Why Accuracy Matters
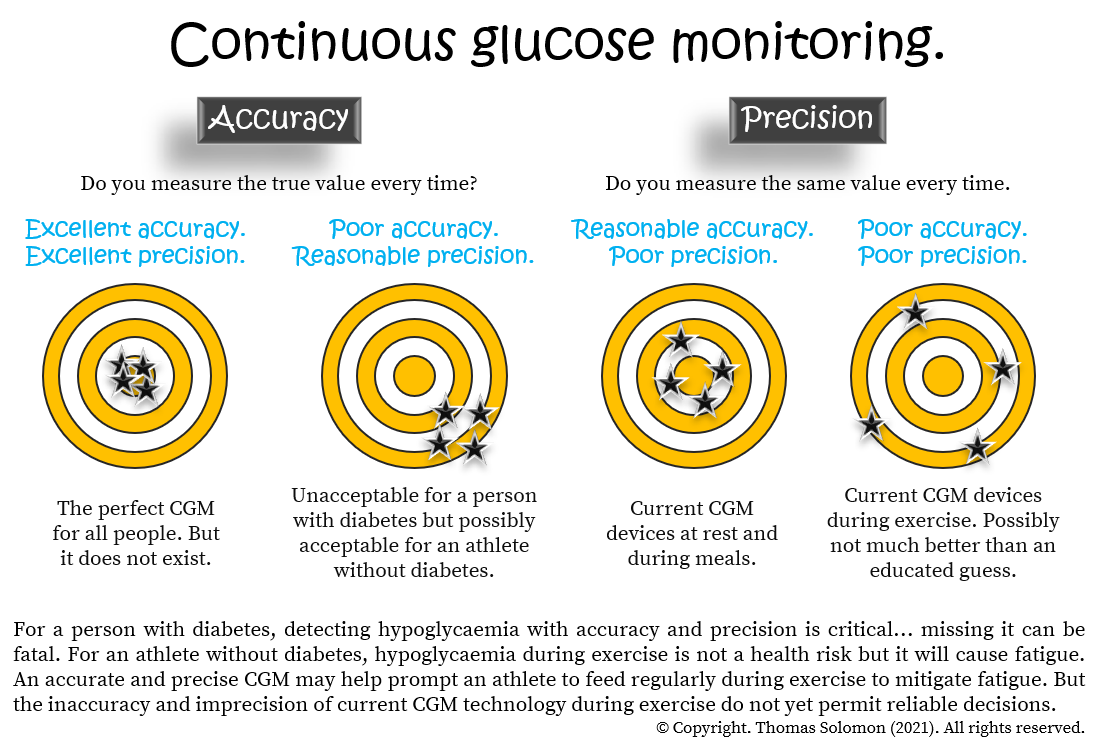
Think of CGM accuracy like the reliability of a trusted friend. When your friend says, Ill pick you up at 5p.m., you plan your day around that promise. If theyre consistently late, you start doublechecking the time. The same goes for glucose data: inaccurate numbers can lead to missed hypo warnings, overcorrections, or unnecessary anxiety.
Balancing the benefits and risks of CGM accuracy isnt about fearing the technologyits about empowering yourself to interpret the data wisely. Whether youre managing type1 diabetes, tracking trends for fitness, or just curious about your bodys sugar dance, knowing the reliability of your sensor helps you trust the numbers and act confidently.
How CGMs Are Tested
Manufacturers dont just guess how accurate their devices are; they run rigorous lab and realworld studies. The gold standard metric is MARDMean Absolute Relative Difference. In plain English, MARD tells you the average percentage offby between the CGM reading and a laboratory reference glucose measurement.
For example, a CGM with a 9% MARD typically means its readings are within 9% of the true value on average. Thats why youll often see claims like Dexcom G7: 9% MARD or FreeStyle Libre2: 9.5% MARD., devices that consistently stay below 10% MARD are considered very reliable for daytoday use.
What is MARD and why does it matter?
MARD condenses thousands of data points into a single, easytounderstand figure. A lower MARD generally means tighter alignment with the gold standard lab measurement, which translates to fewer surprises when your glucose actually changes.
Which clinical trials report the highest accuracy?
Recent trials published in Diabetes Care and the Journal of Diabetes Science and Technology highlight that the latest Dexcom G7 and Abbotts Libre2 consistently achieve sub10% MARD in diverse populations, from children to older adults.
CGM vs FingerStick
Many people still reach for a fingerstick (FS) when they doubt a CGM reading. Thats naturalFS is the old guard. But how do they truly compare?
How accurate is CGM compared to fingersticks?
Fingersticks, when done correctly, have a typical analytical error of about 510mg/dL (0.3mmol/L). CGMs, on the other hand, report a broader 1220% range, depending on sensor age and conditions. In practice, this means a CGM might read 5.5mmol/L when the true value is 5.0mmol/La difference many clinicians deem acceptable for trend monitoring.
When do fingersticks still beat CGM?
