If youve been told you have high blood pressure, youve probably heard doctors mention hypertensive heart disease in passing. In plain language, its the damage highpressure blood can do to your heart over time. It can show up as a thickened heart wall, trouble pumping blood, or even heartfailure symptoms.
Below, Ill walk you through what this condition looks like, why it happens, how you can spot it early, andmost importantlywhat you can do right now to protect your heart. No jargon, just honest, friendly advice that you can actually use.
Understanding Hypertensive Heart Disease
What does the term actually mean?
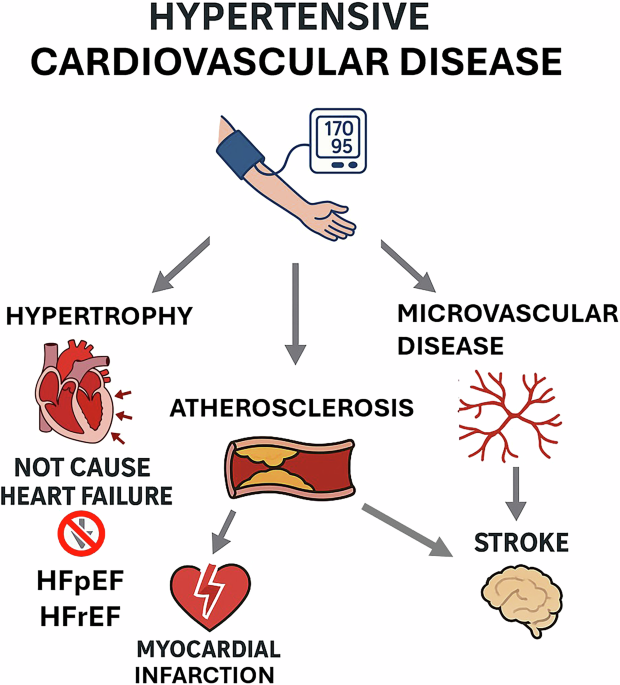
Hypertensive heart disease (HHD) is a blanket term doctors use for any heart trouble caused by longstanding high blood pressure. The damage can range from the left ventricle getting a bit too muscular (called leftventricular hypertrophy) to fullblown heart failure.
Why is it listed as ICD10 I11?
In the International Classification of Diseases, the code I11 stands for Hypertensive heart disease. Having the code handy helps your medical records stay organized and ensures you receive the right insurance coverage for tests and treatments.
ICD10 Quick Reference
| Code | Lay Description |
|---|---|
| I11 | Heart disease caused by high blood pressure |
| I11.0 | Hypertensive heart disease with heart failure |
| I11.9 | Hypertensive heart disease without heart failure |
How common is it?
Almost half of adults with stage2 hypertension develop some form of HHD if the pressure isnt controlled. Thats why early detection mattersonce the heart remodels, reversing the changes can be tougher, though not impossible.
Pressure Damage to Heart
What actually happens inside the heart?
Think of your heart as a garden hose. When the water pressure (blood pressure) stays high, the hose walls thicken to handle the strain. In the heart, the left ventricles muscle fibers grow thicker (hypertrophy) to push against the elevated pressure. Over time, the thick wall becomes stiff, making it harder for the heart to fill with bloodthis is the root cause of many HHD symptoms.
What are the main causes of hypertensive heart disease?
Beyond the obviouspersistently high systolic/diastolic numbersseveral factors can accelerate damage:
- Genetics: a family history of hypertension or heart disease.
- Age: arteries lose elasticity as we get older.
- Obesity and a sedentary lifestyle: both raise blood pressure and strain the heart.
- Sleep apnea: nighttime oxygen dips spike blood pressure.
- Excessive sodium intake and chronic stress.
According to a study published in , each 10mmHg increase in systolic pressure raises the risk of leftventricular hypertrophy by roughly 30%.
Can hypertensive heart disease be reversed?
