Swelling below the knee can feel like an unwelcome surprisetight, heavy, sometimes even painful. In most cases, it's just fluid hanging out where it shouldn't, but on the flip side, it can also be a whisper from your body that something bigger is going on. Below, we'll walk through the most common reasons, tell you when to hit the panic button, and share easy-to-try steps that might bring you relief.
Quick Check Guide
Red Flag Symptoms
If any of these pop up, don't wait: call your doctor or head to urgent care.
- Sudden, severe pain with warmth or rednesscould be a deep vein clot.
- Shortness of breath, chest discomfort, or rapid heartbeatpossible heart failure-related edema.
- Fever, chills, or a rapidly spreading rashsigns of infection like cellulitis.
- Swelling that appears only on one leg and worsens quickly.
Simple Self-Assessment Questions
Before you dive into research, ask yourself:
- Is the swelling only on one side? (If yes, see One-Leg Swelling Reasons below.)
- Does it get worse after a long day of standing or sitting? (Gravity-dependent edema is common.)
- Do you feel any pain, throbbing, or a tight sensation?
- Have you started a new medication or increased your salt intake recently? For instance, calcium channel blockers can cause swelling, similar to issues related to hand swelling.
Common Medical Causes
Fluid Retention & Peripheral Edema
Our bodies love to keep a delicate balance of fluids. When that balance tipsoften because of too much sodium, hormonal shifts, or simply standing for hoursextra fluid leaks into the tissue around the ankle and shin. This is called peripheral edema and usually improves with elevation and movement.
Venous Disorders
Veins in the lower leg are like highways for blood returning to the heart. If the valves in those highways get sloppy (chronic venous insufficiency) or if a clot blocks the road (deep vein thrombosis, or DVT), blood pools, causing swelling that can be both painful and dangerous.
Lymphatic Issues
The lymphatic system is the body's drainage network. When it's damagedsay after surgery, radiation, or a traumatic injurylymph fluid builds up, leading to lymphedema. Unlike regular edema, lymphedema often feels spongy and may be harder to reduce with simple elevation.
Organ-Related Causes
When the heart, kidneys, or liver struggle, they can't keep fluid where it belongs.
- Heart failure: The heart can't push blood efficiently, so pressure backs up into the leg veins.
- Kidney disease: Poor filtration leads to low albumin levels, which pulls fluid into the legs.
- Liver cirrhosis: Scar tissue raises pressure in the portal vein, spilling fluid into the abdomen and legs.
Medication-Induced Swelling
Some drugs love to hold onto water. Calcium channel blockers (often prescribed for high blood pressure), nonsteroidal anti-inflammatory drugs (NSAIDs), and steroids are frequent culprits. If you've recently started any of these, a quick chat with your prescriber might be in order.
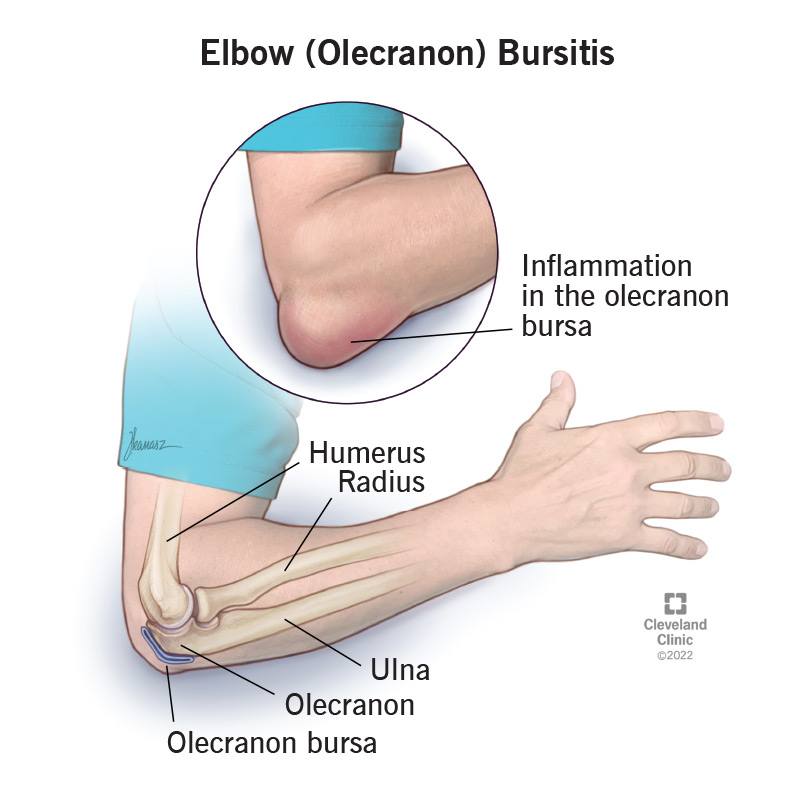
Injuries & Local Inflammation
A twisted ankle, a minor fracture, or even a nasty bite can trigger inflammation. The body sends extra blood and fluid to the scene, which makes the area look puffy and feel sore. Usually, this type of swelling eases as the injury heals.
