Quick Answer Overview
If youre wondering whether the joint pain will stick around for weeks or fade after a few days, the short answer is: migratory arthritis can last anywhere from a handful of hours to several weeks. The exact length depends on whats causing the flare, how quickly you start treatment, and each persons own immune response.
Heres a quick snapshot:
- Viraltriggered episodes usually hours to 35 days
- Reactive or autoimmunerelated flares days to 24 weeks
- COVIDrelated cases highly variable, often 12 weeks
In the sections below well break down why this range exists and what you can do to shorten the uncomfortable part.
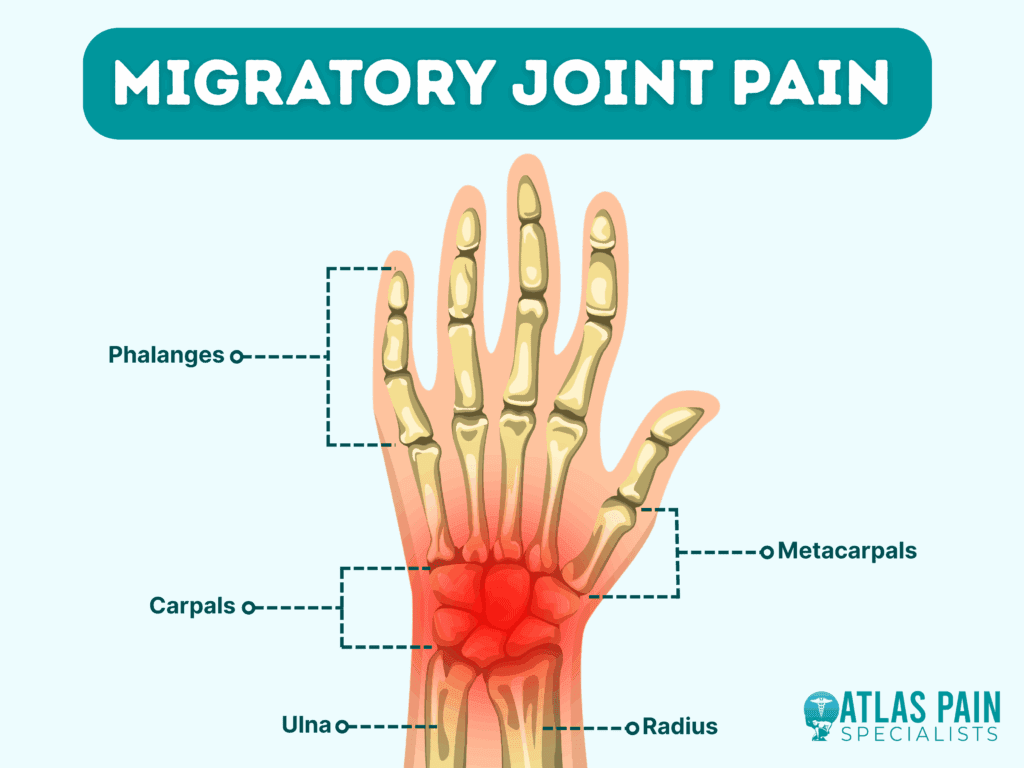
What Is Migratory Arthritis
Definition in plain language
Think of migratory arthritis as a wandering ache. One day you might feel a throbbing in your knee, the next day it has hopped over to your wrist, then your ankle. Its not a single joint thats constantly inflamed; instead the inflammation jumps from place to place, often within 2448 hours.
Key differences from other joint pains
| Condition | Pattern | Typical Duration |
|---|---|---|
| Palindromic rheumatism | Recurrent, brief attacks | Hoursto24hrs |
| Gout | Usually monoarticular | Daysweeks |
| Septic arthritis | Severe, constant | Daysweeks |
| Migratory arthritis | Moves between joints | Hoursweeks |
Top causes (the why)
Here are the most common culprits that set the jointhopping party in motion:
- Viral infections parvovirus B19, hepatitis B/C, EpsteinBarr, and the everpresent COVID19.
- Reactive arthritis a reaction after a gastrointestinal or urogenital infection.
- Autoimmune diseases lupus, spondyloarthritis, and, less often, rheumatoid arthritis.
