Quick answer: Most men receive hormone (ADT) therapy for 624 months when it's paired with radiation, but in advanced or metastatic cases the treatment can extend to 3 years or longer. The exact length depends on cancer stage, overall health, side-effect tolerance, and whether the disease becomes resistant.
What Is Hormone
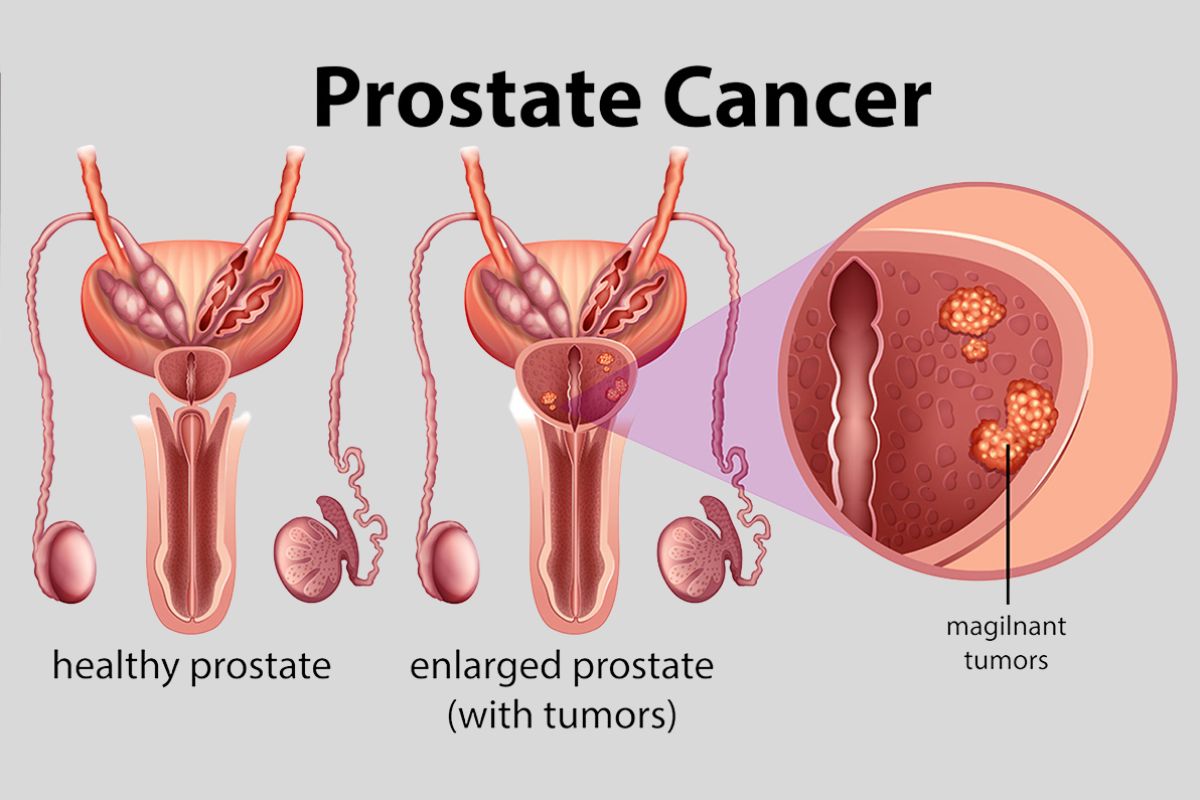
When we talk about hormone therapy for prostate cancer, we're really talking about androgen-deprivation therapy (ADT). Prostate cells love testosterone; ADT lowers the amount of that hormone in the body, starving the cancer cells and slowing their growth. In some cases, ADT is given after prostate removal as an adjunct treatment to reduce risk of recurrence and improve prostate removal life expectancy in high-risk patients.
Common Drugs & Formats
There are three main families of drugs:
- LHRH (GnRH) agonists e.g., leuprolide, goserelin.
- LHRH antagonists e.g., degarelix.
- Anti-androgens e.g., bicalutamide, enzalutamide. For more on advanced hormonal options, see our article on anti-androgens prostate cancer therapy.
