Bottom line: if youve had a uvulopalatopharyngoplasty (UPPP) or a simple uvula removal, you may notice changes that linger for months or even yearsthings like a dryer throat, a slightly different voice, or occasional swallowing quirks. Knowing which of those changes are normal, which might need a doctor's attention, and how to cope with them can turn a scary postop period into a manageable part of life.
Why it matters: you're probably here because you want clear answers fast. This article walks you through the typical recovery timeline, the most common longterm side effects, diet tips, costs, and practical ways to keep the new normal comfortable. Think of it as a friendly chat with someone who's been through it and wants to share what really helped. If you're also dealing with persistent throat symptoms like difficulty swallowing, see our guide on difficulty swallowing symptoms for practical signs to watch for and when to seek help.
Typical Recovery Timeline
When do normal side effects fade?
Right after surgery, most people feel sore, swollen, and a bit gagprone. That's the body's immediate response to tissue trauma. In the first two weeks, pain usually eases with prescribed meds, and you can expect a lot of throat clearing. By the end of the first month, bleeding subsides, and many start noticing a less nasal voice.
When should you start worrying about longterm problems?
If symptoms stick around beyond three monthsespecially persistent dry throat, chronic nasal regurgitation, or a voice that just won't settleyou're entering the longterm zone that deserves a closer look. Around that point, it's wise to check in with your ENT surgeon or a speechlanguage pathologist.
QuickReference Recovery Table
| Time after surgery | Common symptom | Usually resolves? |
|---|---|---|
| 02 weeks | Throat pain, heightened gag reflex | Yes (with meds) |
| 212 weeks | Voice change, dry mouth, mild swallowing difficulty | Varies |
| >12 weeks | Nasal regurgitation, velopharyngeal insufficiency | May persist |
LongTerm Side Effects
Nasal Regurgitation & Velopharyngeal Insufficiency
This sounds fancy, but it basically means food or liquid can slip into the nose when you swallow. It happens because the soft palate can't seal the airway as tightly after part of the uvula is gone. A study found that about 12% of UPPP patients report this issue beyond three months.
Voice Changes (nasal, hoarse, talker effect)
Because the uvula contributes to the way sound resonates in the throat, removing it can create a slightly nasal timbre. Research published in 2019 reported that roughly 3038% of patients notice a lasting voice shift. Most adapt over time, and voice therapy can often restore the balance.
Swallowing Difficulties & Globus Sensation
The lump in the throat feelingknown as globuscan linger. It's usually a sensation rather than a blockage, but it can be unsettling. Swallowing for larger bites may feel odd for a while, especially if you're used to a fuller uvula. If swallowing trouble continues, check our detailed post on swallowing disorder treatment for therapy options and red flags.
Taste & Smell Disturbances
Even a tiny change in airflow can alter how you experience flavors. Some people swear they taste food flatter for weeks after surgery.
Mouth & Throat Dryness / Mucus Overproduction
When the uvula is gone, the airway can become drier, prompting the glands to produce extra mucus as a protective response. A simple humidifier at night often does the trick.
Other Less Common Issues
- Weight loss after UPPP surgerysometimes due to better sleep and reduced nighttime snacking.
- Altered gag reflexsome notice a reduced sensitivity, while others become hyperaware.
- Occasional oral pain during the first few months.
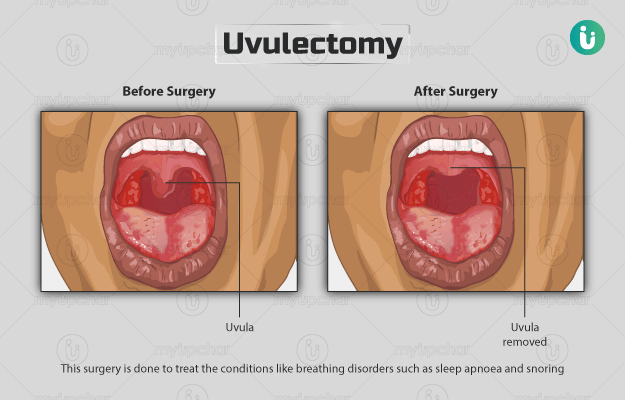
Can Uvula Grow Back?