- Medications or vaccines rarely, certain drugs can trigger a transient migratory pattern.
COVID19 and migratory arthritis
Since the pandemic began, clinicians have reported a surge of jointpain cases that behave just like classic migratory arthritis. A recent study in found that about 12% of postCOVID patients experienced joint pain that moved between joints, usually resolving within two weeks.
Whos most likely to develop it?
While anyone can get a migratory flare, the following groups see it more often:
- Adults aged 2045, especially after a viral illness.
- People with a history of reactive arthritis or other autoimmune conditions.
- Those who have recently recovered from COVID19.
Typical Duration Explained
How long do episodes usually last?
Most people notice a pattern: the pain starts suddenly, hits one joint hard for a day or two, then moves to another spot. In practice, youll see three broad categories:
- Shortlived flares 648hours, often viral.
- Mediumduration attacks 37days, usually reactive.
- Longer episodes 24weeks, linked to autoimmune triggers.
Factors that stretch or shorten an episode
Not all flares are created equal. Several variables can tip the scale:
- Underlying cause A cold virusinduced flare disappears fast; an autoimmune flare may linger.
- Immune system strength A robust immune response can clear the culprit quicker.
- Early treatment NSAIDs or targeted therapy started within 24hrs often curb the pain sooner.
- Lifestyle choices Sleep, stress, and diet all play subtle roles.
When does it become chronic?
If you find yourself dealing with joint pain that keeps migrating for more than a month, or you experience repeated cycles every few weeks, it may be edging into chronic territory. In that case, a rheumatologist will likely discuss diseasemodifying options. For patients with spondyloarthritis, tracking remission status is important; see resources on ankylosing spondylitis remission for guidance on how clinicians define and monitor disease control.
Acute vs. chronic vs. relapsing quick comparison
| Feature | Acute | Chronic | Relapsing |
|---|---|---|---|
| Typical trigger | Viral | Autoimmune/Reactive | Mixed |
| Avg. duration | HoursDays | >4Weeks | 23Weeks per flare |
| Treatment focus | Symptomatic | DMARDs/biologics | Both |
Spotting Symptoms Diagnosis
Common symptoms you might notice
Typical signs of a migratory flare include:
- Sudden joint pain that moves every 2448hours.
- Swelling, warmth, and a mild fever.
- Fatigue that seems out of proportion to the joint ache.
Simple symptom checklist
Use this quick selfscreen to see if youre dealing with migratory arthritis:
- Is the pain shifting from joint to joint? Yes keep reading.
- Did a viral illness or COVID19 infection happen within the past two weeks? Yes likely viral trigger.
- Is there noticeable swelling in each new joint? Yes inflammation present.
- Do you have a fever101F? Yes consider seeing a doctor quickly.
How is migratory arthritis diagnosed?
Doctors rely on a blend of history, physical exam, and targeted tests:
- Blood tests: CBC, ESR/CRP to gauge inflammation; viral panels if a recent infection is suspected; rheumatoid factor (RF) and antiCCP to rule out rheumatoid arthritis.
- Imaging: Xrays usually look normal early on; ultrasound can reveal synovial fluid in the affected joint.
- Joint aspiration: Rarely needed, but useful to exclude septic arthritis.
According to the , a thorough differential diagnosis is vital because conditions like gout or septic arthritis demand very different treatment pathways.
Migratory joint pain differential diagnosis
| Condition | Key Distinguishing Sign | Typical Duration |
|---|---|---|
| Palindromic rheumatism | Brief attacks 24hrs | Hours |
| Gout | Monoarticular, sharp pain, uric acid spikes | DaysWeeks |
| Septic arthritis | Severe pain, fever, rapid joint destruction | DaysWeeks |
| Migratory arthritis | Pain moves, often postviral | HoursWeeks |
Typical Duration Explained
Effective firstline treatment
When the pain starts, most clinicians recommend the classic resticeNSAID combo:
- NSAIDs (ibuprofen, naproxen) reduce inflammation quickly.
- Acetaminophen useful if NSAIDs aggravate the stomach.
- Rest and gentle movement dont bedrest for too long; a short walk keeps joints lubricated.
