Short answer: most of the time the rhythmic whoosh in your ear is harmless, but it can sometimes be a warning sign of a vascular or neurological problem that needs prompt attention.
If the sound is brandnew, getting louder, changes when you tilt your head, or comes with headaches, vision changes, or dizziness, its time to make an appointment with a healthcare professional right away.
What Is Pulsatile Tinnitus
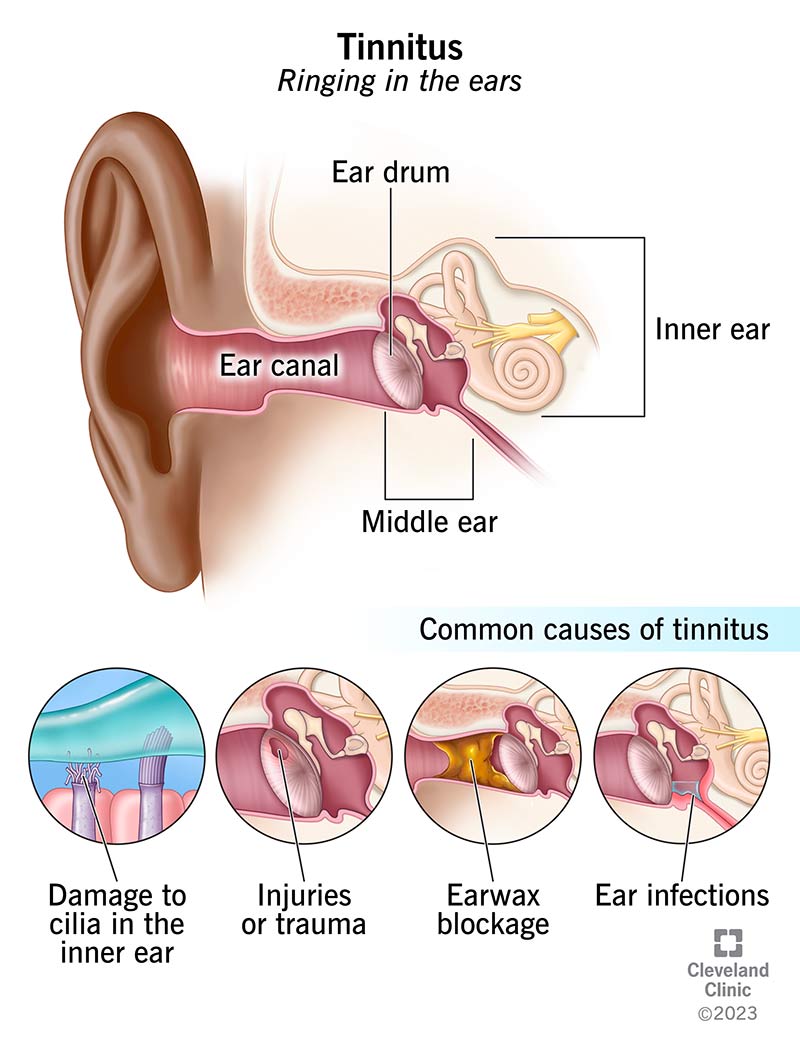
Pulsatile tinnitus is the perception of a rhythmic sound that matches your heartbeat. Unlike the steady ringing of classic tinnitus, this pulsing often feels like a tiny drumbeat inside the ear, and it can be heard in one ear only or both.
It happens when something in or near the ear creates a vibration that the auditory system picks up. The causes range from completely benign (like a temporary rise in blood pressure) to serious (such as an aneurysm). Understanding why its happening is the first step toward deciding whether you need to worry.
How It Differs From Classic Tinnitus
- Timing: Pulsatile matches the pulse; classic is constant.
- Location: Often heard in one ear only.
- Triggers: Can change with head position, stress, or caffeine.
QuickFact Table
| Feature | Pulsatile Tinnitus | Classic Tinnitus |
|---|---|---|
| Sound pattern | Rhythmic, syncs with heartbeat | Continuous or intermittent hum |
| Typical cause | Vascular flow, tumor, hypertension | Noise exposure, earwax, medication |
| Urgency | May need urgent evaluation | Usually nonemergency |
When It Can Be Serious
Even though most cases are benign, a few situations can turn just a weird sound into a medical emergency. Its like discovering a tiny leak in your roof most drips are harmless, but if water starts rushing in, you need to act fast.
