Short answer: Osteoporosis isnt cured in the way a cold disappears, but with the right plan you can halt bone loss, rebuild density, and dramatically lower fracture risk.
Why does that matter? Because the silent thinning of your bones can show up as unexplained leg pain, a sudden dip in height, orworst of alla fracture from a simple stumble. Lets cut through the confusion, talk about what really works, and give you a roadmap you can start using today.
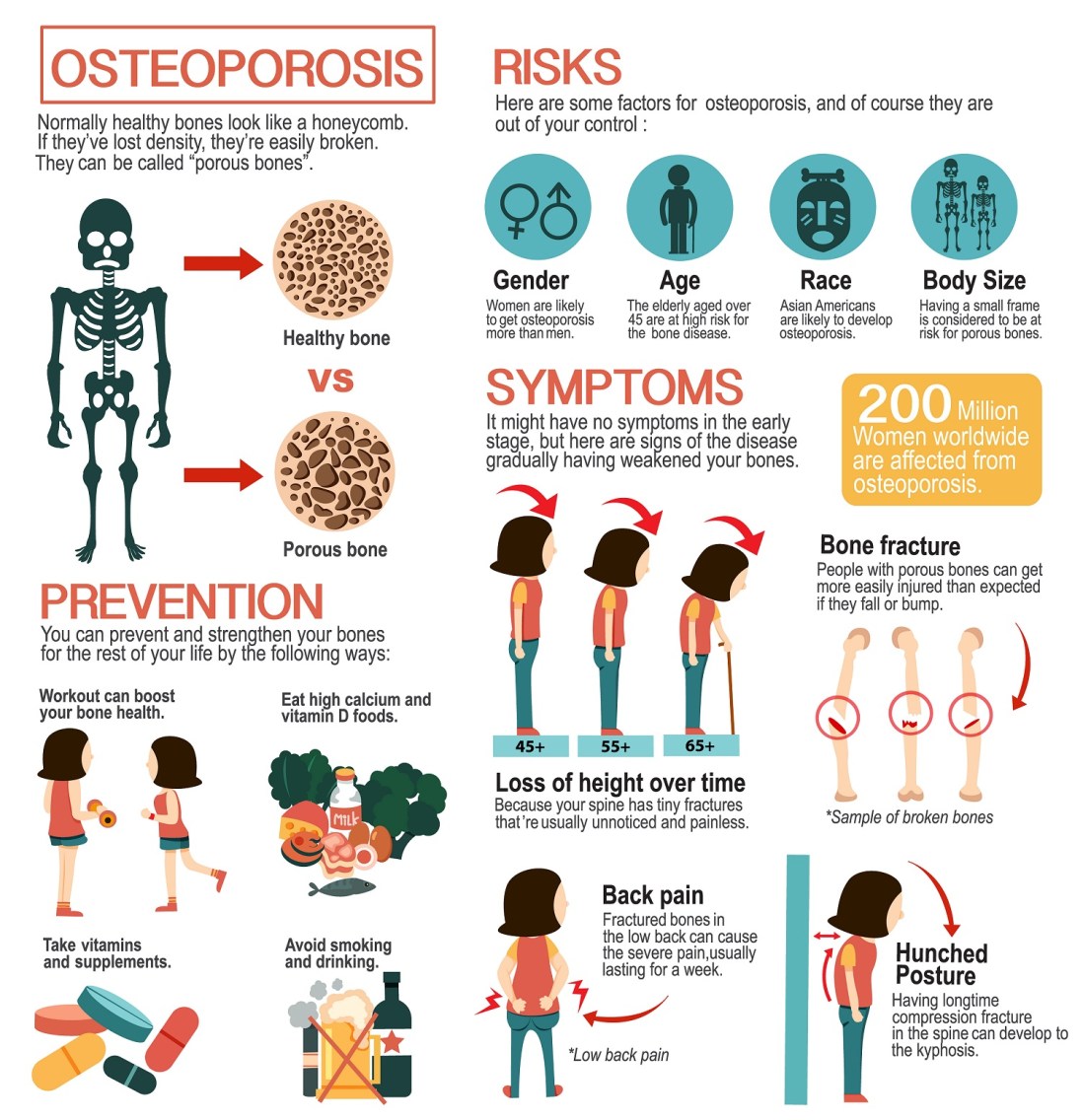
Understanding Osteoporosis
What causes osteoporosis?
