Quick Answers
What is autoimmune progesterone dermatitis?
Think of your skin as a dramaqueen that suddenly decides to put on a show every month, just because your hormones are doing their usual dance. Autoimmune progesterone dermatitis (APD) is a rare condition where your immune system mistakenly attacks your own skin whenever progesterone spikes during the luteal phase of your cycle. The result? Red, itchy, sometimes painful rashes that can appear anywherefrom your chest to the backs of your knees.
Can I treat APD naturally?
Yes, you canbut naturally doesnt mean alone. A thoughtful blend of lifestyle tweaks, diet changes, and targeted supplements can calm the flareups, while medical care remains the safety net, especially if youre dealing with severe symptoms or planning a pregnancy.
Is APD dangerous?
Most cases are uncomfortable, not lifethreatening. However, when the rash spreads to the throat or causes swelling, it can become an emergency. Knowing the redflag signs and when to call a doctor is essential.
What Is APD
How does progesterone trigger the rash?
Progesterone rises after ovulation, preparing the uterus for a potential pregnancy. In people with APD, this hormone is mistakenly identified as an invader. Immune cells release histamine and other inflammatory messengers, leading to the classic hiveslike eruption. Think of it as a false alarm that sets off the entire fire department.
Typical symptoms & timing
Symptoms usually start 310 days after ovulation and fade when progesterone drops. Common signs include:
- Urticaria (raised, red welts)
- Swelling (especially around the eyes or lips)
- Intense itching or burning
- Occasional blistering or eczemalike patches
These are the autoimmune progesterone dermatitis symptoms youll hear people describe on forums.
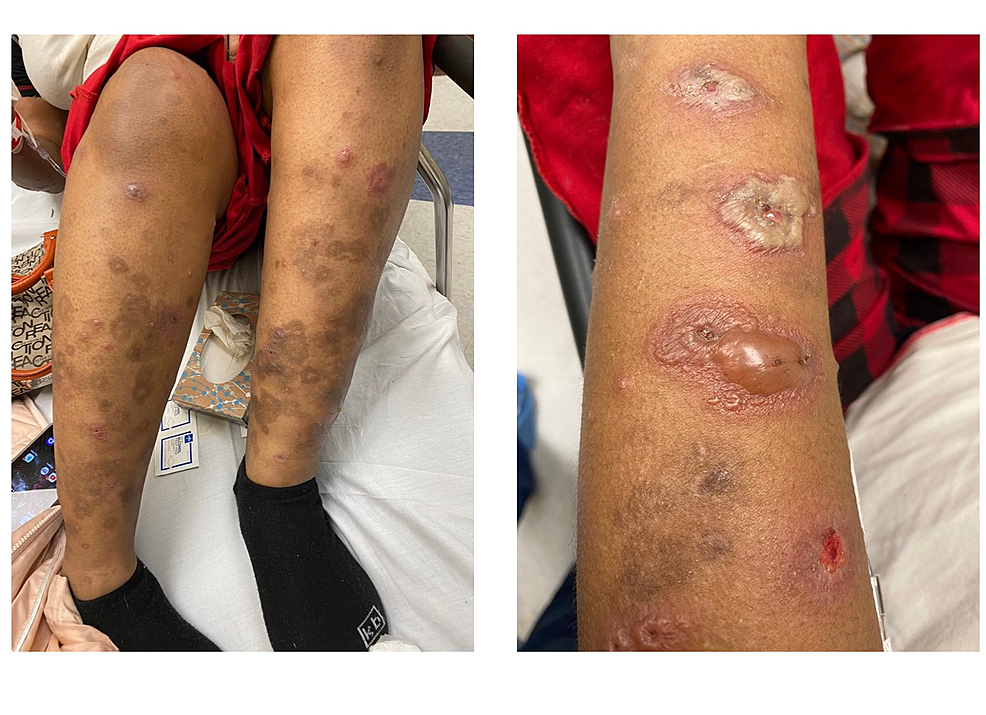
Progesterone rash pictures what to look for
When you search for progesterone rash pictures, youll see a wide rangefrom tiny hives to widespread redness. Trusted sites like showcase clear images that can help you confirm whether your breakout fits the pattern.
How is APD diagnosed?
Diagnosing APD is a bit like detective work. Your doctor may order:
- Skin biopsy to rule out other conditions
- Intracutaneous progesterone test (a tiny amount of hormone injected under the skin)
- Hormone tracking charts to correlate flareups with your menstrual cycle
All of these steps help ensure you get the right labeland the right treatment plan.
