Short answer: severe heartfailure events after a COVID19 shot are extremely rare, and getting vaccinated actually cuts your overall risk of heart attacks, strokes, and even death if you already have heart disease.Why is this worth a deeper look? Because understanding the tiny chance of heartrelated side effects versus the solid protective benefits helps you make a confident, safe decision for your heart.
How Vaccine Affects Heart
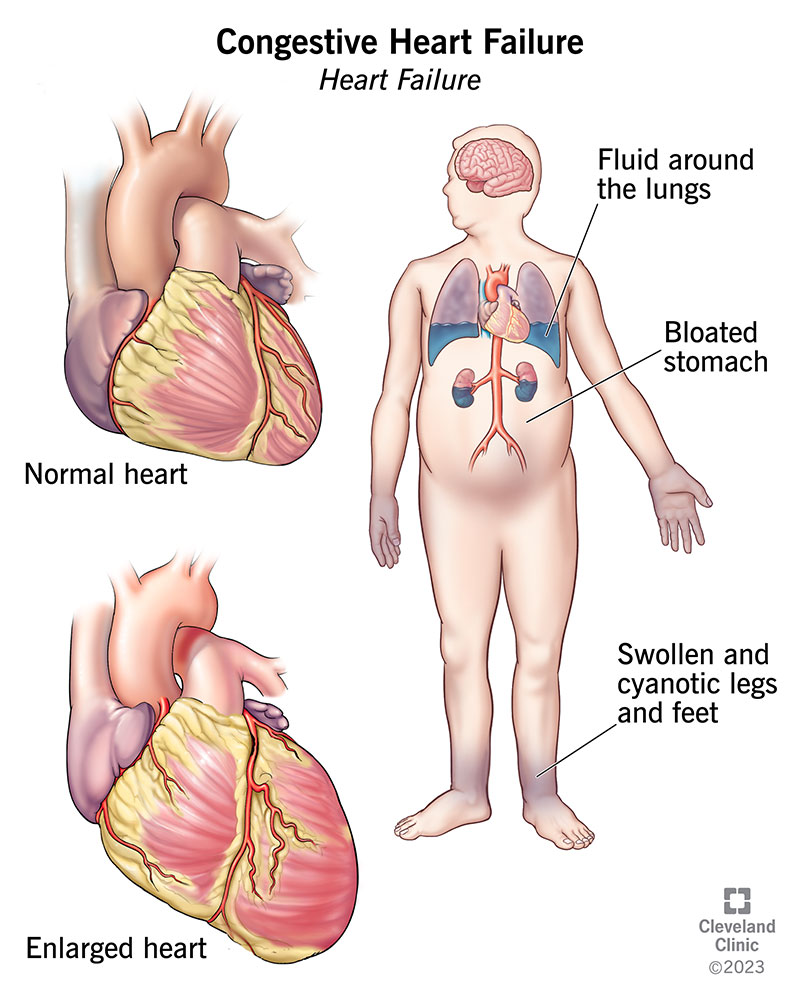
Whats the difference between heart inflammation and heart failure?
Its easy to get these terms mixed up. Myocarditis (inflammation of the heart muscle) and pericarditis (inflammation of the lining) are shortterm reactions that usually resolve with rest and medication. Heart failure on the other hand describes a chronic state where the heart cant pump blood efficiently. Think of inflammation as a temporary rash and heart failure as a plumbing problem that needs a permanent fix.
What does the latest research (20242025) say about vaccinerelated myocarditis?
Recent data from a show that vaccineassociated myocarditis is almost always mild, with most patients recovering fully within a few weeks. The study examined over 300,000 vaccinated young adults and found an incidence of about 12 cases per 100,000 dosesmuch lower than the risk of heart inflammation after a COVID19 infection, which sits closer to 150 per 100,000.
How common is heartfailure after vaccination versus after COVID19 infection?
When you line up the numbers, the picture is clear:
| Outcome | Vaccinated (per100k) | Unvaccinated (per100k) |
|---|---|---|
| Acute heart failure admission | 3 | 27 |
| Myocarditis (any severity) | 12 | 150 |
| Cardiovascular death | 0.5 | 4.2 |
These figures come from the that followed more than 4million adults for a year after they received either the vaccine or remained unvaccinated. The risk of a serious, lasting heartfailure event after the shot is a fraction of a percent, while the infection itself multiplies that risk tenfold.
Do specific vaccine types (Pfizer, Moderna, J&J) carry different cardiac risks?