Biology of uvular regeneration
After removal, the body fills the gap with scar tissue, not a brandnew uvula. The tissue contracts and stiffens, which is why the flap you see postop isn't the same as the original structure.
Rare cases of partial regrowth
There are anecdotal reports on medical forums of a tiny, fibrous nub forming where the uvula once was. These are exceptions, not the rule, and they typically don't restore the original function.
Expert Insight
Dr. Maya Patel, an ENT surgeon with 15 years of experience, notes, "Patients shouldn't expect the uvula to regrow. If you notice new tissue, it's usually scar tissuestill beneficial, but not a true uvula."
PostSurgery Eating Guide
Firstfew weeks: softfood checklist
- Warm broths (chicken, vegetable)
- Greek yogurt or kefir
- Mashed potatoes or sweet potatoes
- Silky smoothies (no seeds)
- Scrambled eggs, wellcooked oatmeal
3 month+ Reintroducing textures
Start adding softcooked veggies, tender fish, or ground meats. Test each new texture slowlyif you feel a catch in the throat, pause and revert to softer foods for a few more days.
Hydration & saliva stimulants
Staying hydrated is key. Sip water throughout the day, and consider sugarfree gum or lozenges to boost saliva production. A humidifier in your bedroom can keep the airway moist while you sleep.
Sample 7Day Meal Plan
| Day | Breakfast | Lunch | Dinner |
|---|---|---|---|
| 1 | Warm chicken broth | Mashed sweet potatoes | Pureed carrot soup |
| 2 | Greek yogurt with honey | Soft scrambled eggs | Silky butternut squash puree |
| 3 | Oatmeal with banana mash | Creamy avocado mash | Gentle fish mousse |
| 47 | Rotate above options, adding gentle protein smoothies | Continue with soft proteins and wellcooked veggies | Introduce finely diced chicken or turkey |
Procedure Cost Overview
Breakdown of typical U.S. pricing (2025)
- Surgeon's fee: $1,200$3,000
- Anesthesia: $500$1,200
- Facility (hospital or ASC) charge: $800$2,500
- Followup appointments & postop care: $200$600
Insurance coverage vs. outofpocket
Many insurers cover UPPP when it's deemed medically necessary for obstructive sleep apnea (OSA). Look for CPT codes 42820 (UPPP) and 42825 (uvula excision) on your Explanation of Benefits. If you're selfpaying, ask the billing office about a bundled discount.
Cost vs. longterm benefit analysis
When you weigh the price against the potential for better sleep, reduced snoring, and lower cardiovascular risk, the investment often makes sense. A 2024 survey in ENTtoday reported that 78% of patients felt the financial cost was justified by the qualityoflife improvements.
QuickCalc Worksheet
| Item | Estimated Cost | Notes |
|---|---|---|
| Surgeon | $2,000 | Depends on region |
| Anesthesia | $800 | General vs. local |
| Facility | $1,500 | Hospital vs. ASC |
| Followup | $400 | Includes speech therapy |
| Total | $4,700 | Typical range $2,500$8,000 |
Managing Side Effects
Voice therapy & speechlanguage pathology
Professional voice coaches can teach techniques to balance resonance, helping many patients restore a more normal tone within 612 weeks. Success rates hover around 85% when therapy starts early.
Swallowing rehab (coughtrigger exercises)
Simple exerciseslike gently swallowing while visualizing the soft palate closingcan strengthen the muscles that compensate for the missing uvula. A speech therapist can show you the safest progressions.
Medications & topical treatments for dryness
Artificial saliva sprays, glycerinbased lozenges, and humidifiers all help. In some cases, a short course of lowdose antihistamine can reduce mucus overproduction without causing excessive dryness.
When to consider revision surgery
If you experience severe velopharyngeal insufficiency (persistent nasal regurgitation despite therapy) or chronic choking episodes, a revision may be recommended. Discuss imaging studies (like a lateral neck Xray) with your surgeon to evaluate the anatomy.
Symptom CheckIn Checklist
- Dry throat lasting >3 months? Talk to your doctor.
- Voice still nasal after 6 weeks? Try voice therapy.
