Looking for a fast rundown of every autoimmune skin disorder? Below youll find a clear, doctorverified list of the most common and rare conditions, key signs to watch for, and the latest treatment pathsso you can spot a problem early and talk to your dermatologist with confidence.
Why it matters: Autoimmune skin diseases can mimic everyday rashes, but the underlying immune attack needs specific care. Knowing the differences helps you get the right help, whether youre exploring medication, lifestyle tweaks, or natural remedies.
Why the List Matters
What is autoimmune in plain language?
In simple terms, an autoimmune reaction is when your immune systemnormally the hero fighting infectionsmistakes your own skin cells for invaders and starts attacking them. That misguided battle shows up as rashes, blisters, discoloration, or hair loss.
How does skinfocused autoimmunity differ from systemic disease?
Some diseases, like rheumatoid arthritis, target joints everywhere. Others, like lupus, affect many organs and the skin at the same time. When the skin is the main stage, the symptoms are often visible first, giving you a chance to catch the problem early.
Who should use this list?
Anyone whos noticed a persistent rash, a family member with an autoimmune condition, a primarycare provider, or a medical student looking for a quick reference can benefit. Think of this list as a friendly cheatsheet you can pull up before a doctor's visit.
Common Autoimmune Skin Disorders
What are the most frequently seen conditions?
Below is a quicklook table that captures the core details youll need when talking to a dermatologist. All data are drawn from reputable sources such as the National Institute of Arthritis and Musculoskeletal and Skin Diseases and DermNet NZ.
| Disorder | Quick Symptom Snapshot | Typical Onset | FirstLine Treatment |
|---|---|---|---|
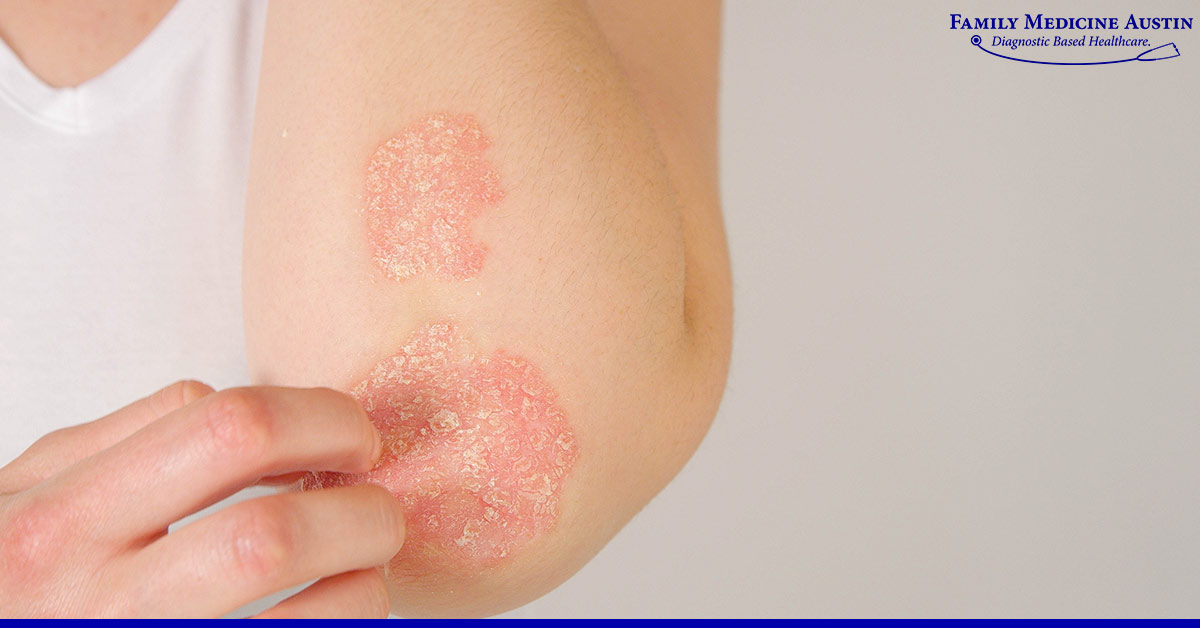
| Psoriasis | Red, scaly plaques, often on elbows/knees | Teens30s | Topical steroids, biologics |
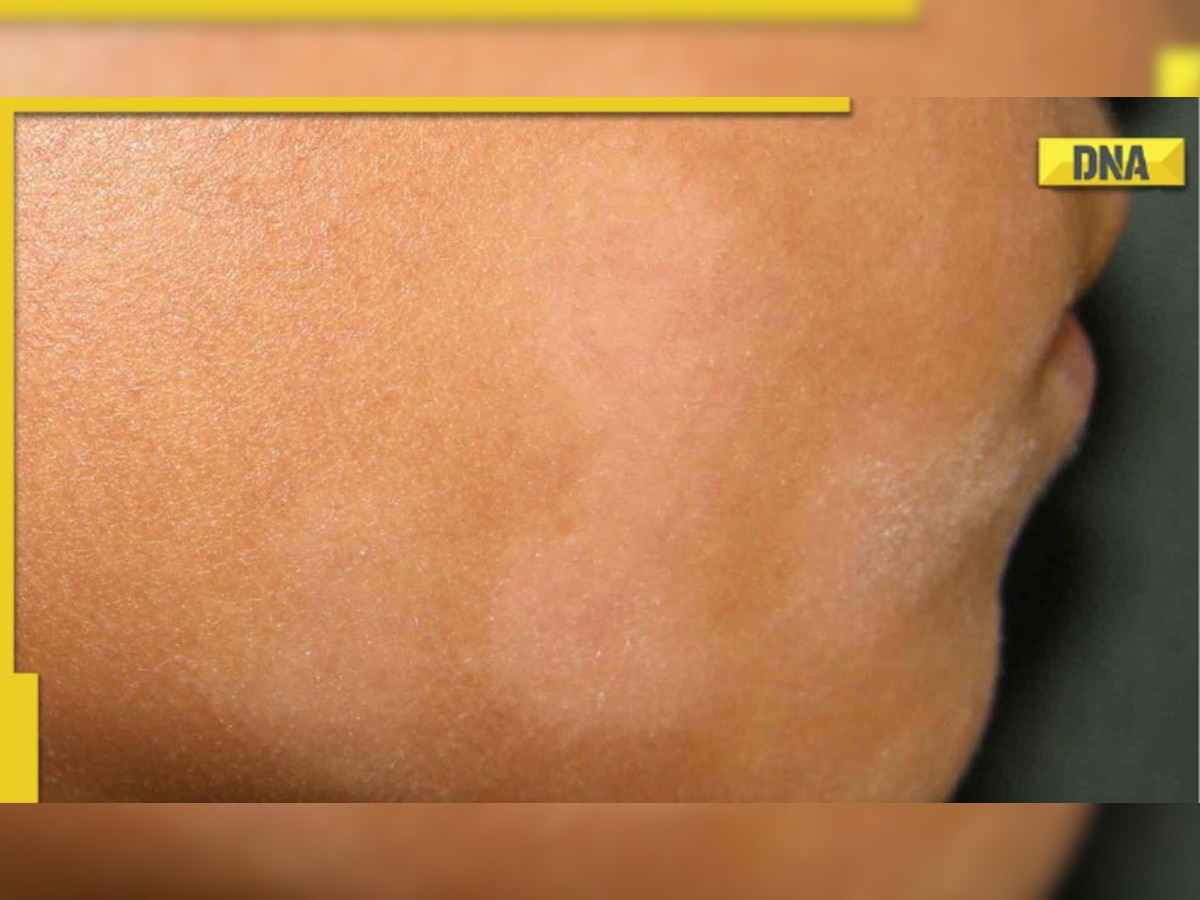
| Vitiligo | Depigmented white patches, variable size | Any age | Topical tacrolimus, NBUVB therapy |
