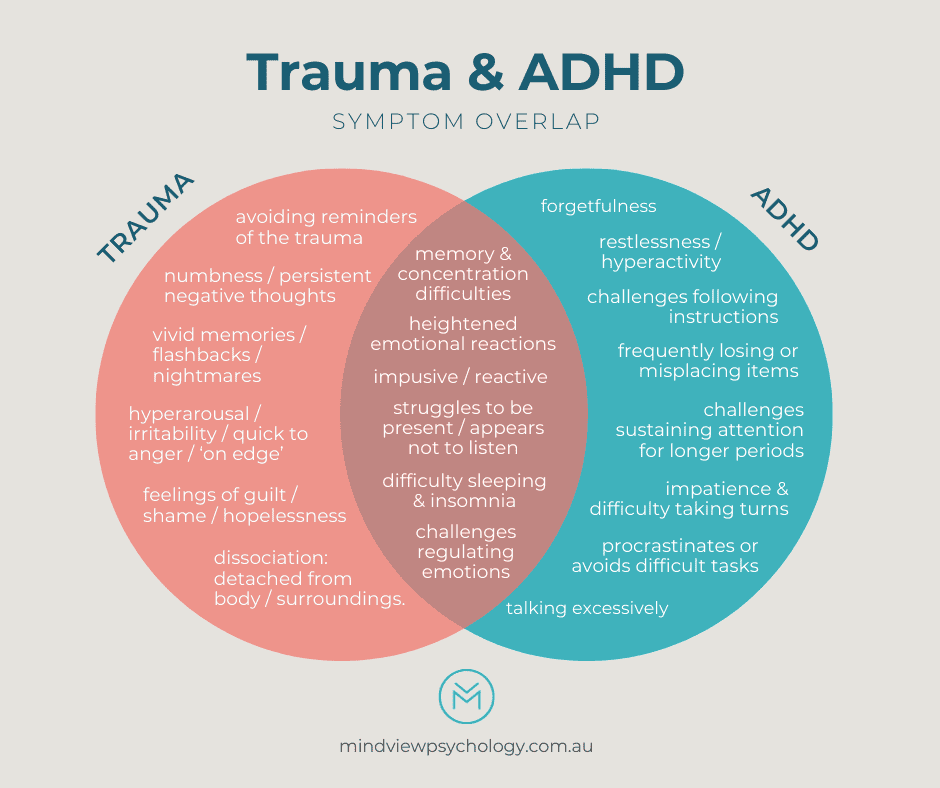
How PTSD Shows Up
What are the hallmark PTSD symptoms for women?
Posttraumatic stress disorder often shows up in four big clusters. For women, the emotional tone can be a little different, with more focus on mood and relationships.
Intrusive memories
Flashbacks, vivid nightmares, or sudden, unwanted thoughts about the traumatic event can feel like a broken record that just wont stop. Its that gutwrenching feeling that something terrible is happening again, even when youre safe at home.
Avoidance behaviours
You might catch yourself steering clear of certain places, people, or even conversations that remind you of the trauma. Its a survival tactic, but over time it can shrink your world.
Negative changes in mood & cognition
Feelings of shame, guilt, or an empty void inside are common. Women often report a deep sense of selfcriticism or a feeling that theyve lost who they once were.
Hyperarousal
Being jumpy, having trouble sleeping, or feeling constantly onalert are classic signs. The body stays in fightorflight mode, even when theres no danger. If sleep issues are prominent, consider reading about practical ADHD sleep disorder strategies many grounding and sleep-hygiene techniques overlap and can help reduce hyperarousal symptoms.
How do these differ from the classic 5symptom list?
| Standard PTSD (NIH) | WomenSpecific Presentation |
|---|---|
| Intrusive memories | Often paired with intense guilt or shame |
| Avoidance | More avoidance of relational triggers (e.g., family gatherings) |
| Negative mood/cognition | Higher rates of depressive symptoms and selfblame |
| Hyperarousal | Sleep disturbances are especially common |
| Area of functioning | Impact on parenting and intimate relationships is pronounced |
What are the 7 core PTSD symptoms and why they matter for women?
