If youve ever wondered whether a cervical cancer scan is something you really need, the quick answer is: its a set of safe, doctorguided tests that can spot abnormal cells long before cancer ever shows up. You dont have to wait for scary symptomsregular screening, done at the right age, is the smartest way to protect yourself. Below, Im breaking down exactly what a cervical cancer scan involves, the pros and cons, and how to get ready so you feel confident and in control.
What is a scan
How does a cervical cancer scan work?
In everyday language, cervical cancer scan is really a catchall for a few different tests that look at the cells of the cervix. The most common combo is a Pap test (or Pap smear) plus an HPV DNA test. The Pap test scrapes a small sample of cells from the cervix and sends it to a lab, while the HPV test looks for the highrisk strains of human papillomavirus that cause most cervical cancers.
Screening vs. diagnostic
Think of screening as a safety net. Its meant for healthy people to catch problems early. If something unusual shows up, a diagnostic procedurelike a colposcopy or a cone biopsywill dive deeper. The terminology can feel confusing, but the key is: screening is preventive; diagnosis is confirmatory.
Who should get scanned and when?
Guidelines vary a bit by country, but most health agencies agree on the same agebased schedule:
- 2129 years: Pap test every 3years.
- 3065 years: Either Pap test every 3years or a cotest (Pap+HPV) every 5years.
- Over 65: You can often stop if youve had several consecutive normal results.
This schedule comes from the and the . If youre unsure where you fit, a quick chat with your primary care provider will clear things up.
Screening methods
Pap test (Pap smear)
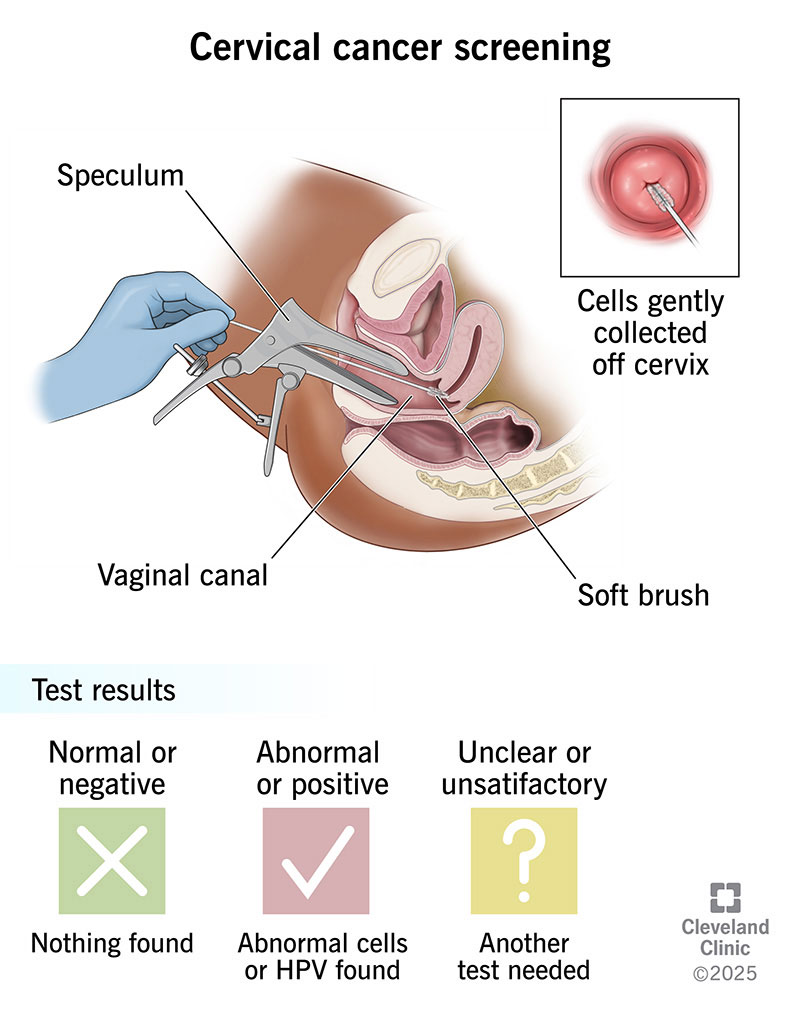
The Pap test is the classic cervical cancer scan youve probably heard about. During the exam, the doctor (or nurse) places a speculum to open the vagina, then gently brushes the surface of the cervix to collect cells. The whole thing usually takes under five minutes, and most women describe it as slightly uncomfortable rather than painful.
