Whats a normal cervix MRI anyway? Imagine a highdefinition photo of the neck of your uterus where everything looks just rightno lumps, no weird signals, just the smooth, healthy tissue that doctors expect. In the next few minutes youll get the lowdown on what the scan shows, why the exact protocol matters, and how you can read those images without feeling lost in medical jargon.
Why does this matter to you? Knowing what normal looks like gives you confidence when you talk to your radiologist, helps spot problems early, and lets you weigh the benefits and risks of the examespecially if you ever need a more detailed scan for cancer staging or treatment planning. Lets dive in, friend to friend.
Why Normal Matters
What does normal look like on MRI?
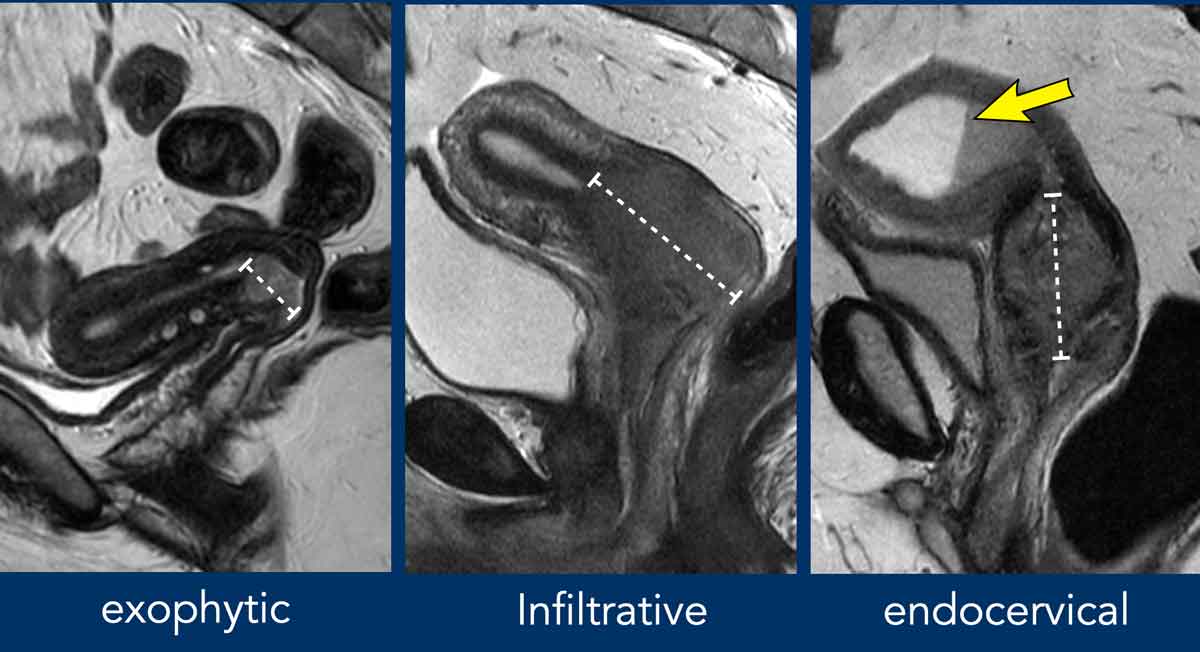
On a typical T2weighted image the cervix shows three distinct zones:
- Endocervical canal bright (hyperintense) because its filled with fluid.
- Cervical stroma a darker, uniform ring surrounding the canal.
- Outer border (external os) a smooth transition to the vagina and uterus.
This pattern is the baseline radiologists compare everything else against. According to , the stromas low signal on T2 gives the cervix its characteristic dark ring thats easy to spot when everythings healthy.
Key anatomical landmarks every radiologist checks
When we talk about the cervix on MRI, a few landmarks keep popping up:
- Endocervical canal runs the length of the cervix, appears bright on T2.
- Fibrous stroma the sturdy, lowsignal tissue that provides structural support.
- External os the opening to the vagina, should be patent and smooth.
- Uterine arteries faint flow voids that you can see on T1postcontrast if a contrast study is done.
Keeping these in mind turns a pretty picture into a useful diagnostic tool.
Typical MRI parameters for a healthy cervix
Heres a quick cheatsheet of the technical settings most centers use for a routine normal cervix study:
| Parameter | Typical Value |
|---|---|
| Field strength | 1.5T or 3T |
| Slice thickness | 3mm with 0mm gap |
| Sequence | T2weighted sagittal & axial, T1pre/postcontrast if needed |
| Fat saturation | Yes, for T2 to improve contrast |
These numbers arent set in stone, but theyre a solid starting point for any technologist aiming for a clear picture.