| Alopeciaareata | Sudden, round hair loss spots | Childrenadults | Intralesional steroids, JAK inhibitors |
| Dermatomyositis | Purple heliotrope rash + muscle weakness | 4060y | Systemic steroids, IVIG |
| Cutaneous lupus | Butterfly rash across cheeks, photosensitivity | 2040y | Antimalarials, diligent sun protection |
Realworld example
Jane, a 28yearold graphic designer, thought her dry skin was just seasonal. When the red, thick patches on her elbows didnt improve with moisturizer, a quick doctor visit confirmed psoriasis. Early diagnosis let her start a topical treatment that cleared the plaques before they spread.
Rare Autoimmune Skin Conditions
Which disorders are easy to miss?
Rare doesnt mean unimportant. Conditions like pemphigus vulgaris or bullous pemphigoid can be lifethreatening if left untreated, yet their signs are often mistaken for simple acne or eczema.
Spot the difference: pemphigus vs. pemphigoid
Pemphigus vulgaris produces flaccid blisters that rupture easily, leaving painful raw skin. Bullous pemphigoid, on the other hand, creates tense blisters that stay intact longer and usually appears in older adults. Recognizing that nuance can guide a dermatologist toward the right biopsy.
Photo gallery ideas
When you search for photos of autoimmune skin disorders, aim for clinical images sourced from reputable medical libraries. Look for clear alttext like Pemphigus vulgaris blister on forearm to ensure accessibility.
Case study prompt
Consider Michael, a 32yearold accountant. He was treated for eczema for months until a dermatologist, noticing the pattern of fragile blisters, ordered a skin biopsy. The result? Pemphigus vulgaris. Early systemic therapy prevented a severe infection.
Spotting Early Symptoms
What redflag skin changes should I watch for?
Not every itch is harmless. Keep an eye on these clues:
- Rash persisting longer than two weeks.
- Symmetry (both sides of the body looking alike).
- Worsening after sun exposure (photosensitivity).
- Concurrent systemic signs: joint pain, fatigue, fever.
When is a rash more than just a rash?