HPV DNA test
Highrisk HPV typesespecially 16 and 18cause about 70% of cervical cancers. The HPV DNA test looks for the genetic material of these viruses. When done together with a Pap test (the cotest), it dramatically improves the chance of catching dangerous changes early. According to , the cotests sensitivity is over 95% for detecting highgrade lesions.
Colposcopy
If your Pap or HPV results are abnormal, your clinician may recommend a colposcopy. This isnt a scan in the imaging sense; its a magnified visual exam of the cervix using a specialized microscope (the colposcope). The doctor may apply a mild solution to highlight abnormal areas and take tiny biopsies if needed. Its the next step toward a definitive diagnosis.
Cone biopsy (LEEP)
When a biopsy shows something suspicious, a cone of tissue might be removed using a loop electrosurgical excision procedure (LEEP). The sample is then examined under a microscope. While the thought of a cone can sound scary, the procedure is quick, done under local anesthesia, and has a high cure rate for early cancers.
Blood tests & emerging markers
Right now, theres no FDAapproved blood test that can replace the Pap or HPV tests. Researchers are exploring bloodbased biomarkers, but for now, the phrase blood test for cervical cancer is more of a future promise than a present reality. If you see claims about a simple blood draw that can detect cervical cancer, treat them with caution.
Home detection myths
Can I selfscreen?
Many people ask, how to detect cervical cancer at home? Unfortunately, a true screening cant be done reliably on your own. Some countries now approve selfsampling kits for HPV, which let you collect a vaginal swab and mail it to a lab. Those kits are useful for people who cant easily access a clinic, but they still need professional followup if the result is positive.
Early symptoms that matter
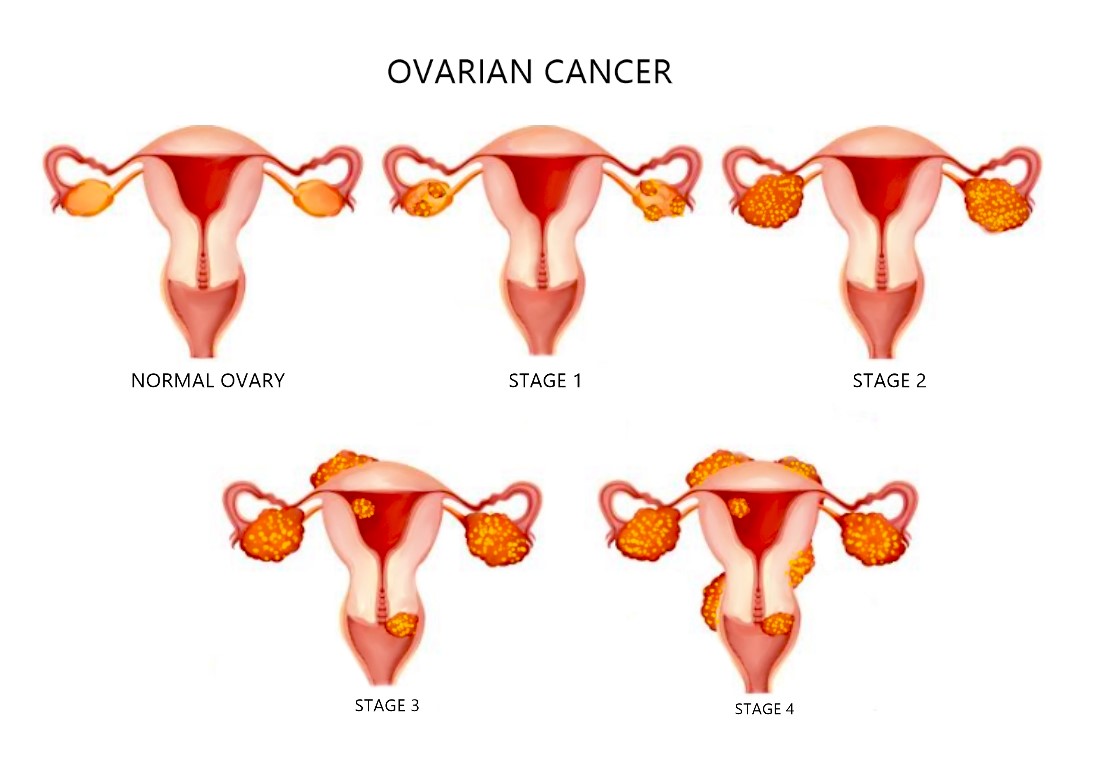
Its tempting to think that spotting or pelvic pain will always sound the alarm, but early cervical cancer (stage1) often has no symptoms at all. When symptoms do appear, they might include:
- Unusual vaginal bleeding (after sex, between periods, or after menopause).
