Feeling a strange ache in your lower belly during menopause? You're not alonemany women notice that uncomfortable, sometimes sharp, sensation as hormones shift. The good news is that most of the time its manageable, and knowing whats really going on can help you tackle it headon.
Why It Happens
Hormonal RollerCoaster
When estrogen and progesterone start to dip, they affect more than just hot flashes. Lower estrogen can slow down gut motility, making bloating and cramping feel worse. It also reduces the elasticity of the pelvic tissues, which can turn everyday movements into a minipain fest.
Uterine & Ovarian Conditions
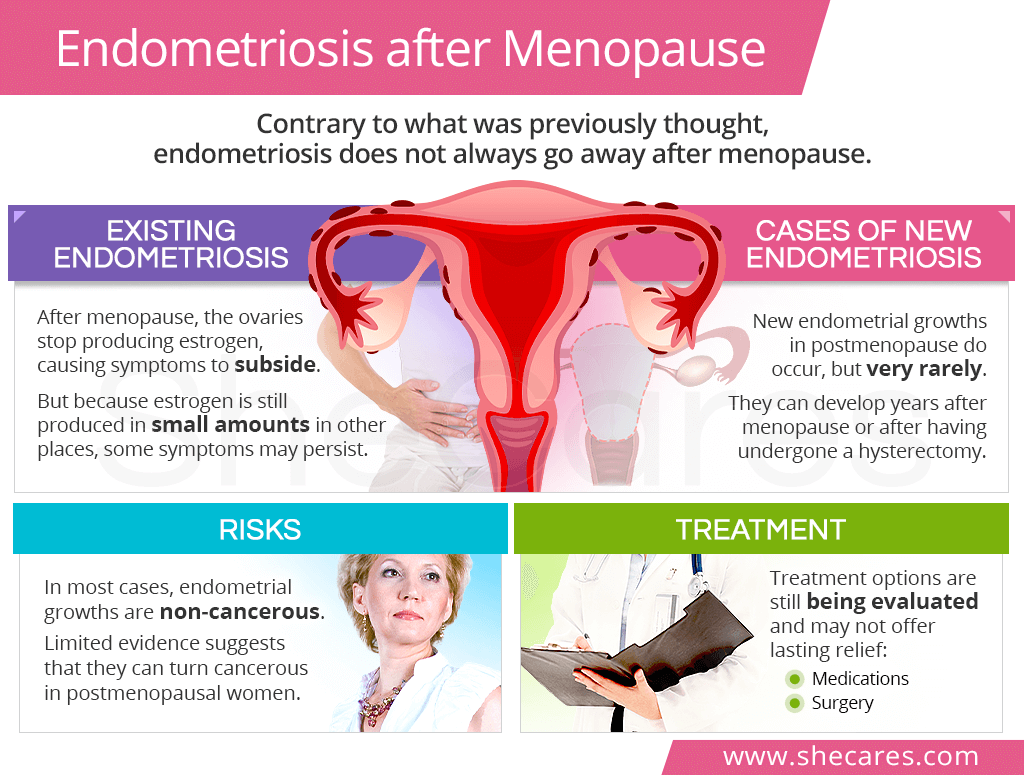
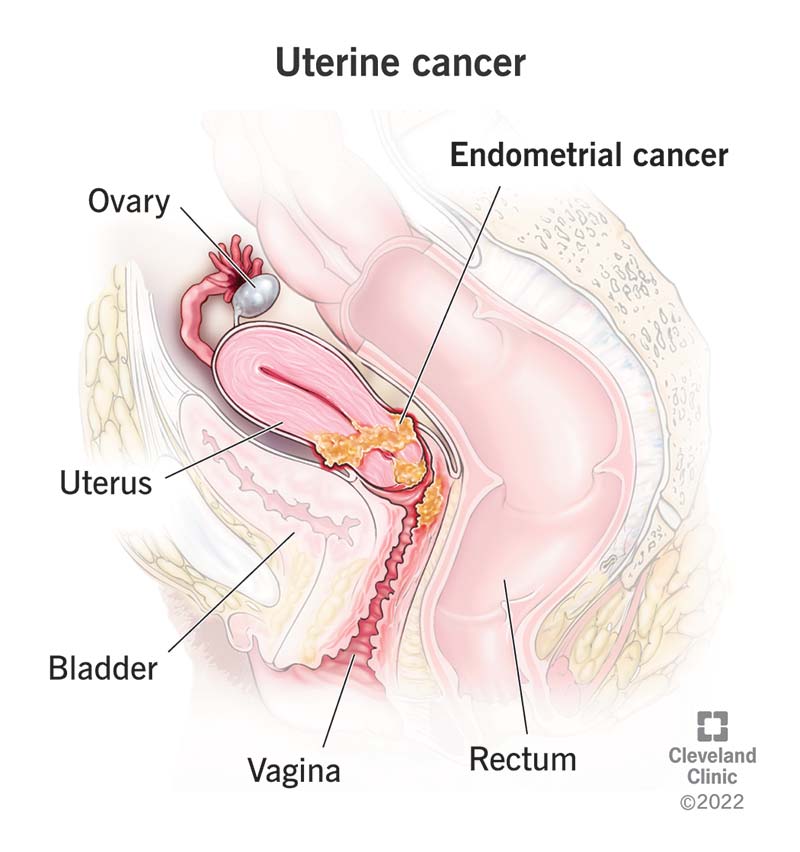
Fibroids, endometriosis, or lingering ovarian cysts dont just vanish because youre hitting 50. In fact, these growths can become more noticeable when the hormonal support fades, leading to menopause pain in lower abdomen and back.
