Most people dont realize that AML can hide in the fluid surrounding your brain and spinal cord, and when it does, the experience feels like navigating a maze in the dark. The good news? With the right info and a supportive team, you can find clear paths forward.
What is AML?
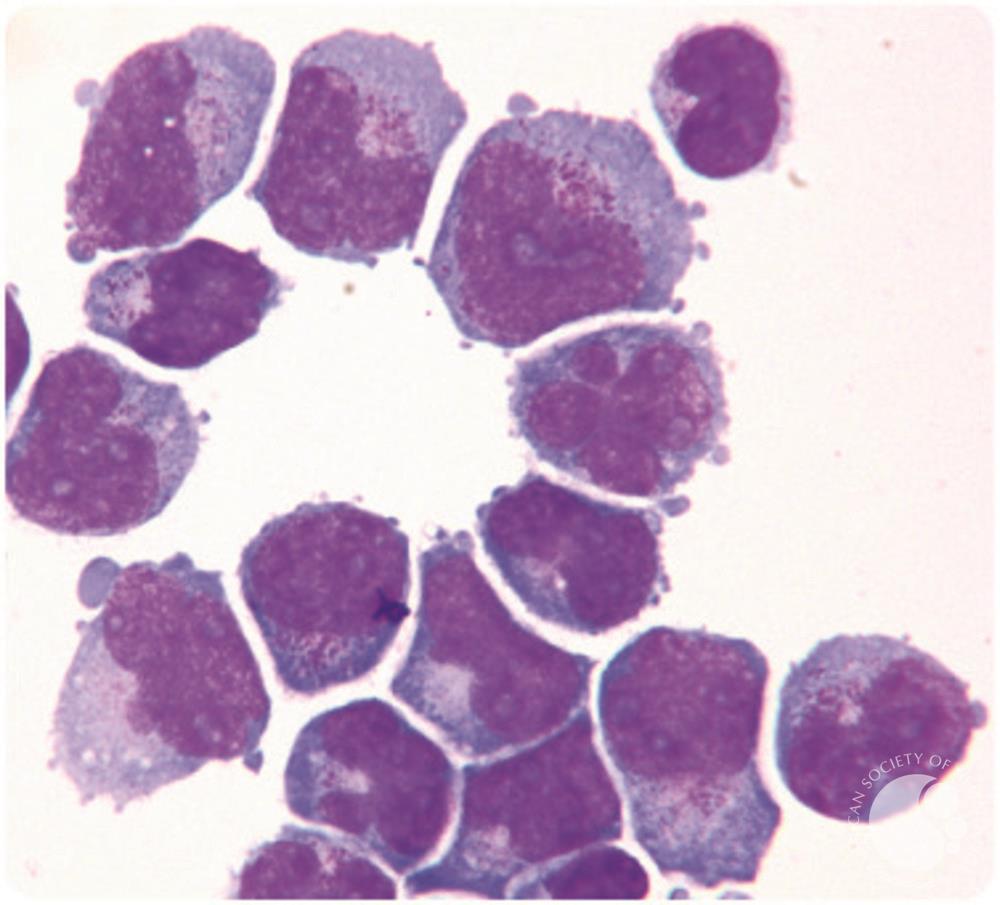
Acute myeloid leukemia (AML) is a fastgrowing cancer of the bloodforming cells in the bone marrow. Occasionally, those rogue cells slip into the cerebrospinal fluid (CSF)the clear liquid that cushions the brain and spinal cord. When that happens, doctors call it AML spinal fluid involvement or CNS (central nervous system) disease.
Definition AML cells in CSF
During a lumbar puncture, doctors examine a tiny sample of CSF. If blast cells (the immature leukemia cells) appear, the disease has crossed the bloodbrain barrier. This finding changes the treatment plan, because the medicines that work in the marrow may not reach the CSF in high enough doses.
How it differs from marrowonly AML
Bonemarrowonly AML stays mostly in the blood and marrow. When it spreads to CSF, the risk of relapse goes up, and symptoms can involve the brain or spine. Its a different battlefield, so you need different weapons.
Why it matters
Research shows that CNS involvement bumps the overall and can affect longterm survival. Knowing early means you can act fast.
Quick fact box
| Patient group | Incidence of CNS involvement |
|---|---|
| Adults with AML | 35% |
| Children with AML | 710% |
Who is at risk?
Not everyone with AML will develop CNS disease. Certain factors raise the odds, and understanding them helps you and your doctor stay vigilant.
Incidence in adults vs. children
Adults see CNS spread in roughly 35% of cases, while children face a slightly higher rateabout 710%especially those with specific genetic subtypes.
