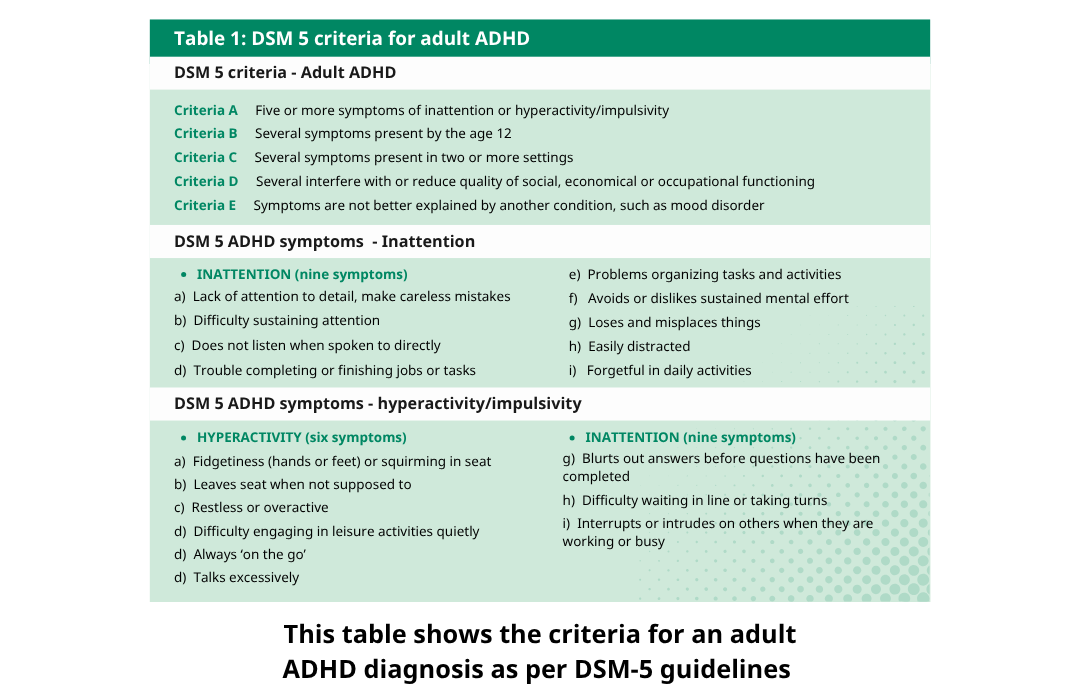
Short answer: most major health plansincluding Blue Cross Blue Shield, UnitedHealthcare, and Cignawill cover an ADHD assessment when its deemed medically necessary and ordered by a qualified provider. If you stay innetwork and have the proper referral, you could pay little to nothing outofpocket. If youre unsure about the details, keep reading; Ill walk you through exactly how it works, what costs you might see, and how to make the process as smooth as possible.
Quick Answer Overview
Think of insurance coverage like a road map. The destination (an ADHD diagnosis) is clear, but you need the right turnbyturn directionsreferrals, preauthorizations, and the correct billing codesto stay on the paved road and avoid costly detours. In most cases, the road is paved: youll get coverage for a full diagnostic evaluation if you have a doctors order and the test is ordered within the plans network.
How Insurance Works
Medical Necessity & Diagnosis Codes
Insurers rely on two key pieces of information:
- Medical necessity: Your provider must document why an ADHD assessment is requiredusually because symptoms interfere with daily life, school, or work.
- ICD10CM codes: The most common ones are
F90.0(ADHD, combined presentation) andF90.1(predominantly inattentive). These codes tell the insurer that the test isnt just a nicetohave but a necessary medical service.
