Quick tip: Most people notice a hoarse or breathy voice for a few days to a couple of weeks, but with simple care and, if needed, a bit of speechtherapy, clear speech usually returns within a month or two.
What Is Esophagectomy
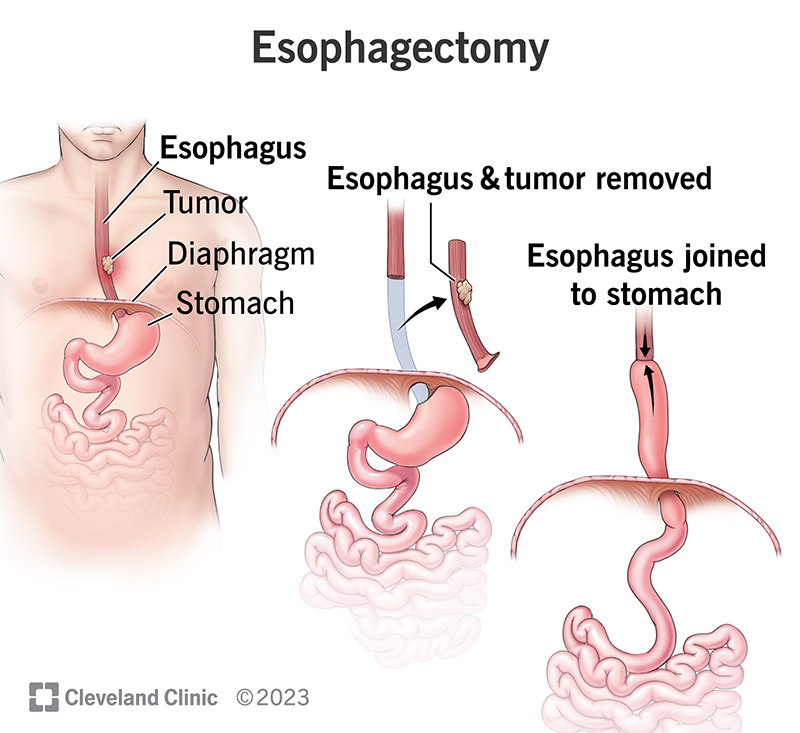
An esophagectomy is the surgical removal of part or all of the esophagus, the tube that carries food from your mouth to your stomach. Its most commonly performed to treat esophageal cancer, but can also be necessary for severe Barretts esophagus, trauma, or benign strictures.
Types of Esophageal Surgery
There are three main techniques, each with its own incision pattern and recovery timeline:
| Technique | Incision(s) | Typical Recovery | Impact on Vocal Cords |
|---|---|---|---|
| Transhiatal | Abdominal + neck | 68 weeks | Usually spares nerves |
| IvorLewis (transthoracic) | Abdominal + right chest | 810 weeks | Potential for nerve irritation |
| McKeown (threestage) | Neck, chest, abdomen | 1012 weeks | Higher risk of nerve stretch |
What Exactly Gets Removed?
Surgeons typically take out the diseased portion of the esophagus and may also reshape part of the stomach to create a new tube (called a gastric conduit) that connects the remaining esophagus to your stomach. The larynx and vocal cords are generally left untouched, but the nerves that run nearbyespecially the recurrent laryngeal nervecan be irritated or, in rare cases, damaged.
Voice After Surgery
Its natural to wonder whether losing your esophagus will also mean losing your voice. The short answer is no, but the journey back to normal speech can have a few bumps.
Why Your Voice Might Change
The esophagus sits right behind the larynx (your voice box). When surgeons operate in that area, they sometimes need to move or stretch the recurrent laryngeal nerve that tells the vocal cords when to open and close. Even a gentle tug can cause temporary hoarseness, a breathy tone, or a slightly lower pitch.
Typical Voice Changes
- Hoarseness: Most patients notice a raspy quality for the first 37 days.
- Reduced pitch range: Higher notes may feel harder to reach.
- Breathy speech: Air leaks around the cords can make words sound airy.
These changes usually improve as swelling subsides and the nerves heal. If a nerve is seriously injured, the hoarseness can become permanent, but thats uncommonespecially when surgeons use intraoperative nerve monitoring. , modern techniques dramatically lower the risk of lasting vocalcord damage.
RealWorld Experiences
Numbers and anatomy are important, but hearing from people whove lived through it makes the picture clearer.
Emilys Story
Emily, a 58yearold teacher, says, The first week after my esophagectomy, I could barely whisper my name without sounding like a wind chime. I was scared my students would notice. By week three, after a few sessions with a speech therapist, I was back to reading aloud without a hitch.
Marks Journey
Mark, who underwent an IvorLewis procedure, adds, My hoarseness lingered for about four months. I joined a support group and practiced humming exercises daily. The progress was slow, but every day I felt my voice getting stronger.
Stories like these show that while the voice may wobble at first, most patients regain comfortable speechoften with a little professional help.
Managing Voice Changes
If youre on the recovery side of an esophagectomy, here are some practical steps to keep your voice on the mend.