Key risk factors
- Very high whitebloodcell count at diagnosis
- Specific cytogenetic abnormalities (e.g., t(8;21) or inv16)
- Previous CNS infections or bleeding
- Having leukemia in spinal fluid child history, such as congenital leukemias
Pediatric specifics
Kids often present with subtle signslike irritability or headachesthat can be mistaken for ordinary childhood ailments. Because their bodies are still growing, early detection is even more crucial.
Risk comparison
| Risk factor | Adults | Children |
|---|---|---|
| High WBC count | Yes | Yes |
| t(8;21) cytogenetics | Moderate | High |
| Previous CNS bleed | Low | Moderate |
Spotting the signs
When AML sneaks into the CSF, the body often gives you a headsup. Recognizing those clues early can shave weeks or months off a painful diagnostic journey.
Common CNSrelated signs
- Persistent headaches that dont improve with medication
- Visual disturbancesblurry vision, double vision, or sudden loss
- Neck stiffness or pain, especially after a lumbar puncture
- Seizures, even if youve never had one before
- Weakness or numbness in the arms or legs
Overlap with other conditions
Many of these symptoms mimic migraines, sinus infections, or even stress. Thats why a simple lumbar puncture becomes the goldstandard test for confirming leukemia in spinal fluid symptoms.
Redflag symptoms
If any of the above appear suddenly, especially in someone already diagnosed with AML, its time to call the oncology team. Prompt CSF analysis can make the difference between a quick response and a delayed treatment.
Symptom checklist (downloadable)
Weve put together a printable PDF you can keep on the fridge. It lists what to watch for and a simple rating system to help you decide when to call your doctor.
How doctors confirm it
The diagnostic process isnt magicalits a series of wellstudied steps that give a clear picture of whats happening inside your central nervous system.
Lumbar puncture & CSF analysis
A thin needle is inserted between two lower back bones to draw a few milliliters of fluid. Lab technicians then look for blasts using microscopy and flow cytometry. According to the , flow cytometry can detect as few as one leukemic cell among 10,000 normal cells.
Imaging adjuncts
MRI scans of the brain and spine help spot any solid lesions or meningeal thickening that might accompany the CSF findings.
Staging & prognostic scoring
Patients are labeled CNSpositive or CNSnegative. This binary status guides how aggressive the therapy will be. Some specialists also use a CNSrisk score that incorporates WBC count, genetics, and symptom severity.
Flowcytometry guide (example image)
Imagine a colorful dot plot where a small cluster of red dotsthose represent leukemic blastsstands out against a sea of blue healthy cells. That visual cue tells the doctor you have AML in the spinal fluid.
What the numbers say
Survival statistics can feel grim, but they also show progress. Lets break down the AML in spinal fluid prognosis in plain language.
Overall survival rates
- Fiveyear overall survival for CNSnegative AML hovers around 3040%.
- For CNSpositive patients, the same fiveyear survival drops to roughly 2025%.
- When an early, aggressive intrathecal regimen is added, some studies report a boost of up to 10% in survival.
Factors that improve outlook
Early detection, highdose cytarabine that crosses the bloodbrain barrier, and timely stemcell transplant are the heavyhitters that swing the odds back in your favor.
Comparing brain vs. spinal involvement
Leukemia in brain survival rate often mirrors that of spinal fluid cases because the underlying disease biology is the same. However, isolated brain lesions (AML brain metastasis) sometimes respond better to targeted radiation, nudging survival a smidge higher.
Survival bar chart (illustrative)
Picture a simple bar chart: the CNSnegative bar reaches 38%, while the CNSpositive bar stops at 23%. Adding intrathecal therapy stretches that second bar to about 30%a visual reminder that treatment matters.
Treating AML in the CSF
Now comes the part most people dreadtreatment options. The good thing is that modern oncology has a toolbox full of weapons, each with its own strengths and sideeffects.
Intrathecal chemotherapy
These are drugs that go directly into the CSF via a lumbar puncture. The classic combo includes:
- Cytarabine
- Methotrexate
- Hydrocortisone (to reduce inflammation)
Doses are given twice a week for the first few weeks, then taper off. The direct delivery bypasses the bloodbrain barrier, hitting the leukemic cells where they hide.
Systemic therapy with CNSpenetrating agents
Highdose cytarabine, FLT3 inhibitors (for patients with FLT3 mutations), and newer targeted agents can cross into the CSF at therapeutic levels. The NCCN 2024 guidelines recommend adding these agents when CSF blasts are detected.
Radiation therapy
Wholebrain or craniospinal irradiation is reserved for cases where blasts form solid masses or when intrathecal chemo alone isnt enough. Its effective but can cause fatigue and longterm cognitive changes, so doctors weigh the benefits carefully.
