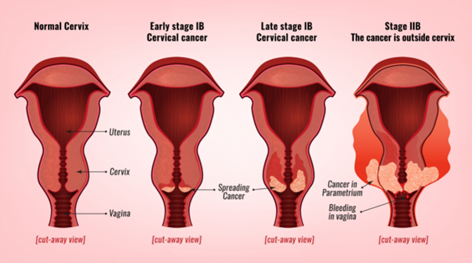
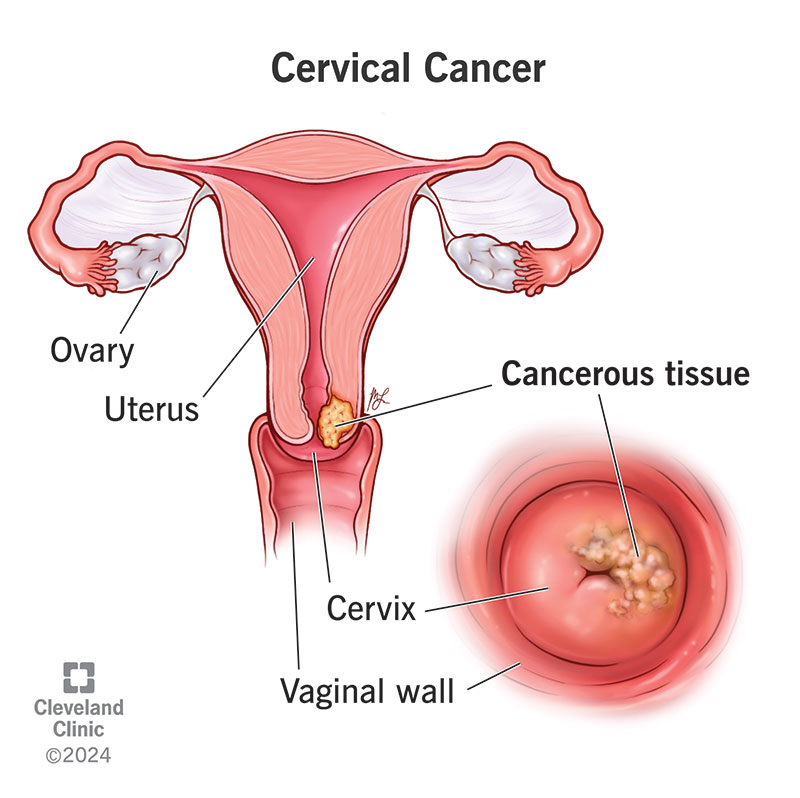
If you or a loved one is facing a hysterectomy because of cervical cancer, the short answer is reassuring:when the disease is caught early, most people survive five years or moreoften with a survival rate of9096%. The exact number depends on the cancer stage, your age, and the type of surgery you receive.
Understanding those numbers, what influences them, and what life looks like after the operation helps you ask the right questions, set realistic expectations, and feel more in control of the journey ahead. For patients worried about long-term outcomes after major cancer surgery, reading about prostate cancer outlook can also provide helpful perspective on survivorship, follow-up care, and lifestyle adjustments that apply across cancer types.
Quick Survival Summary
Overall 5Year Rates
Doctors usually talk about 5year overall survival because it provides a clear benchmark for longterm outcomes. Below is a snapshot of the most commonly cited figures, taken from a handful of peerreviewed studies and national cancer registries.
| Stage (FIGO) | 5Year Overall Survival* | Typical Survival After Hysterectomy |
|---|---|---|
| StageIAIB (early) | 95% | 9096% with radical or simple hysterectomy |
| StageIB3 | 8892% | High when surgery is complete |
| StageIIIII | 7080% | Drops with larger tumour burden |
| StageIV (advanced) | 3045% | Surgery+chemo/radiation can push it toward ~50% |
*Figures represent relative survival compared with a cancerfree population of the same age.
Why the Numbers Vary
Survival isnt just a static number. It reflects a mix of tumor biology, patient health, treatment quality, and followup care. Thats why youll see slightly different percentages in different sourcessome studies focus on only the most aggressive cancers, while others include a broader population.