Many men receive the medication as an injection that lasts every three months. This quarterly depot format makes it easier to stick to the schedule without daily pills.
| Drug | Brand | Administration Frequency | Typical Side-Effects |
|---|---|---|---|
| Leuprolide | Lupron | Every 3 months (injectable) | Hot flashes, fatigue, bone loss |
| Degarelix | Firmagon | Every month (injectable) | Injection site pain, nausea |
| Bicalutamide | Casodex | Daily oral tablet | Liver function changes, breast tenderness |
Standard Durations
Guideline-Based Ranges
Leading cancer societies give us a solid roadmap. Guidelines recommend up to six months of ADT before radiation, then continuing through and after radiotherapy for a total of up to three years in high-risk cases. Harvard Health adds that for many men a 4 to 24-month course hits the sweet spot, balancing effectiveness with side-effect burden. For those diagnosed at an early stage, you can learn more about approaches in our early prostate cancer guide.
Short-Term vs. Long-Term Protocols
| Protocol | Typical Duration | Clinical Goal | Key Studies |
|---|---|---|---|
| Neoadjuvant (pre-RT) | 36mo | Shrink gland before radiation | Prostate Cancer UK guideline |
| Adjuvant (post-RT) | 1236mo | Consolidate control | Harvard 2022 review |
| Metastatic/Advanced | Unlimited until resistance | Symptom control & survival | Mayo Clinic, NCI |
When Doctors Extend Beyond 3 Years
If the cancer has spread (stage 4) or is classified as high-risk locally advanced, many oncologists keep the hormone suppression going until the disease shows signs of becoming castration-resistant. That can be 35 years for some patients.
What Research Says About the Optimal Length
A 2019 Harvard analysis found that an 18-month ADT course improved overall survival compared with a six-month regimen for aggressive disease. On the flip side, a Mayo Clinic series reported that roughly half of men develop hormone resistance after 23 years of continuous therapy.
Influencing Factors
Cancer Stage & Risk Category
Early-stage (stage 12) cancers often don't need ADT at all, while stage 3 cancers usually receive a 12 to 36-month course. Stage 4 (metastatic) disease typically calls for indefinite treatment until resistance develops.
Age & Life Expectancy
Older men with limited life expectancy may forgo long-term ADT to avoid bone-weakening and metabolic side-effects. Conversely, a fit 60-year-old with a ten-year outlook might stay on therapy longer because the survival benefit outweighs the risks.
Side-Effect Profile & Tolerability
Common side-effects include hot flashes, fatigue, loss of libido, weight gain, and decreased bone density. If side-effects become intolerable, doctors may pause therapy, switch agents, or add supportive meds.
Managing Side-Effects Quick Tips
- Hot flashes: Layered clothing, cooling pillows, and low-dose antidepressants (e.g., venlafaxine).
- Bone loss: Weight-bearing exercise, calcium/vitamin D, and bisphosphonates or denosumab.
- Metabolic changes: Balanced diet, regular cardio, and monitoring blood sugar.
Personal Preference & Quality-of-Life Goals
Some men choose refusing hormone therapy after weighing the pros and cons. It's a deeply personal decision, and a good urologist will walk you through the tradeoffs without judgment.
When Therapy Fails
Castration-Resistant Prostate Cancer (CRPC)
After about 23 years of ADT, many cancers adapt and start growing again despite low testosterone. This state is called castration-resistant prostate cancer.
Next-Line Options
When ADT stops working, oncologists often add newer hormonal agents such as abiraterone or enzalutamide. If the disease progresses further, chemotherapy (docetaxel), PARP inhibitors, or even immunotherapy may be considered.
Decision Flow
- Confirm CRPC with PSA trend & imaging.
- Discuss second-line hormonal agents.
- Consider clinical trial enrollment.
- Plan for supportive care and symptom management.
Hormone + Radiation
Why the Combo Works
Radiation attacks the tumor locally, while ADT makes the cancer cells more vulnerable by depriving them of testosterone. Multiple trials show that the combination improves five-year survival by roughly 1015% compared with radiation alone.
