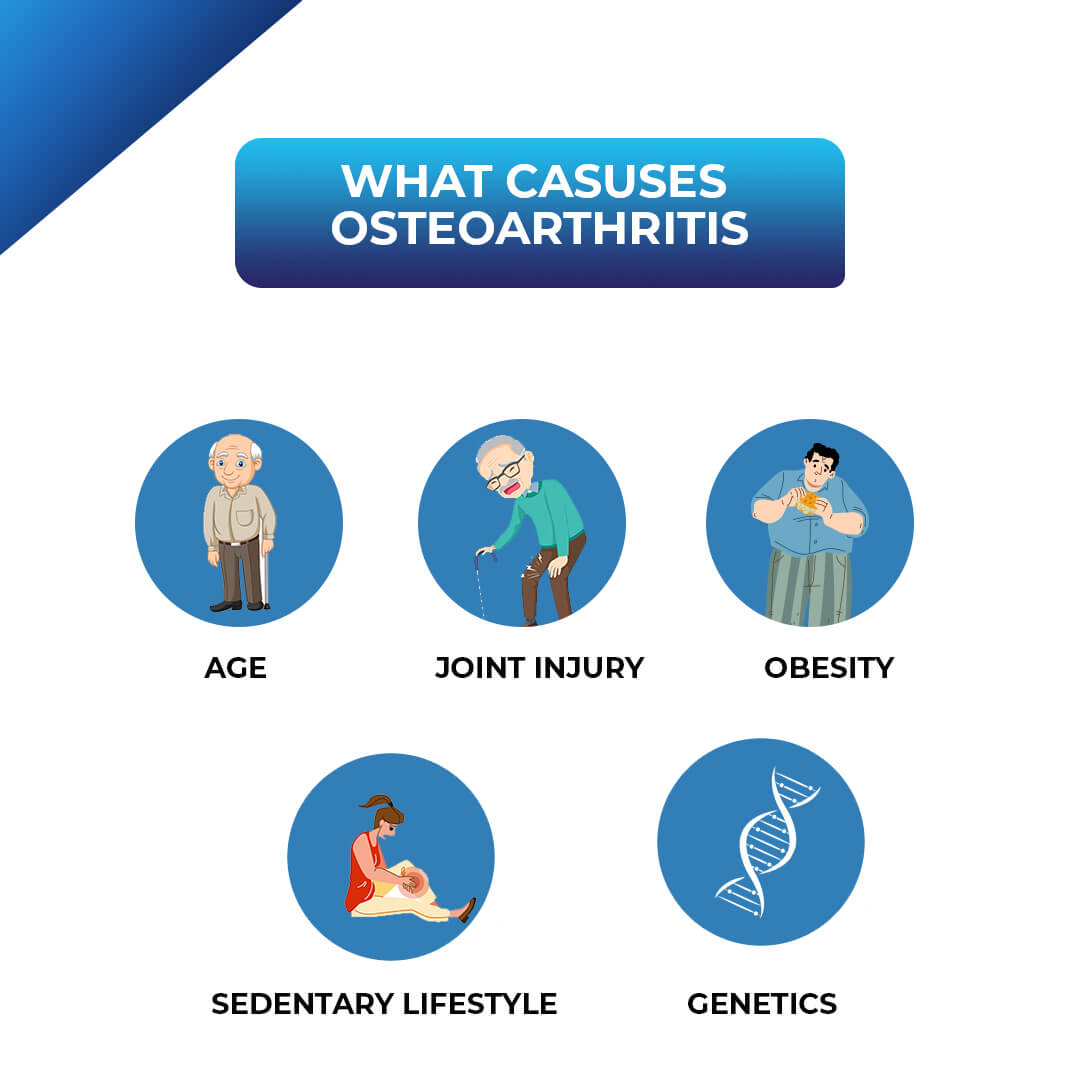
Osteoarthritis happens when the smooth cartilage that cushions your joints slowly wears away, letting bone rub on bone. The biggest triggers are age, extra weight, past injuries, and even the genes you inherited. Knowing causes of osteoarthritis lets you take controlwhether that means tweaking daily habits, catching problems early, or talking to a doctor about the best treatment. For people with inflammatory spine conditions, understanding how systemic inflammation affects joints can be especially important; resources on spine inflammation explain how inflammation elsewhere in the body may worsen joint wear.
