If youve just heard you need an esophagectomy, your mind probably races: Will I live long enough to see my grandkids grow? Will I ever feel normal again? The short answer is that most patients who undergo the operation have a 3045% chance of living five years or more. Those numbers swing up or down depending on age, cancer stage, overall health, and whether the disease comes back.
Knowing the stats, the risks, and the everyday realities can turn that scary whatif into a plan you feel comfortable walking through. Lets talk about what the data really mean, how your own story fits into those figures, and what you can do right now to give yourself the best shot at a long, fulfilling life after surgery.
Survival Numbers
FiveYear Survival The Headline Figure
Across large population studies, the fiveyear survival rate after an esophagectomy sits around 3045%. That means roughly one in three patients make it to the fiveyear mark, and many go on to live much longer.
TenYear & FifteenYear Outlook
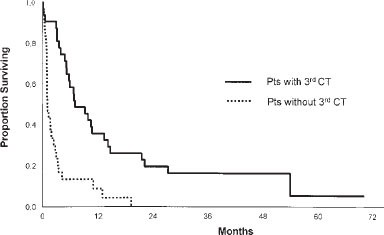
When you look farther out, the picture gets a bit clearer. Tenyear survival hovers near 2025%, while some registries report about a quarter of patients still alive at fifteen years. The dropoff tends to happen between years 6 and 10, a period when cancer recurrence is most common.
How Researchers Compare to the General Population
Scientists use something called the Standardized Mortality Ratio (SMR) to see how much higher the death risk is compared with people who never had cancer. For esophagectomy survivors, the SMR is highest in the first three years postoperation and slowly levels off, but it never quite reaches the baseline risk of the general population.
| Time After Surgery | Survival Rate | Typical SMR |
|---|---|---|
| 1 Year | 80% | 2.53.0 |
| 5 Years | 3045% | 1.82.2 |
| 10 Years | 2025% | 1.31.6 |
| 15 Years | 25% | 1.2 |
Key Influences
Cancer Stage at Diagnosis
Stage matters a lot. Earlystage cancers give you a fiveyear survival of up to 6065%, while stage IIIIV drops that figure to around 2030%.
Age and Overall Health
Age isn't just a number; it's a proxy for how well your body can bounce back. Studies show that patients under 70 have a 90% chance of surviving the first 90 days after surgery, compared with about 85% for those 75 and older. But physiologic age matters too if you stay active, manage weight, and keep chronic illnesses in check, you'll likely fare better than the raw calendar age suggests.
Tumor Histology
Two main types of esophageal cancer adenocarcinoma and squamous cell carcinoma behave slightly differently. Adenocarcinomas, more common in the West, often show a marginally better response to modern multimodal therapy, while squamous cell cancers may have a slightly higher risk of early recurrence.
Surgical Technique & PeriOperative Care
Minimally invasive esophagectomy (MIE) has become the gold standard in many highvolume centers. Compared with the traditional open approach, MIE reduces the risk of major complications by roughly 1520% and shortens hospital stays, which can translate into a modest boost in survival.
PostOperative Complications & Common Causes of Death
Unfortunately, complications still happen. The most frequent cause of death after an esophagectomy is respiratory failure, often stemming from pneumonia or an anastomotic leak. Those complications are most common within the first three months, underscoring the importance of vigilant postop monitoring and early pulmonary rehab.
RealWorld Outcomes
Quality of Life After 5, 10, and 15 Years
Survival numbers are only half the story. A large prospective study found that 88% of survivors report stable healthrelated quality of life (HRQoL) at both five and ten years after surgery. Most people bounce back to enjoy meals, exercise, and social activities though many still need dietary tweaks.
Recurrence Patterns
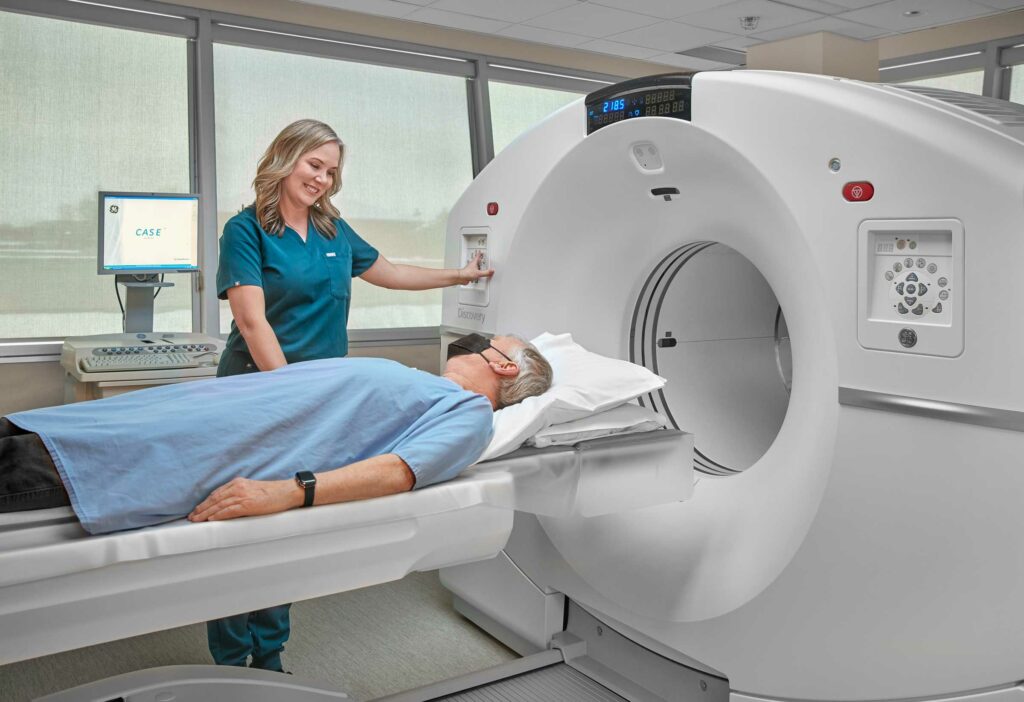
Recurrence is the biggest reason why survival drops after year 5. Roughly 3040% of patients see the cancer come back, and most of those recurrences surface within the first two years. That's why intensive surveillance endoscopy, CT scans, and blood work during the early years is absolutely crucial.