These overthecounter options usually shave a few days off an otherwise selflimited flare.
When prescription meds become necessary
If symptoms linger beyond a week, or if you have an underlying autoimmune condition, your doctor may move to diseasemodifying agents:
- DMARDs sulfasalazine, methotrexate, especially for reactive arthritis.
- Biologics TNF inhibitors (e.g., etanercept) for stubborn cases.
These medications arent for everyone; a rheumatologist will weigh benefits against risks such as infection susceptibility.
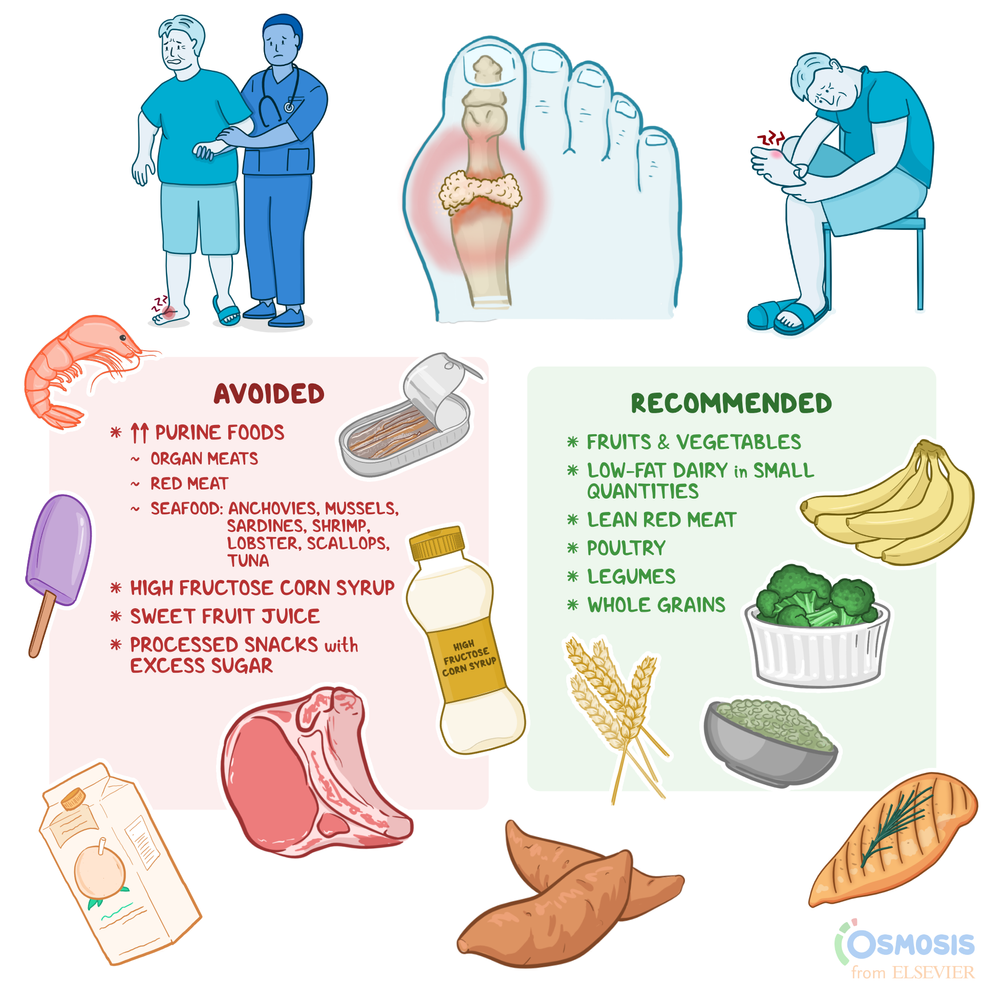
Migratory arthritis diet foods that may help
While no single diet cures the condition, certain foods consistently show antiinflammatory properties:
- Omega3 rich fish salmon, mackerel, sardines.
- Bright berries blueberries, strawberries, full of antioxidants.
- Leafy greens spinach, kale, packed with polyphenols.
- Spices ginger, turmeric, known to calm inflammation.
On the flip side, try to limit:
- Processed sugars and refined carbs.
