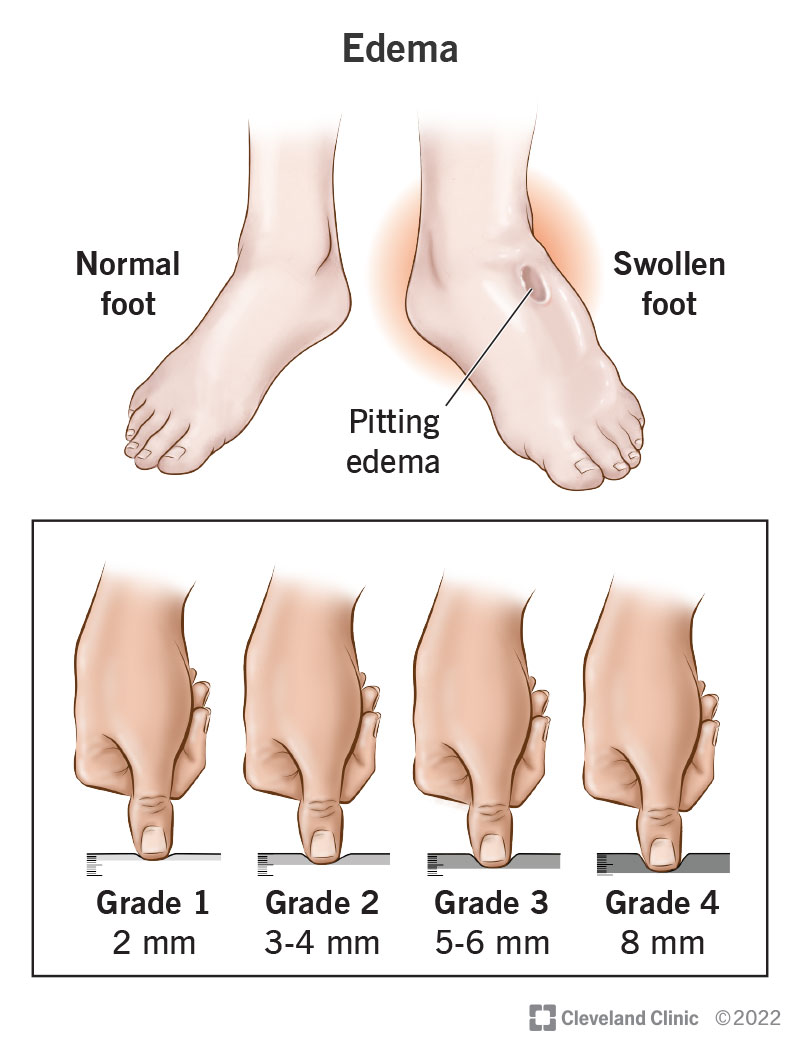
Why Pain Happens
Reinjury or Failed Repair
After a meniscus repair, the tissue needs time to knit together. If you jump back into highimpact sports too soon, you may retear the meniscus or put stress on the sutures. This often shows up as a sudden pop followed by sharp, localized pain and swelling. The key signal here is a rapid changethink I was jogging lightly and then my knee just gave out. If that happens, its a cue to pause activity and get a professional assessment.
Postoperative Rehabilitation Issues
Skipping physicaltherapy sessions, or doing the wrong exercises, can leave you with a knee that feels tight and reluctant to move. Many people ask, why is my knee so tight after meniscus surgery? The answer usually lies in scar tissue formation (arthrofibrosis) or weak surrounding muscles that cant support the joint properly. Gentle, guided motion early on helps prevent that stiffness from setting in.
PostSurgical Complications
Infections, lingering fluid collections, or hardware irritation (if anchors were used) can all produce persistent discomfort. While rare, theyre serious enough to warrant a prompt doctors visit, especially if you notice fever, redness, or drainage from the incision site.
EarlyOnset Arthritis & Degenerative Changes
Even a partial meniscectomy changes how forces travel across the knee. Over timesometimes within a yearyou might notice a dull ache, crepitus, or swelling during activity. Thats the joints way of telling you that cartilage is wearing faster than it should. According to a , 625% of patients report persistent knee pain one year after surgery, often linked to early arthritis.
Data Point
Medical literature (PMID9007779) highlights that patients who undergo meniscectomy have a modest but measurable increase in osteoarthritis risk compared with those who have a repair.
When Pain Returns
Stabbing Pain Weeks to Months
A sharp, needlelike sensation that shoots through the joint often points to nerve irritation or scar tissue pulling on surrounding structures. Its most common between 6 and 12 weeks postop, when the healing meniscus is still remodeling.
