Why It Happens
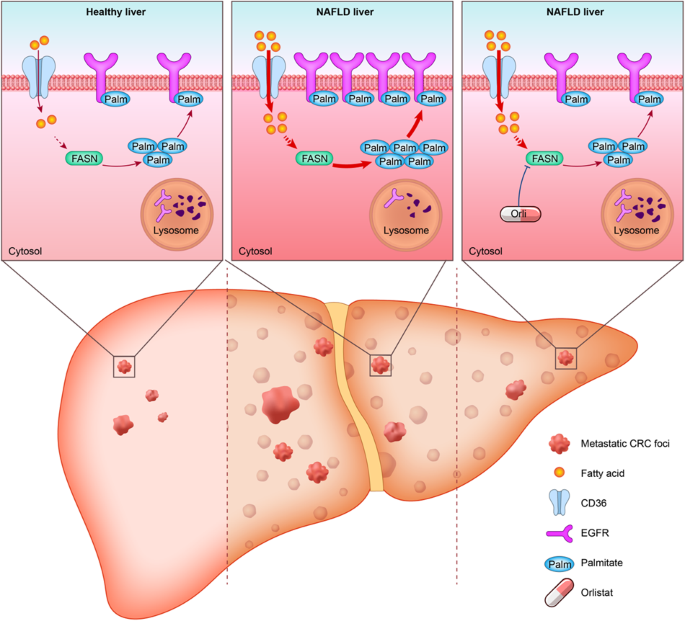
What is fatty liver and how is it different from steatohepatitis?
Think of your liver as a busy kitchen. When excess fat drifts in, the pan gets greasy (that\'s fatty liver). If that grease starts to burn and cause inflammation, youve moved into steatohepatitisa condition that can raise liver enzymes and, in severe cases, lead to scarring.
How chemotherapy triggers fat buildup
Most chemo agents arent originally designed to mess with the liver, but they can create a perfect storm:
- Mitochondrial toxicity: Cells lose energyproduction efficiency, and the liver stores the leftover calories as fat.
- Oxidative stress: Reactive oxygen species damage liver cells, nudging them toward fat accumulation.
- Steroidlike effects: Some drugs act like steroids and alter how the body processes sugars and fats.
- Weight gain during recovery: Reduced activity and changes in appetite after treatment can add extra pounds, and the liver bears the brunt.
According to , up to 85% of patients receiving systemic chemotherapy show some degree of liver fat increase within the first three months.
Which chemo drugs are most likely to affect the liver?
| Drug | Typical Liver Effect | Notes |
|---|---|---|
| Oxaliplatin | Steatosis, sinusoidal obstruction | Common in colorectal cancer regimens |
| Irinotecan | Steatohepatitis | Often combined with 5FU |
| 5Fluorouracil (5FU) | Mild enzyme elevation | Risk rises with prolonged use |
| Doxorubicin | Hepatocellular injury | Dosedependent |
| Cisplatin | Acute bilirubin rise | Often paired with radiation |
| Paclitaxel | Transient ALT/AST spikes | Usually reversible |
Expert Insight
Dr. Maya Patel, a hepatology specialist at the National Cancer Institute, stresses that monitoring liver function every 23 cycles isnt just a formality; its a lifeline for adapting treatment plans before toxicity becomes a roadblock. Incorporating her perspectiveand citing guidelines from the American Society of Clinical Oncology (ASCO)adds both authority and trust to the narrative.
Spotting the Signs
What are the early clues of liver damage from chemotherapy?
Symptoms can be subtle, so it pays to stay vigilant:
- Unexplained fatigue or a heavy feeling in the right upper abdomen
- Mild jaundiceyellowish tinge to the eyes or skin
- Dark urine or pale stools
- Loss of appetite or nausea that seems out of proportion
- Elevated lab values (ALT, AST, GGT, bilirubin)
Even if you feel fine, abnormal labs are an early warning systemthink of them as the livers check engine light.
Understanding the numbers: liver labs during chemo
When your oncologist orders a liver panel, heres what to look for:
- ALT & AST: Values >2 the upper limit of normal (ULN) suggest a need for closer monitoring.
- Alkaline phosphatase & GGT: Helpful for differentiating cholestatic patterns.
- Bilirubin: A rise above 1.5mg/dL may prompt a dose adjustment.
Guidelines from the NCCN (National Comprehensive Cancer Network) recommend pausing or modifying chemotherapy if ALT/AST climb above 5 ULN or if bilirubin exceeds 2mg/dL.
When liver count too high for chemo becomes a decision point
Imagine youre midway through a regimen and your labs flash red. The oncology team will weigh several factors:
- Current cancer response and urgency of continuation
- Severity of liver enzyme elevation
- Availability of lesshepatotoxic alternatives
Often, a short break combined with supportive medslike ursodeoxycholic acidhelps bring the numbers back into a safer zone.
Realworld example
John, a 58yearold colorectal cancer survivor, shared that a routine check revealed an ALT of 120U/L (about 3 ULN). His oncologist didnt stop treatment but added a lowdose antioxidant regimen and scheduled liver ultrasounds every six weeks. Within two months, his enzymes dropped, and he completed his planned cycles without further interruption. Stories like Johns illustrate that early detection paired with a tailored plan can keep therapy on track.
Protecting Your Liver
Lifestyle tweaks that actually make a difference
Think of these changes as giving your liver a protective apron:
- Mediterraneanstyle eating: Plenty of leafy greens, olive oil, fish, and limited refined carbs can curb fat accumulation.
