How EBRT Works
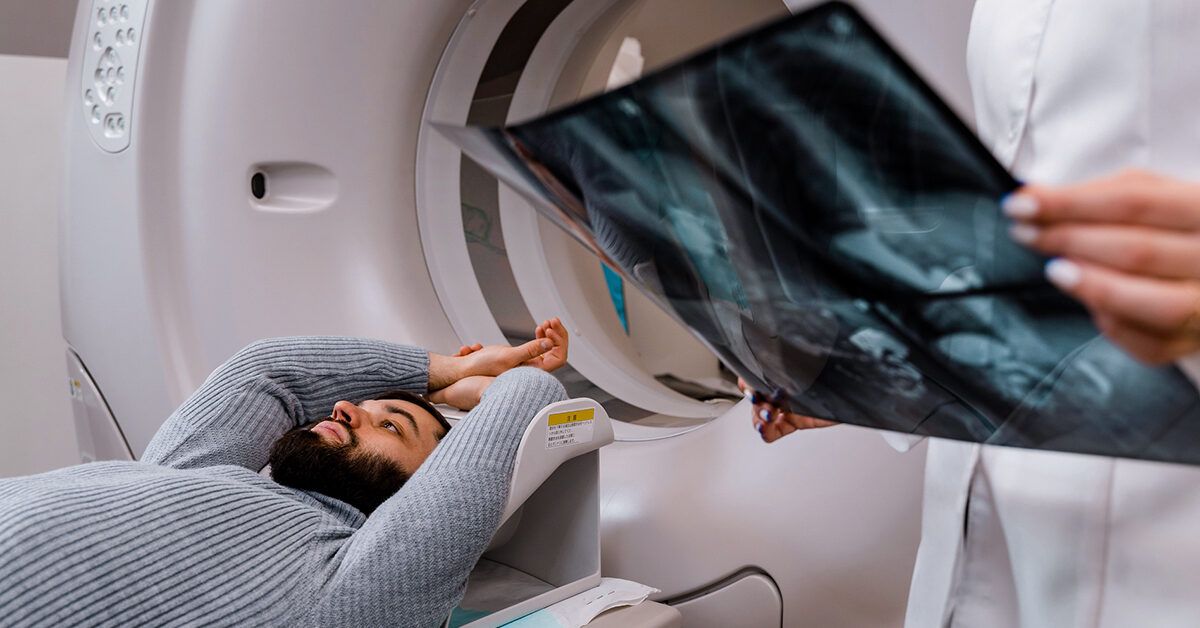
Think of external beam radiation therapy (EBRT) as a highprecision spotlight that zeroes in on the tumor while sparing the surrounding stage. A machine called a linear accelerator (or LINAC) produces highenergy Xrays that travel from outside your body right to the esophagus. The beams are sculpted by movable leaveslike tiny shuttersso they match the shape of the tumor. This shaping process is called multileaf collimation, and it lets doctors target the cancer with millimeter accuracy.
Before the first session, youll go through a simulation CT scan. This isnt a fullblown surgery; its a quick, painless scan that maps the exact location of the tumor and the neighboring heart, lungs, and spinal cord. A radiation oncologist then draws (contours) the tumor and critical structures on the images. After that, a dosimetrist calculates the doseusually between 50 and 60Gy totaldelivered in small hops (1.82Gy per fraction). The plan is reviewed by a physicist to make sure the numbers add up safely.
| Stage | Total Dose | Fractions | Approx. Length |
|---|---|---|---|
| Early (III) | 50Gy | 25 | 5weeks |
| Locally Advanced (III) | 60Gy | 30 | 6weeks |
| Palliative | 30Gy | 10 | 2weeks |
Seeing those numbers on a page can feel clinical, but theyre really just a roadmap for your journey. Every patients plan is customized, so the table is a guidenot a rulebook.
Success Rates Explained
What does success look like? For many, it means keeping the cancer under control long enough to enjoy lifes moments. When EBRT is paired with chemotherapy (the combo most often recommended), fiveyear overall survival rates hover around 3045% for locally advanced diseaseaccording to the . In earlystage cancers, survival can climb even higher.
