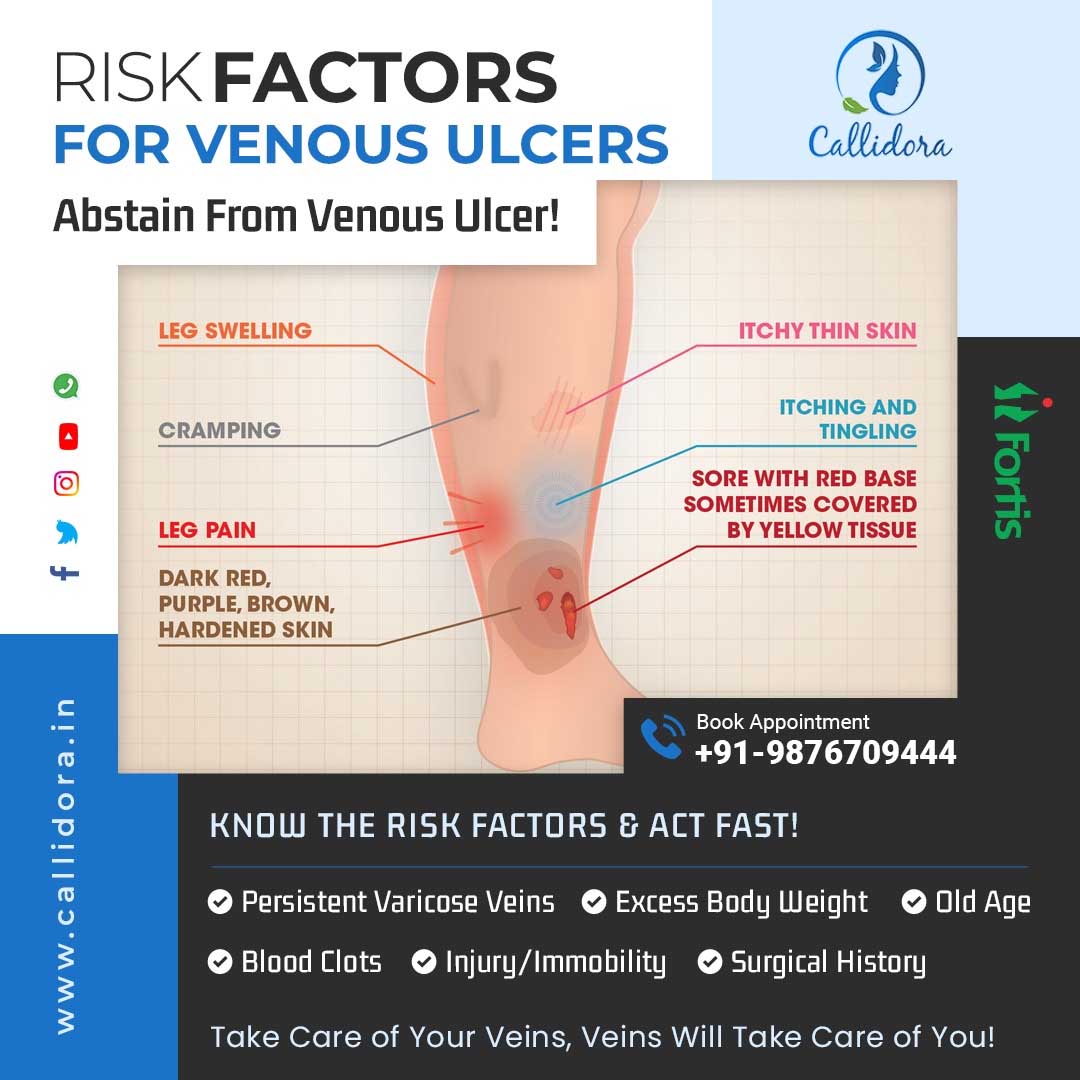
If youve ever spotted a stubborn sore on your lower leg that just wont quit, you might be wondering whether youre facing a leg ulcer risk. The short answer: yes, that could be a sign that something deeper is going on, and acting fast can make a huge difference. Below youll find the biggest risk factors, how to spot an ulcer at the very beginning, and the quickest proven ways to get it healing all backed by trusted medical sources and realpatient stories.
