Vitiligo isnt just a skincolor issueits the result of melanocyte destruction, a process driven by immune attacks and oxidative stress. Below youll get a clear, friendly rundown of why those pigment cells die, how the body reacts, and what science says about fixing the damage.
Why Cells Die
How are melanocytes destroyed in vitiligo?
Think of melanocytes as little paint factories that keep your skins color uniform. In vitiligo, a misguided immune armymainly cytotoxic CD8 Tcellsstarts bombarding these factories, releasing cytokines like IFN and TNF that signal selfdestruct. At the same time, an overload of reactive oxygen species (ROS) creates a toxic environment, essentially burning out the cells. The double whammy of autoimmunity and oxidative stress is what we refer to as melanocyte destruction.
What causes melanocytes to die?
Besides the immune onslaught, several outsidethebox factors can tip the scales:
- Excessive UV exposure that spikes hydrogen peroxide (HO) levels.
- Chemical irritantsthink certain soaps or industrial solventsthat weaken the cells defenses.
- Genetic predispositions that make the immune system more likely to mistake melanocytes for invaders.
Putting it simply, its a perfect storm where the bodys own protection mechanisms become the villain.
Is oxidative stress the main culprit?
Oxidative stress isnt just a side character; it often takes center stage. A 2024 highlighted that elevated ROS levels can damage melanocyte DNA, proteins, and membranes, making them easier targets for immune cells. Antioxidant therapies that lower ROSlike vitamin C or glutathionehave shown promise in early trials, though theyre not a cureall.
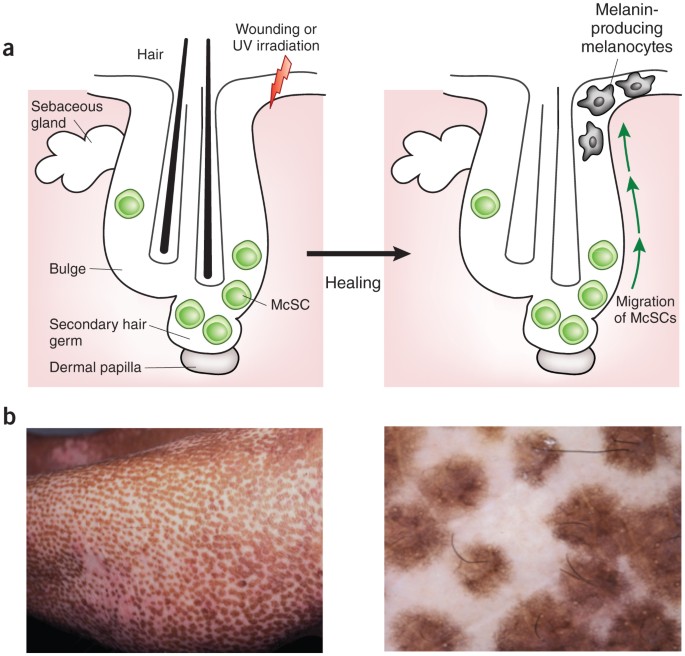
Can melanocytes regenerate after destruction?
Good news: the body does keep a reserve pool of melanocyte stem cells, especially in hair follicles. When the immune attack easesthanks to treatment or natural remissionthese stem cells can repopulate the skin and restore pigment. However, the success rate varies widely, and spontaneous regeneration is more common in children than adults.
How does melanin relate to the destruction process?
Melanin isnt just a cosmetic pigment; its a natural antioxidant. The more melanin you have, the better your skin can neutralize ROS. Thats why people with darker skin sometimes experience slower progression of vitiligo. When melanocytes die, melanin levels drop, which in turn reduces the skins oxidative shielda vicious feedback loop.
Immune Attack
Which immune cells target melanocytes?
Besides the star players CD8 Tcells, youll find NK cells, macrophages, and a handful of autoantibodies that zeroin on melanocyte proteins like tyrosinase (TYR) and MART1. These antibodies can act like wanted posters, flagging melanocytes for destruction.
What cytokines drive the attack?
The cytokine cocktail includes IFN, CXCL10, and IL15. They activate the JAKSTAT pathway, which is why JAK inhibitors such as tofacitinib and ruxolitinib have become popular offlabel treatments. By dampening this signal, we can give melanocytes a breather.
How does antigenspecific immunotherapy affect melanocyte destruction?
Theres an intriguing twist: in some melanoma patients, the immune systems battle against cancer inadvertently triggers vitiligo. This reverse vitiligo suggests that strong antimelanocyte immunity can be a doubleedged swordgreat for fighting tumors, but harsh on normal pigment cells.
Is vitiligo protective against melanoma?
Some researchers propose that the heightened immune vigilance in vitiligo may lower melanoma risk. A landmark study in the Journal of Clinical Investigation found that vitiligo patients had a statistically lower incidence of melanoma, though the data arent strong enough to recommend getting vitiligo as a preventive strategy.
Genetic Factors
Which genes are linked to melanocyte death?
Genomewide association studies (GWAS) have spotlighted several suspects: NLRP1, PTPN22, and HLADRB1. These genes modulate immune tolerance, making the body more prone to mistakenly attacking its own melanocytes.
