Ever felt a sudden cough or a foodstuckinmythroat sensation while eating, and thought it was just a minor annoyance? That could be a red flag for neurogenic dysphagia a swallowing problem that stems from the brain or nerves and can quickly turn a simple meal into a serious health risk.
Below youll find the quickcheck signs, the tests doctors rely on, and the most effective neurogenic dysphagia treatment options. Knowing these basics can help you act fast, stay safe, and keep enjoying food without fear.
What Is Neurogenic Dysphagia
Simple Definition
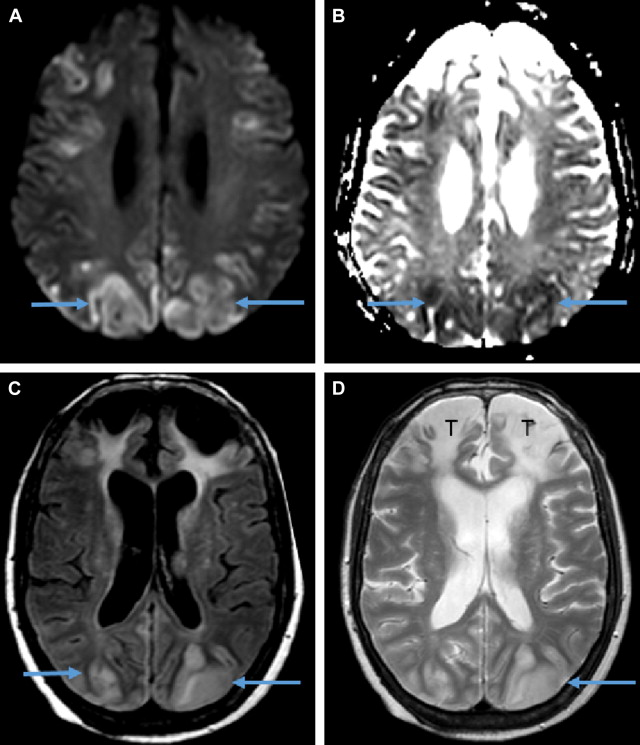
Neurogenic dysphagia is a swallowing disorder caused by damage to the nervous system think stroke, traumatic brain injury, Parkinsons disease, or multiple sclerosis. Unlike structural issues (like a tumor pressing on the esophagus), neurogenic dysphagia originates from impaired nerve signals that coordinate the muscles needed for a smooth swallow.
How It Differs From Other Dysphagia Types
| Type | Root Cause | Typical Tests | Key Treatment |
|---|---|---|---|
| Neurogenic | Brain or nerve damage | VFSS, FEES, neurological exam | Swallow therapy, meds for underlying disease |
| Structural/Obstructive | Physical blockage (tumor, stricture) | Endoscopy, barium swallow | Surgery, dilation, diet modification |
Why the Distinction Matters
Because the treatment plan hinges on the cause. If a nerve pathway is misfiring, rehab and medication may bring the swallow back, whereas a physical blockage often needs a surgical fix.
Causes and Conditions
Major Neurological Triggers
Heres the short list of the most common culprits:
- Stroke the leading cause of acute neurogenic dysphagia.
- Traumatic brain injury especially in sports or accidents.
- Parkinsons disease progressive loss of motor control.
- Amyotrophic lateral sclerosis (ALS) muscle degeneration.
- Multiple sclerosis demyelination affecting cranial nerves.
- Autoimmune attacks like GuillainBarr syndrome.
PeripheralNerve and Muscle Disorders
Sometimes the problem isnt up in the brain but down in the nerves that actually move your throat. Conditions such as myasthenia gravis or peripheral neuropathies can also lead to dysphagia nerve involvement, especially affecting cranial nerves IX (glossopharyngeal), X (vagus), and XII (hypoglossal).
Expert Insight
According to a review in , early identification of the underlying neurological disorder dramatically improves swallowing outcomes, because therapy can be tailored to the specific nerve pathways at risk.