What Is a Leg Ulcer?
Definition and Common Types
A leg ulcer is an open wound that develops on the lower leg or ankle and fails to heal within six weeks. Not all ulcers are the same; they fall into a few main categories:
| Type | Typical Cause | Common Location | Healing Time (average) |
|---|---|---|---|
| Venous | Poor vein return (venous insufficiency) | Inside of the ankle or calf | 812 weeks |
| Arterial | Reduced arterial blood flow | Top of the foot or toes | 48 weeks (if revascularized) |
| Neuropathic | Diabetesrelated nerve damage | Pressure points on the foot | Variable, often chronic |
| Pressure (Decubitus) | Prolonged pressure on skin | Bony prominences, e.g., heel | 610 weeks |
Why Risk Matters
Doctors talk about leg ulcer risk because its easier to intervene before an ulcer becomes a fullblown problem. Knowing your risk helps you adopt preventive habits, catch an ulcer at the hives home treatment, and work with a woundcare team before complications set in.
Major Risk Factors
Age & Life Expectancy
Getting older naturally raises the chance of vascular changes. Studies show that people over 80 have a , and a chronic ulcer can modestly affect life expectancy. Its not a death sentence, but it does mean extra attention to overall health.
Venous Insufficiency & Past DVT
If youve ever had a deepvein thrombosis (DVT), your veins might be scarred, making blood pool in the lower leg. That pooling is the classic setup for a venous ulcer. A vascular surgeon I once chatted with reminded me, A past DVT is like a hidden crack in a dam if you ignore it, the water finds a way out.
Obesity, Immobility, and Lifestyle
Heavy weight presses on the veins, while sitting or standing for long stretches slows circulation. Smoking, pregnancy, and a family history of vascular disease also tip the scales. According to , losing just 510% of body weight can cut your ulcer risk in half.
Diabetes & Neuropathy
High blood sugar damages nerves and blood vessels, creating the perfect storm for neuropathic ulcers. Even a tiny unnoticed cut can turn into a big problem when sensation is dulled.
Occupational Factors
Jobs that require you to stay on your feet for hours (nursing, retail) or sit still at a desk without moving can both increase risk. The key is to keep the blood moving a quick walk or calf raise every hour works wonders.
Early Warning Signs
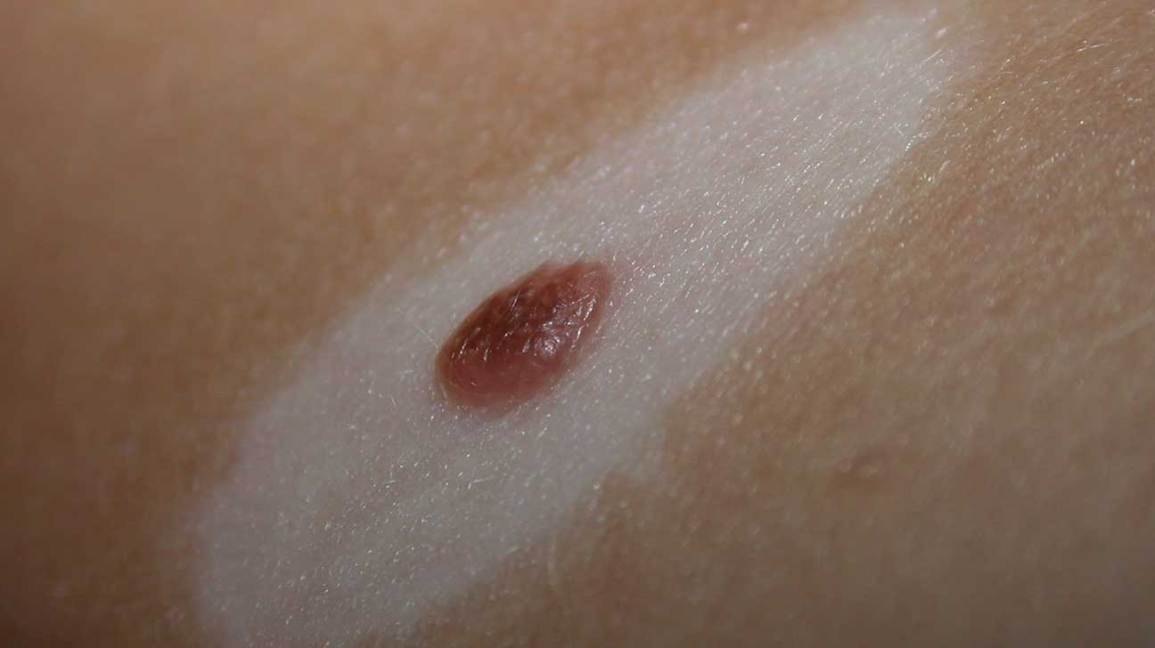
What Does a Leg Ulcer Look Like When It Starts?
