Short answer: Yes, an overactive parathyroid gland can play a part in the breathing pauses you experience at night. In the sections below Ill walk you through why that happens, how doctors figure it out, and what you can do to feel rested again.
Quick Facts Overview
Researchers have been digging into the link between parathyroid hormone (PTH), calcium levels, and sleepdisordered breathing for a few years now. A 2022 study found that people with high PTH and low vitaminD were noticeably more likely to have obstructive sleep apnea (OSA). In simple terms, excess calcium can stiffen the muscles that keep your airway open, while hormonal swings throw off the bodys natural sleep clock.
Here are the headline numbers you might find useful:
- Up to 97% of patients with primary hyperparathyroidism report sleep problems before surgery (Columbia Surgery data).
- After a successful parathyroidectomy, about 7090% notice a marked improvement in sleep quality.
- Primary hyperparathyroidism (the most common form) tends to have a stronger OSA connection than secondary hyperparathyroidism.
Body Effects Explained
Calcium overload & neuromuscular tone
When calcium floods the bloodstream, it doesnt just affect your bones. Calcium is a key player in muscle contraction. Too much of it can make the tiny muscles that line your throat a little tightropeready, so theyre less able to spring open during inhalation. The result? More breathing pauses, especially when you lie flat.
Hormonal turbulence PTH, vitaminD, and circadian rhythm
PTH and vitaminD talk to each other like an old married couple. When PTH shoots up, vitaminD often drops, and that combo can interfere with melatonin, the hormone that signals time to sleep. Think of it as trying to have a conversation in a noisy room the message gets garbled, and you end up tossing and turning.
Brain fog, feeling hot & indirect sleep killers
Hyperparathyroidism isnt just about calcium; it also messes with brain chemistry. Many patients describe foggy thinking, mood swings, and even an uncomfortable heat sensation (hyperparathyroidism and feeling hot). Those symptoms can make it harder to unwind at night, adding another layer to the sleepapnea puzzle.
Real World Stories
Janes 6month journey
Jane, a 52yearold teacher, was convinced her snoring was just agerelated. After a routine blood test revealed high calcium, she got a neck ultrasound and was diagnosed with primary hyperparathyroidism. Her sleep study before surgery showed an apneahypopnea index (AHI) of 22 (moderate OSA). Six months after a minimally invasive parathyroidectomy, her AHI dropped to 5 and she reported feeling refreshed for the first time in years.
Mikes CPAP & vitaminD story
Mike, 38, was already using a CPAP machine for OSA. When his endocrinologist discovered elevated PTH, they added a vitaminD supplement to his regimen. Over the next few months his nightly CPAP pressure needed decreased, and his daytime fatigue vanished. Its a reminder that managing hormone levels can make a CPAP device work smarter, not harder.
Postsurgery concerns many ask
Can I sleep on my side after parathyroid surgery? Absolutely, once your incision has healed (usually 12weeks). Sleeping on your side can actually reduce OSA severity for many people.
Other common postparathyroidectomy problems include temporary hoarseness, calcium cravings, and shortterm insomnia. All of these usually resolve within a few weeks as your body finds its new balance.
Diagnosis Steps Guide
When to suspect the connection
If you notice any of these red flags, its worth talking to your doctor about checking parathyroid function:
- Persistent loud snoring or witnessed pauses in breathing.
- Unexplained fatigue despite a full nights sleep.
- Blood work showing high calcium or elevated PTH.
- Feeling unusually hot, brainfoggy, or gaining weight without a clear reason.
Lab values to watch
| Test | Normal range | Typical PHPT range |
|---|---|---|
| Serum calcium | 8.510.2mg/dL | >10.5mg/dL |
| PTH | 1065pg/mL | >65pg/mL |
| VitaminD (25OH) | 30100ng/mL | Often <30ng/mL |
Sleep study (polysomnography)
A nightlong sleep study tells you how many breathing pauses you have, how low your oxygen drops, and what stage of sleep they occur in. When PTH is high, you might see a pattern of fragmented breathing that improves after the hormone levels normalize.