Stemcell transplant & clinical trials
Allogeneic hematopoietic stemcell transplant (alloHSCT) offers the best chance for a durable cure, especially for younger patients or those with highrisk genetics. Many ongoing clinical trials explore novel agents that may further improve outcomescheck for the latest.
Treatment comparison table
| Approach | Pros | Cons | Typical Response Rate |
|---|---|---|---|
| Intrathecal chemo | Targets CSF directly; minimal systemic toxicity | Requires repeated lumbar punctures; neurotoxicity possible | 6070% |
| Systemic CNSpenetrating drugs | Treats both marrow and CNS simultaneously | Higher systemic sideeffects | 5565% |
| Radiation | Rapid control of bulky CNS disease | Potential longterm cognitive effects | 70% (when combined with chemo) |
| AlloHSCT | Potential cure | Transplantrelated mortality, graftvshost disease | 4555% (longterm) |
Balancing benefits & risks
Every treatment brings a tradeoff. Lets break it down so you can have an honest conversation with your care team.
Potential benefits
- Higher chances of achieving complete remission in the CNS
- Reduced risk of relapse, which translates into longer survival
- Improved quality of life when symptoms like headaches or seizures subside
Risks & toxicities
- Neurotoxicity from intrathecal drugsthink tingling or temporary weakness
- Infections related to repeated lumbar punctures
- Longterm cognitive effects if radiation is used
- Transplantrelated complications (if you go that route)
Decisionmaking framework
Ask yourself these questions:
- How urgent is my CNS disease? (Rapid symptoms aggressive approach)
- Whats my overall health and age? (Younger patients often tolerate transplant better)
- Do I have support for frequent hospital visits? (Intrathecal therapy can be demanding)
- Am I comfortable with potential sideeffects? (Weigh quality of life vs. survival benefit)
Case study: Two different paths
Emily, a 28yearold mother, chose intrathecal chemo plus a reducedintensity transplant. Shes now two years diseasefree and enjoys playing with her kids. Jake, 55, opted for radiation plus systemic chemo; while his CNS disease cleared quickly, he now deals with mild memory lapses. Both stories highlight that the right choice is personal.
Living with AML CNS involvement
Beyond the medical jargon, theres a real human storyhow you navigate daily life, emotions, and practical concerns.
Psychological impact & coping
Being told you have leukemic cells in your spinal fluid can feel like a punch to the gut. Counseling, peersupport groups, and mindfulness practices have helped many patients stay resilient. The AML Foundation hosts online forums where you can share experiences and hear from others whove walked this road.
Practical tips for daily life
- Keep a symptom diarynote any new headaches, vision changes, or tingling.
- Plan your lumbar puncture dates ahead; arrange rides and backup childcare if needed.
- Stay hydrated and maintain a balanced diet; nutrition supports both recovery and immune health.
- Ask your pharmacist about ways to manage sideeffects like nausea or fatigue.
Trusted resources
Organizations such as , the , and HealthTree provide patient guides, financial assistance tips, and uptodate research news.
My CNSAML Care Plan template
Weve created a printable checklist that includes appointment tracking, medication schedules, and space for notes on sideeffects. Download it, print it, and keep it on the fridge so you never miss a step.
Bottom line & next steps
Finding AML cells in the spinal fluid adds a layer of complexity, but its far from a hopeless situation. Early detection, a tailored mix of intrathecal and systemic therapy, andwhen appropriatestemcell transplant can meaningfully improve the AML in spinal fluid prognosis. Remember, youre not alone; lean on your medical team, engage with trusted support groups, and use the tools weve shared to stay informed and proactive.
Whats your biggest question about AML spinal fluid involvement? Have you or a loved one navigated this journey? Share your thoughts in the commentsyour story might be the beacon another reader needs.
FAQs
What does it mean when AML is found in the spinal fluid?
It indicates that leukemic blasts have crossed the blood‑brain barrier and are present in the cerebrospinal fluid, classifying the disease as CNS‑positive AML.
How is AML spinal fluid involvement diagnosed?
Diagnosis is made by performing a lumbar puncture and analyzing the CSF for blasts using microscopy and flow cytometry; imaging (MRI) may be added for further assessment.
What are the common symptoms of AML in the CSF?
Patients may experience persistent headaches, visual disturbances, neck stiffness, seizures, or weakness/numbness in the limbs.
What treatment options are available for AML spinal fluid disease?
Treatment typically includes intrathecal chemotherapy (cytarabine, methotrexate, hydrocortisone), systemic CNS‑penetrating drugs, radiation for bulky disease, and, when appropriate, allogeneic stem‑cell transplantation.
How does CNS involvement affect the prognosis of AML?
CNS involvement raises relapse risk and lowers overall survival (≈20‑25 % 5‑year survival) compared with CNS‑negative AML, but early aggressive therapy can improve outcomes by up to 10 %.