- Excessive red meat and saturated fats.
- Alcohol especially during a flare.
Sample 3day antiinflammatory meal plan
- Day1: Breakfast oatmeal with blueberries; Lunch quinoa salad with kale and grilled salmon; Dinner roasted sweet potatoes, steamed broccoli, and a gingerturmeric broth.
- Day2: Breakfast Greek yogurt with strawberries and chia seeds; Lunch lentil soup with carrots; Dinner baked cod, wild rice, and sauted spinach.
- Day3: Breakfast smoothie (spinach, banana, flaxseed); Lunch turkey wrap with avocado; Dinner stirfried shrimp, bell peppers, and brown rice.
Redflag signs when to see a rheumatologist ASAP
Dont wait if you notice any of these:
- Joint swelling that lasts more than 48hours.
- Fever 101F or chills.
- Severe pain that prevents you from walking or using your hands.
- Rapidly worsening symptoms despite NSAIDs.
Key FAQs Answered
Is migratory arthritis curable?
The short answer: many cases resolve on their own, especially when a virus is the trigger. However, if the underlying cause is an autoimmune disease, the condition can be managed but not always cured. Ongoing treatment can keep flares short and infrequent.
Can it be prevented?
While you cant stop every viral infection, good hygiene, timely vaccination (including COVID19 boosters), and a balanced antiinflammatory diet lower the odds of a severe flare.
How does COVID19 affect the timeline?
Data suggest postCOVID joint pain tends to linger a bit longer than typical viral flaresaveraging around 1014days. Most patients see improvement as the immune system clears residual inflammation.
How is it different from palindromic rheumatism?
Both conditions involve episodic joint pain, but palindromic rheumatism usually hits the same joint repeatedly and resolves within 24hours, whereas migratory arthritis hops between joints and can last several days per episode.
Real World Experience
Story: From a 2hour flare to a 3week bout
Meet Maya, a 32yearold graphic designer. After a mild COVID infection, she woke up with a sharp pain in her left knee that vanished by evening. By day two, her wrist started hurting, then her ankle on day three. She tried ibuprofen and rest, but the pain kept shifting for three weeks. Once she consulted a rheumatologist, she started a short course of corticosteroids and added omega3 supplements. Within a week, the migratory pattern stopped, and shes now back to marathon training.
Takeaway? Early professional guidance can shrink a multiweek saga into a matter of days.
Expert voice: Why early treatment matters
Dr. Elena Martnez, a boardcertified rheumatologist at Mayo Clinic, explains, When we intervene within the first 48hours of a migratory flareespecially with NSAIDs or targeted steroidswe often prevent the immune cascade from locking into a prolonged inflammatory loop. She advises patients to track symptom movement in a simple diary; patterns can help pinpoint the trigger.
Conclusion
So, how long does migratory arthritis last? In a nutshell, the answer ranges from a few fleeting hours to several weeks, shaped by the cause, your bodys response, and how quickly you start treatment. Understanding the typical timeline helps you stay calm, seek help when needed, and adopt lifestyle habitslike an antiinflammatory diet and early NSAID usethat can trim the uncomfortable period.
If youve experienced a wandering joint ache, consider keeping a symptom log and reaching out to a healthcare professional sooner rather than later. You deserve relief, and with the right information and support, the pain doesnt have to linger longer than necessary. Got questions or personal stories about migratory arthritis? Feel free to shareyour experience could guide someone else on the road to recovery.
FAQs
How long does migratory arthritis usually last?
Migratory arthritis typically lasts from a few hours to several weeks, depending on the cause and individual factors.
Can migratory arthritis become chronic?
Yes, if joint pain keeps migrating for more than a month or recurs frequently, it may be considered chronic and require ongoing management.
What causes migratory arthritis?
Common causes include viral infections, reactive arthritis, autoimmune diseases, and sometimes medications or vaccines.
Is migratory arthritis curable?
Many cases resolve on their own, especially if triggered by a virus. Autoimmune-related migratory arthritis can be managed but not always cured.
When should I see a doctor for migratory arthritis?
See a doctor if joint swelling lasts more than 48 hours, you have a fever, severe pain, or symptoms worsen despite treatment.