Why Sleep Matters
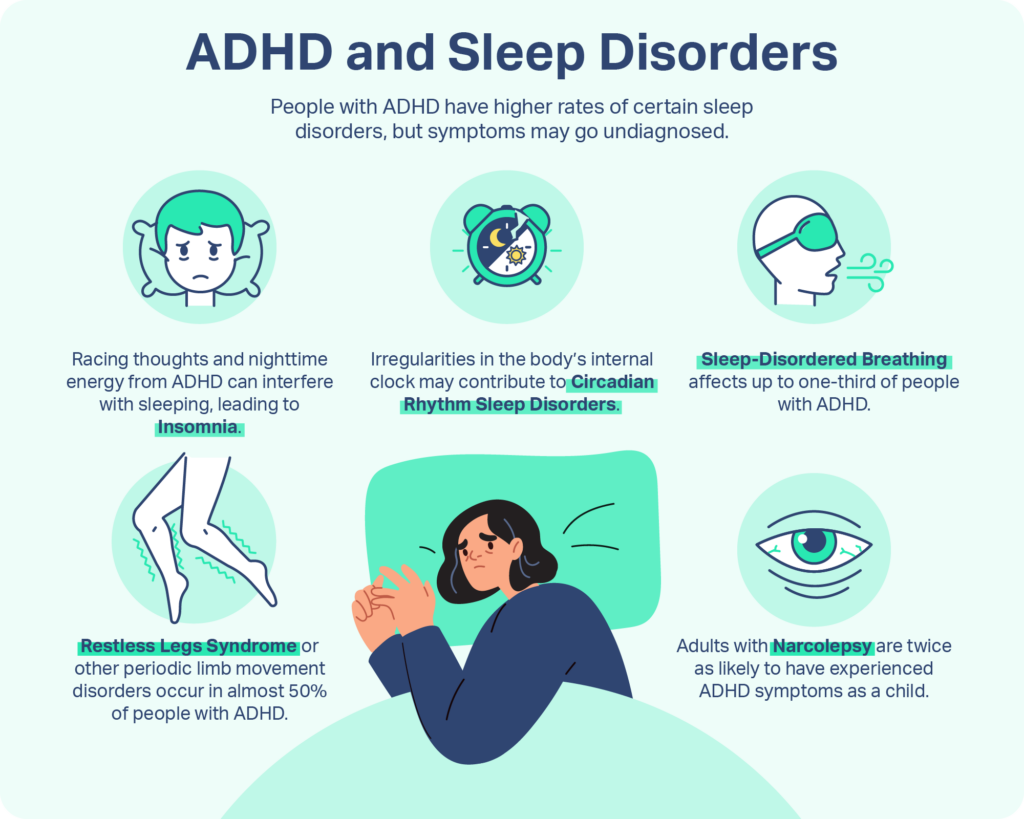
Whats the link between ADHD and insomnia?
ADHD isnt just about staying up late on a video game console. The brain of an ADHD insomnia child often runs on overdrive, producing higher levels of the neurotransmitter dopamine that keep the mind wired. Add in delayed melatonin release, anxiety about the dark, and some medications that can be stimulating, and you have a perfect storm for sleeplessness.
How common is it?
Recent research from the shows that up to 70% of children with ADHD experience frequent sleep disturbances. That means if you have three kids with ADHD, chances are at least two of them are battling bedtime night after night.
Sleep Needs
How much sleep does a child with ADHD need?
Agespecific guidelines dont change for ADHD, but the reality is many kids fall short. Heres a quick snapshot:
| Age | Recommended Hours | Typical Hours for ADHD Kids |
|---|---|---|
| 512years | 911hours | 79hours |
| 1317years | 810hours | 68hours |
Missing even a single hour can amplify hyperactivity, mood swings, and those dreaded ADHD bedtime meltdowns. So think of sleep as the quiet reset button that helps the brain run smoother the next day.
NightTime Challenges
Why wont my ADHD child sleep alone?