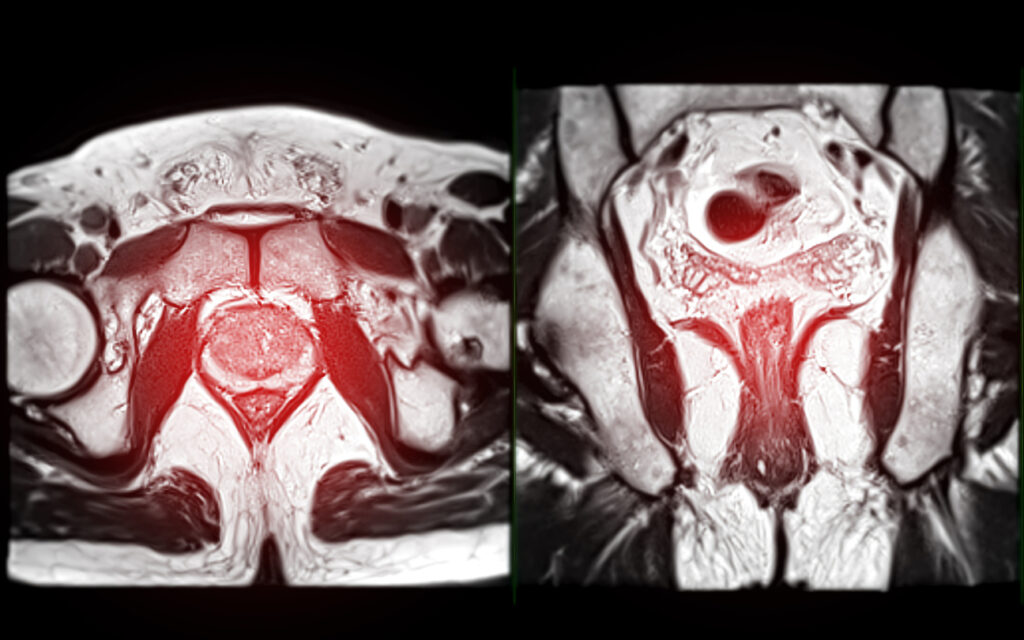
Imaging & gland localization
Ultrasound of the neck and a sestamibi scan are the goto tools for locating an overactive parathyroid gland. These images help surgeons plan a focused, minimally invasive removal.
Treatment Options Summary
Parathyroidectomy the goldstandard cure
Removing the problematic gland(s) restores calcium balance in most cases. Success rates for resolving sleep issues sit around 8090%. After surgery youll likely need a short course of calcium supplements while your body readjusts.
Postop care checklist
- Take prescribed calcium and vitaminD supplements as directed.
- Check your calcium and PTH levels at the 6week followup.
- Sleep on your side if you feel comfortable; avoid stomachsleeping for the first week.
- Keep a sleep diary for the first month to track changes.
CPAP therapy bridging the gap
Even after the gland is gone, some folks need a CPAP machine for a few weeks or months while the airway remembers how to stay open. Interestingly, lowering PTH can also reduce the pressure settings you need on the CPAP.
Lifestyle tweaks that help both conditions
Here are a few everyday moves that can support your sleep and hormone health:
- Boost vitaminD with safe sun exposure or a supplement (under doctor guidance).
- Maintain a healthy weight excess weight can worsen OSA and may be linked to the metabolic effects of high calcium.
- Avoid caffeine after 2p.m. and keep a consistent bedtime routine.
- Practice gentle neck stretches before bed; they can improve airway flexibility.
Bottom Line Takeaway
Hyperparathyroidism can indeed be a silent catalyst for sleep apnea, but the good news is that its a treatable cause. By checking your hormone levels, getting a targeted sleep study, and, when needed, undergoing a focused parathyroidectomy, you give yourself a solid chance at breathing easy at night again. As always, partner with an endocrinologist and a sleepmedicine specialistshared decisionmaking makes the journey smoother.
If youve been wrestling with restless nights, consider asking your doctor whether an overactive parathyroid could be part of the story. You deserve nights of real rest, and the tools to get there are right at your fingertips.
FAQs
Can hyperparathyroidism cause sleep apnea?
Hyperparathyroidism primarily causes insomnia and sleep disturbances rather than obstructive sleep apnea (OSA) specifically. While elevated PTH and calcium levels disrupt sleep quality by affecting nerve function and circadian rhythm, the research distinguishes between general sleep problems and the breathing obstruction characteristic of OSA. Some patients may experience both conditions independently.
How does high calcium affect sleep?
Elevated calcium levels interfere with nerve cell communication, which disrupts sleep regulation and can cause fatigue and sleep disturbances. Additionally, high calcium can contribute to muscle spasms, restless leg syndrome, and joint pain—all of which make it difficult to fall or stay asleep.
What percentage of hyperparathyroidism patients have sleep problems?
Approximately 60% of patients with primary hyperparathyroidism report some form of sleep impairment, and about 25% meet the criteria for clinical insomnia. This rate is more than four times higher than the general population, where approximately 6% experience clinical insomnia.
Does parathyroidectomy improve sleep?
Yes, parathyroidectomy significantly improves sleep in most patients. Studies show that over 70% of patients experience improved sleep quality after surgery, and approximately 72% of those with pre-operative clinical insomnia achieve resolution of symptoms. Patients also report increased total sleep hours and fewer nighttime awakenings.
What causes sleep problems in hyperparathyroidism?
Multiple factors contribute: elevated calcium disrupts nerve communication and circadian rhythm regulation, altered cardiac autonomic nerve function affects sleep cycles, and secondary symptoms like fatigue, muscle spasms, and restless leg syndrome interfere with sleep initiation and maintenance. These effects typically resolve after parathyroid hormone levels normalize.