Why Causes Matter
Ever wonder why two people of the same age can have completely different joint health? The answer lies in the mix of inevitable factors (like getting older) and the choices we make every day. Understanding both sides helps you spot red flags early and decide which lifestyle tweaks could slow the march of joint wear.
Primary Intrinsic Causes
Age and Natural Cartilage Degeneration
Think of cartilage like the rubber on a tire. Over time, the heat and pressure make it crack. After 55, the risk of osteoarthritis roughly doubles, according to the . Collagen production drops, synovial fluid thins, and the joint loses its shock-absorbing power.
Genetics and Family History
If your parents or grandparents had knee or hip replacements, you might be holding a genetic invitation to the same fate. Researchers have pinpointed genes like COL2A1 that affect the cartilage matrix. A quick chat with a genetic counselor can reveal whether you're at higher risk.
Hormonal Influence
Women notice a spike in osteoarthritis after menopause. Lower estrogen levels seem to reduce the protective cushion around joints, making women up to 1.5 times more likely to develop the condition than men of the same age.
Metabolic Factors
Conditions such as diabetes, gout, and metabolic syndrome create a low-grade inflammatory environment that can accelerate cartilage breakdown. Managing blood sugar and uric acid isn't just good for your heartit also shields your joints.
Lifestyle Extrinsic Causes
Obesity and Mechanical Overload
Every extra pound you carry adds about four pounds of pressure to each knee with every step. Imagine dragging a heavy backpack all dayeventually, the straps will stretch and tear. A study in The Lancet found that losing just 10% of body weight can cut knee-pain symptoms by nearly a third.
Real-World Example
John, a 48-year-old accountant, put on 30 lb over five years. He started feeling a grinding sensation in his knees during his morning walk. After a focused diet and weekly swimming sessions, he shed the weight and reported a noticeable drop in pain within three months.
Joint Injuries and Trauma
Ever twisted your ankle badly or suffered a sports injury? Those tearslike ACL ruptures or meniscus damagecan leave your joint vulnerable to osteoarthritis years later. The cartilage never fully recovers, setting the stage for premature wear.
Case Snapshot
Maria, a former college soccer player, tore her ACL at 23. Even after surgery, she developed knee osteoarthritis in her early 30s, illustrating how early trauma can snowball.
Repetitive Overuse
Jobs that involve constant bending, lifting, or kneelingthink construction, farming, or even long-hour desk work without proper ergonomicscreate microinjuries that add up. Over time, those tiny stresses become big problems.
Biomechanics and Alignment Issues
Flat feet, uneven leg length, or a pronounced knee valgus (knock-knee) shift the load to one side of the joint. Over years, the overloaded side wears faster, often showing up as unilateral pain.
Inflammatory Conditions
Rheumatoid arthritis and other inflammatory diseases can evolve into secondary osteoarthritis. While the initial damage comes from inflammation, the end result is the samecartilage loss.
Types of Osteoarthritis
Primary (Idiopathic) Osteoarthritis
This is the classic form that shows up with age, genetics, and normal wear-and-tear. No obvious injury or disease is behind it.
Secondary Osteoarthritis
Here, a clear trigger existswhether it's a past fracture, metabolic disorder, or chronic inflammation. Knowing the type helps doctors tailor the best treatment.
| Type | Typical Onset | Main Trigger | Commonly Affected Joints |
|---|---|---|---|
| Primary | 4565 years | Age, genetics | Knees, hips, hands |
| Secondary | Any age | Injury, metabolic, inflammatory | Depends on injury site |
Four Stages Explained
Stage 1 Early Softening
Cartilage becomes slightly pliable. You might feel occasional stiffness after long periods of rest, but pain is rare.
Stage 2 Moderate Loss
Visible thinning on X-ray, intermittent pain during activity, and occasional swelling. Daily chores may start to feel heavy.
Stage 3 Significant Loss
Joint space narrowing becomes obvious. Pain is more constant, especially after weight-bearing. You may notice a clicking or grinding sensation (crepitus).