These numbers are averages, not predictions for any single person. Your age, overall health, tumor location (upper vs. lower esophagus), and how well you tolerate chemo all shape the outcome. One study highlighted that patients who completed the full course of 60Gy had a 20percent improvement in local control compared with those who stopped early due to toxicity.
Let me share a quick snapshot: Jane, a 58yearold teacher, finished a 28fraction regimen last year. Two years later, her scans show no active disease, and shes back to reading to her grandchildren every night. Her story isnt a guarantee, but it shows that many folks beat the odds with the right blend of treatment and support.
Side Effects Overview
Radiation is a powerful tool, and like any tool, it can leave a mark. The shortterm side effectsoften called acute toxicitiesusually surface within the first few weeks. You might notice:
- Fatigue that feels like youve run a marathon in your mind.
- Sore throat or a burning sensation when you swallow.
- Heartburn or a mild ulceration in the lining of the esophagus.
- Mouth dryness and occasional taste changes.
Most of these symptoms peak around week three and gradually fade after treatment ends, especially with good supportive care. Nutritionists often recommend soft, bland foodsthink oatmeal, smoothies, or wellcooked veggiesplus plenty of hydration.
Longterm (or late) side effects are less common but worth keeping on your radar. They can include:
| Side Effect | Incidence | Management |
|---|---|---|
| Chronic esophagitis | 1015% | Swallowing therapy, topical steroids |
| Stricture formation | 510% | Endoscopic dilations, stents |
| Fibrosis of lung/heart | <5% | Cardiopulmonary monitoring |
| Secondary malignancy | Very low | Longterm surveillance |
If a stricturea narrowing of the tubedevelops, most gastroenterologists can gently stretch it using a dilator or place a temporary stent. Its a manageable step, not a roadblock.
Treatment Schedule
Most curative regimens follow a fivesessionsperweek patternMonday through Friday. For a total dose of 60Gy, thats 30 visits over six weeks. Each session lasts about 1520 minutes, but you should factor in setup time for positioning and imaging, which can add another 1015 minutes.
When the goal shifts to palliative care, the schedule condenses. A common protocol is 30Gy over ten fractionsjust two weeks of visits. The aim here isnt cure; its relief from painful swallowing, bleeding, or choking. According to the , these shorter courses have solid evidence for improving quality of life without the exhaustive commitment of a fullcurative plan.
What influences the number of sessions? A few things:
- Intent (curative vs. palliative).
- How big the tumor is.
- Your overall stamina and any concurrent chemotherapy.
- Sideeffect toleranceif inflammation becomes severe, the team might pause or adjust the dose.
Ask your radiation oncologist for a written schedule. Seeing the dates on paper can turn an abstract timeline into a concrete plan you can prepare for.
Palliative Radiotherapy
When a tumor has spread or surgery isnt an option, palliative external beam radiation steps in like a compassionate friend offering a steady hand. The primary goals are:
- Alleviate dysphagia (difficulty swallowing).
- Stop or reduce bleeding.
- Improve overall comfort.
A typical palliative dose is 30Gy in ten fractions. For some patients, even a brief 20Gy in five fractions can make a big difference. One veteran named Mark, 72, shared that after a twoweek course, he could finally sip thin liquids without coughinga small victory that meant his evenings could include his favorite soup again.
Remember, palliative care isnt giving up. Its an intentional shift to prioritize comfort and daily joys while still harnessing the tumorshrinking power of radiation.
Radiation Damage & Care
Radiation can damage the cells lining the esophagusthink of it as a sunburn on the inside. The process starts with DNA damage, which triggers inflammation, ulceration, and, in some cases, scar tissue (fibrosis). Diagnosis usually involves an endoscopy, a barium swallow, or simply tracking symptoms using a standardized scoring system like CTCAE.
How do we treat that damage?
- Topical steroids swallowed as a liquid can calm inflammationsmall randomized trials show faster healing.
- Protonbeam therapy is an emerging option that reduces dose to nearby heart and lungs, potentially lowering the risk of collateral damage.
- Endoscopic dilation stretches strictures, often paired with a short course of steroids to prevent renarrowing.