MRI Protocol Basics
Patient preparation
Before the scan, patients are usually asked to:
- Empty the bladder (helps reduce artefacts).
- Fast for a couple of hours if contrast will be used.
- Schedule the exam in the midfollicular phase of the menstrual cycle (around days710) for the most consistent cervical thickness, as shown in a study on healthy volunteers.
These simple steps can dramatically improve image quality and make the radiologists job easier.
Sequence lineup: From localizer to highresolution T2
A typical normal cervix protocol runs like this:
- Localizer quick scout to confirm positioning.
- T2weighted sagittal gives an overview of uterine axis.
- T2weighted axial the workhorse for cervical anatomy.
- T1 precontrast baseline for any future enhancement.
- Dynamic contrast (optional) only if a lesion is suspected.
Normal vs. Cancer Staging Protocol (quick comparison)
| Feature | Normal Cervix MRI | Cervical Cancer MRI Staging |
|---|---|---|
| Slice thickness | 3mm | 2mm (higher resolution) |
| Contrast | Usually no | Dynamic T1postcontrast |
| Sequences | T2+optional T1 | T2, DWI, ADC, and contrastenhanced T1 |
Notice the extra diffusionweighted imaging (DWI) and tighter slices in the staging protocoleverything is designed to catch subtle tumour spread.
Common pitfalls & artifacts to watch for
Even the best technologist can run into hiccups:
- Motion blur Ask the patient to breathe shallowly and stay still.
- Bowel gas A light bowel prep can reduce susceptibility artefacts.
- Coil positioning The pelvic coil should hug the pelvis snugly; a loose coil leads to signal loss.
When you hear the technologist say lets take a quick break, its usually to fix one of these issues, not because theyre being slow.
Reading the Scan
Spotcheck checklist for radiologists & clinicians
| Step | What to look for | Normal appearance |
|---|---|---|
| 1 | Endocervical canal | Bright on T2, smooth, no focal thickening |
| 2 | Cervical stroma | Uniform low signal, no irregular borders |
| 3 | External os | Patent, no obstruction, clear transition |
| 4 | Adjacents (uterus, vagina, parametria) | Symmetric, no mass effect, normal signal |
If anything looks out of placesay a focal highsignal noduleits worth a deeper look.
When normal raises a red flag
Here are a few almostnormal findings that can hint at something else:
- Asymmetry of the stroma may suggest a benign polyp or early neoplasia.
- Focal highsignal area on T2 think of a cervical polyp; calls this the classic bright spot that enhances mildly after contrast.
- Irregular outer border could indicate stromal invasion; a red flag for cervical cancer radiology staging.
For example, a clinician considering causes of focal highsignal regions might also review gynecologic topics such as pelvic pain endometriosis when correlating MRI findings with a patients symptoms, since endometriosis can sometimes produce pelvic masses or atypical signals.
Minicase study
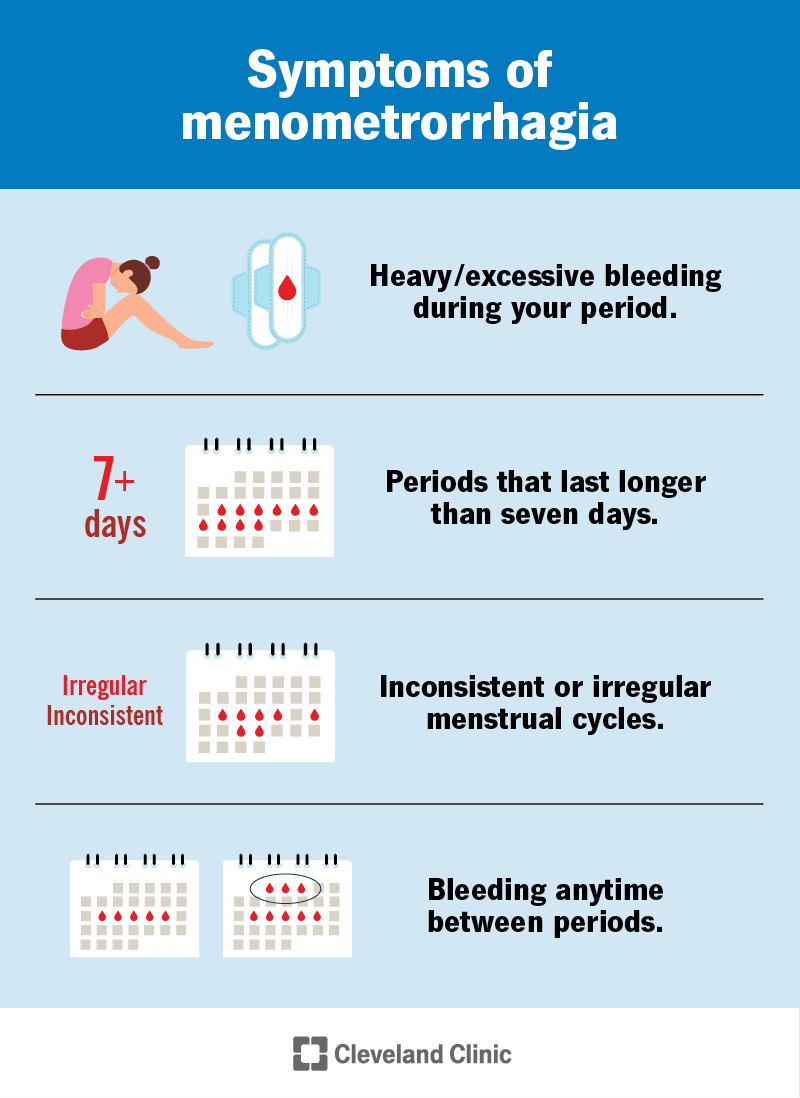
Maria, 34, came in for a routine check because shed had some irregular spotting. Her MRI was ordered just to be safe. The images showed a perfectly smooth stroma, but a tiny 6mm hyperintense nodule in the endocervical canal. The radiologist identified it as a benign polyp, and Maria avoided an unnecessary biopsy. Stories like this highlight why understanding the normal baseline matters.