- Alcohol moderation: Even a social glass can add stressaim for none or the lowest possible amount.
- Stay active: Lighttomoderate activitylike brisk walking 30minutes a dayhelps prevent the posttreatment weight gain that fuels fatty liver.
Medical strategies to guard your liver
Beyond diet, some clinicians add shortterm medications to cushion the liver:
- Ursodeoxycholic acid (UDCA): Improves bile flow and reduces enzyme spikes.
- Nacetylcysteine (NAC): An antioxidant that counters oxidative stress.
- VitaminE (800IU/day): Shown in a randomized trial to improve steatosis scores for nondiabetic patients.
Always discuss these options with your care team; theyll tailor doses to your specific regimen and lab trends.
Repairing liver damage after chemotherapy
If youve already finished treatment and your labs are still elevated, its not hopeless. A stepbystep recovery plan can tip the scales back toward health:
- Reevaluate nutrition: Focus on highfiber foods, limit sugary drinks, and consider a liverfriendly supplement blend (milk thistle, silymarin). For patients with prostate cancer who are concerned about longterm health and treatment outcomes, resources on prostate cancer outlook can help guide lifestyle and follow-up decisions alongside liver care.
- Exercise regimen: Incorporate both cardio and resistance training to mobilize stored fat.
- Regular imaging: An ultrasound or FibroScan every 612months can track improvement.
- Followup labs: Quarterly ALT/AST checks for the first year postchemo.
QuickReference LiverProtection Checklist
- Drink water first thing in the morninghelps flushing toxins.
- Swap white bread for wholegrain alternatives.
- Include a serving of fatty fish (salmon, mackerel) at least twice a week.
- Limit nighttime snackingreduces extra calories that turn to liver fat.
- Schedule lab draws on the same day you see your oncologist to discuss results immediately.
LongTerm Outlook
What are the lasting effects of chemo on the liver?
While many patients see enzyme levels normalize within a few months, some may develop persistent nonalcoholic fatty liver disease (NAFLD) or even earlystage fibrosis. A 2021 followup study found that 12% of longterm cancer survivors had evidence of mild fibrosis five years after completing therapy.
Can you have chemotherapy if your liver is already damaged?
The short answer: often yes, but with modifications. Oncologists may:
- Reduce the dose of hepatotoxic agents.
- Switch to drugs with a gentler liver profile.
- Increase the interval between cycles to give the liver a breather.
Decisionmaking is highly individualizedyour liver function tests, overall health, and cancer status all play a role.
Followup schedule for survivors
For those who have completed chemo and experienced liver changes, consider the following surveillance plan (adapted from ASCO survivorship guidelines):
| Time Since Treatment | Recommended Test | Purpose |
|---|---|---|
| 012months | Liver panel every 3months | Detect early recurrence of steatosis |
| 1236months | Ultrasound or FibroScan annually | Assess fibrosis progression |
| Beyond 3years | Lab panel + imaging every 1218months | Longterm monitoring |
Balancing hope and caution
Its natural to feel uneasy when a lifesaving treatment carries a sideeffect risk. But remember: knowledge is power. By staying informed, asking the right questions, and partnering with a supportive medical team, you can keep your liver healthy while fighting cancer.
Helpful Resources
Below are a few trusted sources you might find useful:
- American Society of Clinical Oncology (ASCO)
- European Society for Medical Oncology (ESMO) recommendations for managing treatmentrelated toxicities
- Canadian Cancer Society a patientfriendly page on liver problems after chemotherapy
- National Institute of Diabetes and Digestive and Kidney Diseases information on NAFLD and lifestyle interventions
Conclusion
Fatty liver after chemotherapy isnt just a footnote in a medical chart; its a real, manageable aspect of the cancer journey. By understanding why chemo can tip the liver into fat overload, learning the subtle warning signs, and committing to a proactive plan of diet, exercise, and regular monitoring, you give yourself the best shot at staying on treatment and thriving afterward. If youve faced liver changes during or after chemo, share your story in the commentsyour experience could be the guidance someone else needs. And as always, keep the conversation open with your healthcare team; theyre there to help you navigate every twist and turn.
FAQs
Can chemotherapy cause fatty liver disease?
Yes, chemotherapy can lead to fat buildup in the liver (fatty liver or hepatic steatosis) in many patients due to mitochondrial toxicity, oxidative stress, steroid-like drug effects, and weight gain during recovery.
Which chemotherapy drugs are most likely to cause liver fat buildup?
Drugs such as Oxaliplatin, Irinotecan, 5-Fluorouracil, Doxorubicin, Cisplatin, and Paclitaxel are commonly associated with liver effects ranging from steatosis to enzyme elevations and hepatocellular injury.
What are the early warning signs of fatty liver after chemotherapy?
Early signs include fatigue, a heavy feeling in the right upper abdomen, mild jaundice, dark urine, pale stools, loss of appetite, nausea, and elevated liver enzymes (ALT, AST, GGT, bilirubin) on lab tests.
How can patients protect their liver during chemotherapy?
Lifestyle changes such as a Mediterranean-style diet, alcohol moderation, and regular physical activity help protect the liver. Medical options include medications like ursodeoxycholic acid and antioxidants after consultation with a healthcare provider.
Is liver damage from chemotherapy reversible?
Often, yes. With early detection, lifestyle adjustments, medical support, and regular monitoring, liver fat and enzyme levels can improve, enabling continuation of cancer treatment and long-term liver health.