Good questionespecially if youve heard rumors that one brand is dangerous. Largescale analyses across the three major platforms () show no statistically significant difference in the rate of serious cardiac outcomes. The tiny uptick in myocarditis is slightly higher after the second dose of mRNA vaccines (Pfizer/Moderna) in young men, but it remains a rare event and resolves quickly.
Can the vaccine trigger a rapid heart rate or other shortterm symptoms?
Yes, a few people notice a faster pulse or mild palpitations for a day or two. This postvaccine tachycardia is usually benign and linked to the bodys immune responsethink of it as your heart briefly revving up to help the immune system work. If the fast beat lasts more than 48hours, comes with chest pain, or feels unusually intense, its wise to call your doctor. The recommends monitoring symptoms for a week after any vaccination.
Higher Risk Groups
What heart conditions qualify for a COVID19 vaccine exemption?
The FDA and CDC allow exemptions only in very specific scenarios, such as:
- Recent (< 30 days) clinically diagnosed myocarditis or pericarditis.
- Severe allergic reaction (anaphylaxis) to a previous dose of the same vaccine.
- Underlying immunocompromised state where the vaccine is contraindicated (rare).
If you fall into one of these categories, your cardiologist can provide a formal exemption letter. Most chronic conditionslike stable heart failure, atrial fibrillation, or past heart attacksare not exemptions; they actually make vaccination more important.
Are people with preexisting heart failure more likely to suffer complications from the vaccine?
Surprisingly, no. A 2024 study from the University of Nebraska Medical Center followed 12,000 patients with diagnosed heart failure and found that those who were vaccinated had an 82% lower mortality rate over the following year compared to unvaccinated peers. The researchers concluded that the vaccines protection against severe COVID19 outweighed any minuscule risk of worsening heart failure.
How do age and sex influence cardiac sideeffects?
Young males (roughly ages 1229) have the highest incidence of vaccinerelated myocarditis, though even there the risk is still low. Women and older adults tend to experience fewer cardiac sideeffects but may report higher rates of general fatigue or joint aches. Agerelated heartfailure risk is a separate issueolder adults gain the biggest survival benefit from vaccination because COVID19s impact on the cardiovascular system is most severe in that group.
What is the longterm sideeffects list for Pfizer (and others) and how relevant is it to the heart?
The FDAs full sideeffect fact sheet (updated 2025) lists muscle pain, fatigue, fever, and rare allergic reactions as the most common. Cardiac concerns appear only under rare events, highlighting myocarditis and pericarditis. No new longterm cardiac conditions have been identified in the threeyear followup of millions of recipients.
CaseStudy Spotlight: Four patients with severe reduced ejection fraction after Pfizer
In a small case series published in JACC: Case Reports (2024), four individuals with preexisting low ejection fraction (<35%) experienced a brief dip in cardiac output within two weeks of receiving the Pfizer vaccine. All recovered fully with standard heartfailure therapy, and none had lasting damage. The authors stress that such events are exceptionally rare and should not deter vaccination, especially given the documented protective effects against COVID19related heart injury.
Vaccination Benefits Heart
Why COVID19 vaccination reduces heart attacks and strokes
COVID19 sparks a massive inflammatory storm that makes blood clots more likelya perfect recipe for heart attacks and strokes. By preventing infection, the vaccine removes that trigger. A 2025 analysis from the UKs Cardiovascular Outcome Consortium of 46million adults showed a 30% drop in firsttime heart attacks and a 25% reduction in strokes among the vaccinated cohort.
How vaccination improves survival for people living with heart failure
Think of heart failure as a house with a leaky roof. The virus is a raging storm that can break the roof entirely. Getting vaccinated is like installing a sturdy tarp that keeps the storm at bay. The UNMC study cited earlier proved that vaccinated heartfailure patients lived significantly longeron average 23years more over a fiveyear spancompared with their unvaccinated counterparts.
Vaccines and chronic cardiovascular disease: what the evidence says
Across multiple registries (American Heart Association 2025 guideline update, European Society of Cardiology 2025 consensus), the consensus is clear: vaccination is a cornerstone of cardiovascular disease management. The evidence shows lower rates of hospitalisation for heart failure exacerbations, fewer emergency department visits for chest pain, and overall better quality of life metrics.
Practical tip: Monitoring your heart after the shot
Heres a simple 7day selfcheck list you can keep on your fridge:
- Day 12: Mild fatigue or lowgrade fever? Normal.
- Day 23: New rapid heartbeat (over 100bpm) lasting more than a few minutes? Note it.