Yesif caught early. Aggressive bloodpressure control, combined with lifestyle tweaks, can shrink the thickened muscle and improve pumping ability. A 12month trial at Penn Medicine showed a 15% reduction in leftventricular mass for patients who kept their systolic pressure below 130mmHg.
Recognizing Common Symptoms
Why does HHD often feel silent?
In its early stage, HHD may produce no noticeable signs. Thats why routine bloodpressure checks are vital. The heart can adapt for years before you feel any strain.
What are the first redflag symptoms?
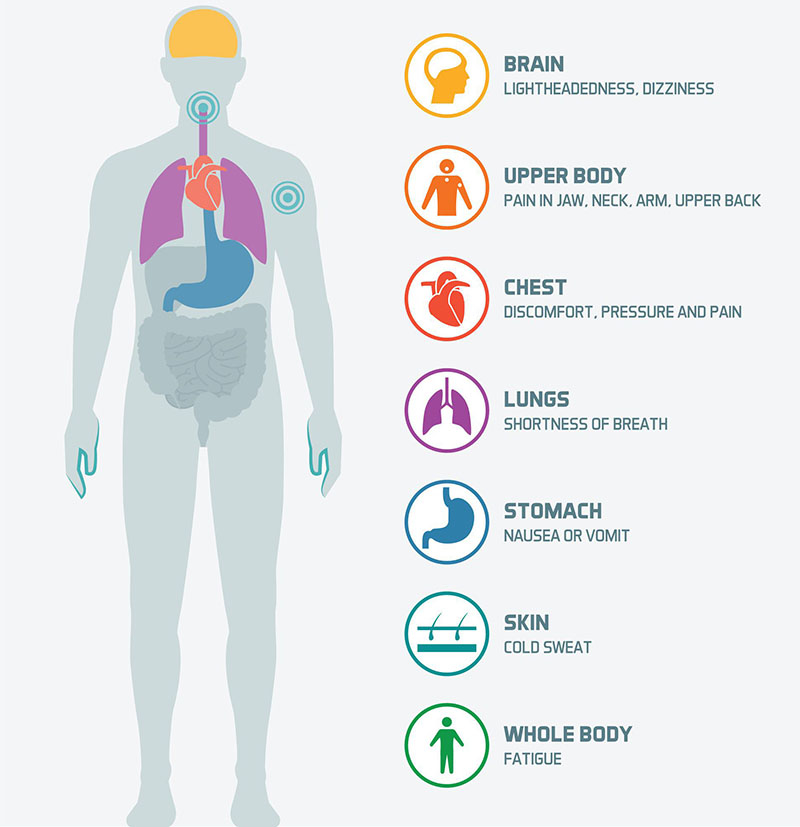
- Shortness of breath during mild activity (e.g., walking up a single flight of stairs).
- Unexplained fatigue or a feeling of heaviness in the chest.
- Occasional palpitationsthose fluttery sensations you cant quite explain.
When does it progress to heartfailure symptoms?
