Most people dont realize that life with a tracheostomy can feel surprisingly normal once you get the hang of it. You can keep talking, eat, and enjoy daily momentsjust like before. Below youll find the shortandsweet answers youre looking for, followed by a friendly walkthrough of everything you need to know to feel confident and in control.
Quick answers:
- Can you live a normal life? Absolutely. Many people live 5, 10 or even 20+ years with a tracheostomy when the underlying condition is stable and proper care is followed.
- How do you keep secretions under control? Stay hydrated, use humidified air, and suction regularlysimple steps that make a huge difference.
- Is drinking water safe? Yes, as long as the cuff is deflated and you can swallow safely. Aim for at least 2L of fluids a day.
Quick Answers Now
Think of this as a cheatsheet you can print and pin on the fridge. If youre reading on the go, skim these bullet pointseverything else below dives deeper into the why and how.
Can I live a full life?
Living with a tracheostomy isnt a death sentence. With the right support, you can work, travel, and stay active. The key is learning to manage your airway and staying on top of routine care.
How long can you live with a tracheostomy?
Survival rates vary. A study in the showed that over 70% of chronic ventilatordependent adults survive beyond five years, and many reach a decade or more. Factors such as age, underlying disease, and home support play big roles.
Can trach patients drink water?
Yes! Once the cuff is deflated and youve been cleared by a speechlanguage pathologist, sipping water is safe and helps thin secretions. Its also a comfortnothing feels better than a cool glass after a long day.
Tracheostomy Basics Overview
What is a tracheostomy tube?
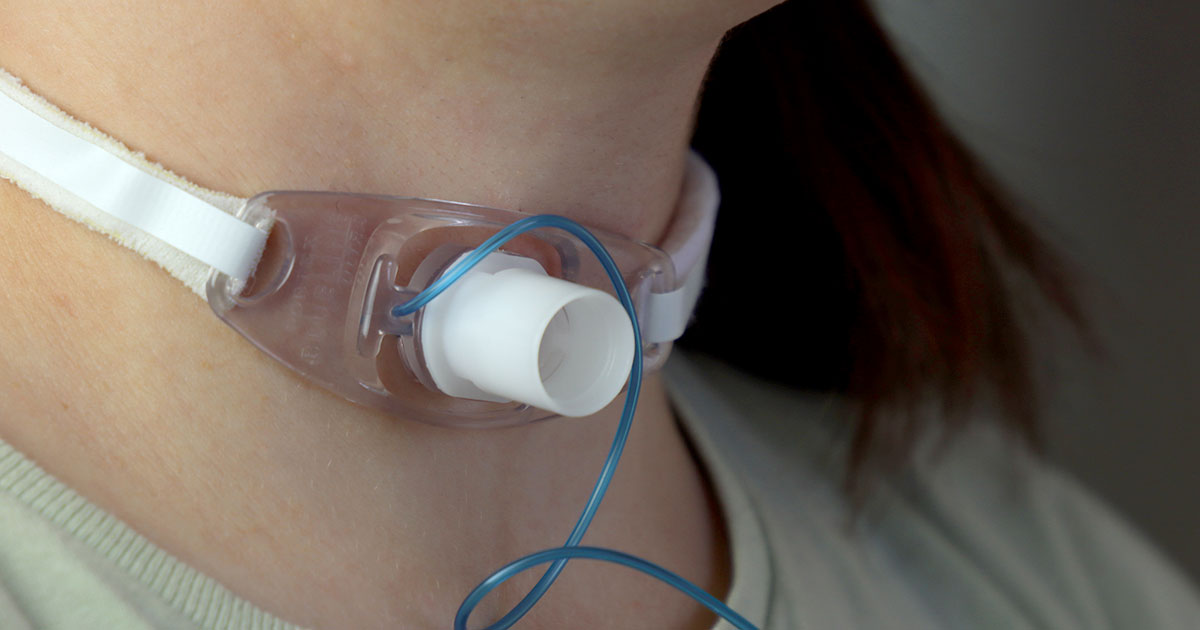
A tracheostomy tube is a short, curved tube that sits in a small opening (the stoma) on the front of your neck, giving air a direct route to your lungs. Most tubes have an inner cannula you can pull out for cleaning, an outer cannula that stays in place, and a flange that secures it to your skin.
Why is it done?
Doctors recommend a trach when the airway is blocked, you need longterm ventilation, or youre recovering from head and neck surgery. It can also make it easier to clear secretions and improve comfort compared to a face mask.
Common myths busted
- Myth: You cant speak. Reality: With a cuffdeflated tube you can speak normally, and many people love the newfound ability to communicate without a mask.
- Myth: Youll always be in the hospital. Reality: With proper training, most patients transition to home care within a week or two.