Separation anxiety isnt exclusive to toddlers. An ADHD child wont sleep alone often because the mind is racing, and the safety of a parents presence feels like a calming anchor. The solution isnt to force independence overnight; its to gradually build confidence.
What causes an ADHD child waking up at night?
Nighttime awakenings can stem from:
- Restless legs or buzzing sensations.
- Sudden spikes in cortisol (the stress hormone).
- Medications wearing off too early, leaving a rebound of hyperactivity.
How to navigate bedtime battles without a meltdown?
Think of bedtime as a negotiation, not a war. Offer clear choices (Do you want the blue nightlight or the green one?) and keep the routine predictable. Consistency lets the brain anticipate sleep time, reducing the odds of an ADHD bedtime battle.
Natural Sleep Aids
Can a natural sleep aid help my ADHD child?
Yeswhen used wisely. A natural sleep aid for ADHD child such as lowdose melatonin (0.5mg to 1mg) can signal the brain that its night. Magnesium glycinate and a warm cup of chamomile tea are also gentle options that promote relaxation without the grogginess of prescription meds.
Safety first: what the experts say
According to a systematic review in , melatonin is generally safe for children when monitored by a pediatrician. Always start with the lowest possible dose and track any changes.
Simple bedtime routine (the 30minute countdown)
- 30 minutes before lights out: Turn off screens, dim the lights, and start a calming activity (reading or a short puzzle).
- 20 minutes: Offer a warm drinkmilk with a pinch of turmeric or chamomile tea.
- 10 minutes: Practice a quick breathing exerciseinhale for four counts, hold for four, exhale for four.
- 0 minutes: Tuck in, use a nightlight if needed, and say a short, positive affirmation.
This predictable flow signals the brain that its time to wind down, reducing the chance that an ADHD child waking up at night becomes a nightly ritual.
Behavioral Strategies
What is the twosession sleep program?
A recent CHADD study found that a brief, 2session behavioral programcovering sleep hygiene, stimulus control, and a bedtime reward chartimproved sleep latency by an average of 30minutes for 78% of participants.
How does CBTI work for kids?
CognitiveBehavioral Therapy for Insomnia (CBTI) teaches children to recognize thoughts that keep them awake and replace them with calming imagery. Sessions are short (3045minutes) and can be done by a trained psychologist or even a telehealth therapist.
Positivereinforcement bedtime chart
Create a simple chart with stickers for went to bed on time and stayed in bed all night. Celebrate small wins with a weekend activity rather than a sugary treat. Over time, the child begins to associate bedtime with positive outcomes.
Sample Bedtime Chart
| Day | In Bed by 9pm | Stayed Asleep | Sticker Earned |
|---|---|---|---|
| Mon | |||
| Tue |
Medication Options
When is medication considered?
If natural methods and behavioral strategies dont move the needle after 46 weeks, it may be time to discuss sleep medication for child with ADHD with your pediatrician. The goal is always to use the lowest effective dose.
Firstline vs. secondline options
- Lowdose melatonin: Often the first step, especially for delayed sleep phase.
- Clonidine: An antihypertensive that can calm hyperactivity at night; watch for morning drowsiness.
- Guanfacine: Helpful for both daytime ADHD symptoms and nighttime sleep, but requires careful titration.
For families also managing other pediatric concerns, resources on related conditions can be helpful; for example, guidance on infant apnea may be relevant if breathing issues are suspected.
Balancing benefits and risks
Every medication carries potential sideeffects. For example, clonidine may cause dry mouth or low blood pressure, while guanfacine can cause fatigue. Thats why a collaborative conversation with a sleepspecialized pediatrician is essential.
DecisionTree: Is Medication Right for My Child?
| Step | Question | Action |
|---|---|---|
| 1 | Are natural and behavioral strategies tried for 4 weeks? | Yes Move to step 2; No Continue with those strategies. |
| 2 | Is sleep latency >30minutes or nighttime waking >2times/week? | Yes Discuss medication options; No Reevaluate routine. |
Professional Help
Who should I see?