Immediate PostOp Care (First 48 Hours)
- Stay hydratedsip warm water or ice chips regularly.
- Use a humidifier in your room to keep throat tissues moist.
- Practice gentle vocal rest: speak softly, avoid shouting, and limit phone calls.
SpeechTherapy Tips
Professional speechlanguage pathologists can guide you through exercises that improve breath support and vocalcord closure. Common techniques include:
- Resonant voice therapy: Helps you find a clear, effortless tone.
- Breathing drills: Strengthen diaphragmatic support for smoother speech.
- Pitch glides: Gently stretch the vocal range without strain.
According to the American SpeechLanguageAudiology Association, patients who start therapy within the first month see faster voice recovery .
When to Call Your Surgeon
If you notice any of the following, seek medical advice promptly:
- Persistent hoarseness beyond six weeks.
- Difficulty swallowing liquids (a sign of possible vocalcord paralysis).
- Sudden loss of voice or painful breathing.
Life After Esophagectomy
Beyond the voice, you might be wondering about overall health, survival odds, and everyday life.
Survival Rates & Life Expectancy
Fiveyear survival after esophageal cancer surgery varies widelyroughly 3060% depending on cancer stage, patient age, and overall health. reports that earlystage patients have the best outcomes, while advanced disease carries a lower survival chance. For readers concerned about related cancers and longterm outlooks, information on prostate cancer outlook can sometimes be useful for understanding how cancer staging affects prognosis across different cancers.
LongTerm Side Effects
Living without a full esophagus does come with a set of chronic considerations:
- Dumping syndrome: Rapid gastric emptying can cause nausea, sweating, and lightheadedness after meals.
- Weight changes: Many patients lose weight initially; regaining healthy weight often takes 36 months of focused nutrition.
- Acid reflux & strictures: The new gastric conduit can develop narrowing, requiring endoscopic dilation.
Nutrition & Gaining Weight
Once youre cleared for solid foods (usually 46 weeks postop), aim for small, frequent meals rich in protein. Blenderbased smoothies, pureed soups, and soft fruits are excellent starters. Over time, you can progress to chewable textures as tolerated. Most patients find that steady, caloriedense meals help them regain lost weight within a few monthsa timeline echoed by dietitians at the Cleveland Clinic.
Quality of Life Improvements
Despite the challenges, many survivors report a return to normal social activities, work, and even hobbies within six to twelve weeks. The key is a supportive medical team, consistent followup, and a willingness to adapt eating and speaking habits.
| Recovery Milestone | Typical Timeframe | VoiceRelated Notes |
|---|---|---|
| Hospital discharge | 510 days | Hoarseness common; gentle vocal rest |
| Start soft solids | 46 weeks | Continue hydration; monitor for coughing |
| First speechtherapy session | 14 weeks | Begin resonant voice exercises |
| Clear speech | 68 weeks | Most patients regain normal tone |
| Full dietary freedom | 36 months | Voice typically stable |
Balancing Benefits & Risks
Choosing to undergo an esophagectomy isnt just a medical decision; its a life decision. On the one hand, removing the cancerous tissue can be lifesaving. On the other, youre trading a familiar anatomy for a new way of eating and speaking.
But heres the good news: modern surgical techniques, meticulous nerve monitoring, and comprehensive rehab programs mean that most patients walk away with a functional voice and a reasonable outlook on life. The key is staying informed, asking questions, and leaning on the expertise of your care team.
Conclusion
Yesyou can talk after having your esophagus removed. While the voice may sound a bit hoarse or lower at first, most people recover clear speech within weeks, especially with hydration, gentle vocal rest, and, when needed, speechtherapy. Survival rates have improved, and longterm side effects are manageable with proper nutrition and followup care. If you or a loved one are facing this surgery, remember youre not alone: surgeons, speech therapists, and countless survivors are ready to guide you every step of the way. Have questions about your specific case? Drop a comment below or reach out to a certified speechtherapistyou deserve answers and support on this journey.
FAQs
Can you speak normally after having your esophagus removed?
Yes, most patients can speak normally after an esophagectomy, though the voice may temporarily sound hoarse or breathy due to nerve irritation near the vocal cords. Speech usually improves within weeks, especially with speech therapy.
Why might my voice change after esophagus removal surgery?
Voice changes happen because the recurrent laryngeal nerve, which controls vocal cord movement, can be stretched or irritated during surgery, causing hoarseness or breathy voice that often improves as nerves heal.
How long does it take to regain clear speech after an esophagectomy?
Most patients regain clear and stable speech within 6 to 8 weeks post-surgery, though some may experience mild voice changes for several months.
Is speech therapy necessary after esophagectomy?
Speech therapy is recommended to help restore voice quality and improve breath support, pitch control, and vocal cord closure. Starting therapy within the first month can speed up voice recovery.
When should I see a doctor about voice problems after esophagus removal?
Seek medical advice if hoarseness persists beyond six weeks, if you experience sudden loss of voice, painful breathing, or difficulty swallowing liquids, as these may indicate vocal cord paralysis or other complications.