- Myth: Youll never eat solid food again. Reality: Many people eat a regular diet; a feeding tube is only needed if swallowing is unsafe.
Home Care Routine
Morning, afternoon, night checklist
Think of it like brushing your teethjust a few extra steps.
- Morning: Wash hands, inspect the stoma for redness, clean the inner cannula with warm soapy water, and suction any visible secretions.
- Afternoon: Rehydratedrink a glass of water, check the cuff pressure (if you have a cuffed tube), and give the tube a quick visual check.
- Night: Apply a mild moisturizer around the stoma to prevent skin drying, secure the tube snugly but comfortably, and set up a suction device within arms reach.
How to reduce tracheostomy secretions
Secretions can feel like a neverending faucet, but a few tricks work wonders:
- Hydration: Aim for 23L of fluid daily. Warm teas, broth, and electrolyte drinks count.
- Humidification: Use a heated humidifier or a heatmoisture exchanger (HME). The table below compares the two.
- Gentle suction: Suction no more than once every 23hours, or whenever you feel discomfort. Oversuctioning can irritate the airway.
- Avoid irritants: No smoking, strong perfumes, or dusty environments.
| Feature | Heated Humidifier | HeatMoisture Exchanger (HME) |
|---|---|---|
| Moisture Level | High (continuous steam) | Moderate (captures exhaled moisture) |
| Portability | Bulky, needs power | Lightweight, fits on the tube |
| Cost | Higher upfront, ongoing electricity | Low cost, replace every 12 weeks |
Emergency basics
Even with the best routine, something can go wrong. Keep this short whattodo guide handy:
- Sudden blockage: Remove the inner cannula, try to pass a suction catheter. If you cant clear it, call emergency services immediately.
- Bleeding: Apply gentle pressure with a clean gauze, keep the head elevated, and contact your clinician.
- Cuff leak: Inflate the cuff with the syringe provided, check the pressure, and monitor for air loss.
Nutrition and Hydration
Can trach patients drink water?
Yesprovided the cuff is deflated and youve been cleared for oral intake. Water not only quenches thirst but also thins mucus, making suction easier. If youre unsure, ask a speechlanguage pathologist to evaluate your swallow.
Living with a trach and feeding tube
Some people need a feeding tube because swallowing isnt safe yet. That doesnt mean you cant enjoy life. A study in found that patients with both a tracheostomy and a feeding tube have comparable qualityoflife scores to those with a trach alone, as long as they receive proper education and support.
Tips to keep your mouth moist
- Brush teeth after each meal; use a fluoridefree mouthwash.
- Chew sugarfree gum or suck on ice chips.
- Apply a thin layer of waterbased lubricant (like glycerin) around the mouth if dryness persists.
Life Expectancy & Quality
How long can you live with a tracheostomy?
The simple answer: a lot longer than many expect. Survival of 510years is common, and some individuals thrive for 20years or more. The most influential factors are:
- Underlying disease: Chronic obstructive pulmonary disease (COPD) or neuromuscular disorders often determine longevity.
- Age at placement: Younger patients generally have better outcomes.
- Home support: Access to trained caregivers, reliable equipment, and regular medical followup dramatically improves survival.
Quality of life after tracheostomy removal
When the trach is finally taken out, many people experience a rebirth of sortsbreathing feels natural again, speech is clearer, and swallowing improves. However, a period of adjustment is normal. According to Vanderbilt Health, patients who receive postremoval speech therapy report higher confidence and lower anxiety within the first month.
Realworld story
Maria, a 52yearold teacher, has lived with a tracheostomy and a feeding tube for eight years. She says, At first I felt like Id lost my voice. But after a few weeks of humidified air and daily suction, I could laugh with my class again. The feeding tube just means I get the nutrition I need without choking. Ive traveled to three states and still enjoy gardening. Marias experience illustrates that, with the right tools, life can be vibrant and full.
Ventilator to Tracheostomy
Why make the switch?
Going from a ventilator to a tracheostomy is often recommended when a patient needs longterm airway support. The benefits are huge:
- Mobility: No more bulky maskyou can sit up, walk, and even go for short outings.
- Communication: Once the cuff is off, speaking becomes possible.
- Comfort: Pressure sores from mask straps disappear.
First two weeks at home
Imagine a timeline graphic: Day0tube placement; Day2first suction training; Day5first attempt at cuffdeflation; Day10begin oral fluids; Day14full home routine established. During this period, youll notice breath sounds becoming clearer, secretions thinning, and your confidence growing.
Tips for caregivers
Caregivers are the unsung heroes. Heres a quick cheatsheet for them:
- Attend a handson training session with a respiratory therapist.
- Keep a suction log note time, amount, and any distress signs.