Vascular Emergencies
Arterial problems such as a carotidartery dissection, an intracranial aneurysm, or an arteriovenous malformation (AVM) can create turbulent blood flow that your ear picks up as a beating noise. These conditions can be lifethreatening if left untreated.
Neurologic Threats
A sudden increase in intracranial pressure, severe hypertension, or a stroke can also produce pulsatile sounds. When the brains blood vessels are under stress, the extra pressure can be transmitted to the inner ear.
RealWorld Example
John, a 52yearold accountant, thought the whooshing in his right ear was just stressrelated. When the sound intensified and he started getting blurry vision, a quick MRI revealed a small carotid aneurysm. Early detection saved him from a potentially catastrophic bleed.
RedFlag Warning Signs
- Sudden onset of the sound
- Increasing intensity, especially at night
- Changes with head position (e.g., louder when tilting the head)
- Associated symptoms: headache, dizziness, visual disturbances, or loss of balance
ImmediateAction Checklist
- Note when the sound started and how it changes.
- Check for accompanying symptoms (headache, vision changes).
- If any redflag is present, call your doctor or go to urgent care today.
Why Most Episodes Are Benign
For the overwhelming majority of people, pulsatile tinnitus is more of an annoyance than a danger. Think of it like a traffic jam you can see on a highway its there, its noisy, but its not going to crash your car.
Common Benign Causes
- Turbulent blood flow: High blood pressure, anemia, or even excitement can make blood rush a little faster, creating a soft hum.
- Benign tumors: Small growths such as glomus jugulare or paragangliomas can produce a vascular sound without being cancerous.
- Venous hums: A normal, lowpressure venous flow near the ear can be picked up as a faint beat.
Positional Influence
Many people notice the sound changes when they lie down, tilt their head, or turn to one side. Thats why pulsatile tinnitus changes with head position pops up in so many searches. The shift moves blood vessels slightly, altering the turbulence and the sound that reaches the inner ear.
For people exploring noninvasive ways to manage tinnitus symptoms alongside medical evaluation, some try techniques like tinnitus meditation to reduce the stress and anxiety that can amplify perception of the pulse.
Comparison Table: Common vs. Dangerous Causes
| Cause | Typical Prognosis | Frequency |
|---|---|---|
| High blood pressure (turbulent flow) | Manageable with medication | 510% of tinnitus patients |
| Benign vascular tumor (glomus) | Often removable surgically | Rare (12% of cases) |
| Carotid artery dissection | Potentially lifethreatening | Very rare (<0.1%) |
| Arteriovenous malformation | Requires specialist treatment | Rare |
How Doctors Diagnose the Cause
The diagnostic journey is a lot like a detective story. Your doctor gathers clues from your history, does a physical exam, and then orders the right forensic tests to pinpoint the source.
FirstStep Evaluation
During the initial visit, expect questions about when the sound started, how it changes, and any accompanying symptoms. Your doctor will also check your blood pressure, listen to your neck vessels with a stethoscope, and look inside your ear with an otoscope.
Imaging Toolbox
When a vascular or structural cause is suspected, imaging is essential. The most common studies include:
- MRI/MRA: Gives a detailed view of soft tissue and blood vessels. According to , MRI with magnetic resonance angiography is the gold standard for detecting AVMs and aneurysms.
- CT Angiography (CTA): Quick, excellent for bone and calcified vessels.
- Doppler Ultrasound: Noninvasive and useful for checking carotid artery flow.
Sample Imaging Report Excerpt
MRA of the head and neck reveals a 6mm saccular aneurysm at the proximal left internal carotid artery with no evidence of rupture. This kind of description helps the ENT or neurosurgeon decide on the next steps.
Specialist Referrals
Depending on the suspected cause, you may be sent to an otolaryngologist (ENT), a neurologist, a vascular surgeon, or a cardiologist. Each brings a different expertise, ensuring the right tool for the right job.
