervised weightloss program.
- Recheck daytime PaCO after 24weeks of PAP therapy.
- Adjust treatment based on followup labs and symptoms.
Expert Tip Box
A drop of >5mmHg in PaCO after 24weeks of PAP is a strong predictor of longterm success, notes Dr. Patel, a pulmonology specialist at a major sleep center. Keeping track of that number can help you and your doctor know whether youre on the right track.
When to Seek Help
RedFlag Checklist
- Morning headaches that dont go away
- Confusion, memory lapses, or unusual mood changes
- Shortness of breath at rest or with minimal activity
- Swelling in ankles or sudden weight gain (signs of rightheart strain)
- Worsening daytime sleepiness despite regular PAP use
Patient Story
Maria, a 47yearold teacher, ignored her escalating fatigue for years. When she finally visited the ER with severe shortness of breath, a blood gas revealed PaCO=58mmHg. She was diagnosed with OHS, started BiPAP, and entered a multidisciplinary weightloss program. Within six months, her energy returned, and her blood gases normalized. Her experience underscores how crucial early recognition is.
Key Takeaways Summary
To wrap things up, heres what you should walk away with:
- OHS OSA. OHS adds daytime hypercapnia and a higher mortality risk.
- Most people with OHS also have OSA, but treatment must address both.
- CPAP may fix OSA; BiPAP/ASV plus weight loss are usually needed for OHS.
- Monitoring daytime CO levels is essential to gauge treatment success.
- Dont wait for redflag symptomsearly evaluation can prevent complications.
If any of this resonates with youor if youve noticed some of the symptoms mentionedconsider chatting with a sleepmedicine specialist. A simple blood test and a nighttime sleep study can reveal a lot, and taking action now could dramatically improve your quality of life. Were all in this together, and staying informed is the first step toward breathing easier.
FAQs
What is the main difference between obesity hypoventilation syndrome and OSA?
Obesity hypoventilation syndrome (OHS) features chronic daytime hypercapnia (PaCO2 >45 mmHg) and hypoxemia even when awake, while obstructive sleep apnea (OSA) primarily involves nighttime upper airway collapses without daytime blood gas abnormalities.[1][5]
Do all OHS patients have OSA?
No, OHS can occur without OSA, but up to 90% of OHS patients also have OSA, making overlap common especially in severe obesity.[2][3]
How is OHS diagnosed differently from OSA?
OHS diagnosis requires BMI ≥30 kg/m², daytime PaCO2 >45 mmHg on two measurements, and exclusion of other causes, plus a sleep study; OSA uses sleep study alone for apnea-hypopnea index.[1][5]
What treatment is used for OHS versus OSA?
OSA is typically treated with CPAP; OHS often needs BiPAP or ASV for better CO2 clearance, plus weight loss and sometimes oxygen, as CPAP alone may be insufficient.[1][2]
Who is at higher risk for OHS compared to OSA?
OHS requires obesity (BMI often >35-40 kg/m²) and affects those with impaired respiratory drive; OSA can occur in non-obese people but prevalence rises with obesity.[2][5]