- Stent placement offers immediate relief if the tube is severely blocked, especially in a palliative setting.
Every step of care should be a partnership. Talk openly with your radiation oncologist about any new pain, difficulty swallowing, or persistent heartburnyou deserve prompt attention to keep side effects from snowballing.
Quick Answers
Lets cut to the chase with the most common concerns that pop up in a clinics waiting room:
What is external beam radiation for the esophagus? Its a noninvasive therapy that delivers highenergy rays from a machine outside your body straight to the tumor.
How long does a typical course last? About 56weeks for curative intent (five sessions each week) and 12weeks for palliative intent.
Will I need chemotherapy as well? Often, yescombining chemo with EBRT improves cure rates, but your doctor will weigh the benefits against your overall health.
Can I eat normally during treatment? Soft, bland foods are safest. Many patients find smoothies and pureed meals help maintain nutrition while the throat heals.
What are the most common side effects? Fatigue, sore throat, heartburn, and occasional difficulty swallowing. Most settle after treatment, and there are proven ways to manage them.
Is radiation curative? For earlystage disease, it can be. For advanced disease, it often aims to control the tumor and extend life, sometimes alongside surgery.
What if my cancer is advanced? Palliative EBRT can still relieve symptoms, improve swallowing, and give you back quality time with loved ones.
How does treatment affect other cancers or conditions? If you have a history of cancers like prostate cancer, or concerns about interactions with hormonal therapies, mention this to your team. For example, patients researching prostate options may find resources on prostate cancer outlook helpful when discussing longterm expectations across different cancer types.
Building Trust with Your Care Team
Knowledge feels empowering, but the real magic happens when you pair it with a trustworthy team. Heres a quick checklist to make sure youre in good hands:
- Confirm that your radiation oncologist is boardcertified.
- Make sure the treatment center is accredited by the American College of Radiology (or an equivalent body).
- Ask for a copy of the treatment planseeing the dose distribution can demystify the process.
- Dont hesitate to request a second opinion if anything feels unclear.
- Ask about support services: dietitians, speechlanguage pathologists, and psychosocial counselors.
Transparency builds confidence. If a clinic can walk you through each step, show you the imaging, and answer every whatif question, youre more likely to feel in control of your journey.
Helpful Resources
When youre ready to dive deeper, trustworthy sources can fill in the details:
- clear explanations of radiation techniques.
- uptodate stats on survival and sideeffects.
- the gold standard for treatment protocols.
Conclusion
External beam radiation for the esophagus is a cornerstone of modern cancer careoffering hope, control, and, in many cases, a return to everyday pleasures like enjoying a warm cup of tea. Yes, the treatment comes with challenges: a schedule of visits, shortterm discomfort, and the possibility of late effects. Yet, armed with clear information, a supportive team, and practical tips for managing side effects, you can navigate the journey with confidence.
Remember, youre not alone. Whether youre asking questions at your next appointment, reaching out to a dietitian, or simply sharing a laugh with a friend whos been through it, every step you take builds a stronger foundation for recovery and quality of life. Whats your biggest concern about radiation therapy right now? Feel free to share in the comments, and lets keep the conversation goingtogether were stronger.
FAQs
How long does a typical curative external beam radiation course last for the esophagus?
Curative EBRT usually involves 5‑6 weeks of treatment, with one session per weekday (total ≈ 25‑30 fractions).
What are the most common acute side effects of external beam radiation to the esophagus?
Patients often experience fatigue, sore throat, heartburn, and temporary difficulty swallowing, which peak around week 3 and improve after treatment.
Is chemotherapy always required with external beam radiation for esophageal cancer?
While not mandatory for every case, combining chemotherapy with EBRT significantly improves local control and overall survival for many patients.
Can palliative external beam radiation relieve swallowing problems?
Yes—short courses such as 30 Gy in 10 fractions can markedly reduce dysphagia and improve quality of life, even when cure isn’t possible.
How are strictures caused by radiation treated?
Endoscopic dilation or temporary stent placement, often paired with topical steroids, are effective ways to manage radiation‑induced esophageal strictures.