At the very beginning you might see:
- A small red spot that doesnt fade
- Swelling around the ankle
- A thin, shiny crust forming over the spot
- Persistent itching or burning
These subtle cues often get dismissed as just a scratch. Thats why are useful they let you compare your own skin to typical earlystage images.
How to Differentiate from Minor Injuries
Unlike a normal scrape, an ulcers edge is usually irregular, and the wound may exude a thin fluid rather than clear blood. If you notice any of these signs lasting more than a few days, its time to call a healthcare professional.
SelfAssessment Flowchart (Quick Check)
- Is there a persistent red or brown spot? Yes: move to step 2.
- Is the area swollen or painful? Yes: consider a leg ulcer.
- Do you have risk factors (age, diabetes, venous disease)? Yes: book a woundcare appointment.
Fastest Healing Methods
Compression Therapy The Gold Standard
For most venous ulcers, properly fitted compression bandages or stockings are the fastest route to closure. A large found that multilayer compression reduced healing time by 30% compared with no compression.
StepbyStep: Applying a Multilayer Bandage
- Clean the wound gently with saline.
- Wrap the first (soft) layer snugly, overlapping 50%.
- Add the second (elastic) layer, stretching slightly.
- Finish with a cohesive layer to hold everything together.
Advanced Dressings
Hydrocolloid, alginate, and antimicrobial foam dressings keep the wound moist, which encourages faster cell growth. Recent trials on new treatment for leg ulcers showed that silverimpregnated dressings shaved off an average of 5 days from healing time.
Cost vs. Healing Time Table
| Dressings | Average Cost (per week) | Typical Healing Time |
|---|---|---|
| Hydrocolloid | $25 | 912 weeks |
| Alginate | $30 | 810 weeks |
| Silverantimicrobial | $40 | 79 weeks |
Adjunct Therapies
If compression and dressings arent enough, doctors may recommend skinreplacement grafts, lowfrequency shockwave therapy, or hyperbaric oxygen (HBOT). These options are usually reserved for ulcers that have stalled after 12 weeks of standard care.
When to Consider Advanced Options
Ask your wound specialist about a graft if you see:
- Less than 20% reduction in size after 8 weeks
- Persistent infection despite antibiotics
- Significant pain that limits mobility
Treatment Roadmap
Diagnosis What to Expect at the Doctor
First, the clinician will assess the wound, take your medical history, and run a few simple tests:
- AnkleBrachial Pressure Index (ABPI) measures arterial flow.
- Duplex ultrasound visualizes vein valves.
- Microbiology swab checks for infection.
Having a checklist of questions ready (e.g., When did the sore first appear?) makes the visit smoother and ensures you dont forget anything important.
Standard Care Pathway
Most leg ulcers follow a threestep regimen:
- Cleaning & Debridement remove dead tissue to promote healthy growth.