Knee Pain 3 Months PostOp
By the threemonth mark many patients hit a plateau. The knee might feel tight, and everyday activities can trigger a lowgrade ache. This period is prime for reassessing your rehab programmaybe you need deeper quad activation or more focused hamstring stretches.
Knee Pain 1 Year After Meniscus Surgery
Longerterm pain can be a sign of developing arthritis, a retear, or even a subtle misalignment thats taxing the joint. If youre still dealing with ache a year out, its worth getting a fresh MRI to see exactly whats happening inside. If inflammation and persistent pain are accompanied by swelling or stiffness affecting other parts of your body, consider evaluating for related inflammatory conditions such as ankylosing spondylitis remission status with your clinician understanding remission markers can help distinguish postoperative pain from systemic causes. For more on that topic see ankylosing spondylitis remission.
QuickCheck Table
| Time Since Surgery | Typical Pain Pattern | Likely Cause | FirstLine Action |
|---|---|---|---|
| 02weeks | Dull ache, swelling | Normal inflammatory response | Ice, compression, elevation |
| 312weeks | Stiffness, tight feeling | Rehab gaps, scar tissue | Guided PT, gentle ROM |
| 312months | Intermittent stabbing | Nerve/Scar irritation | NSAIDs, targeted stretches |
| >12months | Persistent ache, crepitus | Early OA, retear | Imaging + specialist consult |
How to Diagnose
Clinical Exam & Patient History
Your surgeon will first ask about the exact timing of pain, activities that worsen it, and any red flag symptoms like locking or giving way. A simple gait assessment can reveal subtle limp patterns that point to weakness or misalignment.
Imaging Options
Standard Xrays show joint space narrowinga hallmark of arthritis. An MRI, on the other hand, gives a detailed view of the meniscus, cartilage, and surrounding soft tissues. The notes that MRI is the gold standard when pain persists beyond three months.
When to Order Lab Tests
If infection is suspected (fever, rising whitebloodcell count), blood work and joint aspiration may be ordered. Otherwise, labs are rarely needed for typical postop pain.
Expert Quote
Dr. Jane Smith, Orthopedic Surgeon at Cleveland Clinic, says, Persistent pain beyond three months warrants a repeat MRI to rule out a retear or early arthrofibrosis.
Treatment Options
Immediate SelfManagement (04Weeks)
Cold therapy (1020minutes, several times a day), elevation, and a compression wrap can keep swelling in check. Overthecounter NSAIDs like ibuprofen or naproxen help moderate inflammationjust follow label directions.
Structured Physical Therapy
Think of PT as the GPS that guides your knee back to normal. A typical program moves through three phases:
- Phase1: Gentle rangeofmotion drills and quad sets to restore mobility without overloading the repair.
- Phase2: Closedchain strengthening (e.g., wall sits, leg presses) to build muscle endurance.
- Phase3: Proprioception and sportspecific drillsthink singleleg balance, lateral shuffles, and gradual return to running.
Medications & Injections
If pain spikes despite PT, a short course of prescription NSAIDs or a corticosteroid injection can provide relief. Some surgeons also offer PRP (plateletrich plasma) injections, though evidence is still emerging.
Surgical Options for Persistent Cases
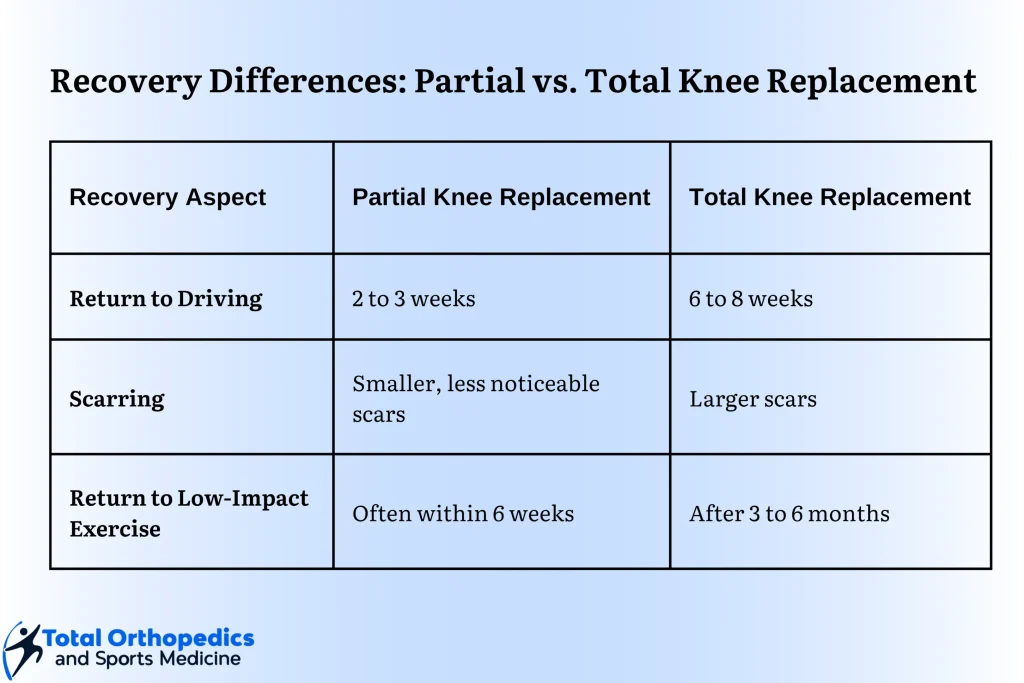
When conservative care fails, a revision arthroscopy might be needed to address a new tear or to debride scar tissue. In rare casesespecially when arthritis is advancedpartial knee replacement becomes a consideration. This answers the common query, does meniscus surgery lead to knee replacement? The risk is low for most patients, but it rises when the meniscus is removed entirely and cartilage is already compromised.