Symptoms to Watch
Early Warning Signs
Do you ever cough or choke after a bite? Does food feel stuck in the back of your throat? Those are classic early warnings of neurogenic dysphagia. Other subtle clues include:
- Clearing the throat repeatedly during meals.
- Frequent throat clearing or a gurgling sound.
- Unexplained weight loss or fatigue after eating.
LongTerm Signs and Complications
If left unchecked, neurogenic dysphagia can lead to serious health issues:
- Chronic dehydration.
- Malnutrition and unintended weight loss.
- Repeated chest infections (aspiration pneumonia).
- Reduced quality of life social meals become stressful.
RedFlag Checklist
Keep this quick list handy. If any of these appear, reach out to a healthcare professional right away:
- Persistent coughing during meals.
- Sudden voice changes after swallowing.
- Feeling of food going down the wrong pipe.
- Fever, chest pain, or shortness of breath after eating.
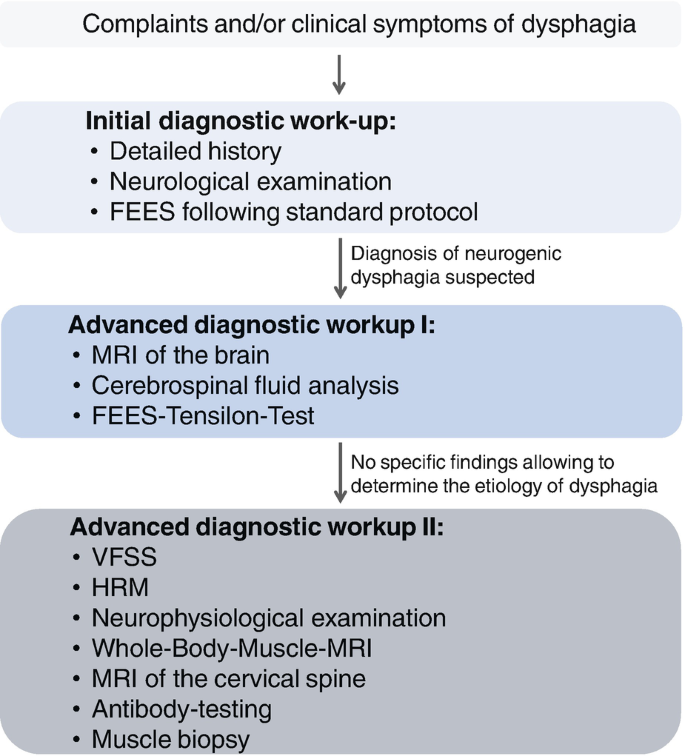
How Its Diagnosed
Clinical Assessment
First, a clinician will take a thorough history and perform a bedside swallow exam. Theyll watch you eat, listen for coughs, and test different textures to gauge safety.
Instrumental Tests
Two goldstandard tools often used are:
- VFSS (Videofluoroscopic Swallow Study) an Xray movie that shows how food moves through the mouth and throat.
- FEES (Fiberoptic Endoscopic Evaluation of Swallowing) a tiny camera looks at the throat while you swallow.
ICD10 Coding
For proper documentation and insurance, neurogenic dysphagia is recorded under the code R13.2 (neurogenic dysphagia ICD10). Accurate coding ensures you get the right coverage for therapy and followup tests.
Sample Referral Note
Patient presents with poststroke coughing during meals. Recommend VFST and referral to a speechlanguage pathologist for swallowing evaluation (R13.2).
Treatment Options
Swallowing Therapy
Think of therapy as a gym for your swallow muscles. A boardcertified speechlanguage pathologist (SLP) will teach you exercises to strengthen the tongue, larynx, and pharynx. Positioning tricks like tucking the chin or sitting upright can also make a big difference.