Expert Insight
Dr. Sarah Patel, a boardcertified ENT at , notes, When pulsatile tinnitus is unilateral and changes with head position, we prioritize vascular imaging because missing a carotid pathology can have serious consequences.
Treatment Options & Outlook
Once the cause is identified, treatment can range from simple lifestyle tweaks to sophisticated surgery. The good news? In many cases, fixing the root problem either eliminates the sound or makes it manageable.
Addressing the Root Cause
- Bloodpressure control: Antihypertensive meds often quiet the tinnitus.
- Surgical repair: For aneurysms, AVMs, or tumor removal.
- Endovascular procedures: Stenting or coiling can stop abnormal blood flow.
SymptomRelief Strategies
If the underlying issue cant be fully correctedor while you wait for surgerythere are ways to mask or lessen the noise:
- Whitenoise machines or hearing aids with builtin sound generators.
- Cognitivebehavioral therapy (CBT) to reduce the emotional impact.
- Reducing caffeine, alcohol, and nicotine, all of which can amplify vascular turbulence.
TreatmentComparison Chart
| Modality | Success Rate | Typical Recovery Time |
|---|---|---|
| Bloodpressure medication | 7080% symptom reduction | Weeks to months |
| Surgical tumor removal | 9095% resolution | Several weeks |
| Endovascular stenting | 8090% resolution | 12 days hospital stay |
| Soundmasking devices | Variable (depends on patient) | Immediate relief |
Is Pulsatile Tinnitus Curable?
When the sound is caused by a treatable lesionlike a tumor or a highpressure arterythe answer is often yes, we can cure it. When its due to chronic hypertension or agerelated vessel changes, we talk about management rather than a cure, but the good news is that many people achieve full relief after their condition is controlled.
Lifestyle Tweaks That Help
- Maintain a healthy weight and exercise regularly to keep blood pressure stable.
- Practice stressreduction techniques such as yoga or meditation.
- Avoid excessive salt, caffeine, and alcohol, which can heighten vascular noise.
Bottom Line & Takeaways
Heres the short version:
- If the pulsating sound is brandnew, getting louder, or comes with other neurological symptoms, treat it as urgentcall your doctor.
- Most of the time, the cause is benign and can be managed with medication, lifestyle changes, or simple soundmasking tools.
- Accurate diagnosis often requires imaging (MRI/MRA, CTA) and possibly a referral to a specialist.
- When a serious vascular or tumor cause is found, modern treatments have high success rates, and many patients experience full symptom resolution.
Dont let the beat in your ear keep you up at night. Keep track of what you hear, note any changes, and reach out for professional help when the redflag signs appear. Remember, you dont have to live with the rhythmtheres help out there, and a friendly doctor is just a phone call away.
Whats your experience with pulsatile tinnitus? Have you found a remedy that works for you? Share your story in the comments, or feel free to ask any questionsyoure not alone in this.
FAQs
What is pulsatile tinnitus and how does it differ from regular tinnitus?
Pulsatile tinnitus is a rhythmic sound that syncs with your heartbeat, often heard in one ear, whereas regular tinnitus is a constant or intermittent ringing not linked to the pulse.
When should I consider pulsatile tinnitus a medical emergency?
If the sound is sudden, getting louder, changes with head position, or is accompanied by headaches, vision changes, dizziness, or loss of balance, seek medical attention promptly.
Which serious conditions can cause pulsatile tinnitus?
Potential serious causes include carotid‑artery dissection, intracranial aneurysms, arteriovenous malformations, severe hypertension, and increased intracranial pressure.
What tests do doctors use to diagnose the cause?
Typical evaluations involve a physical exam, blood‑pressure check, otoscopic exam, and imaging such as MRI/MRA, CT angiography, or Doppler ultrasound to visualize blood vessels.
Can pulsatile tinnitus be treated or cured?
When a treatable lesion (e.g., tumor, aneurysm) is found, surgery or endovascular procedures often resolve the sound. Benign causes are usually managed with medication, lifestyle changes, or sound‑masking devices.