A pediatric sleep specialist can run a polysomnography (sleep study) if sleep apnea is suspected. A child psychologist trained in ADHD can guide CBTI, while an ADHDexperienced pediatrician can finetune any medication.
Trusted resources
Organizations like , the Sleep Health Foundation, and ADDitude Magazine provide evidencebased articles, webinars, and support groups. Theyre great places to stay updated on the latest research.
Success Stories
Sams 4week turnaround
Sam, an 8yearold with ADHD, used to fight bedtime nightly and wake up at 2am crying. After implementing a consistent 30minute winddown, a lowdose melatonin supplement, and a sticker chart, his parents reported that Sam now falls asleep within 15minutes and stays asleep until sunrise Most parents of kids with ADHD have tried everything from a warm bath to a bedtime story, only to end up with a child who still refuses to drift off. The truth is that ADHD can turn a normal nights rest into a battlefield, but with the right mix of habits, natural aids, and professional guidance, you can help your child finally catch the Zs they deserve. ADHD isnt just about staying up late on a video game console. The brain of an ADHD insomnia child often runs on overdrive, producing higher levels of the neurotransmitter dopamine that keep the mind wired. Add in delayed melatonin release, anxiety about the dark, and some medications that can be stimulating, and you have a perfect storm for sleeplessness. Recent research shows that up to 70% of children with ADHD experience frequent sleep disturbances. That means if you have three kids with ADHD, chances are at least two of them are battling bedtime night after night. Agespecific guidelines dont change for ADHD, but the reality is many kids fall short. Heres a quick snapshot: Missing even a single hour can amplify hyperactivity, mood swings, and those dreaded ADHD bedtime meltdowns. So think of sleep as the quiet reset button that helps the brain run smoother the next day. Separation anxiety isnt exclusive to toddlers. An ADHD child wont sleep alone often because the mind is racing, and the safety of a parents presence feels like a calming anchor. The solution isnt to force independence overnight; its to gradually build confidence. Nighttime awakenings can stem from: Think of bedtime as a negotiation, not a war. Offer clear choices (Do you want the blue nightlight or the green one?) and keep the routine predictable. Consistency lets the brain anticipate sleep time, reducing the odds of an ADHD bedtime battle. Yeswhen used wisely. A natural sleep aid for ADHD child such as lowdose melatonin (0.5mg to 1mg) can signal the brain that its night. Magnesium glycinate and a warm cup of chamomile tea are also gentle options that promote relaxation without the grogginess of prescription meds. According to a systematic review, melatonin is generally safe for children when monitored by a pediatrician. Always start with the lowest possible dose and track any changes. If a child has other medical concernslike a history of anemia or respiratory eventstalking with a pediatrician who understands infant apnea and related sleep issues can be helpful. This predictable flow signals the brain that its time to wind down, reducing the chance that an ADHD child waking up at night becomes a nightly ritual. A recent CHADD study found that a brief, 2session behavioral programcovering sleep hygiene, stimulus control, and a bedtime reward chartimproved sleep latency by an average of 30minutes for 78% of participants. CognitiveBehavioral Therapy for Insomnia (CBTI) teaches children to recognize thoughts that keep them awake and replace them with calming imagery. Sessions are short (3045minutes) and can be done by a trained psychologist or even a telehealth therapist. Create a simple chart with stickers for went to bed on time and stayed in bed all night. Celebrate small wins with a weekend activity rather than a sugary treat. Over time, the child begins to associate bedtime with positive outcomes. If natural methods and behavioral strategies dont move the needle after 46 weeks, it may be time to discuss sleep medication for child with ADHD with your pediatrician. The goal is always to use the lowest effective dose. Every medication carries potential sideeffects. For example, clonidine may cause dry mouth or low blood pressure, while guanfacine can