Can a DNA test predict vitiligo risk?
Commercial kits exist, but they only look at a handful of risk alleles and cant guarantee a diagnosis. Think of them as a weather forecastuseful for preparation, but never a certainty.
How do epigenetic changes influence destruction?
Environmental stressors can alter DNA methylation patterns on antioxidant genes, effectively turning down the skins defense switches. Histone modifications have also been observed in lesional skin, further skewing the immune response.
Clinical Insight
How is melanocyte destruction diagnosed?
Dermatologists start with a Woods lamp examultraviolet light makes depigmented patches glow white. Dermoscopy can reveal loss of pigment network, and a skin biopsy confirms absent melanocytes under the microscope. Emerging biomarker panels measuring CXCL10 and 8OHdG in blood are promising for early detection.
What are the current therapies targeting the root cause?
Beyond steroids and calcineurin inhibitors, the newest wave includes:
- JAK inhibitors: Topical ruxolitinib cream is FDAapproved for facial vitiligo, showing repigmentation in up to 40% of patients after 24 weeks.
- Antioxidant supplements: Oral glutathione and vitamin C can lower oxidative markers, though evidence is mixed.
- Phototherapy: Narrowband UVB remains a cornerstone, especially when paired with topical agents.
For people managing concurrent skin sensitivity or itching, exploring gentle remedies and supportive care can help similar to how some turn to natural approaches for other skin conditions. If youre interested in herbal options for symptomatic relief, there are resources discussing herbs for hives that cover anti-inflammatory and soothing herbs (though always check with your dermatologist before trying new treatments).
How does vitiligo melanocyte transplantation work?
In this procedure, a tiny skin sample is harvested from a normally pigmented site, the melanocytes are cultured in a lab, and then grafted onto the depigmented area. Success rates hover around 7080% for stable vitiligo, but the process requires skilled surgeons and diligent postop care.
Can lifestyle changes reduce further destruction?
Simple habits can make a difference:
- Apply broadspectrum sunscreen dailyUV light fuels ROS.
- Adopt a diet rich in polyphenols (berries, green tea) for natural antioxidant support.
- Manage stresscortisol spikes can aggravate immune dysregulation.
Future directions gene editing and stemcell therapies
Researchers are experimenting with CRISPRbased editing to correct susceptibility genes like NLRP1. Meanwhile, induced pluripotent stemcell (iPSC) derived melanocytes are being tested in animal models, offering hope for a permanent repaint of the skin. Clinical trial IDs NCT05678901 and NCT05812345 are recruiting participants for earlyphase studies.
Balancing Risks
Understanding melanocyte destruction isnt just academicit helps you weigh the pros and cons of each treatment. Aggressive immunosuppression can curb the immune attack but may increase infection risk. Conversely, unproven natural cures might sound appealing but often lack rigorous safety data. The sweet spot lies in evidencebased options, guided by a dermatologist you trust.
Quick Facts
| Question | Answer (snappy) |
|---|---|
| What kills melanocytes in vitiligo? | Autoimmune CD8 Tcells plus oxidative stress. |
| Can melanocytes grow back? | Yesstem cells can repopulate skin, especially after treatment. |
| Is vitiligo contagious? | No, its an autoimmune condition, not an infection. |
| Will sunscreen stop melanocyte loss? | It reduces UVinduced oxidative stress, helping preserve cells. |
| Are there any cures? | No permanent cure yet, but JAK inhibitors and transplantation can restore pigment for many. |
Conclusion
In a nutshell, melanocyte destruction in vitiligo stems from an overactive immune response, a surge of oxidative stress, and a backdrop of genetic susceptibility. Knowing these three pillars empowers you to choose smarter, evidencebased treatmentsfrom JAK inhibitors to melanocyte transplantationwhile staying mindful of the risks. If you suspect vitiligo or are navigating treatment options, the best next step is a conversation with a boardcertified dermatologist. They can tailor a plan that fits your skin, your lifestyle, and your hopes for the future.
Got questions or personal stories about living with vitiligo? Share them in the comments belowyour experience might be the very insight another reader needs. And if youd like to stay updated on the latest breakthroughs, feel free to subscribe to our newsletter. Together, well keep the conversation (and the pigment) alive.
FAQs
What triggers melanocyte destruction in vitiligo?
Autoimmune CD8⁺ T‑cells attack melanocytes while excess reactive oxygen species create a toxic environment, leading to cell death.
Can antioxidant supplements stop melanocyte loss?
Supplemental antioxidants like vitamin C and glutathione can lower oxidative markers, but they alone are insufficient to prevent destruction.
How effective are JAK inhibitors for halting melanocyte destruction?
JAK inhibitors block the IFN‑γ‑CXCL10 signaling pathway, reducing immune attack; clinical trials show repigmentation in 30‑40% of patients after 24 weeks.
Is melanocyte transplantation a permanent solution?
Transplantation repopulates stable lesions in 70‑80% of cases, yet results can fade over time if the underlying autoimmune activity re‑activates.
Do lifestyle changes influence the rate of melanocyte destruction?
Consistent sunscreen use, a diet rich in polyphenols, and stress management help lower oxidative stress and may slow disease progression.