Sometimes youll see a shorter list of seven symptomsbasically the four clusters broken down a bit more. They include intrusive memories, avoidance, negative thoughts, guilt, emotional numbness, hypervigilance, and sleep problems. Knowing each helps you spot patterns in daily life, like why you might feel off at work or with your kids.
Complex PTSD Explained
What makes Complex PTSD (CPTSD) different?
While regular PTSD often follows a single traumatic event, CPTSD usually stems from prolonged or repeated abusethink ongoing domestic violence or chronic childhood neglect. This adds three extra symptom groups: affect dysregulation, a persistent negative selfconcept, and severe interpersonal problems.
What are the 17 symptoms of CPTSD, and which show up most in women?
Below is the full list. In women, the following five tend to surface most often:
- Chronic shame or guilt
- Dissociation (feeling detached from reality)
- Intense fear of abandonment
- Difficulty trusting others
- Selfharm or suicidal thoughts
Commonly, the other twelve symptomslike recurring nightmares, emotional numbness, or sudden anger burstsround out the picture.
A realworld glimpse
Anna (name changed) shared that after years of an abusive partnership, she found herself freezing during arguments, even when the conflict was harmless. She described the nighttime flashbacks as movie scenes I couldnt pause, and the lingering guilt made her think she deserved the abuse. Hearing stories like Annas reminds us that symptoms arent abstracttheyre lived, messy, and deeply human.
Daily Life Impact
How does PTSD affect emotional and mental wellbeing?
Beyond the core symptoms, women often wrestle with secondary issuesdepression, anxiety, and a persistent sense of being broken. These mood swings can strain friendships, make parenting feel impossible, and erode selfesteem.
What physical signs might show up?
Headaches, stomachaches, and chronic fatigue are surprising but common. The body holds onto trauma the same way the mind does, turning stress into real, tangible pain.
How does it show up at work or school?
Concentration lapses, brain fog, and the need to leave a meeting early because of a flashback are all too real. You might notice a drop in performance or avoidance of deadlines, not because youre lazy, but because the brain is busy fighting invisible battles.
Quick selfcheck: Am I letting PTSD run my day?
Answer yes to any of these five questions, and consider reaching out for help:
- Do I wake up feeling onedge at least three times a week?
- Do I avoid places or people because they remind me of a trauma?
- Do I feel overwhelming guilt or shame for no clear reason?
- Do I have trouble sleeping more than five nights a month?
- Do I feel detached from my emotions or from people I love?
Getting Diagnosed
When should a woman seek professional help?
If symptoms linger longer than a month and interfere with daily functioningwork, relationships, sleepits time to talk to a mentalhealth professional. Remember, you deserve care, not judgment.
How do clinicians assess PTSD in women?
Therapists often use validated tools like the PTSD Checklist for DSM5 (PCL5) or the ClinicianAdministered PTSD Scale (CAPS5). These questionnaires are gendersensitive, meaning they probe relational and emotional nuances that women commonly experience.
Common myths that delay diagnosis
Myth #1: Its just stress. Stress feels bad, but it doesnt cause flashbacks or persistent avoidance. , PTSD is a distinct medical condition with specific diagnostic criteria.
Myth #2: Ill get over it on my own. While selfcare helps, professional treatment dramatically increases the odds of lasting recovery.
Treatment Options
What are the firstline therapies?
Two approaches dominate the evidence base:
- TraumaFocused Cognitive Behavioral Therapy (TFCBT) Structured, goaloriented, and often adapted for womens experiences of relational trauma.
- Eye Movement Desensitization & Reprocessing (EMDR) Uses bilateral stimulation to reprocess memories; many women find it less retraumatizing than prolonged exposure.
Is medication part of the picture?
Selective serotonin reuptake inhibitors (SSRIs) like sertraline and paroxetine are FDAapproved for PTSD. For women, its worth discussing hormonal interactionsespecially if youre on birth control or navigating menopause. notes that medication can reduce hyperarousal and improve sleep, paving the way for therapy to work more effectively.