Stage 4 End-Stage Bone-on-Bone
Cartilage is gone. Bones rub directly, causing chronic pain, severe stiffness, and limited range of motion. Surgery is often considered at this point.
Common Symptoms
- Joint pain that worsens with activity and eases with rest.
- Morning stiffness lasting less than 30 minutes.
- Visible swelling or a feeling of grinding inside the joint.
- Reduced flexibility or difficulty performing everyday tasks (e.g., climbing stairs).
If you notice these signs, especially in weight-bearing joints like knees or hips, it's worth getting a professional opinion sooner rather than later.
How It's Diagnosed
Clinical Exam & History
Your doctor will ask about pain patterns, past injuries, family history, and daily activities. A physical exam can reveal tenderness, limited motion, or audible crepitus.
Imaging Tools
Standard X-rays show joint space narrowing, osteophytes (bone spurs), and other structural changes. For a more detailed look, especially in early disease, an MRI can visualize cartilage thickness and soft-tissue integrity.
Laboratory Tests
Blood work helps rule out inflammatory arthritis (like rheumatoid arthritis). Elevated C-reactive protein (CRP) or rheumatoid factor would point away from primary osteoarthritis.
Prevention Tips
Maintain a Healthy Weight
Even a modest 510% weight loss can dramatically reduce knee stress. Think of it as giving your joints a vacation from excess load.
Stay Active with Low-Impact Exercise
Swimming, cycling, and brisk walking keep muscles strong without pounding the joints. Strong surrounding muscles act as natural shock absorbers.
Strengthen Core and Leg Muscles
Exercises like squats (performed with proper form), lunges, and hip bridges improve joint alignment and distribute forces more evenly.
Mind Your Posture and Ergonomics
Whether you're at a desk or lifting boxes, keeping the spine neutral and using tools (like knee pads) reduces unnecessary joint strain.
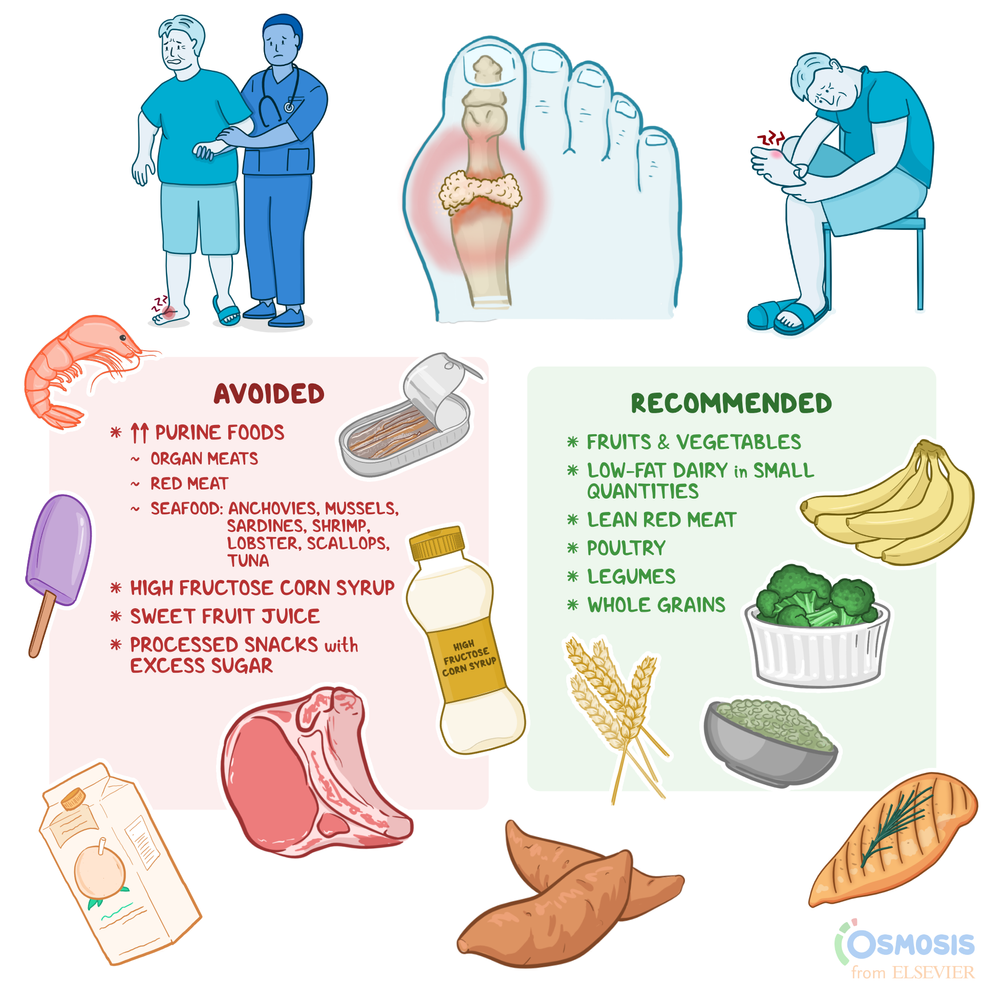
Nutrition Matters
Foods rich in omega-3 fatty acids (salmon, walnuts), antioxidants (berries, leafy greens), and vitamin D support cartilage health. Hydration also keeps the synovial fluid lubricated.