Think of your skeleton as a house. Calcium and vitaminD are the bricks, while hormones like estrogen act as the mortar. When the mortar weakensoften during menopause, with low testosterone, or because of certain medicationsthe bricks start to crumble. Nutrient gaps, a sedentary lifestyle, smoking, and excessive alcohol also chip away at bone strength. Genetics plays a part, too; if close relatives have osteoporosis, your risk climbs.
Who is at risk?
Age is the biggest factorwomen over 55 and men over 65 see the steepest drops in bone density. But its not just about getting older. Anyone with a family history, a history of low-trauma fractures, or chronic conditions like rheumatoid arthritis should keep an eye on their bones.
Early warning signs
- Loss of height (more than 2cm)
- Persistent back or neck pain
- Fractures from minor falls
- Stooped posture (often called a dowagers hump)
- Unexplained leg painyes, osteoporosis can feel painful in the legs when tiny fractures develop in the femur.
Is osteoporosis hereditary?
About a quarter of your bonedensity risk comes from your DNA. A parent or sibling with osteoporosis raises your odds, but lifestyle choices can offset genetics. Regular weightbearing exercise and a calciumrich diet are your best defenses.
Cure or Control?
What does cure really mean?
In medicine, a cure eliminates disease entirely and permanently. For osteoporosis, we cant erase the underlying boneremodeling imbalance forever, but we can control it so effectively that you might never notice it again.
Can bone loss be reversed?
Yesseveral studies show that certain medications can increase bone mineral density (BMD) by 510% over a year. For example, a found that denosumab users gained an average of 8% BMD after 12months.
Is reverse osteoporosis in 6 months realistic?
Probably not for most people. Bone remodeling is a slow process; even the most potent drugs need several months to show measurable gains. Expect steady improvement, not an overnight miracle.
Balancing benefits and risks
Every medication carries potential side effects. Bisphosphonates, for instance, are great at slowing bone loss but can rarely cause jaw osteonecrosis. Denosumab is effective but requires continuous dosingmissing a shot can cause a rapid drop in BMD. Think of it like choosing a car: you weigh fuel efficiency against performance, safety, and cost.
Best Treatment Options
Medication comparison
| Drug Class | How It Works | Typical Dose | Main Benefits | Key Risks |
|---|---|---|---|---|
| Bisphosphonates (e.g., alendronate) | Inhibits boneresorbing cells | Weekly tablet | Proven fracture reduction | Esophageal irritation, rare jaw issues |
| Denosumab (Prolia) | Monoclonal antibody that blocks RANKL | Injection every 6months | Rapid BMD gains | Skin infection, rebound loss if stopped |
| Romosozumab (Evenity) | Stimulates bone formation, blocks resorption | Monthly injection (12months) | Highest BMD increase | Potential cardiovascular events |
| Hormone Therapy (estrogen/ testosterone) | Replaces lost hormones | Individualized | Improves bone & hot flashes | Breast cancer, clot risk |
What is the best and safest treatment for osteoporosis?
Best depends on your age, health, and personal preferences. For many postmenopausal women, a firstline bisphosphonate works well and has a solid safety record. If you cant tolerate oral meds, denosumab offers a convenient injection schedule. Always discuss your full medical history with a doctor before starting.
Nonpharmacologic approaches
- Calcium & VitaminD: Aim for 1,200mg of calcium and 8001,000IU of vitaminD daily. Food sources like leafy greens, fortified milk, and salmon are gold.
- Weightbearing exercise: Walking, jogging, dancing, or resistance training 34 times a week signals your body to lay down new bone.
- Fallprevention: Keep walkways clear, install grab bars, and wear shoes with good traction.
Emerging therapies
Researchers are exploring bonebuilding peptides and stemcell approaches, but most are still in clinical trials. Keep an eye on reputable news sites for updatesjust remember that miracle cures often turn out to be hype.
Lifestyle Strategies
Nutrition hacks
Heres a quick 7day meal plan to boost bone health:
- Breakfast: Greek yogurt with fortified granola and berries.
- Lunch: Spinach salad with salmon, almonds, and orange slices.
