Short answer: most people with ulcerative colitis (UC) can safely use a multivitamin, but you have to pick the right one. Not every formula is created equalsome ingredients can irritate a sensitive gut or clash with your meds.
What you'll get from this post: a clear picture of why vitamins matter when you have UC, the redflags to watch for, a handful of toprated multivitamins (including options for women), dosing tips for vitaminD, and a simple plan to fit supplements into your daily routine without drama.
Nutrient Gaps Explained
Why ulcerative colitis creates deficiencies
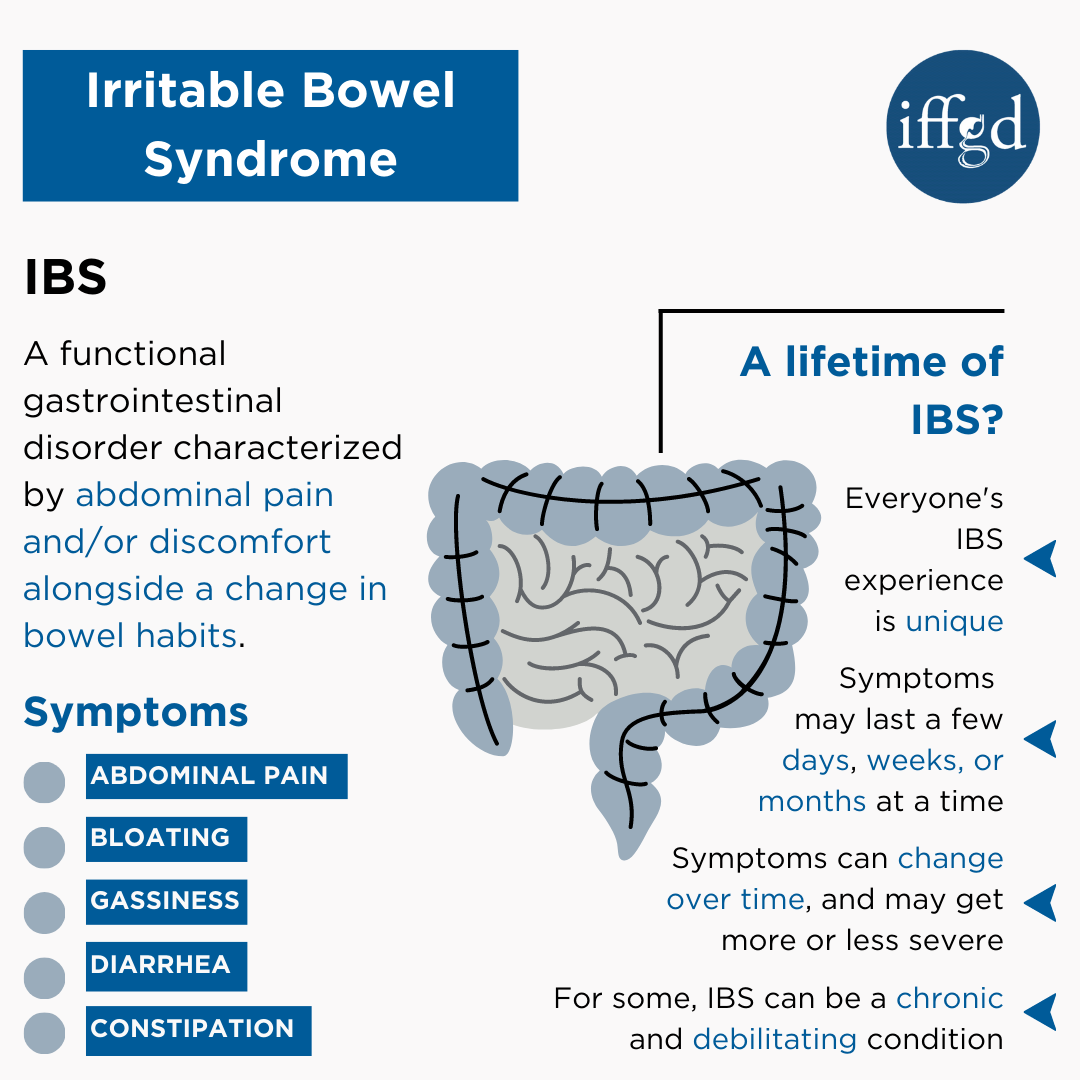
UC is a chronic inflammation of the colon. Between flareups, strict diets, and medications like 5ASA or steroids, your body often struggles to absorb key nutrients. Think of your gut as a busy highway; when there's construction (inflammation), traffic (nutrients) gets backed up or rerouted. Patients frequently experience deficiencies in vitamins and minerals vital for overall health. Supplements for ulcerative colitis can help bridge these gaps, especially when food intake is limited or absorption is compromised.