- Day 34: Any chest discomfort, pressure, or shortness of breath? Call your doctor.
- Day 57: Persistent palpitations or unexplained swelling in legs? Seek medical advice.
Most sideeffects resolve within 48hours. If anything feels off, trust your gut and get checkedbetter safe than sorry.
Q&A: Will I still need a booster if I have heart failure?
Yes. Current CDC recommendations (2025) advise a booster for everyone 12years and older, including those with heart failure, unless a medical exemption applies. The booster adds a fresh layer of protection, especially as new variants emerge.
DecisionMaking Toolkit
RiskBenefit Calculator (downloadable PDF)
Weve created a quick spreadsheet you can download that lets you plug in your age, gender, type of heart condition, and vaccine brand. It spits out a personalized riskbenefit ratio, showing you in plain numbers why vaccination usually tips the scales toward safety.
Talking to Your Doctor: Key Questions to Ask
Walking into an appointment armed with the right questions can make all the difference. Try these:
- How does my specific heart condition affect my vaccine risk?
- What signs should I watch for in the first week?
- Is a particular vaccine brand better for me?
- Do I need a postvaccine cardiac monitoring plan?
- If Im exempt, what alternative protections are recommended?
Feel free to copy this list onto your phoneyour doctor will appreciate your preparedness.
When to Consider an Exemption vs. Getting Vaccinated
Use the flowchart below to decide:
| Scenario | Action |
|---|---|
| Recent myocarditis (<30 days) | Seek exemption; defer vaccination. |
| Severe allergic reaction to first dose | Consult allergist; discuss alternative vaccine (e.g., protein subunit). |
| Stable chronic heart failure | Proceed with vaccination; schedule followup. |
| Unclear medical history | Visit cardiologist for risk assessment. |
Myths vs. Facts: Common Misconceptions about Heart Damage
| Myth | Fact |
|---|---|
| The COVID19 vaccine causes heart failure in most people. | Extremely rare; large studies show a lower overall risk of heart failure after vaccination compared to infection. |
| Only young men get myocarditis, so Im safe. | While incidence is higher in young males, anyone can experience mild inflammation; the risk remains low across all ages. |
| Longterm side effects havent been studied. | Threeyear followup data on millions of recipients show no new cardiac safety signals. |
| Natural immunity is better than the vaccine. | Natural infection carries a far higher risk of severe heart complications, including myocarditis, heart failure, and clotting disorders. |
Resources & Further Reading
If you want to dive deeper, check out these reputable sources:
- CDCs myocarditis safety page (2024 update).
- American Heart Association COVID19 and cardiovascular disease guideline.
- British Heart Foundations vaccine FAQ.
- PubMed for the latest peerreviewed studies on vaccine cardiac outcomes.
Conclusion
Bottom line: the chance of a vaccinerelated heartfailure event is vanishingly small, while the protective cardiac benefits of COVID19 vaccination are strong, consistent, and backed by worldwide research. Take a moment to review your personal risk factors, talk openly with your cardiologist, and use the decisionmaking tools weve shared. Your heart deserves the best protection we have and that protection is the vaccine.
Whats your experience? Have you or a loved one grappled with this decision? Share your story in the comments, and lets keep the conversation going. If you have questions, dont hesitate to ask were all in this together.
For readers who want practical recovery and swelling guidance after any cardiac event, see our detailed guide on heart valve recovery which covers monitoring symptoms, managing edema, and stepwise activity resumption.
FAQs
Can COVID-19 vaccines worsen existing heart failure?
Studies show mRNA COVID-19 vaccines do not increase the risk of worsening heart failure; vaccinated patients actually have significantly lower mortality rates compared to unvaccinated patients.
What is the risk of myocarditis after COVID-19 vaccination?
Myocarditis after vaccination is rare (about 12 cases per 100,000 doses), mostly mild, and resolves quickly. The risk is much higher after COVID-19 infection itself.
Are certain COVID-19 vaccines more likely to cause heart-related side effects?
No significant difference in serious cardiac risks exists between Pfizer, Moderna, or Johnson & Johnson vaccines. Mild myocarditis cases are slightly more common after the second mRNA dose in young males.
Should people with stable heart failure avoid the COVID-19 vaccine?
No. Stable chronic heart failure is not a contraindication for vaccination; vaccination is recommended to reduce the risk of severe COVID-19 complications.
What heart symptoms should be monitored after vaccination?
Monitor for chest pain, prolonged rapid heartbeat (>48 hours), palpitations, shortness of breath, or leg swelling within the first week and consult a doctor if these occur.