cause fatigue. Thats why a collaborative conversation with a sleepspecialized pediatrician is essential. A pediatric sleep specialist can run a polysomnography (sleep study) if sleep apnea is suspected. A child psychologist trained in ADHD can guide CBTI, while an ADHDexperienced pediatrician can finetune any medication. Organizations like the Sleep Health Foundation and ADDitude Magazine provide evidencebased articles, webinars, and support groups. Theyre great places to stay updated on the latest research. Sam, an 8yearold with ADHD, used to fight bedtime nightly and wake up at 2am crying. After implementing a consistent 30minute winddown, a lowdose melatonin supplement, and a sticker chart, his parents reported that Sam now falls asleep within 15minutes and stays asleep until sunrise. It felt like we finally found the right combination, his mom says, smiling. Hearing that another family walked the same path can be a huge relief. If you have a story, consider reaching out to a local ADHD support groupyour experience could be the lighthouse another parent needs. Living with an ADHD insomnia child can feel like navigating a stormy sea, but with a blend of solid sleep hygiene, gentle natural aids, proven behavioral tactics, and, when necessary, carefully chosen medication, calm waters are within reach. Start smallpick one habit from the 30minute countdown and stick with it for a week. Track the changes, celebrate the victories, and remember youre not alone. If you have questions or want to share your own bedtime triumphs, feel free to reach out. Together we can turn sleepless nights into peaceful mornings. Children with ADHD frequently experience insomnia due to overactive brain activity with elevated dopamine levels, delayed melatonin release, anxiety, and some stimulant medications contributing to difficulties falling and staying asleep. A consistent, calming bedtime routine including turning off screens 30 minutes before bed, dimming lights, quiet reading, warm drinks like chamomile tea, and breathing exercises can help signal the brain to wind down for sleep. Low-dose melatonin (0.5–1 mg) and magnesium glycinate are generally safe when used under pediatrician supervision and can help regulate sleep cycles without significant grogginess or side effects. If natural and behavioral approaches have been tried for 4–6 weeks without improvement and sleep latency exceeds 30 minutes or waking occurs multiple times per week, discussing medication such as low-dose melatonin, clonidine, or guanfacine with a doctor is advised. Night awakenings can be caused by restless legs, stress hormone spikes, or medication wearing off. Maintaining a consistent bedtime routine, creating a sleep-friendly environment, and gradual comfort techniques help reduce awakenings and anxiety.Why Sleep Matters
Whats the link between ADHD and insomnia?
How common is it?
Sleep Needs
How much sleep does a child with ADHD need?
Age Recommended Hours Typical Hours for ADHD Kids 512years 911hours 79hours 1317years 810hours 68hours NightTime Challenges
Why wont my ADHD child sleep alone?
What causes an ADHD child waking up at night?
How to navigate bedtime battles without a meltdown?
Natural Sleep Aids
Can a natural sleep aid help my ADHD child?
Safety first: what the experts say
Simple bedtime routine (the 30minute countdown)
Behavioral Strategies
What is the twosession sleep program?
How does CBTI work for kids?
Positivereinforcement bedtime chart
Sample Bedtime Chart
Day In Bed by 9pm Stayed Asleep Sticker Earned Mon Tue Medication Options
When is medication considered?
Firstline vs. secondline options
Balancing benefits and risks
DecisionTree: Is Medication Right for My Child?
Step Question Action 1 Are natural and behavioral strategies tried for 4 weeks? Yes Move to step 2; No Continue with those strategies. 2 Is sleep latency >30minutes or nighttime waking >2times/week? Yes Discuss medication options; No Reevaluate routine. Professional Help
Who should I see?
Trusted resources
Success Stories
Sams 4week turnaround
Why sharing matters
Conclusion
FAQs
Why do children with ADHD often have trouble sleeping?
What bedtime routines help an ADHD child sleep better?
Are natural sleep aids safe for children with ADHD?
When should medication be considered for an ADHD child's insomnia?
How can parents manage nighttime awakenings in children with ADHD?