Common deficiencies you'll see
Studies from the Crohn's & Colitis Foundation and consistently point out low levels of vitaminD, vitaminB12, iron, calcium, folate, and magnesium in UC patients. Low vitaminD can worsen inflammation, while iron deficiency often shows up as fatigue or pale skin.
Quick reference table
| Deficiency | Typical symptom | Why it happens in UC |
|---|---|---|
| VitaminD | Bone pain, mood swings | Malabsorption + limited sunlight |
| VitaminB12 | Weakness, tingling | Damage to ilealterminal area |
| Iron | Fatigue, shortness of breath | Blood loss during flares |
| Calcium | Muscle cramps | Low dietary intake, steroid use |
Safety First
What the evidence says
According to a review in MedicalNewsToday, multivitamins are generally safe for most people with inflammatory bowel disease (IBD) as long as you avoid highdose iron and certain herbal extracts. The key is to treat the supplement as a supportive toolnot a cureall.
When a multivitamin can help
- During flareups when you're eating less.
- After surgery or when you're on a liquid diet.
- When labs show borderline vitamin levels.
When a multivitamin might hurt
Highdose iron, zinc, or vitaminK can aggravate inflammation, cause constipation, or interfere with blood thinners. Also, some herbal blend formulas contain ginseng or turmeric in amounts that may trigger cramping.
Redflag ingredients to avoid
- Iron (high dose): >18mg/day can be harsh on the gut.
- Zinc (excess): >40mg may suppress immunity.
- VitaminK: If you're on anticoagulants.
- Herbal stimulants: Ginseng, bitter orange, etc.
Choosing the Right
Criteria for a UCfriendly formula
Think of a good multivitamin as a gentle companion. Look for:
- Low or ironfree version.
- Added vitaminD (8001000IU) and calcium.
- Probiotic strains that support gut health.
- Glutenfree, no added sugars, and a smooth capsule or powder.
Best multivitamin for UC (quick comparison)
| Brand | Form | Iron % DV | VitaminD (IU) | Probiotic? | Price | Why UCfriendly |
|---|---|---|---|---|---|---|
| IBDEase | Softgel | 5% | 800 | Yes (Lactobacillus) | $$ | Low iron, easy on stomach |
| GentleBlend | Powder (mix) | 0% | 1000 | No | $ | Ironfree, ideal for flareups |
| CalCare Plus | Coated tablet | 10% | 600 | Yes | $$$ | Calciumbalanced, glutenfree |
Best multivitamin for women with ulcerative colitis
Women often need a bit more iron and folate, especially if they're of childbearing age. Choose a formula that offers lowdose iron (around 10mg) plus extra folic acid (400g). The CalCare Plus table above meets those needs without overloading the gut. For those seeking more nutritional advice tailored to inflammatory bowel disease, check out resources on ulcerative colitis supplements for patient-focused guidance from expert sources.
Best multivitamin for IBD (broader view)
If you have both UC and occasional Crohnstype symptoms, you might appreciate a product that adds a probiotic blend and a modest amount of magnesium (easier on the colon than magnesium oxide).
Specific Nutrient Answers
How much vitaminD should I take for ulcerative colitis?
The Endocrine Society recommends 8002000IU daily for adults with low vitaminD, and many gastroenterologists aim for the middle of that range. If your blood test shows 25OHD below 30ng/mL, start at 800IU and reassess in three months.
Best iron supplement for ulcerative colitis
When iron is truly needed, ferrous bisglycinate (a chelated form) at 1520mg per day is gentler on the gut than ferrous sulfate. Take it with food and separate it from calcium or multivitamin iron by at least two hours.