CaseStudy Snapshots
- Case A: John, 62, stage II adenocarcinoma, underwent MIE. He stayed active, followed a strict nutrition plan, and adhered to his followup schedule. Twelve years later, he's still grilling burgers (with a softer bun) and playing with his grandchildren.
- Case B: Mary, 74, stage III squamous cell cancer, had an open esophagectomy. She experienced a leak that prolonged her hospital stay. Recurrence was detected at 18 months, and she chose palliative care. She says the clear communication from her care team helped her feel empowered during a difficult time.
Balancing Hope with Reality
Weighing Surgery vs. NonSurgical Options
Not every patient is a surgical candidate. Chemoradiation alone, targeted therapy, or bestsupportive care might be appropriate for those with extensive comorbidities or very advanced disease. While these alternatives can control symptoms, they generally offer lower longterm survival than a combinedmodality approach that includes surgery.
Talking to Your Care Team
Preparation is power. Bring a notebook and ask questions like:
- What's my personalized fiveyear survival estimate?
- How often will I need endoscopy or imaging?
- Are there clinical trials that might fit my case?
- What lifestyle changes will give me the biggest boost?
Clear answers build trust and help you feel like a partner, not just a patient. For information about related cancer survival topics and longterm outlooks, you may also find resources on prostate cancer outlook helpful when comparing survivorship and followup approaches across cancer types.
Planning for the Future: Emotional & Financial Support
Beyond the medical side, think about practical matters: insurance coverage for followup scans, caregiver respite, and mentalhealth resources. Organizations like the American Cancer Society and Cancer Support Community provide counseling, financial aid, and peersupport groups that can make the journey feel less lonely.
Tools & Resources
Survival Calculator (Download)
We've built a simple spreadsheet where you plug in age, stage, and histology to see an individualized fiveyear survival estimate. It's not a crystal ball, but it gives a clearer picture than a generic statistic.
FollowUp Timeline Checklist
Downloadable PDF that maps out when you should see your surgeon, get a CT, have an endoscopy, and schedule blood tests from 3 months up to 5 years postop.
SymptomWatch List
Keep an eye out for these redflag signs of recurrence:
- New or worsening difficulty swallowing
- Unexplained weight loss (more than 5% of body weight)
- Persistent cough or hoarseness
- Chest pain that doesn't improve with medication
If any of these pop up, call your oncology team right away. Early detection can mean the difference between a curative boost and a more palliative approach.
Conclusion
Bottom line: after an esophagectomy, you have roughly a 3045% chance of making it five years, with better odds if you're younger, have an earlystage tumor, and receive highquality perioperative care. Survival isn't just a number; it's a roadmap that tells you where the risks lie and where hope lives. By staying on top of followup appointments, adopting a hearthealthy lifestyle, and leaning on trusted medical and support networks, you can tilt those odds in your favor and enjoy a life that's not just longer, but richer.
What's your biggest question about life after esophageal cancer surgery? Share your thoughts in the comments, download the tools we've prepared, or reach out to a specialist you trust. You deserve clear, compassionate information and a community that walks with you every step of the way.
FAQs
What is the average five‑year survival rate after esophagectomy?
Large population studies show a five‑year survival of roughly 30 %‑45 % for patients who undergo an esophagectomy, with higher rates for early‑stage disease.
Which factors most influence life expectancy after esophageal cancer surgery?
Key factors include cancer stage at diagnosis, patient age and overall health, tumor histology (adenocarcinoma vs. squamous cell), surgical technique (minimally invasive vs. open), and the presence or absence of post‑operative complications.
How does minimally invasive esophagectomy affect long‑term outcomes?
Minimally invasive esophagectomy reduces major complications by about 15‑20 % and shortens hospital stays, which can translate into a modest improvement in long‑term survival compared with traditional open surgery.
What are the most common signs of cancer recurrence after surgery?
Watch for new or worsening difficulty swallowing, unexplained weight loss (more than 5 % of body weight), persistent cough or hoarseness, and chest pain that does not improve with medication.
How often should I have follow‑up tests to monitor my health post‑surgery?
Guidelines typically recommend a CT scan and blood work every 3‑6 months for the first 2 years, then annually up to 5 years. Endoscopy is usually performed at 6‑12 months and then as clinically indicated.