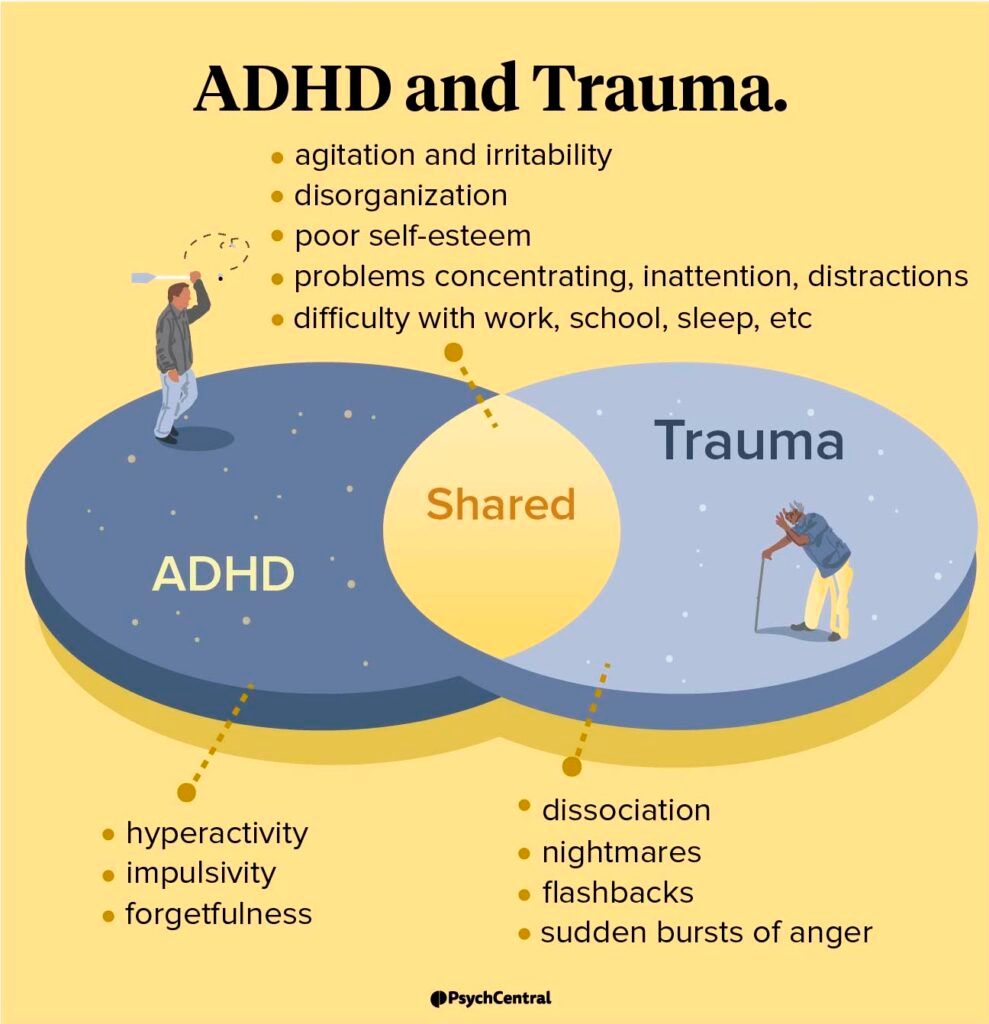
Once those pieces are in place, most plans will move forward with coverageespecially if you have a preauthorization letter from your doctor. If you suspect past trauma may be contributing to symptoms, consider discussing the ADHD and trauma connection with your clinician so documentation reflects all relevant factors.
Tests That Are Usually Covered
| Test Type | Who Performs It? | Typical CPT Code | Covered By Most Plans? |
|---|---|---|---|
| Full neuropsychological evaluation | Psychologist / Neuropsychologist | 96118, 96119 | |
| Brief screening questionnaire | Primary care or pediatrician | 96127 | (often) |
| Followup monitoring | Same provider | 96136 | (if documented) |
These CPT codes are the language insurers use to understand what service youre receiving. When you see a in the table, thats a green light for most private and public plans.
When Tests Might Not Be Covered
Insurance isnt a magic wand. Here are common roadblocks:
- Screeningonly questionnaires without a formal DSM5 evaluation.
- Tests ordered by providers who arent licensed to diagnose ADHD (e.g., some life coaches).
- Duplicate testing within a short windowmost plans view this as unnecessary and will deny the second claim.
Major Insurers Reviewed
Blue Cross Blue Shield
BCBS generally covers ADHD assessments when a physician writes a referral and the test is classified as medically necessary. If youre wondering does blue cross blue shield cover adhd testing? the answer is usually yesespecially for innetwork psychologists. Outofnetwork services are often reimbursed at about 70% of the providers fee, but youll need to submit a claim yourself.
UnitedHealthcare
UnitedHealthcare typically covers both innetwork and outofnetwork evaluations, though outofnetwork comes with a higher coinsurance. A preauthorization is recommended to avoid surprises, and many members report seeing a $10$40 copay for a full assessment when they stay innetwork.
Cigna
Cigna explicitly lists ADHD diagnostic services under its mentalhealth benefits. A recent confirms that a qualified professionals evaluation is covered when the claim includes the proper ICD10 code and a physicians referral.
Medicaid & Medicare
Statebystate differences matter. Most Medicaid programs treat ADHD as a mentalhealth condition, so evaluations are covered as long as the provider is enrolled in the states Medicaid network. Medicare Part B also covers diagnostic assessments when ordered by a qualified provider, though the process can be more paperworkheavy.
Quick Comparison Table
| Insurer | InNetwork Coverage | OutofNetwork Coverage | PreAuth Needed? | Typical Patient Cost* |
|---|---|---|---|---|
| BCBS | Full | 70% of fee | Yes | $0$30 copay |
| UnitedHealthcare | Full | 80% of fee | Yes | $10$40 copay |
| Cigna | Full | 75% of fee | Yes | $0$25 copay |
| Medicaid | Full (varies) | Not applicable | Usually No | $0 |
*Costs are based on a typical $30$40 deductible plan; always verify your own policy.
Testing Costs Explained
Typical OutofPocket Prices With Insurance
If everything lines up, you might see a $0$150 billa modest copay or coinsurance. The exact amount depends on your plans deductible, coinsurance rate, and whether the provider is innetwork.