Pelvic Floor & Muscle Changes
As the vaginal walls thin and natural lubrication drops, the surrounding muscles can tighten or spasm. This tension often radiates upward, making you feel that ache in the lower belly as well as the lower back.
Digestive & GI Contributors
Hormone swings can trigger IBSlike symptomsthink gas, constipation, or diarrhea. When the gut is upset, the abdomen lights up with discomfort that many women attribute solely to menopause.
RedFlag Signals
If the pain is sudden, severe, or comes with bleeding, fever, or unexplained weight loss, its time to call a doctor. These could be signs of something more serious, like an infection or, rarely, cancer.
Typical Patterns
Lower Abdomen & Back
Many women notice that the pain spreads from the belly to the lumbar area. The nerves that serve the uterus and pelvic floor also share pathways with the lower back, so a twinge in one spot often shows up in the other.
AgeSpecific Prevalence
Studies show that lower abdominal pain in 50yearold women peaks during the early to midmenopausal transition, when hormone levels are most erratic.
Upper vs. Lower Pain
While perimenopause upper abdominal pain often points to gallbladder or liver issues, the lower belly is more likely linked to pelvic organs and the gut.
Cramps Without a Period
Even when periods cease, the uterus can still contract. Those cramps during menopause with no period are a normal hormonal quirk, but they shouldnt be ignored if theyre intense.
Timeline Snapshot
| Stage | Typical Symptoms |
|---|---|
| Early Perimenopause | Irregular cycles, mild lowerabdominal cramping |
| MidTransition | Increased bloating, occasional back pain, menopause stomach pain and bloating |
| Postmenopause | Persistent pelvic pressure, possible postmenopausal pelvic pain and pressure |
Diagnosing the Pain
SelfAssessment Checklist
- When did the pain start? (days, weeks, months?)
- How would you describe it? (sharp, dull, cramping?)
- What makes it better or worse? (food, movement, stress?)
- Any other symptoms? (bleeding, fever, changes in bowel habits?)
When to See a Doctor
A pelvic exam and a transvaginal ultrasound can spot fibroids, cysts, or endometriosis. Blood workchecking hormone panels, thyroid function, and inflammatory markershelps rule out systemic causes.
Differential Diagnosis
| Possible Source | Key Signs | Typical Tests |
|---|---|---|
| Hormonal (estrogen drop) | Widespread bloating, mild cramping | Hormone panel |
| Gynecologic (fibroids, cysts) | Pain radiates to back, occasional spotting | Ultrasound, MRI |
| GI (IBS, constipation) | Changes in stool, gas, relief after bowel movement | Stool studies, colonoscopy if needed |
| Musculoskeletal (pelvic floor tension) | Worsens with certain movements, improved with stretching | Physical exam, pelvic floor assessment |
Relief Strategies
Lifestyle & Nutrition Hacks
Antiinflammatory foodsthink turmeric, ginger, salmon, and leafy greenscan calm the gut and reduce pelvic soreness. Fiberrich meals and plenty of water keep things moving, easing constipationrelated cramps.
Targeted Exercises
Gentle yoga poses like Childs Pose, CatCow, and pelvic tilts stretch the lower back and core. Pilates routines that focus on deep abdominal breathing help relax the pelvic floor.
HormoneBased Treatments
Lowdose estrogen therapy or a combined estrogenprogesterone regimen can smooth out the hormonal rollercoaster. Discuss the risks (like clotting) and benefits with your providersometimes a small patch or cream does the trick.
Medications
Overthecounter NSAIDs (ibuprofen, naproxen) are effective for shortterm relief. If cramps are severe, a doctor might prescribe a muscle relaxant or a short course of lowdose hormonal pills.
Alternative Therapies
Acupuncture has modest evidence for reducing pelvic pain, and applying a warm compress can soothe tight muscles. Mindfulness meditation helps lower stressinduced gut spasms.
When to Seek Immediate Help
If the ache lasts more than two weeks, worsens, or is accompanied by heavy bleeding, fever, or unexplained weight loss, dont waitschedule a medical appointment right away.
RealWorld Stories
Sarahs Story
Sarah, 52, started feeling a deep gurgle in her lower belly three months after her last period. She tried overthecounter painkillers with little relief. After a pelvic ultrasound revealed a small fibroid, her doctor recommended a lowdose estrogen patch plus a daily probiotic. Within six weeks, her bloating faded and the pain eased dramatically. I felt like I finally got my body to listen, she says.
Expert Insight
Dr. Maya Dooley, a menopause specialist at Gennev, notes, When women mention lowerabdominal pain, I first check for hormonal imbalance, then rule out structural issues. Often, a combination of diet tweaks and mild hormone therapy does the trick. She adds that persistent pain should never be ignored, especially if its paired with new bleeding.
Helpful Resources
For deeper dives into the science, you can read the study on abdominal pain prevalence during menopause in the . Healthgrades also lists redflag symptoms to watch for, such as sudden severe pain or unexpected bleeding.
Bottom Line
Lowerabdominal discomfort during menopause is usually a mix of hormonal shifts, pelvic changes, and digestive quirks. By understanding the why, tracking your symptoms, and using a blend of lifestyle tweaks, targeted exercises, and, when needed, medical therapies, you can reclaim comfort and confidence. If anything feels off, trust your instincts and reach out to a health professional. You deserve reliefand a smoother journey through this next chapter of life.