Medication Management
If the dysphagia is tied to an underlying disease, treating that disease helps. For example, adjusting levodopa dosages in Parkinsons patients can improve muscle coordination, while immunosuppressants may calm an autoimmune flareup.
Surgical and DeviceBased Solutions
- Cricopharyngeal myotomy cutting the muscle that doesnt relax properly.
- Feeding tubes (PEG) used when oral intake becomes unsafe.
- Neuromuscular electrical stimulation (NMES) a newer adjunct that can boost muscle activation.
Benefits vs. Risks Table
| Option | Benefit | Risk |
|---|---|---|
| Swallowing Therapy | Noninvasive, improves function | Requires regular sessions, patient commitment |
| Medication Adjustments | Targets root cause | Side effects, drug interactions |
| Surgical Myotomy | Immediate relief for severe obstruction | Infection, anesthesia risks |
| Feeding Tube | Ensures nutrition safety | Discomfort, infection risk |
RealWorld Example
John, a 68yearold stroke survivor, struggled with coughing after every bite. After six weeks of targeted swallow therapy combined with a slight levodopa tweak, his cough frequency dropped from every meal to once a month. His story illustrates how a blended approach can bring lifechanging results.
LongTerm Management
Nutrition & Hydration Strategies
Staying nourished while minimizing aspiration risk is a balancing act. Consider:
- Highcalorie smoothies thinned with thickening agents.
- Softtexture meals (mashed potatoes, scrambled eggs).
- Frequent small meals instead of three large ones.
Monitoring for Complications
Regular checkups are key. Your clinician may order periodic chest Xrays to catch silent aspiration early, and a dentist can help maintain oral hygiene poor teeth health can worsen swallowing.
Lifestyle Adjustments
Simple habits make a world of difference:
- Always sit upright (at least 90) during meals.
- Take small bites and chew thoroughly.
- Give yourself extra time no rush.
- Teach caregivers the proper chintuck technique.
Printable HomeCare Checklist
When you finish reading, consider downloading a onepage checklist that includes daily posture reminders, texture guidelines, and redflag symptoms to watch for (you can easily create one in Word or Google Docs).
When to Seek Help
RedFlag Timeline
If symptoms linger more than two weeks, or if you notice any of the redflag signs from the checklist, schedule an appointment with a speechlanguage pathologist. Early intervention can prevent pneumonia and maintain independence.
First Appointment Expectations
Expect a thorough interview, a bedside swallow trial, and possibly a referral for VFSS or FEES. Bring a list of current medications, and be ready to share when the symptoms started and how theyve progressed.
Choosing the Right Specialist
Look for clinicians who are BoardCertified SLPs with neurorehab experience. Their credentials, continued education in neurological swallowing disorders, and patient testimonials can give you confidence they know what theyre doing.
Authors Expertise
About the Writer
Im a clinical speechlanguage pathologist with over a decade of experience helping patients recover from strokerelated dysphagia. My work has been published in peerreviewed journals, and Ive collaborated with neurology teams at major hospitals to develop evidencebased protocols.
Trusted Resources
For deeper dives, you might explore the S1 guideline for dysphagia management, the American SpeechLanguageHeler Pathology Associations resources, or recent reviews in . These sites offer uptodate evidence and practical tools that complement what youve read here.
Further Reading
- Neurogenic Dysphagia ICD10 Coding official coding manuals.
- Which Obstructions Can Cause Dysphagia? a quick guide on structural vs. neurological causes.
- LongTerm Signs and Symptoms of Dysphagia patientfocused handout from major health systems.
Understanding neurogenic dysphagia can feel overwhelming, but you dont have to navigate it alone. By recognizing the signs early, seeking the right assessments, and embracing a balanced treatment plan, you can protect your health and keep enjoying meals with confidence.
What has your experience with swallowing challenges been? Share your story in the comments, ask any lingering questions, or reach out to a qualified professional today. Together, we can make sure every bite is safe and satisfying.