If the pressure continues unchecked, the hearts ability to pump efficiently declines. You might notice:
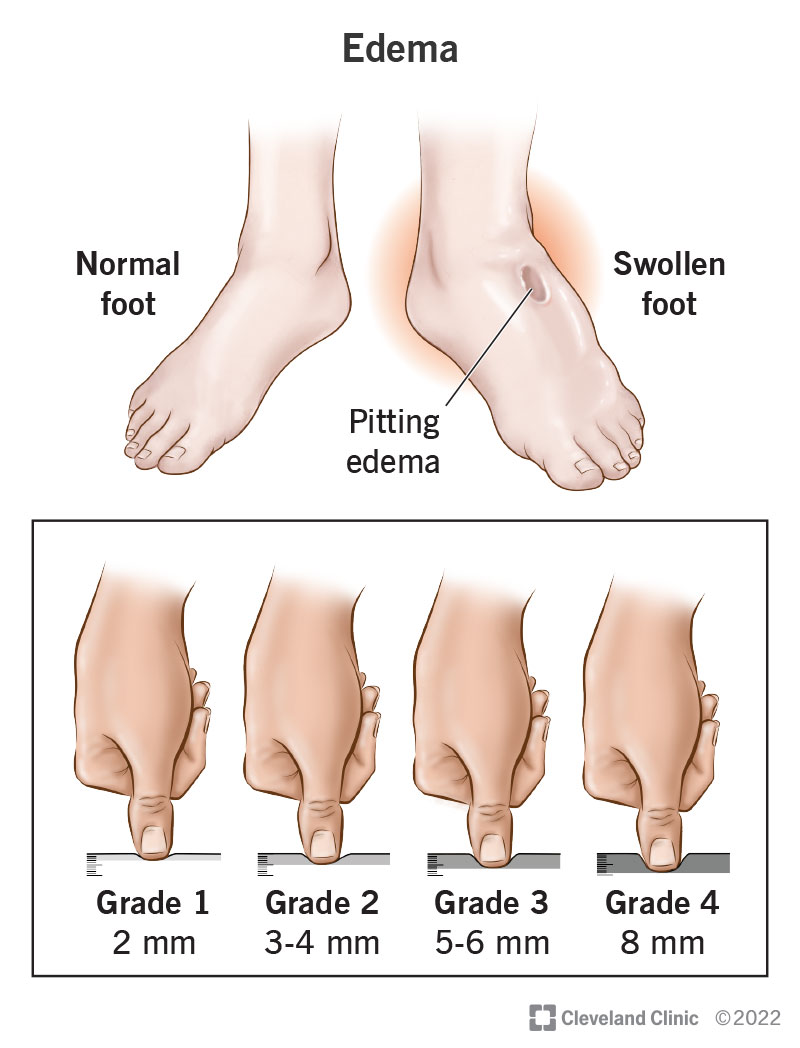
- Swelling in the ankles or lower legs (edema).
- A persistent cough, especially at night.
- Orthopneahaving to prop yourself up with pillows to breathe while lying down.
- Sudden weight gain from fluid retention.
Is sudden death a real risk?
While rare, uncontrolled HHD can set the stage for deadly arrhythmias. A metaanalysis in linked severe leftventricular hypertrophy with a 2fold increase in sudden cardiac death.
How Doctors Diagnose It
What does the physical exam reveal?
Doctors often feel a thrilla vibration over the chest wallindicating thickened heart muscle. Theyll also listen for abnormal heart sounds (S4 gallop) that hint at a stiff ventricle.
Which imaging tests are most useful?
- Echocardiogram: The goto tool for spotting leftventricular hypertrophy and measuring heartfunction numbers.
- Electrocardiogram (ECG): Shows characteristic voltage changes in HHD.
- Cardiac MRI: Offers a detailed picture when echo results are ambiguous.
Do blood tests help?
Lab work can reveal underlying contributorslike high cholesterol, kidney dysfunction, or diabetesthat often accompany high blood pressure.
Treatment Options Overview
Whats the first line of treatment?
Controlling blood pressure is the cornerstone. Most patients start with a combination of lifestyle changes and medication.
Medication Classes (Pros & Cons)
| Class | Typical Drug | Pros | Cons |
|---|---|---|---|
| ACE Inhibitors | Lisinopril | Renal protection, lowers afterload | Cough, rare angioedema |
| ARBs | Losartan | Similar to ACE inhibitors, no cough | Higher cost |
| Thiazide Diuretics | Hydrochlorothiazide | Effective, inexpensive | Electrolyte imbalance |
| CalciumChannel Blockers | Amlodipine | Good for isolated systolic HTN | Edema, gum overgrowth |
How do lifestyle changes fit in?
Think of them as the secret sauce that boosts medication effectiveness. Here are the top evidencebased habits:
- DASH diet: Emphasizes fruits, veggies, whole grains, and lowfat dairy while cutting sodium.