From Normal to Disease
How normal anatomy underpins cervical cancer MRI staging
When cancer creeps in, it disrupts the tidy layers we just described. The lowsignal stromal ring is often replaced by a heterogeneous, highersignal mass that may invade the parametria. According to the , the contrast between bright tumour tissue and dark stroma makes MRI the gold standard for local staging (stageIBIIA).
Role of normal MRI in treatment planning
Radiation oncologists rely on the clear delineation of healthy cervix tissue to contour treatment fields. A normal cervix scan becomes the baseline map, and any deviation tells the planner where to boost the dose or spare nearby organs. This is why the cervix MRI planning step is a bridge between diagnosis and therapy.
Flowchart: Normal Suspicious Targeted protocol Staging Management
- Start with a normal cervix MRI (baseline).
- If an abnormality appears, order a targeted protocol (add DWI, contrast).
- Radiologist stages the tumour using the FIGO system.
- Multidisciplinary team decides on surgery, radiotherapy, or chemoradiation.
Balancing Benefits & Risks
Benefits of a normal cervix MRI
- High softtissue contrast unparalleled view of the cervixs layers.
- No ionizing radiation safe for repeated followup, even in younger women.
- Accurate baseline essential for detecting subtle changes over time.
Risks & limitations
- Contrast reactions rare but possible; discuss any allergies beforehand.
- Cost & accessibility MRI can be pricey and not available in every community.
- Falsepositives a benign cyst can look suspicious, leading to extra tests.
Overall, the benefits far outweigh the drawbacks for most patients needing detailed pelvic imaging.
Expert tip
If you have metal implants, are pregnant, or have severe claustrophobia, let the radiology team know. There are openMRI options and sedation protocols that keep you safe and comfortable.
Trusted Sources
- Radiology Assistant detailed pictorial essays on cervix anatomy and cancer staging.
- Radiopaedia free, peerreviewed articles on cervical polyp MRI radiology.
- National Cancer Institute guidelines on MRI use in cervical cancer management.
- Peerreviewed studies from PubMed on normal cervical dimensions across menstrual phases.
All of these references are from respected medical institutions and peerreviewed journals, ensuring the information youre reading is accurate and uptodate.
Conclusion
A normal cervix MRI is more than just a pretty pictureits the baseline map that lets doctors detect problems early, plan precise treatments, and reassure patients that everything looks healthy. By understanding the typical anatomy, the standard protocol, and how to read the images, you gain a powerful tool for your health journey. Remember, the scan is safe, radiationfree, and most valuable when used for specific clinical questions, not as a routine screen. If you ever have questions about your own imaging or want to discuss what you saw in a report, dont hesitate to ask your radiologist; theyre happy to walk you through the pictures, one slice at a time.
Whats your experience with pelvic imaging? Have you ever felt nervous before an MRI? Share your thoughts in the commentsId love to hear your story!