Age and Survival
Cervical Cancer Survival Rate by Age
Age is a surprisingly strong predictor. Heres a quick breakdown based on data from Cancer Research UK and the National Cancer Institute:
| Age Group | 5Year Survival (Early Stage) | Key Factors |
|---|---|---|
| Under40 | 9698% | Fewer comorbidities, higher tolerance for aggressive surgery |
| 4060 | 9294% | Gradual rise in other health issues, but still good outcomes |
| Over60 | 8085% | Higher likelihood of heart disease, diabetes; slower healing |
What Makes Older Patients Face Lower Odds?
Older bodies often carry other health conditions that can complicate surgerythink heart disease, hypertension, or reduced kidney function. These comorbidities can increase surgical risk, delay recovery, and sometimes limit the use of aggressive adjuvant therapies.
Tips for Older Adults to Boost Outcomes
- Engage in a preoperative fitness programlight cardio, strength work, and breathing exercises can improve tolerance.
- Coordinate care among a multidisciplinary team (oncologist, cardiologist, nutritionist).
- Stay vigilant with postoperative followup: regular imaging, blood work, and pelvic exams.
Types of Hysterectomy
Simple vs. Radical Hysterectomy Which Is Right?
A simple hysterectomy removes only the uterus and cervix. Its generally reserved for very early cancers (stageIA). A radical hysterectomy goes furthertaking out part of the vagina, surrounding ligaments, and sometimes lymph nodes. This is the standard for stagesIBII.
Minimally Invasive vs. Open Surgery
In the early 2010s, many surgeons embraced laparoscopy and roboticassisted hysterectomy because of smaller scars and faster recovery. However, a landmark study in the found a slightly higher recurrence rate for minimally invasive radical hysterectomy in cervical cancer patients.
Today, most highvolume cancer centers prefer an open approach for stageIB2 or higher, while still offering minimally invasive options for very early disease when the surgeon is experienced.
When Hysterectomy Isnt Enough
For stageIIIV disease, surgery is often followed by chemotherapy, radiation, or both. This adjuvant therapy tackles microscopic disease that might have escaped the scalpel. Studies show that adding chemoradiation can improve 5year survival by 1015% in stageIII patients.
PostSurgery Outlook
Signs of Cervical Cancer After Hysterectomy
Even after a successful operation, its important to stay aware of warning signs. Call your doctor if you notice:
- New pelvic or lowerback pain that doesnt go away
- Unusual vaginal bleeding or spotting (sometimes from the cuff line)
- Foul discharge or a noticeable lump near the surgical site
Early detection of recurrence usually leads to better outcomes, so dont ignore subtle changes.
How Long Can You Live Without Treatment?
If a cervical cancer is left untreated, especially in stageIII orIV, the median survival is roughly 1218months. Earlystage disease might linger a bit longer, but cure rates without any therapy are extremely low. This underscores why timely treatment matters.
EndStage Cervical Cancer Life Expectancy
When the cancer has spread to distant organs (stageIV) and becomes endstage, life expectancy drops to 614months on average, depending on the extent of spread and whether palliative treatment is offered. Palliative care focuses on comfort, pain control, and maintaining quality of life.
Lifestyle Factors That Improve LongTerm Survival
Surviving the surgery is only part of the story. Your everyday choices can tip the odds in your favor:
- Nutrition: A diet rich in fruits, vegetables, lean protein, and whole grains supports healing.
- Smoking cessation: Quitting dramatically reduces the risk of recurrence and improves lung health.
- Regular followup: Keep every scheduled visit; imaging and Pap tests (if your doctor recommends) catch problems early.
- Physical activity: Light walking or yoga helps manage fatigue and keeps the immune system active.
Common Questions
What is the cervical cancer hysterectomy survival rate?
For earlystage (IAIB) disease, the 5year survival after a hysterectomy is about 95%. For stageIB3, its roughly 9092%. Survival drops to around 7080% for stageIIIII and 3045% for stageIV, even when combined with other therapies.
Can you survive cervical cancer without treatment?
Untreated advanced cervical cancer typically leads to death within a year. Earlystage cancers might survive a bit longer, but the chance of cure is virtually nil without surgery, radiation, or chemotherapy.
Does age change the survival odds?