Cost Without Insurance
When youre paying outofpocket, a full neuropsychological evaluation can range from $300 to $1,200. The price hinges on the providers hourly rate, the number of testing hours, and any additional feedback sessions.
Breakdown of Fees (per hour)
| Service | Avg. Hourly Rate | Total Hours | Approx. Cost |
|---|---|---|---|
| Intake & History | $150$200 | 1 | $150$200 |
| Cognitive Testing | $200$250 | 23 | $400$750 |
| Feedback Session | $150$200 | 1 | $150$200 |
| Full Package | 45 | $700$1,150 |
These figures give you a realistic sense of what how much does adhd testing cost for adults really looks like when youre not covered by insurance.
Maximizing Your Coverage
StepbyStep Checklist
- Verify your benefits: Call the member services line and ask specifically about ADHD diagnostic evaluation. Write down the answer.
- Get a referral: Most plansBCBS, UnitedHealthcare, Cignarequire a primarycare or pediatrician referral before theyll approve the test.
- Request preauthorization: Your provider should submit the ICD10 code (F90.0 or F90.1) along with a brief note on medical necessity.
- Choose an innetwork provider: This can save you 2030% compared with outofnetwork services.
- Ask about outofnetwork reimbursement: If you have a trusted specialist whos out of network, see whether the plan will reimburse a portion after you submit the claim.
If Your Claim Is Denied
Denial doesnt have to be the end of the road. Heres a quick rescue plan:
- Read the denial codecommon ones include Medical Necessity Not Established.
- Gather supporting documents: clinical notes, school or work reports, and a copy of the DSM5 criteria you meet.
- Draft an appeal letter. that you can customize.
- Submit the appeal within the timeframe the insurer specifies (usually 3060 days).
Many people get a reversal when they provide clear, documented evidence of need. Its worth the effort. If background factors like childhood stressors are relevant, include a clear history and consider referencing resources on childhood trauma ADHD when explaining medical necessity.
Bottom Line Summary
In short, if you have a reputable plan like Blue Cross Blue Shield, UnitedHealthcare, or Cigna, and you follow the steps abovereferral, preauthorization, and innetwork provideryour ADHD testing will most likely be covered. The biggest hurdles are paperwork and making sure the insurer sees your assessment as medically necessary. When those boxes are checked, you can focus on what matters: getting a proper diagnosis and the support you need.
Feel a little more confident about navigating insurance? Great! Grab the downloadable Insurance Coverage Checklist (you can create one from the steps above) and keep it handy the next time you call your provider. If youve already gone through the processwhether it was smooth sailing or a bumpy rideshare your experience with a friend who might be in the same boat. Were all learning together, and a little shared knowledge can make a huge difference.
FAQs
Does my insurance automatically cover ADHD testing?
No, coverage is not automatic. Most insurance plans cover ADHD testing when it's deemed medically necessary, but you must have a referral from a qualified provider, proper diagnosis coding, and preauthorization. Coverage also depends on your specific plan type and whether you use in-network providers.
What's the difference between in-network and out-of-network ADHD testing coverage?
In-network providers have negotiated rates with your insurance, typically resulting in full coverage or minimal copays. Out-of-network providers are reimbursed at a lower percentage (typically 70-80% of fees), and you may need to submit claims yourself for reimbursement. Out-of-network services usually require higher out-of-pocket costs.
Do I need a referral for ADHD testing to be covered?
Most insurance plans require a referral from your primary care physician or pediatrician before approving ADHD testing. Some plans may also require preauthorization. Check your specific plan requirements by contacting your insurance provider directly.
What if my insurance denies coverage for ADHD testing?
You have the right to appeal the denial. Gather supporting documentation including clinical notes, work or school performance reports, and information showing how ADHD symptoms affect your daily life. Submit an appeal letter with this evidence within the timeframe your insurer specifies, typically 30-60 days. Many appeals are successful with proper documentation.
How much will I pay out-of-pocket for ADHD testing with insurance?
With insurance coverage, you typically pay $0-$150, depending on your plan's copay, coinsurance, and deductible. With preauthorization and an in-network provider, many people pay only a standard copay ($10-$40). Without insurance, full evaluations range from $300-$1,200.
Are online ADHD assessments covered by insurance?
Insurance coverage for online assessments depends on your plan and provider. Many insurers now cover telehealth evaluations similarly to in-person services, but you should confirm with your insurer beforehand. Note that self-assessment tools available online cannot provide a medical diagnosis.
Do Medicaid and Medicare cover ADHD testing?
Most Medicaid programs cover ADHD evaluation as a mental health service when the provider is enrolled in the state's network, though coverage varies by state. Medicare Part B covers diagnostic assessments ordered by qualified providers. Contact your state's Medicaid office or Medicare representative to confirm your specific coverage.
What testing codes do insurers use for ADHD assessments?
Common CPT codes for ADHD testing include 96118 and 96119 for full neuropsychological evaluations, 96127 for brief screening questionnaires, and 96136 for follow-up monitoring. Your provider uses these codes to bill your insurance. ICD-10 diagnosis codes F90.0 and F90.1 indicate ADHD for billing purposes.