If youve just stumbled on the term familial dysautonomia gene, youre probably wondering what it means for you or someone you love. In a nutshell, a mutation in the ELP1 (formerly IKBKAP) gene throws a wrench into the nervous system and creates a rare disorder called familial dysautonomia.
\nBelow youll get the quick answers you need which gene is involved, how it shows up, how doctors test for it, and what treatment options exist today all written in plainlanguage, like a friend explaining the basics. Lets dive in.
\nWhat Is the Gene?
\nWhich gene causes familial dysautonomia?
\nThe culprit is the ELP1 gene, located on chromosome9q31. Most people with the condition carry a specific founder mutation thats especially common among individuals of Ashkenazi Jewish ancestry. This mutation reduces the production of a protein called IKAP, which is crucial for the development and maintenance of certain nerve cells.
\nWhere is the ELP1 gene located?
\nELP1 sits on the long arm of chromosome9, at bandq31. When a doctor orders a genetic test, the lab looks specifically at this region to spot the tiny change that can cause the disorder.
\nHow does the mutation affect the body?
\nIKAP is part of a larger complex that helps assemble proteins inside cells. When the ELP1 gene is faulty, nerve cells that control autonomic functionslike blood pressure, swallowing, and pain perceptiondont develop properly. The result is a cascade of symptoms that can feel like the bodys autopilot has gone haywire.
\nAccording to a review in NCBI GeneReviews, these nervecell deficits explain why patients experience chronic nausea, unstable blood pressure, and a blunted sense of pain.
\nKey Symptoms
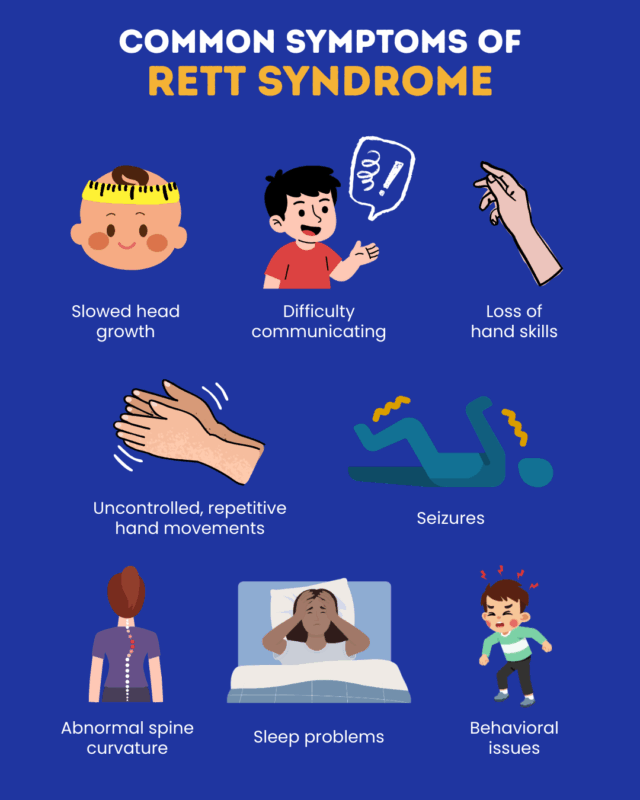
\nWhat are the hallmark symptoms?
\nThink of familial dysautonomia as a silent storm affecting many body systems, sometimes leading to autonomic neuropathy symptoms like low blood pressure or impaired pain sensation. The most common signs include:
\n- \n
- Frequent vomiting or nausea that doesnt respond to typical remedies \n
- Low blood pressure, especially when standing (orthostatic hypotension) \n
- Impaired ability to feel pain or temperature changes \n
- Reduced tear production leading to dry eyes \n
- Developmental delays in speech and motor skills \n
- Difficulty swallowing, which can cause aspiration pneumonia \n
Which symptoms are often brushed off?
\nBecause some of these signslike occasional dizziness or feeling clumsyare common in everyday life, they can be dismissed. However, when they appear together or early in childhood, theyre red flags that merit a closer look, potentially mimicking conditions with stress headache symptoms or other autonomic issues.
\nHow do symptoms differ in adults vs. children?
\n| Age Group | Typical Symptoms | Additional Concerns |
|---|---|---|
| Children | Recurrent vomiting, delayed milestones, poor growth | Feeding difficulties, frequent respiratory infections |
| Adults | Vertigo, chronic fatigue, autonomic crises | Joint degeneration, increased risk of hypertension |
Seeing this table, you might recognize familiar patterns. A teenager I once consulted described coffeeinduced jitters that lasted for hoursa classic autonomic crisis that appears more often after adolescence.
\nGenetic Testing
\nWho should get tested?
\nIf you have Ashkenazi Jewish heritage, a family history of the disorder, or a child showing the symptoms listed above, genetic testing is strongly advised. Prenatal screening can also identify the mutation before birth, giving families the chance to plan ahead.
\nWhat tests are available?