If youre in a highrisk scenariolike an overnight hypoglycemia episode, rapid glucose swings during intense exercise, or when the sensor displays errora confirmatory FS is the safest move. In realworld settings, users often backup CGM alerts with a quick FS just to be sure.
DeviceSpecific Accuracy
Not all CGMs are created equal. Lets peek under the hood of the three most talkedabout systems: Dexcom, FreeStyle Libre, and Lingo.
Dexcom CGM accuracy latest numbers?
Dexcoms G7 reports a MARD of 9% across its sensor life, making it one of the most precise devices on the market today.
How accurate is FreeStyle Libre CGM?
Libre2 and Libre3 hover around 9.5% MARD. While slightly higher than Dexcom, theyre praised for ease of use and affordable sensor cost.
Is Lingo CGM the most accurate on the market?
Lingo, a newer entrant, claims a 7% MARD in its initial studiespotentially the lowest reported. However, realworld data is still emerging, and longterm reliability remains under observation.
Comparison Table MARD & % OutofRange
| Device | MARD (Mean) | Typical % OutofRange (20%) | Sensor Life |
|---|---|---|---|
| Dexcom G7 | 9% | 5% | 10 days |
| FreeStyle Libre2 | 9.5% | 6% | 14 days |
| Lingo | 7% (study) | 3% | 12 days |
These numbers give you a snapshot, but rememberrealworld performance can shift with placement, temperature, and personal physiology.
Factors Skewing Readings
Even the best sensor can falter if conditions arent optimal. Below are the usual suspects that can throw your CGM offtrack.
How does sensor placement affect accuracy?
Most manufacturers recommend the abdomen or upper arm. Placing the sensor on a bony area or an area with a lot of scar tissue can cause compression lag, where the sensor reads lower glucose during rapid spikes.
Do medications or hydration change sensor glucose?
Certain drugslike acetaminophen or high doses of vitaminCcan interfere with the enzyme chemistry inside the sensor, leading to brief spikes or dips. Dehydration, on the other hand, can concentrate interstitial fluid and make readings appear higher.
Whats the impact of compressioninduced lag?
Think of it as a traffic jam for glucose molecules. When you tighten a watch band too much, the sensor can register lower glucose because blood flow is restricted. Loosening the band often restores normal readings within a few minutes.
Reading the Data
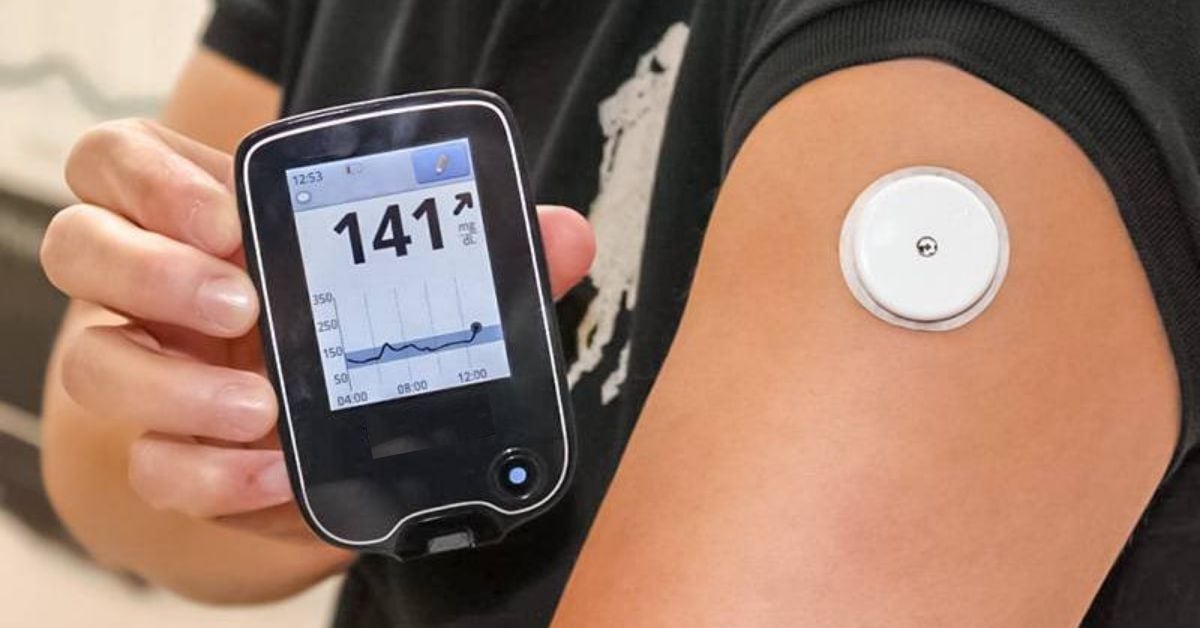
Seeing a number like 6.2mmol/L on your phone can feel abstract. Lets translate that into something more tangible.
If my real glucose is 5mmol/L, what range might the CGM show?