Elderly Age Insights
Why Older Adults Get Swollen Legs More Often
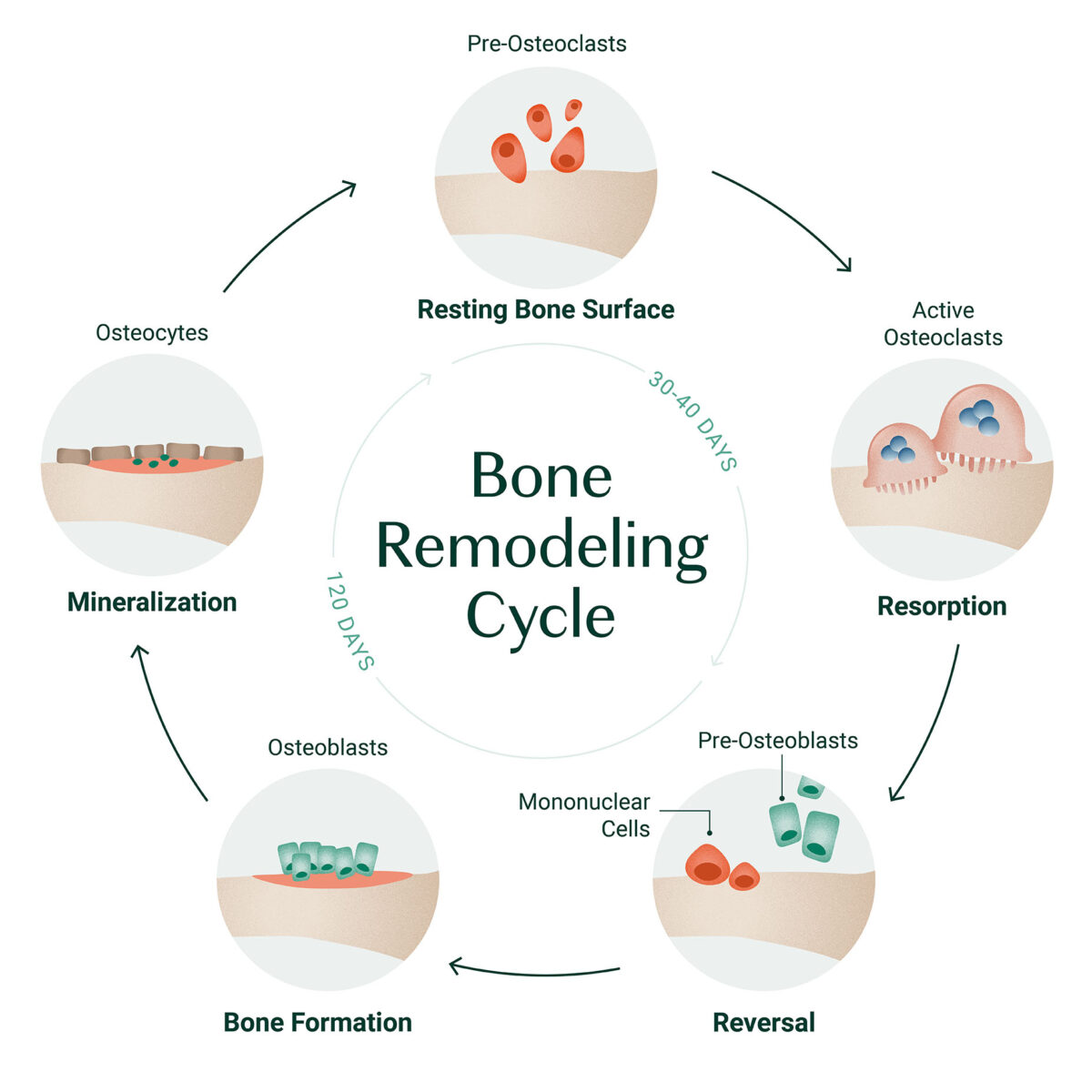
Age brings a few built-in challenges: veins get less elastic, mobility often drops, and the number of prescriptions climbs. All of these factors make fluid retention a regular guest for many seniors. Maintaining bone health through exercises like those for osteoporosis exercises can also help overall physical resilience.
Top Three Culprits in the Elderly
- Venous insufficiency: Weak valves let blood pool.
- Congestive heart failure: The heart's pump power wanes.
- Medication side effects: Diuretics help, but many other meds add water.
Caregiver Tips That Actually Work
Even simple moves can keep swelling at bay:
- Elevate: Prop the legs on pillows for 15-20 minutes a few times a day.
- Compression stockings: Choose a light to moderate pressure (15-20 mmHg) for daily wear.
- Gentle exercise: Ankle pumps, seated marching, or short walks keep the blood flowing.
Take Mrs. Lee's story, for instance. At 78, she noticed her shins puffing up each evening. By adding a 5-minute leg-raise routine before bed, her swelling dropped dramatically within a week.
FAQs
What are the most common reasons for swelling below the knee?
Typical causes include peripheral edema from fluid retention, chronic venous insufficiency, deep‑vein thrombosis (DVT), lymphedema, medication side‑effects, and injuries that trigger local inflammation.
When should swelling in one leg be considered an emergency?
If the swelling appears suddenly, is painful, warm, red, or accompanied by shortness of breath, seek medical care right away—these can signal a DVT or infection.
Can everyday habits like diet and activity influence leg swelling?
Yes. High‑sodium meals, prolonged sitting or standing, and lack of movement can worsen fluid buildup. Regular calf exercises, leg elevation, and a low‑salt diet help prevent swelling.
Are compression stockings safe for everyone with swollen legs?
Compression stockings are helpful for many people, but the pressure level should match the underlying cause. Those with severe arterial disease or certain skin conditions should consult a physician before using them.
What simple home measures can reduce swelling from the knee down?
Elevate the legs above heart level for 15‑20 minutes several times a day, wear appropriate compression, stay hydrated, limit salt, and perform ankle‑pump exercises every hour.