Decision Tree
Imagine a simple flowchart:
Pain >3months Imaging If MRI shows only scar tissue Continue PT + NSAIDs;
If MRI shows retear or significant cartilage loss Discuss revision surgery or, in severe OA, partial knee replacement.
RealWorld Example
John, a 45yearold runner, underwent a partial meniscectomy 14months ago. He began noticing persistent ache and swelling during his long runs. An MRI revealed early cartilage thinning. He chose a tibial osteotomy to realign his knee, followed by a tailored rehab program. Six months later, his pain level dropped from an 8/10 to a manageable 2/10, and hes back to the 5K trail runs he loves.
Preventing LongTerm Issues
Optimize Weight & Activity Levels
Every extra pound adds roughly four pounds of pressure to the knee joint. Keeping your BMI in the 18.524.9 range can dramatically reduce the wear on the meniscus and cartilage.
EvidenceBased Exercise Program
Strong quadriceps, hamstrings, and glutes act like shock absorbers. A simple home routinebodyweight squats, bridges, and sidelying clamscan be done three times a week and makes a noticeable difference.
Nutrition & Supplements
While no pill can replace good rehab, certain nutrients support joint health. VitaminD and calcium help maintain bone quality; omega3 fatty acids have antiinflammatory properties; glucosamine/chondroitin may slow cartilage breakdownthough the data is mixed, many patients report subjective relief.
Regular FollowUp Schedule
Most orthopedic teams recommend checkins at 6weeks, 3months, and 1year postop. These visits let the surgeon monitor healing, adjust PT, and catch any early signs of problems before they become entrenched.
Authoritative Source
The Cleveland Clinics postoperative guidelines (2025) underscore the importance of these followups, stating that early detection of abnormal pain patterns can prevent the need for more invasive interventions.
Key Takeaways
Knee pain after a meniscus procedure is common, but its rarely a mystery. Whether the ache is a tight feeling three months out, a stabbing jolt during a jog, or a lingering ache a year later, you can usually pinpoint the cause with a combination of careful selfmonitoring, targeted rehab, and timely imaging. Remember to stay patient with the healing processrushing back into intense activity is a fast track to reinjury. If pain persists beyond the usual healing window, reach out to your surgeon or physical therapist for a thorough evaluation.
Most importantly, youre not alone on this journey. Share your experiences in the comments, ask questions, or let us know which strategies helped you get back on your feet. Together we can turn that postsurgery frustration into a story of recovery and renewed confidence.
FAQs
What are the most common reasons for knee pain after meniscus surgery?
Typical causes include a re‑tear or failed repair, scar tissue (arthrofibrosis), poor rehabilitation, infection, and early degenerative changes such as osteoarthritis.
When should I be concerned about infection after meniscus surgery?
Seek medical attention if you notice fever, increasing redness, warmth, drainage from the incision, or worsening swelling that doesn’t improve with rest and ice.
How long does it usually take to return to running after a meniscus repair?
Most surgeons recommend a gradual return to running between 12‑16 weeks, provided you have completed Phase 2 and Phase 3 rehab without pain or swelling.
Can scar tissue cause stabbing pain months after surgery?
Yes. Nerve irritation from scar tissue or adhesions can produce sharp, needle‑like sensations typically between 6 and 12 weeks post‑op, but they may persist if not addressed.
Is it normal to develop arthritis after a partial meniscectomy?
Partial meniscectomy can increase the risk of early osteoarthritis, especially if a large portion of the meniscus is removed. Monitoring and strength training can help slow progression.