\nThe most reliable method is a targeted DNA sequencing test that looks directly at the ELP1 region. Many commercial labs, including , offer carrier panels that include the familial dysautonomia mutation. In the United States, newborn screening programs in several states already test for the disorder.
\nHow accurate are the tests?
\nClinical laboratories report sensitivity and specificity rates well above 99%. According to a study from the Cleveland Clinic, falsenegative results are exceedingly rare when the proper assay is used.
\nWhat do results mean?
\nResults fall into three categories:
\n- \n
- Positive: Two copies of the faulty genediagnosis confirmed. \n
- Carrier: One copyno disease but a 50% chance of passing it to offspring if the partner is also a carrier. \n
- Negative: No mutation detected; however, rare variants might require further investigation. \n
Treatment Options
\nIs there a cure?
\nUnfortunately, theres no cure yet. But the good news is that a combination of medication, therapy, and lifestyle tweaks can dramatically improve quality of life. Think of it as tuning a complicated instrumentyou cant replace the instrument, but you can keep it in harmony.
\nWhat medications help?
\nDoctors often prescribe drugs to manage specific symptoms:
\n- \n
- Midodrine for low blood pressure \n
- Ondansetron for chronic nausea \n
- Artificial tears for dry eyes \n
- Physical therapy to maintain muscle strength \n
These treatments arent a onesizefitsall; a neurologist will tailor the regimen to each persons symptom profile.
\nEmerging therapies
\nResearchers are exploring splicemodulating compounds that can coax cells to produce a functional version of the IKAP protein. Early-phase trials reported by show promising improvements in motor function, although the approach is still experimental.
\nLifestyle adjustments
\nSimple daily habits can make a world of difference:
\n- \n
- Stay hydratedsmall sips every hour help stabilize blood pressure. \n
- Eat smaller, more frequent meals to reduce nausea. \n
- Avoid extreme temperatures; a cool environment can lessen autonomic storms. \n
- Use a supportive cushion or harness when standing for long periods. \n
Life Expectancy
\nWhat is the typical life expectancy?
\nThanks to advances in supportive care, the median life expectancy has risen from the early 30s in the 1970s to the mid40s or early50s today. A recent epidemiological review in NCBI highlighted that early diagnosis and coordinated multidisciplinary care are key drivers of this improvement.
\nHow does early diagnosis affect outcomes?
\nChildren diagnosed before age three who receive regular physiotherapy and tailored medications tend to maintain better mobility and fewer hospitalizations. Early intervention also helps families make informed decisions about schooling and longterm planning.
\nCarrier Information
\nWho is considered a carrier?
\nA carrier has one copy of the mutated ELP1 gene but does not develop the disease. Carriers can pass the mutation to their children, especially if their partner is also a carrier.
\nCarrier testing and counseling
\nGenetic counselors play a vital role. They can explain reproductive options such as preimplantation genetic diagnosis (PGD) with invitro fertilization, or prenatal testing via chorionic villus sampling. Knowing your carrier status empowers you to make choices that align with your family goals.
\nReproductive planning
\nIf both parents are carriers, theres a 25% chance with each pregnancy of having a child with familial dysautonomia. Awareness early on allows couples to explore alternatives, whether its donor gametes, adoption, or deciding to accept the risk.
\nHelpful Resources
\nTrusted medical sites
\nFor reliable, uptodate information, check out:
\n- \n
- MedlinePlus \n
- CDC Genetics \n\n
Patient advocacy groups
\nConnecting with others can turn isolation into community. The offers support groups, research updates, and a donor registry.
\nPractical tools
\nConsider using symptomtracker apps (available on both iOS and Android) to log episodes of low blood pressure or nausea. These records are gold for your medical team when adjusting treatment plans.
\nConclusion
\nUnderstanding the ELP1 (familial dysautonomia gene) is the first step toward taking control of a complex condition. By recognizing key symptoms, pursuing accurate genetic testing, and embracing both current treatments and emerging therapies, patients and families can improve daily life and outlook. If you suspect you or a loved one might be affected, reach out to a genetics professional, explore the resources above, and stay informed about the latest research. Knowledge is powerand together we can navigate this journey with confidence and compassion.
FAQs
What gene causes familial dysautonomia?
The ELP1 gene (formerly IKBKAP), located on chromosome 9q31, causes familial dysautonomia through a specific mutation that reduces IKAP protein production, affecting nerve cell development.[1][2][3]
What are the main symptoms of familial dysautonomia?
Hallmark symptoms include frequent vomiting, orthostatic hypotension, reduced pain and temperature sensation, dry eyes, developmental delays, and swallowing difficulties.[1][2][3]
How is familial dysautonomia tested?
Targeted DNA sequencing of the ELP1 gene offers over 99% accuracy, identifying affected individuals, carriers, or negatives; recommended for those with Ashkenazi heritage or symptoms.[1][2][3]
Is there a cure for familial dysautonomia?
No cure exists, but symptom management with medications like midodrine and ondansetron, physical therapy, and lifestyle changes improves quality of life.[1][2]