Medical Options
Firstline drugs
Antihistamines (like cetirizine) and short courses of oral corticosteroids can tame the itching and redness fast. Theyre often the goto autoimmune progesterone dermatitis: treatment for a sudden flare.
Hormonal suppression
Because progesterone is the spark, many physicians try to dim the flame by lowering its levels:
- Combined oral contraceptives (COCs) that contain estrogenonly or lowdose progesterone
- Gonadotropinreleasing hormone (GnRH) agonists, which temporarily pause ovarian hormone production
- Tamoxifen or even surgical oophorectomy in the most stubborn cases
These approaches can be effective, but they also come with sideeffectsthink mood swings, bone density loss, or reduced fertility, which is why many look to natural adjuncts first.
Progesterone desensitization
In specialty centers, some patients undergo a gradual allergy shots protocol, where tiny amounts of progesterone are introduced under medical supervision. Success rates vary, and the process can be lengthy, but its a lifesaver for a minority who cant tolerate hormonal suppression.
Case study: pregnancy remission
A 2022 study in reported a woman whose APD completely vanished during pregnancylikely because the immune system shifts toward tolerance. While fascinating, pregnancy isnt a guaranteed cure, and careful monitoring remains essential.
Natural Strategies
Lifestyle tweaks that calm the immune response
Stress is a silent partner in many autoimmune flareups. Simple habits can make a big difference:
- Prioritize 78 hours of sleep each nightyour body repairs immune misfires while you snooze.
- Practice gentle stressreduction techniques: a 10minute breathing exercise, short walks, or a favorite hobby.
- Stay active. Moderate exercise (like yoga or brisk walking) improves circulation and reduces inflammatory markers.
Dietary approaches foods to avoid & foods to embrace
Food can either fan the flame or douse it. Below is a quick reference you can print and stick on your fridge.
| Foods to Avoid (Potential Triggers) | Foods to Embrace (Soothing Allies) |
|---|---|
| Highhistamine items: aged cheese, fermented soy, smoked meats, alcohol | Omega3rich fish (salmon, sardines) |
| Nightshades: tomatoes, peppers, eggplant, potatoes | Leafy greens (spinach, kale, arugula) |
| Processed sugars & refined carbs | Probioticrich foods: kefir, sauerkraut, plain yogurt |
| Dairy (if youre lactosesensitive) | Glutenfree whole grains: quinoa, millet |
Sample 7day meal plan
Heres a lowhistamine, antiinflammatory menu that keeps the gut happy and the skin calm. Feel free to swap proteins or veggies based on your preferences.
- Day 1: Breakfast Smoothie with kale, frozen berries, coconut water, and a scoop of plant protein. Lunch Quinoa salad with cucumber, avocado, and grilled salmon. Dinner Steamed broccoli, roasted sweet potato, and a side of fermented kimchi (if tolerated).
- Day 2: Breakfast Overnight oats made with oat milk, chia seeds, and a drizzle of maple syrup. Lunch Lentil soup (no tomatoes) with carrots and spinach. Dinner Baked cod, asparagus, and a mixed greens salad with oliveoil vinaigrette.
- continue similarly for Days 37.
Supplemental allies
While food is the foundation, a few wellchosen supplements can give your immune system a gentle nudge toward balance:
- VitaminD (1,0002,000IU daily) supports overall immune regulation.
- Quercetin (500mg twice daily) a natural antihistamine that can blunt flareups.
- Zinc (30mg daily) essential for skin repair.
- Highquality probiotic (Lactobacillusplantarum, Bifidobacteriumlongum) promotes gutskin axis health.
Always check with your doctor before starting any new supplement, especially if youre on hormonal medication.
Topical natural remedies
When the itch gets intense, reach for gentle, soothing options:
- Cool oatmeal baths (colloidal oatmeal) to calm inflammation.
- Calendula oil or creamhas mild antiinflammatory properties.
- Cold compresses (wrapped in a cloth) for 1015minutes, several times a day.
Functionalmedicine protocols
Some practitioners go deeper, aiming to reset the immune system. Common steps include:
- Detoxifying the liver with milk thistle or Nacetylcysteine.
- Balancing blood sugar to avoid spikes that can worsen inflammation.
- Testing for hidden food sensitivities (e.g., gluten, dairy) and eliminating triggers.
These protocols can be powerful, but they require professional guidance to avoid nutrient gaps.
Pregnancy & Fertility
Can I get pregnant with APD?