If your skin issue comes with unexplained joint aches, sudden weight loss, or a fever that wont break, the immune system is probably sending you a louder alarm. In those cases, a full autoimmune disease skin rashes workupincluding blood tests for ANA, dsDNA, and specific autoantibodieswill give the doctor a clearer picture.
Earlystage rash picture resources
Highquality early stage images can be found on the University of Utah Dermatology gallery and the , which describe the subtle beginnings of many conditions.
Personal anecdote
I once thought a faint red line on my forearm was a scratch. Weeks later it turned into a welldefined, itchy plaque. A quick visit to my dermatologist revealed early cutaneous lupus. The takeaway? Trust your instincts and act fast.
Treatment Options Overview
What are the standard medical therapies?
For most autoimmune skin diseases, the first line is a blend of topical agents (steroids, calcineurin inhibitors) and systemic meds if the disease is moderatetosevere. Biologicslike adalimumab for psoriasistarget specific immune pathways, offering powerful control with fewer broadscale side effects.
Which emerging drugs are on the horizon?
JAK inhibitors (tofacitinib, upadacitinib) have shown promise for alopecia areata and vitiligo, while newer PDE4 inhibitors such as crisaborole are gaining traction for mild-to-moderate eczematype presentations. Ongoing clinical trials continue to expand the toolbox.
How to treat autoimmune skin disorders naturally?
Naturally doesnt replace prescription care, but it can complement it. Here are three evidencebacked tweaks:
- Stress reduction Mindbody practices (yoga, meditation) lower cortisol, which can calm an overactive immune system.
- Nutrition Omega3 fatty acids (found in salmon, flaxseed) have antiinflammatory properties, while vitaminD deficiency is linked to worse psoriasis outcomes.
- Gentle skin care Fragrancefree moisturizers and barrierrepair creams (ceramidebased) help protect compromised skin.
Always discuss supplement use with your physician to avoid interactions with systemic meds.
Safety disclaimer
Natural approaches should be viewed as adjuncts. If a rash spreads rapidly, bleeds, or is accompanied by fever, seek professional care immediately.
Build Your Action Plan
What should my selfscreen checklist look like?
Print or write down the following and compare it with any skin changes you notice:
- Duration: Is the rash >2weeks?
- Pattern: Symmetrical? Located on sunexposed areas?
- Accompanying signs: Joint pain, fatigue, fever?
- Photos: Take clear pictures (good lighting, closeup) to show your doctor.
How to prepare for a dermatologist visit?
Bring these items:
- A printed copy of your checklist.
- Photos (including earlystage images) of the rash.
- List of current medications, supplements, and any allergies.
- Specific questions: What tests do you recommend? What are the short and longterm risks of the treatment options?
Where can I find reliable support?
Trusted resources include the Autoimmune Registry, the National Institute of Arthritis and Musculoskeletal and Skin Diseases (), and patientled communities on platforms like Reddits r/AutoimmuneSkin. Connecting with others who have walked the same path can provide emotional relief and practical tips.
Conclusion
Understanding the full autoimmune skin disease list empowers you to recognize warning signs, ask the right questions, and partner effectively with your healthcare team. Whether youre dealing with a common condition like psoriasis or navigating the uncertainty of a rare disorder, a balanced approachcombining evidencebased medication, lifestyle tweaks, and trusted supportoffers the best chance for clear skin and peace of mind. Take the checklist, capture those photos, and remember: youre not alone.
For readers specifically concerned about loss of pigment, learning more about the vitiligo causes can help you and your clinician trace potential triggers and decide whether treatments like NBUVB or topical tacrolimus are appropriate.
FAQs
What are the most common autoimmune skin diseases?
The most common autoimmune skin diseases include psoriasis, vitiligo, alopecia areata, dermatomyositis, and cutaneous lupus. These conditions have distinct symptoms such as scaly plaques, white depigmented patches, hair loss spots, purple rashes, and butterfly-shaped facial rashes.
How are autoimmune skin diseases typically treated?
Treatments often start with topical corticosteroids and calcineurin inhibitors. For moderate to severe cases, systemic medications including immunosuppressants, biologics, and JAK inhibitors are used. Phototherapy and natural adjuncts like stress reduction and nutrition may also support therapy.
What symptoms suggest an autoimmune cause rather than a common rash?
Signs include rashes lasting more than two weeks, symmetrical distribution, photosensitivity, and systemic symptoms like joint pain, fatigue, or fever. Persistent or worsening skin changes should prompt evaluation.
What is the difference between pemphigus vulgaris and bullous pemphigoid?
Pemphigus vulgaris causes fragile, flaccid blisters that rupture easily, leading to painful raw areas, while bullous pemphigoid produces tense blisters that remain intact longer, mostly affecting older adults.
Can lifestyle changes improve autoimmune skin disease outcomes?
Yes, while they do not replace medical treatment, practices such as stress management, anti-inflammatory nutrition (like omega-3 fatty acids), and gentle skin care can help modulate symptoms and improve skin barrier function.