Supplements to avoid with ulcerative colitis
Besides the redflag ingredients we listed earlier, steer clear of:
- Highdose calcium carbonate (can bind other minerals).
- Magnesium oxide (acts as a laxative).
- Heavy herbal blends that aren't standardized.
Quick checklist Do I need to stop this supplement?
| Supplement | Yes/No | Reason |
|---|---|---|
| Ironrich multivitamin | No (if iron >18mg) | Potential gut irritation |
| Calcium carbonate 1200mg | Yes | Can interfere with iron absorption |
| Probiotic blend | Yes | Usually beneficial |
Daily Integration Tips
Timing with meals & medication
Take your multivitamin with a modest meal (breakfast or lunch) to cushion the stomach. If you're on 5ASA pills, keep a twohour gap between them and any ironcontaining supplementthis helps each ingredient work its magic without stepping on each other's toes. You can read more about this practical approach and comprehensive nutrient management for UC in vitamins and supplements for UC.
Managing flareups
During a flare, swap your regular multivitamin for an ironfree, liquid version. Liquids travel faster and are less likely to cause cramping. Monitor your symptoms for a week or two; if the gut feels calmer, you're on the right track.
Tracking your response
Keeping a simple diary can be a gamechanger. Note the date, what you took (dose, brand), stool consistency (using the Bristol Stool Chart), energy level, and any tummy aches. After a month, patterns emerge, and your doctor can adjust the plan with real data.
Sample diary template (downloadable PDF)
Feel free to copy the table below into a spreadsheet or print it out.
| Date | Supplement + Dose | Meal Time | Stool (Bristol #) | Energy (110) | Notes |
|---|
Expert Insights
What gastroenterologists say
Dr. Maya Patel, a gastroenterologist at the IBD Center of Boston, explained, We usually recommend a modest multivitamin that covers vitaminD, calcium, and Bcomplex vitamins, but we keep iron low unless labs show a clear deficiency. Oversupplementation can be as harmful as undersupplementation.
Patient story: Sarah's 3month trial
Sarah, a 34yearold teacher, started the GentleBlend powder during a mild flare. Within six weeks, her blood work showed a 12% rise in vitaminD and her fatigue scores dropped from 5/10 to 2/10. She credits the lowiron formula for not worsening her cramps.
Sources you can trust
Throughout this article we drew from reputable outlets such as the Crohn's & Colitis Foundation, , and peerreviewed journals (see PMC6342481). These references help keep the advice evidencebased and trustworthy.
Bottom Line
In short, yesyou can take multivitamins with ulcerative colitis, but choose wisely. Look for lowiron, vitaminDrich formulations, consider probiotic additions, and always sync your supplements with your medication schedule. Keep an eye on redflag ingredients, track how you feel, and stay in close contact with your gastroenterologist or dietitian. If you're ready to give your body the nutritional backup it deserves, start with a gentle, UCfriendly multivitamin and watch your energy and mood improve.
Got a favorite brand or a story to share? Drop a comment below, or download the quickstart guide to get your supplement routine off the ground. Here's to feeling stronger, one vitamin at a time!
FAQs
Can multivitamins worsen ulcerative colitis symptoms?
Most multivitamins are well‑tolerated, but high‑dose iron, zinc, or certain herbal extracts can irritate an inflamed colon. Choose low‑iron, gut‑friendly formulas to minimize risk.
What ingredients should I look for in a multivitamin for UC?
Prioritize vitamin D (800‑1000 IU), calcium, B‑complex vitamins, and a probiotic blend. Avoid high‑dose iron, excessive zinc, vitamin K (if on anticoagulants), and herbal stimulants.
How much vitamin D is safe for ulcerative colitis patients?
The Endocrine Society recommends 800–2000 IU daily for adults with low levels. Start at 800 IU if your 25‑OH‑D is below 30 ng/mL and recheck labs after three months.
Is an iron‑free multivitamin better during a flare?
Yes. During flares, an iron‑free or low‑iron formula reduces gut irritation and constipation. If iron is needed, use a chelated form like ferrous bisglycinate, taken separately from other supplements.
Can I take a multivitamin with my UC medication?
Generally you can, but keep a two‑hour gap between multivitamins that contain iron or calcium and medications such as 5‑ASA or steroids. This helps both the drug and the nutrients absorb properly.