- Food/saliva entering nose? Seek evaluation for velopharyngeal insufficiency.
- Weight loss >10%? Review sleep study results.
RealWorld Patient Stories
Case study A 45yearold male, OSA, 2yr followup
Mark underwent UPPP to treat moderate obstructive sleep apnea. Six months postop he reported a mild nasal voice and occasional dry throat. He started voice therapy at month 8, which reduced the nasality by 60%. At the twoyear mark, his apneahypopnea index dropped from 28 to 5, and he felt like a new person.
Case study B 28yearold female, chronic gag reflex
Sara had a uvula excision after recurrent infections. The first month was a swirl of throat soreness and heightened gag reflex. By week 6 she introduced soft foods and used a humidifier nightly. Her gag reflex gradually normalized, and by month 4 she could eat a softcooked vegetable without any fliptheswitch feeling.
Share Your Experience
What's your story? If you've lived without a uvula for a while, drop a comment below. Your insights could guide someone else through the same journey.
Frequently Asked Questions
Can the uvula grow back after removal?
No, the uvula is replaced by scar tissue; true regrowth is extremely rare.
What can I eat after uvula surgery?
Stick to soft, nonirritating foodsthink broth, smoothies, mashed potatoesfor the first two weeks, then slowly reintroduce textures.
Will my voice change permanently?
Up to 30% notice a lasting nasal tone; speech therapy can improve it in most cases.
Is weight loss common after UPPP?
Some patients lose weight due to better sleep and reduced nighttime eating, but it isn't inevitable.
How much does the procedure cost?
In the United States, total outofpocket costs typically range from $2,500$8,000, depending on insurance, surgeon fees, and facility charges.
Balancing Benefits & Risks
Why many still choose uvula removal
The biggest draw is relief from chronic snoring and obstructive sleep apnea, which can dramatically improve quality of life, daytime alertness, and even longterm heart health.
When the longterm side effects outweigh the gains
If you develop severe velopharyngeal insufficiency, chronic dysphagia, or a voice that affects your professional life, those downsides may tip the scales toward reconsidering the surgery or seeking corrective procedures.
Pros vs. Cons QuickDecision Matrix
| Pros | Cons |
|---|---|
| Reduced snoring & apnea | Potential nasal regurgitation |
| Improved sleep quality | Voice changes (nasal tone) |
| Lower cardiovascular risk | Dry throat & mucus issues |
| Possible weight loss | Rare chance of needing revision |
Conclusion
Living without a uvula can feel like stepping onto a new terrainthere are adjustments, but also unexpected freedoms. Most people see the biggest payoff in better sleep and quieter nights, while a minority wrestle with lingering side effects such as dry throat, voice changes, or occasional nasal regurgitation. By understanding the typical recovery timeline, recognizing which longterm symptoms merit medical attention, and adopting practical diet and therapy strategies, you can keep the new normal comfortable and confident. If you've been through uvula removal, share your story below or ask a questionyou're not alone on this journey, and together we can turn uncertainty into empowerment.
FAQs
How long do the side effects of uvula removal typically last?
Most acute symptoms such as pain and swelling improve within 2‑4 weeks. If dry throat, voice changes, or mild swallowing issues persist beyond three months, they are considered long‑term and should be evaluated by your ENT or a speech‑language pathologist.
Can the uvula grow back after it’s been removed?
True regrowth does not occur. The space where the uvula was is filled with scar tissue, which may look like a small nub but does not restore the original function.
What are the most common voice changes after uvula removal?
Patients often notice a slightly nasal timbre or a “talker” quality because the uvula helps shape resonance. About 30‑38 % report a lasting change, but voice therapy can improve clarity for most people.
How can I relieve chronic dry throat after the surgery?
Stay well‑hydrated, use a humidifier at night, and consider saliva‑stimulating lozenges or artificial saliva sprays. A glycerin‑based mouth rinse can also soothe irritation.
When should I see a doctor for swallowing problems post‑uvula removal?
If you experience frequent choking, food or liquid entering the nose, or a sensation of food “sticking” that lasts longer than three months, schedule an appointment. An ENT can assess for velopharyngeal insufficiency and recommend swallowing therapy or, in rare cases, revision surgery.