- Maintain a stock of spare tubes, extra humidifier filters, and clean gauze.
- Know the emergency numbers and have the trach kit within arms reach.
Emotional & Social Support
Coping with stigma
Its normal to feel selfconscious the first few weeks. A simple trick: practice a short elevator pitch to explain your trach in 30 seconds. Something like, I have a small tube in my neck that helps me breathe better; its a part of my daily routine, just like glasses for some people. Sharing this calmly can defuse awkward questions.
Keeping work and friends involved
Inform your employer about any needed accommodationsperhaps a portable suction device or a short break for cleaning. Most workplaces are supportive once they understand the basics.
Mentalhealth resources
Living with a medical device can bring anxiety or depression. Talking to a therapist who specializes in chronic illness can be a gamechanger. Cognitivebehavioral therapy (CBT) has been shown to reduce healthrelated anxiety by up to 30% in trach patients, according to a study in .
Building a Support Network
Finding trustworthy clinicians
Look for providers who are boardcertified in pulmonology or otolaryngology and have a dedicated tracheostomy clinic. Verify credentials, read patient reviews, and ask about their experience with homecare transitions.
Reliable online resources
Here are a few sources that consistently publish evidencebased information:
- Hopkins Medicine comprehensive tracheostomy care guides.
- American Thoracic Society guidelines on longterm ventilation.
- MyHealth Alberta stepbystep videos for suctioning.
- Medtronic product manuals for tube and humidifier maintenance.
Spotting misinformation
When you search the web, ask yourself:
- Is the source a recognized medical institution?
- Does the article cite peerreviewed studies?
- Are there clear author credentials?
Conclusion
Living with a tracheostomy is a journey that blends daily routines, medical knowhow, and a dash of courage. You can enjoy a full life, stay hydrated, keep secretions in check, and even drink water safely. Remember that the length of time you can live with a trach depends on many factorsbut many thrive for years, especially when they have solid support, reliable equipment, and trusted caregivers.
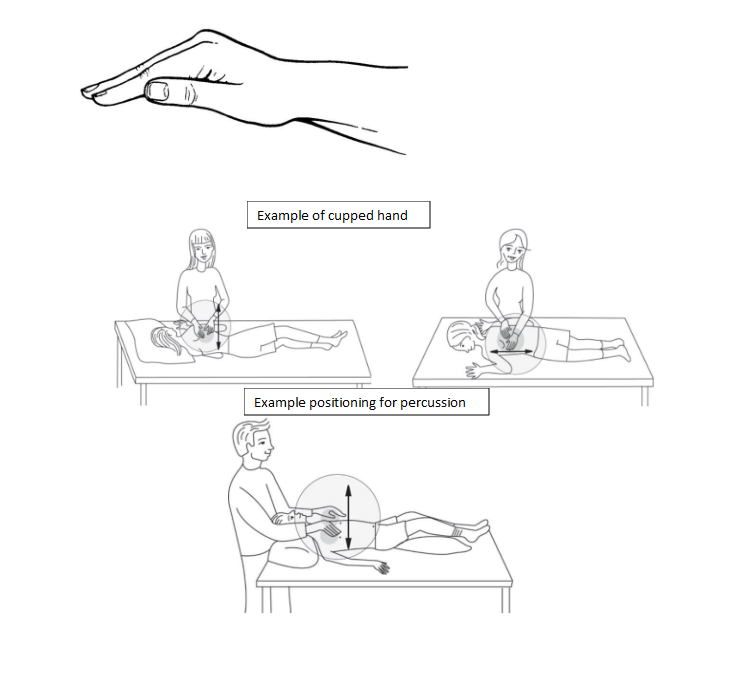
If anything in this guide sparked a question or you have a tip to share, drop a comment below. And if youd like a printable version of the daily care checklist, chest physiotherapy cystic fibrosis click here to download
FAQs
How often should I change my tracheostomy tube?
Most tubes are replaced every 2–4 weeks, but the schedule depends on the tube type, skin condition, and any blockage or wear you notice.
Can I speak with a tracheostomy tube in place?
Yes—once the cuff is deflated and you have clearance from a speech‑language pathologist, you can speak normally through the tube.
What signs indicate I need emergency medical help?
Sudden inability to breathe, heavy bleeding, rapid swelling around the stoma, or loss of cuff pressure that causes air leakage all require immediate emergency assistance.
How can I keep my airway moist at home?
Use a heated humidifier or a heat‑moisture exchanger, stay well‑hydrated (2–3 L daily), and avoid dry or smoky environments.
Is it safe to exercise with a tracheostomy?
Yes—most patients can walk, light‑strength train, or do low‑impact cardio after a short acclimation period; just keep suction equipment nearby and monitor your breathing.