Typical Schedule
In practice, many men receive six months of ADT before radiation (to shrink the gland), the radiation itself (usually over 8 weeks), and then another 1218 months of ADT afterward. That adds up to a 2 to 3-year total exposure.
John's Story
John, 68, was diagnosed with stage 3 disease in 2021. His doctor recommended a 30-month combined plan. After finishing radiation and hormone injections every three months, his PSA stayed undetectable for more than two years. He says the 30-month journey felt long, but knowing it gave him extra years with his grandkids made it worth it.
Cost Considerations
Average Annual Expense
In the United States, yearly ADT costs (drug + administration) range from $2,500 to $6,000, depending on the medication and insurance coverage. In the UK, NHS typically covers the cost, but private patients may face similar out-of-pocket fees.
Ways to Reduce Out-of-Pocket Costs
- Ask for the three-month depot formulation fewer clinic visits, often cheaper than monthly doses.
- Check manufacturer patient-assistance programs (many pharma companies offer free or discounted meds for qualifying patients).
- Discuss generic alternatives with your oncologist.
Real-World Experiences
Expert Insight
Dr. Emily Chen, a uro-oncologist with 15 years of experience, says: The goal isn't to keep a man on hormones forever; it's to tailor the duration to his disease biology and his personal tolerance. We constantly reassess PSA, imaging, and quality of life.
Patient Case Studies
- Mark, 55, stage 2: Chose a short six-month neoadjuvant course before radiation. He reported mild hot flashes but returned to work quickly.
- Antonio, 72, metastatic: Remains on ADT for four years. He adds a bone-protective bisphosphonate and says the therapy keeps my cancer in check, and I still enjoy gardening.
Takeaway Boxes
Lesson 1: Early-stage disease often needs only a brief hormone boost.
Lesson 2: Advanced disease may require indefinite therapy, but regular reassessment is key.
Talking To Your Doctor
Questions To Ask
- What is the specific goal of hormone therapy in my case?
- How long do you anticipate the treatment lasting?
- What side-effects should I watch for, and how can we manage them?
- Are there cheaper formulation options or assistance programs?
Preparing For The Appointment
Bring a simple symptom diary, a list of current medications, and any insurance information. Having these on hand makes the conversation smoother and shows you're an active partner in your care.
Printable Checklist (Downloadable)
Feel free to copy this list into a note-taking app before your next oncology visit.
- PSA trend chart
- List of side-effects experienced
- Questions about duration & cost
- Desired lifestyle goals (e.g., staying active, traveling)
Conclusion
In a nutshell, most men stay on hormone therapy for 624 months when it's combined with radiation, while those with high-risk or metastatic disease may continue for 3 years or more. The exact timeline hinges on cancer stage, personal health, side-effect tolerance, and individual goals. Talk openly with your oncology team, track how you feel, and remember that the length of therapy is a flexible decisionadjusted as you and your doctor learn more about how the cancer behaves. If you have questions or want to share your own experience, drop a comment below or reach out to a specialist you trust. Your journey is unique, and staying informed is the best ally you have.
FAQs
What is the typical length of hormone therapy when combined with radiation?
Most men receive hormone (ADT) therapy for 6 – 24 months when it’s paired with radiation, often split into a short pre‑radiation phase and a longer post‑radiation phase.
Can hormone therapy be stopped after a few months if side‑effects become severe?
Yes. Doctors may pause, switch agents, or add supportive medications. The decision is individualized based on cancer control, side‑effect burden, and patient preferences.
Why do some men need indefinite hormone therapy?
In metastatic or high‑risk locally advanced disease, hormone suppression is continued until the cancer becomes castration‑resistant, which can be 3 years or more.
What are the most common side‑effects of long‑term hormone therapy?
Hot flashes, fatigue, loss of libido, bone density loss, weight gain, and metabolic changes are typical. Lifestyle measures and meds (e.g., bisphosphonates, antidepressants) can help.
How is castration‑resistant prostate cancer (CRPC) managed after ADT fails?
When ADT no longer controls the disease (usually after 2–3 years), doctors add newer hormonal agents such as abiraterone or enzalutamide, and may consider chemotherapy, PARP inhibitors, or clinical trials.