- Compression the cornerstone of venous ulcer healing.
- Dressing Choice tailored to wound depth and exudate level.
Following this plan, many patients see visible improvement within the first 4 weeks.
Typical 12Week Healing Curve (Graphic Description)
Imagine a line that starts flat (week 02), then climbs steeply as the ulcer shrinks (week 38), and finally levels off as the skin fully closes (week 912). Thats the pattern most clinicians aim for.
When Healing Stalls
If after 810 weeks the ulcer hasnt shrunk by at least 20%, its time to reassess. Possible culprits include inadequate compression, uncontrolled diabetes, or hidden infection. A decisiontree approach helps:
- Is compression correctly applied? If no, adjust fit.
- Is blood sugar under control? If no, coordinate with your GP.
- Any signs of infection? If yes, start targeted antibiotics.
Referral to a Specialist
When standard measures fail, a vascular surgeon or woundcare nurse can offer specialized interventions like skin grafts or endovascular procedures. For complementary skin concerns that sometimes appear alongside vascular issues, patients occasionally ask about topical remedies and broader skin conditions such as white skin lesion, which a clinician can evaluate during the same visit.
Living With an Ulcer
Impact on Daily Life
Beyond the physical wound, a leg ulcer can affect sleep, mood, and even social activities. Ive spoken with Sarah, a retired teacher, who said the constant dressing changes made her feel tethered to the bathroom. Acknowledging these feelings is the first step toward coping.
Life Expectancy with Leg Ulcers
Research published in the indicates that chronic leg ulcers slightly raise mortality risk, mainly because they often coexist with heart disease or diabetes. However, proactive treatment and lifestyle changes can bring those numbers back down to nearaverage levels.
Prevention Tips Reducing Future Risk
Heres a quick, printable checklist you can stick on your fridge:
- Wear graduated compression stockings daily (if advised).
- Elevate legs when sitting for more than 30 minutes.
- Do calfraise exercises 1015 times, 3 times a day.
- Keep blood sugar and blood pressure in target ranges.
- Quit smoking even cutting down makes a big difference.
- Inspect your legs every night for new spots or changes.
Emotional Support and Resources
Dont underestimate the power of community. Online forums, local woundcare support groups, and even a trusted friend who checks in can lift spirits on tough days. Sharing stories, like What is the fastest way to heal a leg ulcer? can spark ideas you hadnt considered.
Conclusion
Understanding your leg ulcer risk isnt just about memorizing medical jargon; its about recognizing the signs early, taking decisive action, and partnering with knowledgeable caregivers. By knowing the main risk factors, spotting an ulcer at its first whisper, and using the fastest evidencebased treatments, you dramatically boost your chance of a swift recovery and a healthier future.
If anything in this article resonated with you, grab the riskreduction checklist, share your own story in the comments, or reach out to a woundcare specialist today. Your feet deserve the same love and attention you give the rest of your body.
FAQs
What are the most common risk factors for leg ulcer risk?
Age, venous insufficiency, previous deep‑vein thrombosis, obesity, immobility, diabetes, smoking, and certain occupations increase the likelihood of developing a leg ulcer.
How can I tell if a skin spot is an early leg ulcer?
Early ulcers often appear as a small, persistent red or brown spot, may be itchy or burning, can have a thin crust, and are usually surrounded by swelling.
Is compression therapy safe for everyone with a leg ulcer?
Compression is the gold‑standard for venous ulcers, but it should be avoided or adjusted in patients with severe arterial disease, heart failure, or uncontrolled hypertension; a vascular assessment is essential.
Which dressing type promotes the fastest healing?
Silver‑impregnated antimicrobial dressings have shown the quickest healing times, followed by alginate and hydrocolloid dressings, especially when combined with proper compression.
When should I seek specialist care for a leg ulcer?
If the ulcer hasn’t reduced in size by at least 20 % after 8‑10 weeks, shows signs of infection, or causes significant pain, a referral to a wound‑care specialist or vascular surgeon is recommended.