Absolutely. Many women with APD have healthy pregnancies. The condition doesnt affect the ability to conceive, but it does mean youll need a close partnership with your OBGYN and dermatologist to manage flareups safely.
How does pregnancy affect the rash?
Hormonal shifts during pregnancy can sometimes put APD into remissionas the Frontiers case notedwhile in other instances, the rash may intensify. Monitoring your skin and keeping a symptom diary can help you and your care team spot patterns early.
How to relieve hives and soothe flareups naturally
When flares look like hives, consider gentle antiinflammatory herbs and remedies alongside medical advice. For mild, intermittent hives, some people find relief from herbal approaches; for example, specific hives relief herbs (like butterbur or nettle extracts) taken under guidance may reduce itch and histamine responses. Always tell your clinician about any herbal product before use to avoid interactions with other treatments.
Safe natural options during preconception and pregnancy
While youre planning a baby, stick to lowrisk strategies:
- Maintain the antiinflammatory diet described above.
- Focus on stressreduction (prenatal yoga, meditation).
- Choose supplements that are pregnancysafelike prenatal vitamin D and gentle probiotics.
If your symptoms become unmanageable, your doctor may suggest a short course of lowdose steroids or a carefully selected hormonal therapy that wont harm a developing fetus.
Risks vs Benefits
Potential benefits of natural treatment
Going the natural route can lower medication sideeffects, empower you with daily control, and often improve overall wellbeing (better sleep, clearer skin, more energy). Plus, youll learn a lot about how your body reacts to food, stress, and environmenta priceless skill set.
Possible risks & red flags
Nothing is riskfree. Some pitfalls to watch for:
- Nutrient deficiencies if you cut out entire food groups without replacements.
- Insufficient symptom control, which could lead to chronic skin damage or secondary infections.
- Delaying professional medical care when a flare becomes severe.
Checklist: Is my natural plan safe?
Ask yourself:
- Do I still see a dermatologist regularly?
- Am I tracking my cycle and symptoms accurately?
- Do I have a backup medication (antihistamine or steroid) for emergencies?
- Am I getting enough protein, calcium, and essential vitamins?
If you answered yes to most, youre on solid ground.
Finding Trusted Professional Help
What to ask your dermatologist
When you schedule an appointment, bring these questions:
- Do you offer a progesterone skin test, and how reliable is it?
- Can I combine a lowdose hormonal method with my natural plan?
- What signs mean I should start a short steroid burst?
- Are there any clinical trials for new therapies I could consider?
When to seek urgent care
If you notice any of the following, call 911 or head to the ER immediately:
- Swelling of the lips, tongue, or throat
- Difficulty breathing or wheezing
- Sudden, widespread rash accompanied by fever
List of reputable clinics & support groups
Many countries have dedicated allergy and dermatology centers that specialize in hormonerelated skin disorders. A quick search for progesterone hypersensitivity clinic plus your city can point you to experts. Online support groupslike the Hormone Allergy Associationalso offer peertopeer advice and a sense of community.
Conclusion
Autoimmune progesterone dermatitis can feel like an unwelcome monthly visitor, but you dont have to endure it alone. By pairing proven medical treatments with thoughtful natural strategiesbalanced diet, stress control, safe supplements, and gentle skin careyou can dramatically reduce flareups and reclaim comfort. Remember, the goal isnt to replace your doctor, but to empower yourself with knowledge and habits that keep the skin calm while your hormones do their thing. Have you tried any of these natural ideas? Share your experience in the comments, download the printable symptomtracker, and feel free to ask any questions. Together, well turn those monthly rashes into a thing of the past.
FAQs
What causes autoimmune progesterone dermatitis?
Autoimmune progesterone dermatitis is caused by an immune system reaction that mistakenly attacks the skin in response to rising progesterone levels during the luteal phase of the menstrual cycle.
Can lifestyle changes help manage APD symptoms?
Yes. Stress reduction, adequate sleep, gentle exercise, and an anti-inflammatory diet can help calm immune responses and reduce flare-ups in APD.
Are there safe natural supplements for autoimmune progesterone dermatitis?
Supplements such as vitamin D, quercetin, zinc, and high-quality probiotics may support immune balance and skin health but should be taken under medical supervision.
Is it possible to get pregnant with autoimmune progesterone dermatitis?
Yes, many women with APD have healthy pregnancies. Close medical monitoring is essential to manage flare-ups safely during pregnancy and preconception.
When should I seek emergency care for APD?
Urgent care is needed if you experience swelling of the lips, tongue, or throat, difficulty breathing, or sudden widespread rash with fever, as these can signal a severe allergic reaction.