- Persistent pelvic pain.
- Abnormal discharge (watery, bloody, or foulsmelling).
One reader once told me, I thought my light spotting was just hormonal, and only after a year of worrying did I finally get a Pap test. I wish Id known the silence of early disease. Stories like that underline why routine screening matters more than hunting for symptoms.
Benefits and risks
Why its worth it
When caught early, cervical cancer is one of the most treatable cancers5year survival rates soar above 90% for stage1 disease (see ). Regular scans give you peace of mind, reduce anxiety about the unknown, and empower you to act fast if something shows up.
Potential downsides
No medical test is completely riskfree. With cervical cancer scans you might experience:
- Shortterm discomfort from the speculum.
- Falsepositive results, which can lead to extra appointments and a bit of emotional rollercoaster.
- Rarely, infection after a biopsy.
Falsepositive rates for Pap tests alone hover around 510%, but they drop significantly when you add HPV testing (). Knowing these numbers helps you weigh the pros and cons without panic.
Balancing the decision
Ask yourself these quick questions before your appointment:
- Do I fit the agebased guidelines?
- Am I comfortable with the speculum, or should I discuss painrelief options?
- Do I have a trusted provider who will explain abnormal results calmly?
Most clinicians appreciate an open dialogueyoure not a passive patient, youre an active partner in your health.
Preparing for your scan
Dayofappointment checklist
Heres a simple timeline that many of my friends swear by:
- Morning: Avoid douching, tampons, or vaginal meds for 48hours.
- Before you go: Empty your bladderthis makes the speculum easier to insert.
- During the exam: Take slow, deep breaths; tell the provider if you feel any sharp pain.
- Afterward: You might see a little spotting for a day or two; thats normal.
Reducing discomfort
Relaxation tricks work wonders. Some women find that lying on their side with a pillow between the knees eases the speculum insertion. Others request a smaller speculum sizemost clinics have a range of options, so dont be shy about asking.
Understanding your results
Typical turnaround time is 714days. Results usually fall into one of several categories:
- ASCUS (Atypical Squamous Cells of Undetermined Significance) often just repeat testing.
- LSIL (LowGrade Squamous Intraepithelial Lesion) usually monitored, sometimes HPV reflex testing.
- HSIL (HighGrade Squamous Intraepithelial Lesion) may lead to colposcopy.
If you get an abnormal result, remember: its a signal to look closer, not a diagnosis of cancer.
Followup steps
After an abnormal finding, a colposcopy is the typical next move. Depending on biopsies, your provider might recommend:
- Repeat Pap/HPV in 612months.
- LEEP or cone biopsy to remove suspicious tissue.
- In rare cases, referral to a gynecologic oncologist for further treatment.
Women who face a cancer diagnosis may look into broader cancer care topics while planning treatment; for example, understanding early prostate cancer resources can illustrate how early detection shapes outcomes across cancer types.
Cost & insurance basics
Most insurance plans cover Pap and HPV testing as preventative servicesno copay needed under the Affordable Care Act. If youre on Medicaid or Medicare, youre still covered. For the uninsured, community health centers often offer lowcost or free screening. A quick call to your local health department can reveal options you didnt know existed.
Key takeaways
To sum it all up, a cervical cancer scan is a safe, evidencebased bundle of tests that can catch dangerous cell changes long before they turn into cancer. The agebased schedulestarting at 21ensures youre screened at just the right time. While a brief speculum insertion can feel odd, the benefits (early detection, higher cure rates) far outweigh the minor discomfort. If an abnormal result pops up, followup steps are clear and effective, and youll always have a healthcare professional guiding you through the next steps.
Now that youre armed with the facts, why not schedule that appointment youve been putting off? Its a simple act of selfcare that could save your life and give you peace of mind. Got a question, or want to share your own screening story? Drop a comment belowyoure not alone, and were all learning together.
FAQs
What age should I start getting a cervical cancer scan?
Screening typically begins at age 21, with a Pap test every three years until age 29.
How often do I need a Pap test and HPV test?
From age 30 to 65 you can have a Pap test every three years or a combined Pap + HPV test (co‑test) every five years.
Is a cervical cancer scan painful?
Most women describe the speculum insertion as uncomfortable but not painful; using a smaller speculum or relaxation techniques can help.
What do abnormal results mean?
An abnormal result signals that further evaluation (like colposcopy or biopsy) is needed; it does not mean you have cancer.
Can I do a cervical cancer scan at home?
Self‑sampling kits for HPV are available in some regions, but a full Pap test must be performed by a healthcare professional.