Treatment Overview
Non-Pharmacologic Approaches
Physical therapy, customized orthotics, and lifestyle modifications are the first line. Simple changeslike swapping high-heeled shoes for supportive flatscan soothe pain quickly.
Pharmacologic Options
Over-the-counter NSAIDs (ibuprofen, naproxen) help control inflammation. For persistent pain, doctors may prescribe stronger pain relievers, corticosteroid injections, or hyaluronic acid (HA) fillings directly into the joint.
Surgical Interventions
When conservative measures fail, options include arthroscopy (to clean out debris), osteotomy (realigning bone), or total joint replacement. A decision-making flowchartstarting with symptom severity, functional limitation, and imaging findingsguides whether surgery is appropriate.
What Is the Best Treatment?
There's no one-size-fits-all answer. The best treatment depends on the stage of disease, your activity goals, and overall health. A combination of weight management, targeted exercise, and appropriate medication often yields the most sustainable relief.
Real-World Stories & Myths
I Cured My Osteoarthritis FactCheck
Claims of a complete curewhether through miracle diets, extreme detoxes, or unverified supplementsrarely hold up under scientific scrutiny. Osteoarthritis is a chronic condition; it can be managed and its progression slowed, but not magically erased.
Personal Anecdote
My aunt, Linda, was diagnosed with knee osteoarthritis at 58. After adopting a low-impact water aerobics routine, losing 12 lb, and using a knee brace during gardening, she reported a 40% drop in pain within six months. Her story underscores how lifestyle adjustments can make a huge difference.
Myth-Busting Table
| Myth | Reality |
|---|---|
| Heat therapy cures OA | Heat eases muscle tension but doesn't reverse cartilage loss. |
| Only older people get OA | You can develop secondary OA after injury at any age. |
| Supplements alone stop progression | Evidence for supplements is mixed; they work best alongside exercise and weight control. |
Conclusion
Understanding the causes of osteoarthritis gives you a roadmap for action. Age and genetics set the stage, but weight, injuries, and daily habits dictate how fast the curtain falls. By staying active, watching your weight, and seeking early diagnosis, you can keep your joints moving comfortably for years to come. Have you noticed any early signs, or made a lifestyle tweak that helped your joints? Share your experience in the commentsyour story might be the spark someone else needs to start their own joint-health journey.
FAQs
What are the main causes of osteoarthritis?
The main causes of osteoarthritis include aging, joint injury, obesity, genetics, and repetitive joint stress.
Can being overweight cause osteoarthritis?
Yes, extra weight increases pressure on joints and raises the risk of developing osteoarthritis, especially in the knees and hips.
Does genetics play a role in osteoarthritis?
Yes, having family members with osteoarthritis increases your risk due to inherited genetic factors.
Can joint injuries lead to osteoarthritis?
Yes, past injuries such as fractures or ligament tears can damage joints and lead to osteoarthritis later in life.
Is osteoarthritis only caused by aging?
No, while age is a major factor, osteoarthritis can also result from injury, obesity, genetics, and other health conditions.