With a 20% margin, a true value of 5mmol/L could appear anywhere between 4.0 and 6.0mmol/L on the CGM. Thats why trend arrowsshowing the direction and speed of changeare essential for context.
How to use trend arrows to compensate for lag?
If the arrow points upward rapidly, even a normal reading might be climbing toward a high. Conversely, a downward arrow during a known lowrisk period (like overnight) can signal a looming hypoglycemia, prompting a quick FS confirm.
For people also monitoring dietary impacts closely, noting how specific foods change interstitial glucose can help interpret shortterm deviations; for example, research and guides on strawberries blood sugar show how certain lowglycemic foods may produce milder postmeal rises, useful context when you see modest spikes on your CGM. strawberries blood sugar
Is CGM Worth It?
Now the big question many of us ask: Is a CGM worth the cost and effort, especially if Im not diagnosed with diabetes?
Can a CGM help detect prediabetes early?
Yes. Continuous data can reveal subtle patternslike prolonged periods of postmeal spikesthat routine fingersticks might miss. Spotting these trends early can spark lifestyle changes before a fullblown diagnosis.
What are the costbenefit considerations?
In the U.S., sensor packages range from $300 to $400 per month. Insurance often covers a portion for diabetics, but for healthconscious individuals the outofpocket cost can be steep. Weigh the expense against potential benefits: reduced clinic visits, better glucose control, and peace of mind.
Boost Your Accuracy
Even if youre already using a toptier device, a few tweaks can sharpen those numbers.
Best sensor insertion sites and adhesion tricks
Follow the manufacturers site guideusually the abdomen for Dexcom and the upper arm for Libre. Clean the skin with alcohol, let it dry, and apply a siliconebased adhesive patch if you tend to sweat a lot.
Calibration frequency too much or too little?
Dexcom G7 uses factorycalibrated sensors, meaning no routine calibrations. Libre devices also dont require users to calibrate. If youre using an older model that asks for calibration, stick to the recommended scheduletypically twice dailyto avoid drift.
When to trust the CGM vs. confirming with a fingerstick
Trust the CGM for trends and daytoday decisions. Reach for a FS when you see a rapid change, an alert at an unusual time, or before making a big decision (e.g., insulin dosing for a newborn). This balanced approach keeps you safe without overchecking.
What Experts Say
Endocrinologists and diabetes educators emphasize that CGM accuracy is a moving target, improving each generation.
Key findings from recent reviews
A systematic review in Diabetes Technology & Therapeutics found that newer CGMs (G7, Libre3) consistently achieve sub10% MARD and show lower rates of data gaps compared to older models., this translates to higher confidence in both clinical and personal settings.
Realworld accuracy data from inpatient studies
Hospitals that integrated CGM data into insulin dosing protocols reported a 15% reduction in hypoglycemic events, underscoring the practical safety gains when accuracy is high.
Safety and regulatory statements
The FDA classifies CGMs as ClassII medical devices, requiring manufacturers to demonstrate safety and performance in welldesigned trials. EMA (European Medicines Agency) follows similar scrutiny, ensuring that the claims you see on packaging are backed by rigorous testing.
Conclusion
Understanding CGM accuracy isnt just a technical deepdive; its about gaining confidence in the numbers that guide your health decisions. By knowing what MARD means, comparing devices, spotting factors that can skew data, and applying practical tips, you can turn a sleek sensor into a trustworthy ally. Whether youre managing diabetes, curious about your metabolism, or simply want a clearer picture of your glucose trends, an accurate CGM can be a gamechangerprovided you use it wisely.
Whats your experience with CGM accuracy? Have you found a placement trick that works wonders, or a device that feels just right? Share your story in the comments, and lets keep the conversation rolling. If you have questions, dont hesitate to askI\'m here to help!
FAQs
What does MARD tell me about CGM accuracy?
MARD (Mean Absolute Relative Difference) shows the average percentage difference between CGM readings and laboratory‑grade glucose measurements; a lower MARD means the sensor’s numbers stay closer to the true value.
How does CGM accuracy compare to finger‑stick testing?
Finger‑sticks generally have a ±5–10 mg/dL analytical error, while CGMs usually show a ±12–20 % range. CGMs are great for trends, but a quick finger‑stick is advisable for rapid changes or critical decisions.
Which CGM currently has the lowest reported MARD?
Early studies suggest Lingo’s CGM may achieve around 7 % MARD, slightly better than Dexcom G7 (≈9 %) and FreeStyle Libre (≈9.5 %). Real‑world data is still being gathered.
Can sensor placement affect CGM accuracy?
Yes. Placing the sensor on recommended sites (abdomen for Dexcom, upper arm for Libre) and avoiding tight bands or scarred skin helps minimize compression lag and improves reading reliability.
When should I confirm a CGM reading with a finger‑stick?
Confirm with a finger‑stick if you receive an alert during rapid glucose swings, notice an “error” message, experience symptoms that don’t match the CGM, or before making important dosing decisions.