- Regular aerobic activity: Aim for 150minutes of moderateintensity exercise per week (brisk walking, cycling, swimming).
- Weight management: Losing even 510% of body weight can drop systolic pressure by 510mmHg.
- Stress reduction: Mindfulness, deepbreathing, or yoga can blunt the bloodpressure spikes caused by anxiety.
What about hypertensive heart disease with heartfailure symptoms?
If youve already developed HHD with heartfailure signs, doctors add drugs proven to improve mortality:
- Betablockers (e.g., carvedilol) to lessen the hearts workload.
- Aldosterone antagonists (e.g., spironolactone) to reduce fluid retention.
- SGLT2 inhibitors (e.g., dapagliflozin)originally for diabetes but now a frontline heartfailure therapy.
Patients who develop significant leg or peripheral swelling from heart failure should also have evaluation for causes and treatment; useful background on managing swelling and leg swelling cause can help guide conversations with your clinician.
Can this condition be reversed?
Yes, partially. Early, sustained bloodpressure control can shrink the thickened muscle and improve functional capacity. Its not a cure, but its a powerful way to halt progression and even regain some lost ground.
Managing Without Heart Failure
How can you keep tabs on your heart at home?
Invest in a validated automatic bloodpressure cuff. Measure twice a day (morning and evening) and record the numbers in a notebook or app. Consistency beats occasional perfection.
When should you see a specialist?
If any of the following occur, its time for a cardiology visit:
- Persistent systolic pressure above 140mmHg despite medication.
- New onset of shortness of breath, swelling, or chest discomfort.
- Abnormal results on your routine echo or ECG.
How to lower the risk of sudden death?
Beyond bloodpressure control, consider these strategies:
- Periodic Holter monitoring to catch silent arrhythmias.
- Discuss with your doctor whether an implantable cardioverterdefibrillator (ICD) is appropriate if you have severe leftventricular hypertrophy.
- Avoid excessive caffeine or stimulants that can precipitate arrhythmias.
Practical Takeaways Checklist
What can you do today?
- Check your blood pressure nowif you dont have a cuff, schedule a quick reading at a pharmacy.
- Swap one salty snack for a fresh fruit serving.
- Walk briskly for 10minutes after dinner; set a timer so you actually finish.
- Call your provider to discuss whether you need a medication adjustment.
Longterm roadmap
- Monthly: Record bloodpressure numbers and share them with your doctor.
- Quarterly: Request an echocardiogram if you have any new symptoms.
- Annually: Review medications and lifestyle plan with your cardiologist.
Remember, managing hypertensive heart disease is a marathon, not a sprint. Small, consistent steps add up to a healthier heart.
Conclusion
Hypertensive heart disease may feel intimidating, but you have the power to influence its course. By understanding the symptoms, staying on top of bloodpressure numbers, and pairing medication with heartfriendly habits, you can protect your heart and even reverse some of the damage. If anything in this guide sparked a question or youve got a personal story to share, drop a comment belowlets keep the conversation going. Your heart deserves the best care, and youre already on the right path.
FAQs
What is hypertensive heart disease?
Hypertensive heart disease is heart damage caused by prolonged high blood pressure, including thickened heart muscle and heart failure.
What are the common symptoms of hypertensive heart disease?
Early symptoms may include shortness of breath, fatigue, chest heaviness, and palpitations; advanced stages may cause swelling, cough, and difficulty breathing lying down.
How is hypertensive heart disease diagnosed?
Diagnosis involves physical exams, blood pressure monitoring, echocardiograms, ECGs, and sometimes cardiac MRI to assess heart structure and function.
Can hypertensive heart disease be treated or reversed?
Yes, early and sustained blood pressure control with medication and lifestyle changes can partially reverse heart muscle thickening and improve heart function.
When should I see a doctor for hypertensive heart disease?
Consult a cardiologist if blood pressure remains above 140 mm Hg despite treatment, or if symptoms like shortness of breath, swelling, or chest discomfort develop.