- Dinner: Stirfried kale, tofu, and brown rice, topped with sesame seeds.
- Snack: Cheese sticks or a handful of fortified orange juice.
This combo delivers calcium, vitaminD, magnesium, and vitaminK2all essential for bone remodeling.
Exercise routine
Try this threeday weekly template:
- Day1 Strength: 3 sets of 812 reps of squats, lunges, and dumbbell presses.
- Day2 Cardio + Weightbearing: 30minutes of brisk walking or dancing.
- Day3 Balance & Flexibility: Yoga or taichi for 20minutes, followed by light stretching.
Consistency beats intensityyour bones respond better to regular, moderate stress than occasional highimpact workouts.
Quit smoking & limit alcohol
Smoking cuts blood flow to bone tissue, while heavy drinking (>2 drinks per day) accelerates calcium loss. Cutting these habits can add up to 12% gain in BMD each year, according to the .
Supplements: what works?
Calcium carbonate is cheap and effective, but if you have stomach acid issues, calcium citrate absorbs better. VitaminD3 (cholecalciferol) is the preferred form; a daily 2,000IU dose is safe for most adults. Magnesium and vitaminK2 (found in fermented foods) can further support bone mineralizationjust check with your doctor before stacking supplements.
Monitoring progress
Schedule a DXA (dualenergy Xray absorptiometry) scan every 12years. Your doctor will give you a Tscore; a score above 1.0 is considered normal, between 1.0 and 2.5 indicates osteopenia, and below 2.5 signals osteoporosis. Tracking changes over time lets you see whether treatment is truly moving the needle.
When to Seek Help
Redflag situations
If you notice sudden, severe back pain, a noticeable height loss, or a fracture after a lowimpact fall, call your healthcare provider right away. Those can signal a compression fracture or advanced bone loss that needs immediate attention.
What to expect at the doctors office
A typical visit includes:
- A medical history review (family history, medications, lifestyle).
- A physical exam focusing on posture and gait.
- Lab tests: serum calcium, vitaminD level, and possibly parathyroid hormone.
- A DXA scan to quantify bone density.
Finding the right specialist
Endocrinologists, rheumatologists, and orthopedic doctors all treat osteoporosis. A good starter is your primary care physician, who can refer you to a bonehealth clinic if needed. When you meet a specialist, ask about their experience with the latest therapies and how they monitor side effects.
Insurance and cost considerations
In many countries, DXA scans are covered under preventive health benefits. Medications like bisphosphonates are often generic and inexpensive, while biologics (denosumab, romosozumab) may require prior authorization. Talk to your pharmacist about patientassistance programs if cost is a concern.
Conclusion
Bottom line: osteoporosis isnt curable in the classic sense, but it is highly manageable. By understanding the causes, recognizing early warning signs, and pairing evidencebased medication with solid nutrition and exercise, you can protectand even improveyour bone health.
Take the first step today: schedule a bonedensity test, discuss treatment options with a trusted doctor, and start adding a daily walk or a weightlifting routine to your schedule. Your skeleton will thank you, and youll feel more confident stepping into each new day.
For practical guidance on improving bone strength through targeted physical programs, consider reading more about osteoporosis physical therapy which outlines specific rehab and exercise approaches that complement medical treatment.
FAQs
Can osteoporosis be cured completely?
Osteoporosis cannot be “cured” like an infection, but it can be managed and bone loss can be halted or even modestly reversed with medication, nutrition, and exercise.
What medications actually increase bone density?
Bisphosphonates, denosumab, and romosozumab have all been shown in clinical studies to raise bone mineral density by 5‑10 % over 12‑24 months, reducing fracture risk.
How long does it take to see results from treatment?
Most patients notice measurable improvements in bone density after 6‑12 months of consistent therapy; significant fracture‑risk reduction often appears after the first year.
Are lifestyle changes enough to stop osteoporosis?
Nutrition (adequate calcium, vitamin D, magnesium, and vitamin K2) and regular weight‑bearing exercise are essential foundations, but most people also need medication to achieve optimal results.
When should I schedule a DXA scan?
Adults over 55 (women) and 65 (men), or anyone with risk factors like family history or low‑trauma fractures, should get a baseline DXA and repeat it every 1‑2 years to monitor progress.