Complementary & selfcare strategies
Mindbody practices such as yoga, deepbreathing, and progressive muscle relaxation have growing evidence for reducing anxiety and intrusive thoughts. Support groupsespecially womenonly circlesprovide a safe space for sharing without judgment.
Building a personalized recovery plan
Heres a simple fourweek template you can tweak:
- Week 1 Grounding & Safety: Practice the 54321 grounding technique daily.
- Week 2 Professional Guidance: Book a TFCBT or EMDR session; discuss medication options if needed.
- Week 3 Body Awareness: Add 15 minutes of yoga or a walk in nature three times a week.
- Week 4 Community Connection: Join a local or online womenfocused PTSD group, share a brief story, and listen.
Adjust the pace as you feel comfortablerecovery isnt a race. If attention or focus problems make it hard to stick with plans, see strategies for managing overlaps between trauma and attention differences in resources on the ADHD trauma link.
Frequently Asked Questions
What are the 5 signs of PTSD in women?
Intrusive memories, avoidance, persistent negative mood, hypervigilance, and physical reactions like sleep problems or irritability. If any of these linger beyond a month, seek help.
How do I know if I have Complex PTSD?
Beyond the core PTSD symptoms, look for chronic shame, relational instability, emotional dysregulation, and a persistent sense that the trauma will never end. These often stem from prolonged abuse.
Can PTSD symptoms disappear without treatment?
Its rare. Symptoms may lessen a bit over time, but without targeted support they often worsen, affecting health, relationships, and overall quality of life.
Whats the fastest way to get relief?
Grounding techniques (like the 54321 method), a brief therapistguided exposure session, andif appropriatean SSRI starter dose can bring noticeable relief within weeks.
Are there any genderspecific risks?
Women with PTSD are more prone to cooccurring depression, anxiety disorders, chronic pain, and higher rates of selfharm. Understanding these risks helps clinicians tailor treatment.
Practical Resources & Where to Find Help
Trusted medical sites
For deeper reading, consider the Office on Womens Health, the NHS, and the Mayo Cliniceach offers evidencebased overviews of PTSD in women.
Crisis hotlines & support groups
The national suicide prevention line (988 in the U.S.) is free, 24/7. For womenspecific peer support, look for the Womens PTSD Network or local traumainformed groups.
Apps & tools for tracking symptoms
Apps like PTSD Coach or MyStrength let you log flashbacks, mood swings, and sleep quality, creating a visual picture you can share with your therapist.
Conclusion
Women with PTSD often face a mix of intrusive memories, mood swings, and a constant feeling of being onedge that sneaks into every corner of daily life. Recognizing the full spectrumfrom the classic fivesymptom checklist to the expansive 17point list of Complex PTSDmeans you or a loved one can get the right help sooner rather than later. Evidencebased therapies, thoughtful medication, and supportive selfcare strategies can turn the tide, letting you reclaim space for peace, connection, and hope.
If you found this guide useful, consider downloading the printable Womens PTSD Symptom Tracker below and share it with anyone who might need a gentle nudge toward help. You deserve support, and youre not alone on this journey.
FAQs
What are the most common women PTSD symptoms?
Typical symptoms include intrusive memories, avoidance of trauma reminders, persistent negative mood, hyper‑arousal (such as sleep problems), and physical reactions like headaches or fatigue.
How can I tell if I have Complex PTSD?
Complex PTSD adds chronic shame, difficulty trusting others, intense fear of abandonment, emotional dysregulation, and a persistent negative self‑concept to the core PTSD symptoms.
Can medication help women with PTSD symptoms?
Yes. SSRIs such as sertraline or paroxetine are FDA‑approved for PTSD and can reduce hyper‑arousal and improve sleep, making psychotherapy more effective.
What self‑care practices are effective for managing PTSD symptoms?
Grounding techniques (e.g., the 5‑4‑3‑2‑1 method), yoga, deep‑breathing, progressive muscle relaxation, and regular exercise are proven to lower anxiety and intrusive thoughts.
Where can I find women‑specific PTSD support groups?
Look for local women‑only trauma‑informed groups, online communities like the Women’s PTSD Network, or ask your therapist for referrals to gender‑sensitive peer support.