Yespatients under 40 enjoy the highest survival (9698%). Those in their 60s see a dip to about 8085% for early disease, mainly due to other health conditions that affect treatment tolerance.
Is a minimally invasive hysterectomy safe for cancer?
Recent evidence suggests that for larger tumors (stageIB2+), an open approach may lower the risk of recurrence. Minimally invasive surgery remains a good option for very early cancers when performed by an experienced team.
RealWorld Cases
Case1 34YearOld, StageIA2, Robotic Radical Hysterectomy
Maria, a mother of two, opted for a robotassisted radical hysterectomy after a routine Pap test caught a small lesion. Pathology confirmed clear margins, and she completed a brief course of chemotherapy. Five years later, shes cancerfree, active, and back to running halfmarathons.
Case2 62YearOld, StageIB3, Open Radical Hysterectomy + Chemo
James was diagnosed after persistent pelvic pain. An open radical hysterectomy removed the tumor, and adjuvant chemo helped eradicate microscopic disease. At his threeyear followup, imaging shows no recurrence, and he reports a good quality of life despite mild neuropathy from chemo.
Case3 55YearOld, StageIV, Palliative Hysterectomy
Lenas cancer had spread to the lungs and liver. A palliative hysterectomy was performed to control severe vaginal bleeding. Combined with targeted therapy, she gained an additional 10months of relatively comfortable life, emphasizing that even in endstage disease, surgical intervention can improve symptom control.
Understanding Statistics
Relative vs. Absolute Survival
Relative survival compares cancer patients to the general population of the same age and sex. Absolute survival tells you the actual percentage of people still alive. Both are useful, but relative survival is often higher because it assumes the patient would have survived otherwise.
Why the 5Year Benchmark?
The fiveyear mark became a standard because most cancers that recur do so within that window. Surviving five years usually means the disease is well controlled, though longterm monitoring is still essential.
Limitations of Published Data
Study populations can be skewed toward patients treated at major cancer centers, which often have better outcomes than community hospitals. Geographic variations, socioeconomic factors, and genetic differences also affect survival.
Why the 5Year Benchmark?
The fiveyear mark became a standard because most cancers that recur do so within that window. Surviving five years usually means the disease is well controlled, though longterm monitoring is still essential.
Using the Numbers in Your Conversation
When you sit down with your oncologist, bring a short checklist:
- Ask about your specific stage and expected 5year survival.
- Inquire how your age and any other health issues might shift those odds.
- Discuss the pros and cons of simple vs. radical hysterectomy for you.
- Clarify the role of adjuvant therapy and its impact on overall survival.
Trusted Sources
All statistics and recommendations above are drawn from peerreviewed journals, national cancer registries, and reputable health organizations. For deeper dives, consult the following sources:
Conclusion
Bottom line: if cervical cancer is caught early, a hysterectomy offers a 9096% chance of surviving five years or more, and many patients live cancerfree for the rest of their lives. Age, cancer stage, and the type of surgery you undergo all shift those odds, which is why an honest, open dialogue with your care team is essential. Stay proactive, keep an eye on warning signs, and lean on trusted medical resources. If you have more questions or need guidance, reach out to a certified gynecologic oncologistyou deserve clear answers and compassionate care.
FAQs
What is the 5-year survival rate after hysterectomy for cervical cancer?
For early-stage cervical cancer (stages IA to IB1), the 5-year survival rate after hysterectomy is approximately 90-96%, depending on the surgery type and patient factors.
Does age affect survival rates after cervical cancer hysterectomy?
Yes, younger patients under 40 tend to have higher survival rates (96-98%), while those over 60 have lower rates (80-85%) due to additional health conditions.
Is minimally invasive hysterectomy safe for cervical cancer?
Minimally invasive hysterectomy is a safe option for very early-stage cervical cancer; however, open surgery is generally preferred for larger tumors due to lower recurrence risk.
What are the survival chances for advanced cervical cancer after surgery?
For advanced stages (III–IV), survival after hysterectomy combined with chemo/radiation ranges from about 30-50%, with adjuvant therapy improving outcomes.
Can cervical cancer be cured without treatment?
Untreated cervical cancer usually has very poor survival, especially in advanced stages, with median survival of 12-18 months without appropriate therapy.